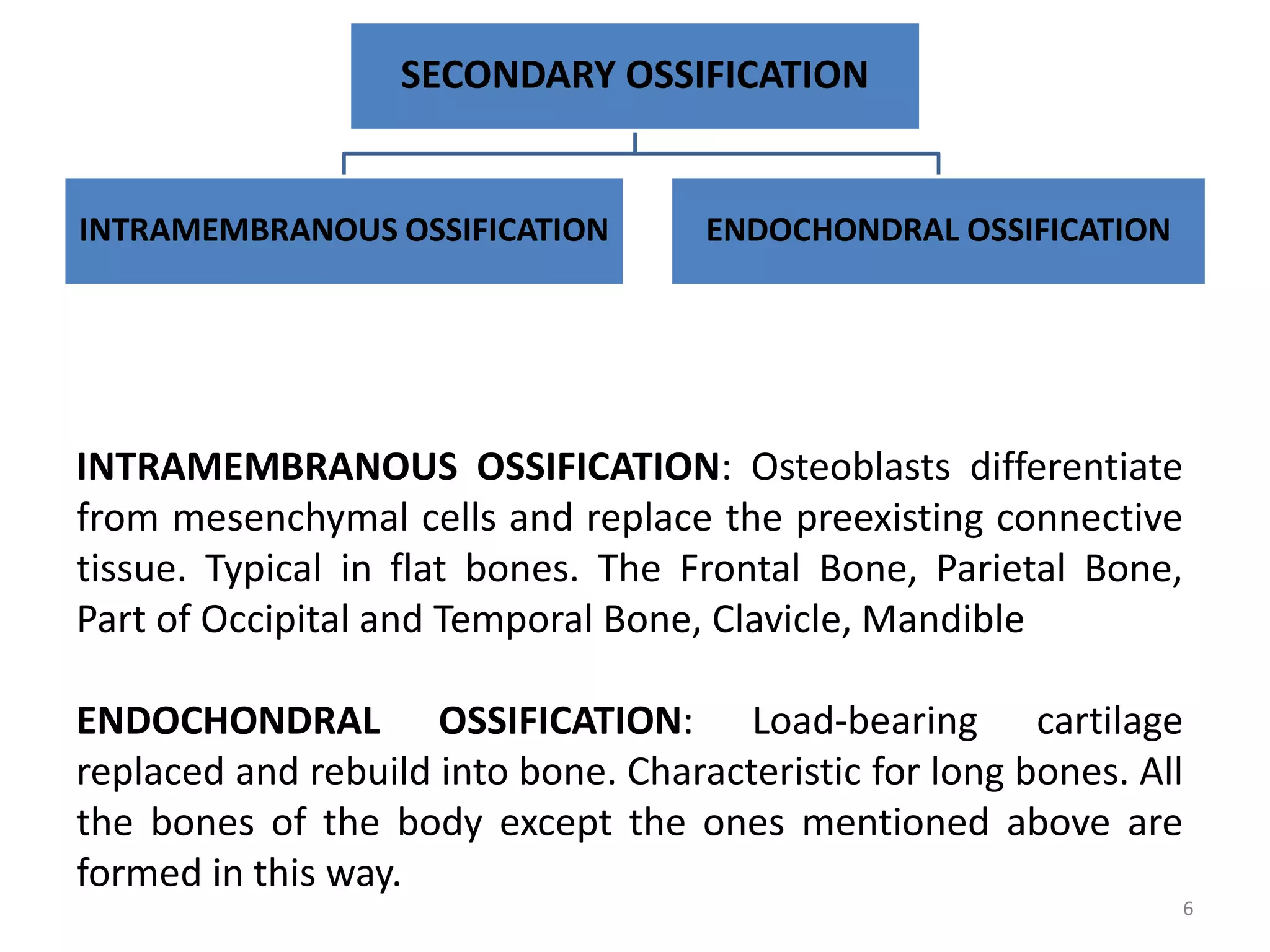
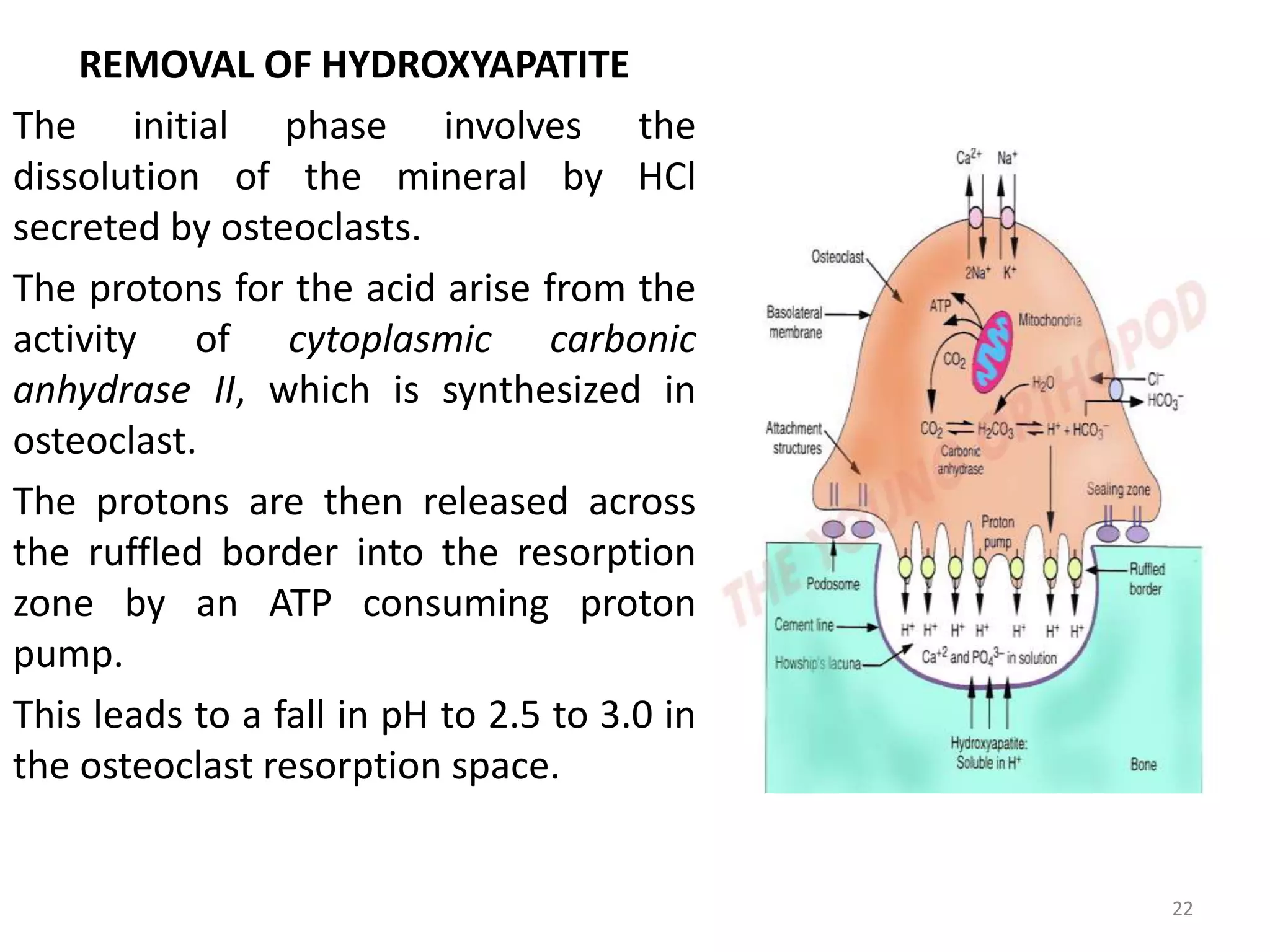
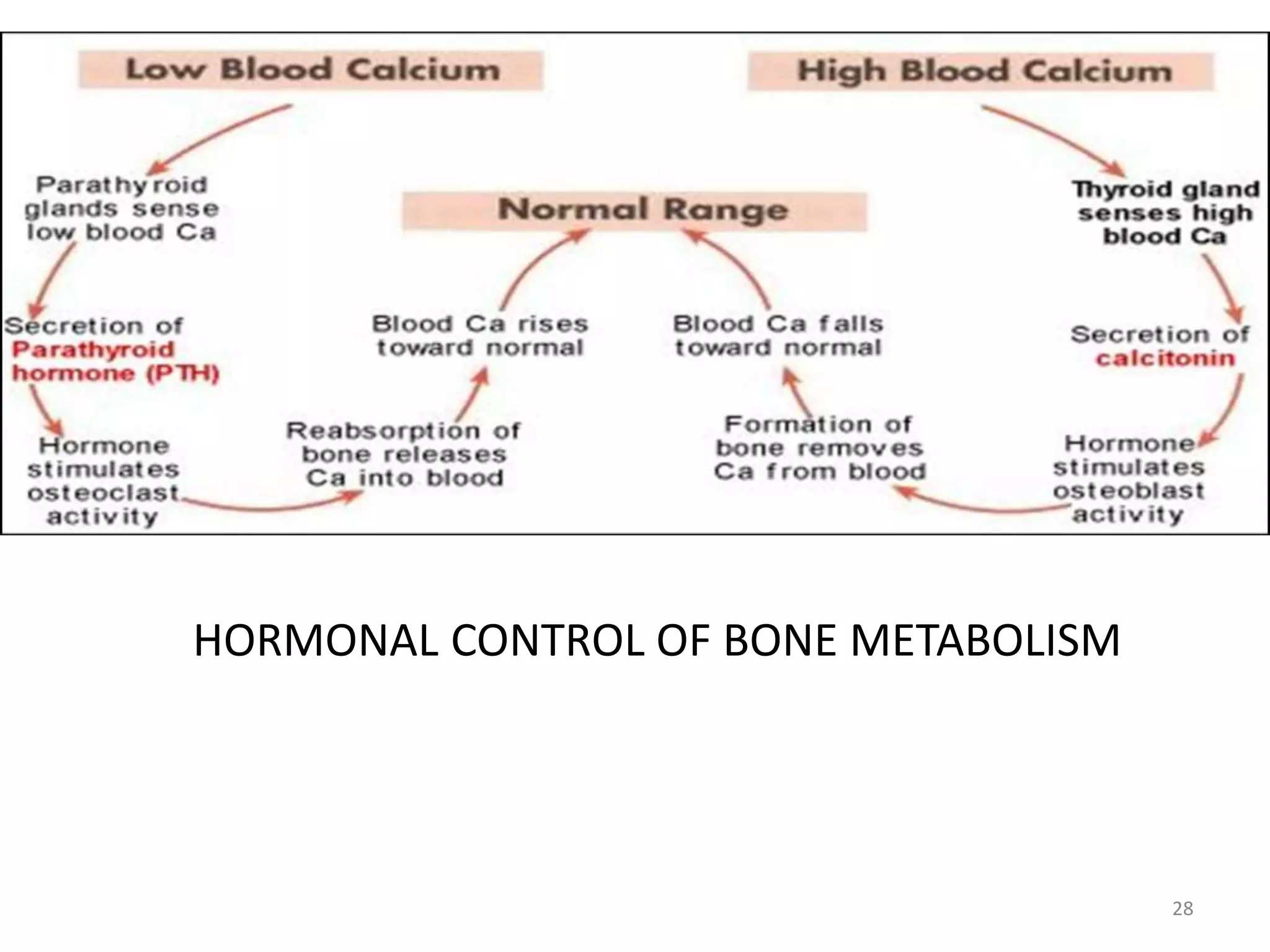
This document provides an overview of ossification, the process of bone formation. It discusses the classification of ossification into primary and secondary ossification, with the latter including intramembranous and endochondral ossification. The stages and factors involved in intramembranous and endochondral ossification are described in detail. Bone resorption, remodeling and the factors that influence these processes are also summarized.