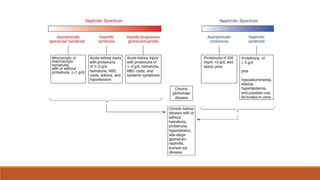
The document discusses nephrotic syndrome and nephritic syndrome. It covers:
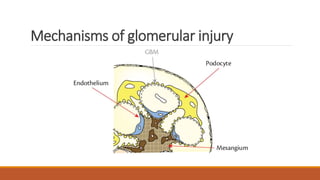
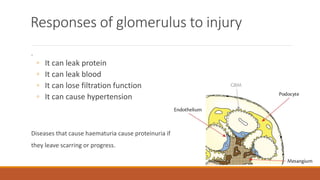
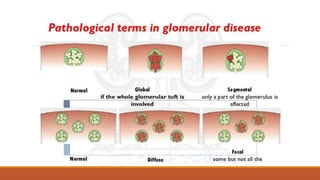
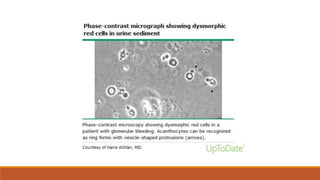
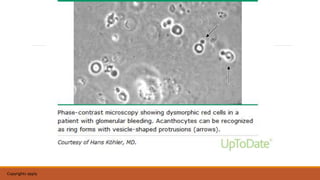
- Mechanisms of glomerular injury including proteinuria, hematuria, loss of filtration function, and hypertension.
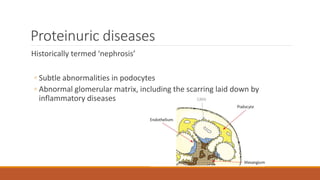
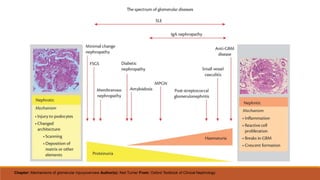
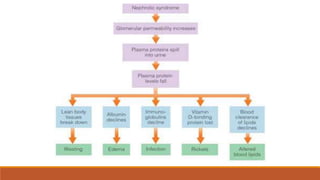
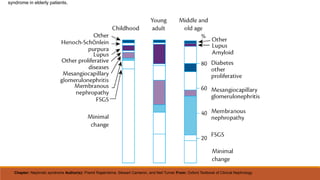
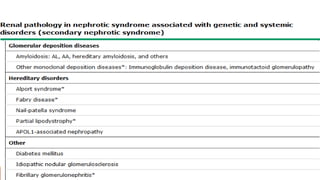
- Causes of nephrotic syndrome including minimal change disease, membranous nephropathy, and focal segmental glomerulosclerosis which often involve podocyte dysfunction.
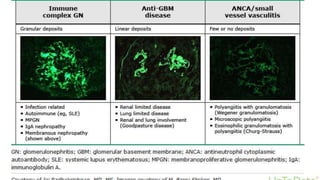
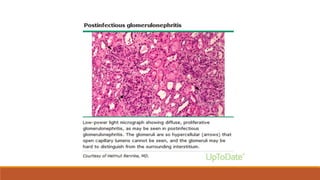
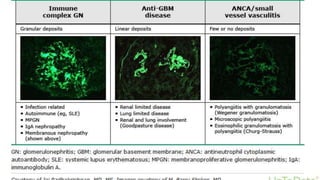
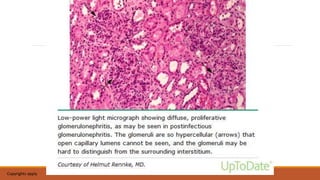
- Causes of nephritic syndrome include inflammatory diseases that break the glomerular basement membrane such as post-streptococcal glomerulonephritis.