New Options, Emerging Combinations in Advanced Hepatocellular Carcinoma: Are Management Approaches Poised For Transformation?
•
1 like•158 views
Ghassan Abou-Alfa, MD, MBA, Anthony El-Khoueiry, MD, and Richard S. Finn, MD, prepared useful practice aids pertaining to HCC management for this CME activity titled "New Options, Emerging Combinations in Advanced Hepatocellular Carcinoma: Are Management Approaches Poised For Transformation?" For the full presentation, monograph, complete CME information, and to apply for credit, please visit us at http://bit.ly/2okTvdb. CME credit will be available until March 7, 2019.
Report
Share
Report
Share
Download to read offline
Recommended
Teaming Up to Improve Outcomes in Advanced Hepatocellular Carcinoma: A Tumor ...

Teaming Up to Improve Outcomes in Advanced Hepatocellular Carcinoma: A Tumor ...PVI, PeerView Institute for Medical Education
Ghassan Abou-Alfa, MD, MBA, Anthony El-Khoueiry, MD, and R. Kate Kelley, MD, prepared useful Practice Aids pertaining to liver cancer for this CME/CE activity titled "Teaming Up to Improve Outcomes in Advanced Hepatocellular Carcinoma: A Tumor Board Evaluating the Potential of Immunotherapy and Novel Targeted Approaches." For the full presentation, monograph, complete CME/CE information, and to apply for credit, please visit us at http://bit.ly/2FG0J75. CME/CE credit will be available until March 25, 2019.Keeping Pace With Immunotherapy Advances in Bladder Cancer: Tools for Winning...

Keeping Pace With Immunotherapy Advances in Bladder Cancer: Tools for Winning...PVI, PeerView Institute for Medical Education
Arjun Balar, MD, and Petros Grivas, MD, PhD, prepared useful practice aids pertaining to bladder cancer management for this CME activity titled "Keeping Pace With Immunotherapy Advances in Bladder Cancer: Tools for Winning the Race and Optimizing Patient Outcomes." For the full presentation, monograph, complete CME information, and to apply for credit, please visit us at http://bit.ly/2GpacAq. CME credit will be available until December 30, 2019.Strengthening Our Grip on Immuno-Oncology in Genitourinary Cancers: Understan...

Strengthening Our Grip on Immuno-Oncology in Genitourinary Cancers: Understan...PVI, PeerView Institute for Medical Education
Jonathan E. Rosenberg, MD, Hans Hammers, MD, PhD, and Ravi A. Madan, MD, prepared useful practice aids pertaining to genitourinary cancers for this CME activity titled "Strengthening Our Grip on Immuno-Oncology in Genitourinary Cancers: Understanding Science Through Stories." For the full presentation, monograph, complete CME information, and to apply for credit, please visit us at http://bit.ly/2FAbCH0. CME credit will be available until March 21, 2019.
Management of menopausal symptoms in breast cancer survivors

Management of menopausal symptoms in breast cancer survivors- hormonal and nonhormonal
Patient Controlled Analgesia: Return to Nursing Program

This presentation outlines how nurses can use Patient Controlled Analgesia (PCA) to benefit patients/clients. This presentation covers:
1. Indications and contraindications of PCA use
2. The advantages of PCA
and
3. The pharmacological principles of pain management
This presentation was compiled by Gulzar Malik, an experienced and qualified Nursing Educator at IHNA. For more information about our return to nursing programs, please call 1800 22 52 83.
New Concepts in Prostate Cancer Care: What Oncologists Need to Know to Optimi...

New Concepts in Prostate Cancer Care: What Oncologists Need to Know to Optimi...PVI, PeerView Institute for Medical Education
Robert Dreicer, MD, MS, MACP, FASCO, Philip Kantoff, MD, Charles J. Ryan, MD, and Evan Y. Yu, MD, prepared useful practice aids pertaining to prostate cancer for this CME activity titled "New Concepts in Prostate Cancer Care: What Oncologists Need to Know to Optimize Patient Outcomes.” For the full presentation, monograph, complete CME information, and to apply for credit, please visit us at http://bit.ly/2FLnDrG. CME credit will be available until July 15, 2020.PCA Documentation

After discovering a lapse in documentation for PCAs in the Operating Room I created a short RN education inservice to correct this. Here is a presentation of my findings.
How I Think, How I Treat: Learning to Navigate the Modern Prostate Cancer Lan...

How I Think, How I Treat: Learning to Navigate the Modern Prostate Cancer Lan...PVI, PeerView Institute for Medical Education
William K. Oh, MD; Charles J. Ryan, MD; Evan Y. Yu, MD, prepared useful Practice Aids pertaining to prostate cancer for this CME/MOC activity titled "How I Think, How I Treat: Learning to Navigate the Modern Prostate Cancer Landscape." For the full presentation, downloadable Practice Aids, and complete CME/MOC information and instructions on applying for credit, please visit us at https://bit.ly/3dOsCXN. CME/MOC credit will be available until July 7, 2021.Recommended
Teaming Up to Improve Outcomes in Advanced Hepatocellular Carcinoma: A Tumor ...

Teaming Up to Improve Outcomes in Advanced Hepatocellular Carcinoma: A Tumor ...PVI, PeerView Institute for Medical Education
Ghassan Abou-Alfa, MD, MBA, Anthony El-Khoueiry, MD, and R. Kate Kelley, MD, prepared useful Practice Aids pertaining to liver cancer for this CME/CE activity titled "Teaming Up to Improve Outcomes in Advanced Hepatocellular Carcinoma: A Tumor Board Evaluating the Potential of Immunotherapy and Novel Targeted Approaches." For the full presentation, monograph, complete CME/CE information, and to apply for credit, please visit us at http://bit.ly/2FG0J75. CME/CE credit will be available until March 25, 2019.Keeping Pace With Immunotherapy Advances in Bladder Cancer: Tools for Winning...

Keeping Pace With Immunotherapy Advances in Bladder Cancer: Tools for Winning...PVI, PeerView Institute for Medical Education
Arjun Balar, MD, and Petros Grivas, MD, PhD, prepared useful practice aids pertaining to bladder cancer management for this CME activity titled "Keeping Pace With Immunotherapy Advances in Bladder Cancer: Tools for Winning the Race and Optimizing Patient Outcomes." For the full presentation, monograph, complete CME information, and to apply for credit, please visit us at http://bit.ly/2GpacAq. CME credit will be available until December 30, 2019.Strengthening Our Grip on Immuno-Oncology in Genitourinary Cancers: Understan...

Strengthening Our Grip on Immuno-Oncology in Genitourinary Cancers: Understan...PVI, PeerView Institute for Medical Education
Jonathan E. Rosenberg, MD, Hans Hammers, MD, PhD, and Ravi A. Madan, MD, prepared useful practice aids pertaining to genitourinary cancers for this CME activity titled "Strengthening Our Grip on Immuno-Oncology in Genitourinary Cancers: Understanding Science Through Stories." For the full presentation, monograph, complete CME information, and to apply for credit, please visit us at http://bit.ly/2FAbCH0. CME credit will be available until March 21, 2019.
Management of menopausal symptoms in breast cancer survivors

Management of menopausal symptoms in breast cancer survivors- hormonal and nonhormonal
Patient Controlled Analgesia: Return to Nursing Program

This presentation outlines how nurses can use Patient Controlled Analgesia (PCA) to benefit patients/clients. This presentation covers:
1. Indications and contraindications of PCA use
2. The advantages of PCA
and
3. The pharmacological principles of pain management
This presentation was compiled by Gulzar Malik, an experienced and qualified Nursing Educator at IHNA. For more information about our return to nursing programs, please call 1800 22 52 83.
New Concepts in Prostate Cancer Care: What Oncologists Need to Know to Optimi...

New Concepts in Prostate Cancer Care: What Oncologists Need to Know to Optimi...PVI, PeerView Institute for Medical Education
Robert Dreicer, MD, MS, MACP, FASCO, Philip Kantoff, MD, Charles J. Ryan, MD, and Evan Y. Yu, MD, prepared useful practice aids pertaining to prostate cancer for this CME activity titled "New Concepts in Prostate Cancer Care: What Oncologists Need to Know to Optimize Patient Outcomes.” For the full presentation, monograph, complete CME information, and to apply for credit, please visit us at http://bit.ly/2FLnDrG. CME credit will be available until July 15, 2020.PCA Documentation

After discovering a lapse in documentation for PCAs in the Operating Room I created a short RN education inservice to correct this. Here is a presentation of my findings.
How I Think, How I Treat: Learning to Navigate the Modern Prostate Cancer Lan...

How I Think, How I Treat: Learning to Navigate the Modern Prostate Cancer Lan...PVI, PeerView Institute for Medical Education
William K. Oh, MD; Charles J. Ryan, MD; Evan Y. Yu, MD, prepared useful Practice Aids pertaining to prostate cancer for this CME/MOC activity titled "How I Think, How I Treat: Learning to Navigate the Modern Prostate Cancer Landscape." For the full presentation, downloadable Practice Aids, and complete CME/MOC information and instructions on applying for credit, please visit us at https://bit.ly/3dOsCXN. CME/MOC credit will be available until July 7, 2021.Bja 2015 114(4)

Les NVPO sont un événement fréquent en post-anesthésie puisqu'ils touchent environ un tiers des patients. Les différents scores et prophylaxies utilisées bien que souvent efficaces ne closent pas le chapitre de leur prévention. La gabapentine, antivonvusilvant, a montré par ailleurs son effet analgésique en post-opératoire.
Plus récemment, la gabapentine a montré un effet anti-émétique lorsqu'elle était administrée en prévention dans la chimiothérapie du cancer du sein.
Cette étude est une méta-analyse des essais randomisés de la gabapentine en prévention des NVPO. Elle conclut à son efficacité, efficacité d'autant plus marquée que le propofol n'est pas utilisé comme agent d'induction et/ou d'entretien.
Antimicrobial Stewardship and Applications to Common Infections

Justin Kosar BSc., BSP
Lead – Antimicrobial Stewardship Pharmacist
Saskatoon Health Region
&
Lynette Kosar BSP, MSc
RxFiles Academic Detailing Program
Short and snappy topics - smbg, diabetic foot uclers, point of care testing ...

Short and snappy topics smbg,diabetic foot uclers, point of care testing CADTH
Value of Preoperative Gabapentin: An update from the literature

Journal club reviewing recent JAMA surgery and Anesthesia & Analgesia publications on the topic, in addition to background on mechanism of action, pharmocokinetics, and evidence based medicine thus far.
What is New for the Prostate Cancer Patient with Non-Metastatic Castration Re...

What is New for the Prostate Cancer Patient with Non-Metastatic Castration Re...Canadian Cancer Survivor Network
Don’t miss our upcoming webinars: Subscribe today!
In this webinar:
The basics of advanced prostate cancer, what it means to have non-metastatic castration resistant prostate cancer, the new treatment options now available for this disease space, and the prognosis for patients in this state of disease.
Presented by Dr. Robert Hamilton, urologic oncologist at Princess Margaret Cancer Centre and Associate Professor in the Department of Surgery (Urology) at the University of Toronto, this webinar will provide an overview of this subset of prostate cancer.
Dr. Hamilton’s clinical and research interests are in prostate cancer and testicular cancer. Dr. Hamilton trained at the University of Toronto and has completed a Masters of Public Health at The University of North Carolina at Chapel Hill, and a research fellowship at Duke University. He has also completed a fellowship at Memorial Sloan-Kettering Cancer Centre.
View the video:
https://youtu.be/wE3EVJm5Oo4
To learn more about CCSN, visit us at survivornet.ca
Follow CCSN on social media:
Twitter - https://twitter.com/survivornetca
Facebook - https://www.facebook.com/CanadianSurvivorNet
Instagram: https://www.instagram.com/survivornet_ca/
Pinterest - https://www.pinterest.com/survivornetworkImproving Management of Non-Metastatic Castration-Resistant Prostate Cancer (...

NOT FOR CME - FOR REFERENCE ONLY
In 2018, there will be an estimated 164,690 new cases of prostate cancer (PC) in the U.S. and approximately 29,430 patients will die of the disease, making it the third-leading cause of cancer death in men (American Cancer Society [ACS], 2018). The majority of men with PC are treated with curative intent (i.e., with radical prostatectomy or radiation therapy) with good outcomes, but a fraction of men with locoregional PC will develop progressive disease. Men who have initial PSA/biochemical recurrence after curative treatment are a heterogeneous group of individuals with good overall prognosis, including a median metastasis-free survival (MFS) >8 years and a median overall survival (OS) of >23 years (Rozet et al., 2016).
Approximately 10%-20% of prostate cancer patients develop castration-resistant PC (CRPC) within approximately 5 years of follow-up. Decisions about clinical management (i.e., when to start treatment) are challenging because it is unclear which patients will have shorter versus longer survival, and metastatic disease is not always reliably detected with imaging (Rozet et al., 2016).
Multiple new targeted agents, including immunotherapy, second-generation hormone therapy, and androgen biosynthesis inhibitors have been recently approved. Two recently published studies (PROSPER and SPARTAN) have changed the standard of care for patients with nmCRPC.
At the Nexus of Locoregional and Systemic Liver Cancer Therapy: A Multidiscip...

At the Nexus of Locoregional and Systemic Liver Cancer Therapy: A Multidiscip...PVI, PeerView Institute for Medical Education
Co-Chairs Matthew S. Johnson, MD, FSIR, and Richard S. Finn, MD, and Laura M. Kulik, MD, prepared useful Practice Aids pertaining to hepatocellular carcinoma for this CME activity titled “At the Nexus of Locoregional and Systemic Liver Cancer Therapy: A Multidisciplinary Tumor Board on Improving Outcomes in Intermediate to Advanced HCC.” For the full presentation, downloadable Practice Aids, and complete CME information, and to apply for credit, please visit us at http://bit.ly/2MrchQr. CME credit will be available until April 13, 2022.Enhancing Treatment Experiences in Castration-Resistant Prostate Cancer: The ...

i3 Health is pleased to make the speaker slides from this activity available for use as a nonaccredited self-study or teaching resource.
Guidelines for the Management of Transfusion Dependent Thalassaemia (4th Edit...

Guidelines for the Management of Transfusion Dependent Thalassaemia (4th Edit...Thalassaemia International Federation
TIF, its Board of Directors, and its International Scientific Advisory Board proudly present the 4th Edition of the Federation’s most prestigious and renowned publication, the TIF Guidelines For The Management of Transfusion-Dependent Thalassaemia (TDT).
Since 1999, when the very first edition was originally released as part of the Federation’s Educational Programme, the TIF Guidelines have been adopted and used extensively by academics, researchers and healthcare professionals all over the world as the only evidence-based reference text concerning the treatment of patients with TDT.
The newly launched edition includes brand new chapters on the recently approved modalities of patient treatment, the value of patient engagement at the decision-making level, the Reference Centres’ contribution to patient care, and much more.
Chair’s Take on Advances in Gynecologic Cancer Care: Exploring New Advances a...

Chair’s Take on Advances in Gynecologic Cancer Care: Exploring New Advances a...PVI, PeerView Institute for Medical Education
Linda R. Duska, MD, MPH, prepared useful practice aids pertaining to endometrial and cervical cancers for this CME/MOC activity titled Chair’s Take on Advances in Gynecologic Cancer Care: Exploring New Advances and Innovative Therapies in Endometrial and Cervical Cancers. For the full presentation, monograph, complete CME/MOC information, and to apply for credit, please visit us at https://bit.ly/2Uk5F72. CME/MOC credit will be available until June 17, 2021.Breaking the Paradox: Expanding Options and New Questions in HCC Management—M...

Breaking the Paradox: Expanding Options and New Questions in HCC Management—M...PVI, PeerView Institute for Medical Education
Richard S. Finn, MD, Anthony El-Khoueiry, MD, and Josep M. Llovet, MD, PhD, prepared useful practice aids pertaining to hepatocellular carcinoma for this CME activity titled "Breaking the Paradox: Expanding Options and New Questions in HCC Management: Mapping the Pathways to Better Patient Outcomes." For the full presentation, monograph, complete CME information, and to apply for credit, please visit us at http://bit.ly/2HU6L5K. CME credit will be available until February 14, 2020.More Related Content
What's hot
Bja 2015 114(4)

Les NVPO sont un événement fréquent en post-anesthésie puisqu'ils touchent environ un tiers des patients. Les différents scores et prophylaxies utilisées bien que souvent efficaces ne closent pas le chapitre de leur prévention. La gabapentine, antivonvusilvant, a montré par ailleurs son effet analgésique en post-opératoire.
Plus récemment, la gabapentine a montré un effet anti-émétique lorsqu'elle était administrée en prévention dans la chimiothérapie du cancer du sein.
Cette étude est une méta-analyse des essais randomisés de la gabapentine en prévention des NVPO. Elle conclut à son efficacité, efficacité d'autant plus marquée que le propofol n'est pas utilisé comme agent d'induction et/ou d'entretien.
Antimicrobial Stewardship and Applications to Common Infections

Justin Kosar BSc., BSP
Lead – Antimicrobial Stewardship Pharmacist
Saskatoon Health Region
&
Lynette Kosar BSP, MSc
RxFiles Academic Detailing Program
Short and snappy topics - smbg, diabetic foot uclers, point of care testing ...

Short and snappy topics smbg,diabetic foot uclers, point of care testing CADTH
Value of Preoperative Gabapentin: An update from the literature

Journal club reviewing recent JAMA surgery and Anesthesia & Analgesia publications on the topic, in addition to background on mechanism of action, pharmocokinetics, and evidence based medicine thus far.
What is New for the Prostate Cancer Patient with Non-Metastatic Castration Re...

What is New for the Prostate Cancer Patient with Non-Metastatic Castration Re...Canadian Cancer Survivor Network
Don’t miss our upcoming webinars: Subscribe today!
In this webinar:
The basics of advanced prostate cancer, what it means to have non-metastatic castration resistant prostate cancer, the new treatment options now available for this disease space, and the prognosis for patients in this state of disease.
Presented by Dr. Robert Hamilton, urologic oncologist at Princess Margaret Cancer Centre and Associate Professor in the Department of Surgery (Urology) at the University of Toronto, this webinar will provide an overview of this subset of prostate cancer.
Dr. Hamilton’s clinical and research interests are in prostate cancer and testicular cancer. Dr. Hamilton trained at the University of Toronto and has completed a Masters of Public Health at The University of North Carolina at Chapel Hill, and a research fellowship at Duke University. He has also completed a fellowship at Memorial Sloan-Kettering Cancer Centre.
View the video:
https://youtu.be/wE3EVJm5Oo4
To learn more about CCSN, visit us at survivornet.ca
Follow CCSN on social media:
Twitter - https://twitter.com/survivornetca
Facebook - https://www.facebook.com/CanadianSurvivorNet
Instagram: https://www.instagram.com/survivornet_ca/
Pinterest - https://www.pinterest.com/survivornetworkImproving Management of Non-Metastatic Castration-Resistant Prostate Cancer (...

NOT FOR CME - FOR REFERENCE ONLY
In 2018, there will be an estimated 164,690 new cases of prostate cancer (PC) in the U.S. and approximately 29,430 patients will die of the disease, making it the third-leading cause of cancer death in men (American Cancer Society [ACS], 2018). The majority of men with PC are treated with curative intent (i.e., with radical prostatectomy or radiation therapy) with good outcomes, but a fraction of men with locoregional PC will develop progressive disease. Men who have initial PSA/biochemical recurrence after curative treatment are a heterogeneous group of individuals with good overall prognosis, including a median metastasis-free survival (MFS) >8 years and a median overall survival (OS) of >23 years (Rozet et al., 2016).
Approximately 10%-20% of prostate cancer patients develop castration-resistant PC (CRPC) within approximately 5 years of follow-up. Decisions about clinical management (i.e., when to start treatment) are challenging because it is unclear which patients will have shorter versus longer survival, and metastatic disease is not always reliably detected with imaging (Rozet et al., 2016).
Multiple new targeted agents, including immunotherapy, second-generation hormone therapy, and androgen biosynthesis inhibitors have been recently approved. Two recently published studies (PROSPER and SPARTAN) have changed the standard of care for patients with nmCRPC.
At the Nexus of Locoregional and Systemic Liver Cancer Therapy: A Multidiscip...

At the Nexus of Locoregional and Systemic Liver Cancer Therapy: A Multidiscip...PVI, PeerView Institute for Medical Education
Co-Chairs Matthew S. Johnson, MD, FSIR, and Richard S. Finn, MD, and Laura M. Kulik, MD, prepared useful Practice Aids pertaining to hepatocellular carcinoma for this CME activity titled “At the Nexus of Locoregional and Systemic Liver Cancer Therapy: A Multidisciplinary Tumor Board on Improving Outcomes in Intermediate to Advanced HCC.” For the full presentation, downloadable Practice Aids, and complete CME information, and to apply for credit, please visit us at http://bit.ly/2MrchQr. CME credit will be available until April 13, 2022.Enhancing Treatment Experiences in Castration-Resistant Prostate Cancer: The ...

i3 Health is pleased to make the speaker slides from this activity available for use as a nonaccredited self-study or teaching resource.
Guidelines for the Management of Transfusion Dependent Thalassaemia (4th Edit...

Guidelines for the Management of Transfusion Dependent Thalassaemia (4th Edit...Thalassaemia International Federation
TIF, its Board of Directors, and its International Scientific Advisory Board proudly present the 4th Edition of the Federation’s most prestigious and renowned publication, the TIF Guidelines For The Management of Transfusion-Dependent Thalassaemia (TDT).
Since 1999, when the very first edition was originally released as part of the Federation’s Educational Programme, the TIF Guidelines have been adopted and used extensively by academics, researchers and healthcare professionals all over the world as the only evidence-based reference text concerning the treatment of patients with TDT.
The newly launched edition includes brand new chapters on the recently approved modalities of patient treatment, the value of patient engagement at the decision-making level, the Reference Centres’ contribution to patient care, and much more.
What's hot (20)
Antimicrobial Stewardship and Applications to Common Infections

Antimicrobial Stewardship and Applications to Common Infections
Short and snappy topics - smbg, diabetic foot uclers, point of care testing ...

Short and snappy topics - smbg, diabetic foot uclers, point of care testing ...
Spanish Multi-Center Fast-Track Group - Protocol and Preliminary Results

Spanish Multi-Center Fast-Track Group - Protocol and Preliminary Results
Value of Preoperative Gabapentin: An update from the literature

Value of Preoperative Gabapentin: An update from the literature
What is New for the Prostate Cancer Patient with Non-Metastatic Castration Re...

What is New for the Prostate Cancer Patient with Non-Metastatic Castration Re...
Improving Management of Non-Metastatic Castration-Resistant Prostate Cancer (...

Improving Management of Non-Metastatic Castration-Resistant Prostate Cancer (...
At the Nexus of Locoregional and Systemic Liver Cancer Therapy: A Multidiscip...

At the Nexus of Locoregional and Systemic Liver Cancer Therapy: A Multidiscip...
Enhancing Treatment Experiences in Castration-Resistant Prostate Cancer: The ...

Enhancing Treatment Experiences in Castration-Resistant Prostate Cancer: The ...
Non-Hormonal Drug-Therapy Options to Treat Postmenopausal Vasomotor Symptoms

Non-Hormonal Drug-Therapy Options to Treat Postmenopausal Vasomotor Symptoms
Guidelines for the Management of Transfusion Dependent Thalassaemia (4th Edit...

Guidelines for the Management of Transfusion Dependent Thalassaemia (4th Edit...
Similar to New Options, Emerging Combinations in Advanced Hepatocellular Carcinoma: Are Management Approaches Poised For Transformation?
Chair’s Take on Advances in Gynecologic Cancer Care: Exploring New Advances a...

Chair’s Take on Advances in Gynecologic Cancer Care: Exploring New Advances a...PVI, PeerView Institute for Medical Education
Linda R. Duska, MD, MPH, prepared useful practice aids pertaining to endometrial and cervical cancers for this CME/MOC activity titled Chair’s Take on Advances in Gynecologic Cancer Care: Exploring New Advances and Innovative Therapies in Endometrial and Cervical Cancers. For the full presentation, monograph, complete CME/MOC information, and to apply for credit, please visit us at https://bit.ly/2Uk5F72. CME/MOC credit will be available until June 17, 2021.Breaking the Paradox: Expanding Options and New Questions in HCC Management—M...

Breaking the Paradox: Expanding Options and New Questions in HCC Management—M...PVI, PeerView Institute for Medical Education
Richard S. Finn, MD, Anthony El-Khoueiry, MD, and Josep M. Llovet, MD, PhD, prepared useful practice aids pertaining to hepatocellular carcinoma for this CME activity titled "Breaking the Paradox: Expanding Options and New Questions in HCC Management: Mapping the Pathways to Better Patient Outcomes." For the full presentation, monograph, complete CME information, and to apply for credit, please visit us at http://bit.ly/2HU6L5K. CME credit will be available until February 14, 2020.Breaking Down the Evidence in Bladder Cancer: Expert Perspectives and Practic...

Breaking Down the Evidence in Bladder Cancer: Expert Perspectives and Practic...PVI, PeerView Institute for Medical Education
Chair and Moderator, Petros Grivas, MD, PhD, Shilpa Gupta, MD, and Gary D. Steinberg, MD, prepared useful Practice Aids pertaining to bladder cancer for this CME/MOC activity titled “Breaking Down the Evidence in Bladder Cancer: Expert Perspectives and Practical Strategies on Immune, Targeted, and Antibody-Based Therapies.” For the full presentation, downloadable Practice Aids, and complete CME/MOC information, and to apply for credit, please visit us at https://bit.ly/2WcJp3n. CME/MOC credit will be available until December 31, 2022.
Rethinking Successful Care for Pancreatic Cancer: Therapeutic Sequencing, Inn...

Rethinking Successful Care for Pancreatic Cancer: Therapeutic Sequencing, Inn...PVI, PeerView Institute for Medical Education
Johanna C. Bendell, MD, George P. Kim, MD, and Eileen M. O'Reilly, MD, prepared useful practice aids pertaining to pancreatic cancer management for this CME activity titled "Rethinking Successful Care for Pancreatic Cancer: Therapeutic Sequencing, Innovative Strategies, and Patient Perspectives on Disease Management." For the full presentation, monograph, complete CME information, and to apply for credit, please visit us at http://bit.ly/2K1bR0N. CME credit will be available until July 4, 2019.Surveying the View From the Driver’s Seat in Hepatocellular Carcinoma: Bringi...

Surveying the View From the Driver’s Seat in Hepatocellular Carcinoma: Bringi...PVI, PeerView Institute for Medical Education
Jorge A. Marrero, MD, MS, Anthony El-Khoueiry, MD, Richard S. Finn, MD, and Laura M. Kulik, MD, prepared useful practice aids pertaining to HCC management for this CME activity titled "Surveying the View From the Driver’s Seat in Hepatocellular Carcinoma: Bringing Into Focus Hepatology’s Key Role in Guiding HCC Care Down the Path to Improved Outcomes." For the full presentation, monograph, complete CME information, and to apply for credit, please visit us at http://bit.ly/2Pj9wM8. CME credit will be available until December 20, 2019.Urgent Care of Patients Receiving Cancer Immunotherapy: Recognition and Manag...

Urgent Care of Patients Receiving Cancer Immunotherapy: Recognition and Manag...PVI, PeerView Institute for Medical Education
Evan J. Lipson, MD, Andrew Stolbach, MD, MPH, and Trish Brothers, BSN, RN, OCN®, prepared useful practice aids pertaining to oncologic emergencies for this CME/MOC/CNE/CPE activity titled "Urgent Care of Patients Receiving Cancer Immunotherapy: Recognition and Management of Immune-Mediated Adverse Reactions in the ED." For the full presentation, monograph, complete CME/MOC/CNE/CPE information, and to apply for credit, please visit us at http://bit.ly/2TGpnYl. CME/MOC/CNE/CPE credit will be available until February 21, 2020.Pancreatic cancer presentaion

An disease state review of pancreatic cancer and some in progress investigational treatment options.
Immunotherapy as a Component of Multimodal Therapy in Locally Advanced and Ea...

Immunotherapy as a Component of Multimodal Therapy in Locally Advanced and Ea...PVI, PeerView Institute for Medical Education
Brendon Stiles, MD, Jamie E. Chaft, MD, and David H. Harpole Jr., MD, prepared useful Practice Aids pertaining to immunotherapy in earlier stages of lung cancer for this CME/MOC activity titled, "Immunotherapy as a Component of Multimodal Therapy in Locally Advanced and Earlier Stages of Lung Cancer: Rationale, Evidence, and Implications for the Multidisciplinary Team." For the full presentation, complete CME/MOC information, and to apply for credit, please visit us at https://bit.ly/2UnPFkF. CME/MOC credit will be available until June 24, 2021.CORALLEEN phase 2 trial: Neoadjuvant Ribociclib plus Letrozole in Early Stage...

First trial regarding molecular down-staging in breast cancer and First neoadjuvant approach in Luminal B early stage breast cancer
Pioneering Precision Medicine in Bladder Cancer: Multidisciplinary Perspectiv...

Pioneering Precision Medicine in Bladder Cancer: Multidisciplinary Perspectiv...PVI, PeerView Institute for Medical Education
Chair and Presenter Neal D. Shore, MD, FACS, Sia Daneshmand, MD, and Guru P. Sonpavde, MD, prepared useful Practice Aids pertaining to bladder cancer for this CME/MOC/AAPA activity titled “Pioneering Precision Medicine in Bladder Cancer: Multidisciplinary Perspectives on Personalizing Patient Care.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/AAPA information, and to apply for credit, please visit us at https://bit.ly/40qGkJH. CME/MOC/AAPA credit will be available until December 28, 2024.Ulcerative Colitis: Applying Guidelines in Practice

This presentation developed was by David Rubin, MD, Millie Long, MD, MPH, and Anita Afzali, MD, MPH, for a CME activity titled, Ulcerative Colitis: Applying Guidelines in Practice
GOG 240 Bevacizumab in carcinoma cervix

GOG 240 Bevacizumab in carcinoma cervix, 2nd interim and Final analysis
Transitioning Survival from Months to Years in Advanced Non-Small Cell Lung C...

Dr. Jack West reviews the evolution of new treatment options for advanced NSCLC that have steadily improved survival. This progress has been incremental but now means that an ever-growing proportion of patients with advanced NSCLC have a realistic promise of potentially living several years after their diagnosis and the start of treatment. Note that this presentation does not address advances in immunotherapy, which were covered in a separate talk at the same conference at which Dr. West delivered this presentation.
What's New in Treatment and Clinical Trials for Advanced Triple-Negative Brea...

What's New in Treatment and Clinical Trials for Advanced Triple-Negative Brea...Dana-Farber Cancer Institute
Learn about the latest treatment options for advanced triple-negative breast cancer. Nancy Lin, MD, a breast oncologist in the Susan F. Smith Center for Women's Cancers at Dana-Farber, discusses new research.
This presentation was originally given as part of the 2015 Metastatic Breast Cancer Forum, held at Dana-Farber Cancer Institute in Boston, Mass. on Oct. 17, 2015.
More information is available at http://www.susanfsmith.org.How I Think, How I Treat—Personal Insights on Current Practices and Evolving ...

How I Think, How I Treat—Personal Insights on Current Practices and Evolving ...PVI, PeerView Institute for Medical Education
Johanna C. Bendell, MD; Tanios Bekaii-Saab, MD, FACP; Michael J. Pishvaian, MD, PhD; and Rachna T. Shroff, MD, MS prepared useful practice aids pertaining to pancreatic cancer for this CME/MOC activity titled How I Think, How I Treat—Personal Insights on Current Practices and Evolving Standards of Care in Pancreatic Cancer: Expert Perspectives on Implementing State-of-the-Art Care in the Clinic. For the full presentation, monograph, complete CME/MOC information, and to apply for credit, please visit us at http://bit.ly/2uNJtbI. CME/MOC credit will be available until March 4, 2021.Similar to New Options, Emerging Combinations in Advanced Hepatocellular Carcinoma: Are Management Approaches Poised For Transformation? (20)
Chair’s Take on Advances in Gynecologic Cancer Care: Exploring New Advances a...

Chair’s Take on Advances in Gynecologic Cancer Care: Exploring New Advances a...
Breaking the Paradox: Expanding Options and New Questions in HCC Management—M...

Breaking the Paradox: Expanding Options and New Questions in HCC Management—M...
Breaking Down the Evidence in Bladder Cancer: Expert Perspectives and Practic...

Breaking Down the Evidence in Bladder Cancer: Expert Perspectives and Practic...
Rethinking Successful Care for Pancreatic Cancer: Therapeutic Sequencing, Inn...

Rethinking Successful Care for Pancreatic Cancer: Therapeutic Sequencing, Inn...
Surveying the View From the Driver’s Seat in Hepatocellular Carcinoma: Bringi...

Surveying the View From the Driver’s Seat in Hepatocellular Carcinoma: Bringi...
Urgent Care of Patients Receiving Cancer Immunotherapy: Recognition and Manag...

Urgent Care of Patients Receiving Cancer Immunotherapy: Recognition and Manag...
Immunotherapy as a Component of Multimodal Therapy in Locally Advanced and Ea...

Immunotherapy as a Component of Multimodal Therapy in Locally Advanced and Ea...
CORALLEEN phase 2 trial: Neoadjuvant Ribociclib plus Letrozole in Early Stage...

CORALLEEN phase 2 trial: Neoadjuvant Ribociclib plus Letrozole in Early Stage...
Pioneering Precision Medicine in Bladder Cancer: Multidisciplinary Perspectiv...

Pioneering Precision Medicine in Bladder Cancer: Multidisciplinary Perspectiv...
Ulcerative Colitis: Applying Guidelines in Practice

Ulcerative Colitis: Applying Guidelines in Practice
Transitioning Survival from Months to Years in Advanced Non-Small Cell Lung C...

Transitioning Survival from Months to Years in Advanced Non-Small Cell Lung C...
What's New in Treatment and Clinical Trials for Advanced Triple-Negative Brea...

What's New in Treatment and Clinical Trials for Advanced Triple-Negative Brea...
How I Think, How I Treat—Personal Insights on Current Practices and Evolving ...

How I Think, How I Treat—Personal Insights on Current Practices and Evolving ...
More from PVI, PeerView Institute for Medical Education
Establishing the Collaborative Benchmark for HCC Care: Critical Discussions B...

Establishing the Collaborative Benchmark for HCC Care: Critical Discussions B...PVI, PeerView Institute for Medical Education
Co-Chairs Riad Salem, MD, MBA, and Mark Yarchoan, MD, discuss liver cancer in this CME/MOC activity titled “Establishing the Collaborative Benchmark for HCC Care: Critical Discussions Between Interventional Radiologists and Oncologists to Maximize Therapeutic Benefit.” For the full presentation, downloadable Practice Aids, and complete CME/MOC information, and to apply for credit, please visit us at https://bit.ly/3IOQvQ6. CME/MOC credit will be available until June 14, 2025.Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...

Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...PVI, PeerView Institute for Medical Education
Co-Chairs, Brett Elicker, MD, and David E. Griffith, MD, ATSF, ACCP, OFRSM, prepared useful Practice Aids pertaining to non-cystic fibrosis bronchiectasis for this CME/MOC activity titled “Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: Ensuring Prompt Diagnosis Through Accurate Interpretation of CT Imaging.” For the full presentation, downloadable Practice Aids, and complete CME/MOC information, and to apply for credit, please visit us at https://bit.ly/48WUULu. CME/MOC credit will be available until June 4, 2025.Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...

Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...PVI, PeerView Institute for Medical Education
Co-Chairs, Brett Elicker, MD, and David E. Griffith, MD, ATSF, ACCP, OFRSM, discuss non-cystic fibrosis bronchiectasis in this CME/MOC activity titled “Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: Ensuring Prompt Diagnosis Through Accurate Interpretation of CT Imaging.” For the full presentation, downloadable Practice Aids, and complete CME/MOC information, and to apply for credit, please visit us at https://bit.ly/48WUULu. CME/MOC credit will be available until June 4, 2025.Applying Advances in PET Imaging to Facilitate the Early Diagnosis of Alzheim...

Applying Advances in PET Imaging to Facilitate the Early Diagnosis of Alzheim...PVI, PeerView Institute for Medical Education
Co-Chairs, Jonathan E. McConathy, MD, PhD, and Gil Rabinovici, MD, discuss Alzheimer's disease in this CME/AAPA activity titled “Applying Advances in PET Imaging to Facilitate the Early Diagnosis of Alzheimer’s Disease: Preparing Nuclear Medicine and Radiology Specialists for New Diagnostic Workflows.” For the full presentation, downloadable Practice Aids, and complete CME/AAPA information, and to apply for credit, please visit us at https://bit.ly/45RFl6g. CME/AAPA credit will be available until June 15, 2025.A Pharmacist’s Take on Navigating the Expanding Therapeutic Landscape for End...

A Pharmacist’s Take on Navigating the Expanding Therapeutic Landscape for End...PVI, PeerView Institute for Medical Education
Co-Chairs Sarah Hayward, PharmD, BCOP, and Ambar Khan, PharmD, BCOP, discuss endometrial and cervical cancers in this CME/CPE/IPCE activity titled “A Pharmacist’s Take on Navigating the Expanding Therapeutic Landscape for Endometrial and Cervical Cancers: Insights on Coordinating and Delivering Effective Modern Care.” For the full presentation, downloadable Practice Aids, and complete CME/CPE/IPCE information, and to apply for credit, please visit us at https://bit.ly/3wGBPQp. CME/CPE/IPCE credit will be available until May 27, 2025.
“Four-Ward” Progress in NDMM: New Developments With CD38 Antibody Quadruplets

“Four-Ward” Progress in NDMM: New Developments With CD38 Antibody QuadrupletsPVI, PeerView Institute for Medical Education
Co-Chairs, Suzanne Lentzsch, MD, PhD, and Joshua Richter, MD, discuss multiple myeloma in this CME activity titled “‘Four-Ward’ Progress in NDMM: New Developments With CD38 Antibody Quadruplets.” For the full presentation and complete CME information, and to apply for credit, please visit us at https://bit.ly/3x3oWA3. CME credit will be available until May 23, 2025.Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable N...

Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable N...PVI, PeerView Institute for Medical Education
Co-Chairs, Jessica Donington, MD, and Jonathan D. Spicer, MD, PhD, FRCSC, prepared useful Practice Aids pertaining to lung cancer for this CME/MOC/AAPA activity titled “Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable NSCLC: A Case Exploration of New Standards and Emerging Approaches.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/AAPA information, and to apply for credit, please visit us at https://bit.ly/3TxdcP5. CME/MOC/AAPA credit will be available until June 7, 2025.Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable N...

Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable N...PVI, PeerView Institute for Medical Education
Co-Chairs, Jessica Donington, MD, and Jonathan D. Spicer, MD, PhD, FRCSC, discuss lung cancer in this CME/MOC/AAPA activity titled “Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable NSCLC: A Case Exploration of New Standards and Emerging Approaches.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/AAPA information, and to apply for credit, please visit us at https://bit.ly/3TxdcP5. CME/MOC/AAPA credit will be available until June 7, 2025.On Target: Understanding the Impact of PSMA for Diagnostic and Therapeutic St...

On Target: Understanding the Impact of PSMA for Diagnostic and Therapeutic St...PVI, PeerView Institute for Medical Education
Chair Oliver Sartor, MD, discusses prostate cancer in this CME activity titled “On Target: Understanding the Impact of PSMA for Diagnostic and Therapeutic Strategies in Prostate Cancer.” For the full presentation, downloadable Practice Aids, and complete CME information, and to apply for credit, please visit us at https://bit.ly/49oY4IJ. CME credit will be available until May 23, 2025.Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Impl...

Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Impl...PVI, PeerView Institute for Medical Education
Chair and Presenters, Neal D. Shore, MD, FACS, Ashish M. Kamat, MD, MBBS, and Joshua J. Meeks, MD, PhD, prepared useful Practice Aids pertaining to bladder cancer for this CME/MOC/NCPD/AAPA/IPCE activity titled “Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Implementing Modern Therapeutic Advances Across the Disease Continuum.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/NCPD/AAPA/IPCE information, and to apply for credit, please visit us at https://bit.ly/3PH0RVQ. CME/MOC/NCPD/AAPA/IPCE credit will be available until June 2, 2025.Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Impl...

Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Impl...PVI, PeerView Institute for Medical Education
Chair and Presenters, Neal D. Shore, MD, FACS, Ashish M. Kamat, MD, MBBS, and Joshua J. Meeks, MD, PhD, discuss bladder cancer in this CME/MOC/NCPD/AAPA/IPCE activity titled “Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Implementing Modern Therapeutic Advances Across the Disease Continuum.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/NCPD/AAPA/IPCE information, and to apply for credit, please visit us at https://bit.ly/3PH0RVQ. CME/MOC/NCPD/AAPA/IPCE credit will be available until June 2, 2025.Striking Back at ALL: Achieving Lasting Benefits with Bispecific Antibodies &...

Striking Back at ALL: Achieving Lasting Benefits with Bispecific Antibodies &...PVI, PeerView Institute for Medical Education
Chair, Nicholas J. Short, MD, discusses acute lymphoblastic leukemia in this CME/NCPD/CPE/AAPA/IPCE activity titled “Striking Back at ALL: Achieving Lasting Benefits with Bispecific Antibodies & MRD-Guided Strategies Across Disease Settings.” For the full presentation, downloadable Practice Aids, and complete CME/NCPD/CPE/AAPA/IPCE information, and to apply for credit, please visit us at https://bit.ly/42QsTDT. CME/NCPD/CPE/AAPA/IPCE credit will be available until May 22, 2025.
Specialty Training for the New Era in Alzheimer’s Disease: Building Skills fo...

Specialty Training for the New Era in Alzheimer’s Disease: Building Skills fo...PVI, PeerView Institute for Medical Education
Chair, Sharon Cohen, MD, FRCPC, prepared useful Practice Aids pertaining to Alzheimer’s disease for this CME/MOC/AAPA activity titled “Specialty Training for the New Era in Alzheimer’s Disease: Building Skills for Making an Early Diagnosis and Implementing Disease-Modifying Treatment.” For the full presentation, downloadable Practice Aids, monograph, and complete CME/MOC/AAPA information, and to apply for credit, please visit us at https://bit.ly/472bp8g. CME/MOC/AAPA credit will be available until May 20, 2025.
Specialty Training for the New Era in Alzheimer’s Disease: Building Skills fo...

Specialty Training for the New Era in Alzheimer’s Disease: Building Skills fo...PVI, PeerView Institute for Medical Education
Chair, Sharon Cohen, MD, FRCPC, discusses Alzheimer’s disease in this CME/MOC/AAPA activity titled “Specialty Training for the New Era in Alzheimer’s Disease: Building Skills for Making an Early Diagnosis and Implementing Disease-Modifying Treatment.” For the full presentation, downloadable Practice Aids, monograph, and complete CME/MOC/AAPA information, and to apply for credit, please visit us at https://bit.ly/472bp8g. CME/MOC/AAPA credit will be available until May 20, 2025.Ten Steps for Highly Successful Myeloma Care: Guidance on the Road to Remissi...

Ten Steps for Highly Successful Myeloma Care: Guidance on the Road to Remissi...PVI, PeerView Institute for Medical Education
Chair and Presenter, Beth Faiman, PhD, MSN, APN-BC, AOCN, BMTCN, FAAN, FAPO, Donna D. Catamero, ANP-BC, OCN, CCRC, and Charise Gleason, MSN, NP-C, AOCNP, discuss multiple myeloma in this CME/MOC/NCPD/ILNA/IPCE activity titled “Ten Steps for Highly Successful Myeloma Care: Guidance on the Road to Remission With Antibodies, BCMA Immunotherapy, and Other Innovations.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/NCPD/ILNA/IPCE information, and to apply for credit, please visit us at https://bit.ly/47mtUnM. CME/MOC/NCPD/ILNA/IPCE credit will be available until May 25, 2025.Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices...

Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices...PVI, PeerView Institute for Medical Education
Co-Chairs and Presenter Marianne Davies, DNP, ACNP, AOCNP, FAAN, Beth Sandy, MSN, CRNP, FAPO, and Matthew A. Gubens, MD, MS, FASCO, prepared useful Practice Aids pertaining to NSCLC for this CME/MOC/NCPD/ILNA/IPCE activity titled “Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices for Patient Education, irAE Management, and Survivorship Care.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/NCPD/ILNA/IPCE information, and to apply for credit, please visit us at https://bit.ly/3RDokbZ. CME/MOC/NCPD/ILNA/IPCE credit will be available until May 24, 2025.Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices...

Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices...PVI, PeerView Institute for Medical Education
Co-Chairs and Presenter Marianne Davies, DNP, ACNP, AOCNP, FAAN, Beth Sandy, MSN, CRNP, FAPO, and Matthew A. Gubens, MD, MS, FASCO, discuss NSCLC in this CME/MOC/NCPD/ILNA/IPCE activity titled “Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices for Patient Education, irAE Management, and Survivorship Care.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/NCPD/ILNA/IPCE information, and to apply for credit, please visit us at https://bit.ly/3RDokbZ. CME/MOC/NCPD/ILNA/IPCE credit will be available until May 24, 2025.Modern Team-Based Therapeutic Management for Bladder Cancer Care: Expert Stra...

Modern Team-Based Therapeutic Management for Bladder Cancer Care: Expert Stra...PVI, PeerView Institute for Medical Education
Co-Chairs, Sia Daneshmand, MD, and Matthew D. Galsky, MD, discuss bladder cancer in this CME/MOC/NCPD/AAPA/IPCE activity titled “Modern Team-Based Therapeutic Management for Bladder Cancer Care: Expert Strategies for Integrating the Latest Evidence and Treatment Advances.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/NCPD/AAPA/IPCE information, and to apply for credit, please visit us at https://bit.ly/3OOeYbO. CME/MOC/NCPD/AAPA/IPCE credit will be available until May 13, 2025.Nurses at the Forefront of Maximizing the Potential of TROP2-Targeted Therapy...

Nurses at the Forefront of Maximizing the Potential of TROP2-Targeted Therapy...PVI, PeerView Institute for Medical Education
Chair Jamie Carroll, APRN, CNP, MSN, discusses breast cancer in this NCPD/ILNA/AAPA activity titled “Nurses at the Forefront of Maximizing the Potential of TROP2-Targeted Therapy in TNBC and HR+, HER2- Breast Cancer: Best Practices for Adverse Event Management and Patient Education.” For the full presentation, downloadable Practice Aids, and complete NCPD/ILNA/AAPA information, and to apply for credit, please visit us at https://bit.ly/3SdnvWt. NCPD/ILNA/AAPA credit will be available until May 8, 2025.BTK Inhibition Transforming the Landscape of Chronic Spontaneous Urticaria Tr...

BTK Inhibition Transforming the Landscape of Chronic Spontaneous Urticaria Tr...PVI, PeerView Institute for Medical Education
Chair Jonathan A. Bernstein, MD, discusses chronic spontaneous urticaria in this CME activity titled “BTK Inhibition Transforming the Landscape of Chronic Spontaneous Urticaria Treatment.” For the full presentation, downloadable Practice Aids, and complete CME information, and to apply for credit, please visit us at https://bit.ly/3P0cnvi. CME credit will be available until May 6, 2025.More from PVI, PeerView Institute for Medical Education (20)
Establishing the Collaborative Benchmark for HCC Care: Critical Discussions B...

Establishing the Collaborative Benchmark for HCC Care: Critical Discussions B...
Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...

Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...
Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...

Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...
Applying Advances in PET Imaging to Facilitate the Early Diagnosis of Alzheim...

Applying Advances in PET Imaging to Facilitate the Early Diagnosis of Alzheim...
A Pharmacist’s Take on Navigating the Expanding Therapeutic Landscape for End...

A Pharmacist’s Take on Navigating the Expanding Therapeutic Landscape for End...
“Four-Ward” Progress in NDMM: New Developments With CD38 Antibody Quadruplets

“Four-Ward” Progress in NDMM: New Developments With CD38 Antibody Quadruplets
Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable N...

Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable N...
Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable N...

Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable N...
On Target: Understanding the Impact of PSMA for Diagnostic and Therapeutic St...

On Target: Understanding the Impact of PSMA for Diagnostic and Therapeutic St...
Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Impl...

Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Impl...
Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Impl...

Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Impl...
Striking Back at ALL: Achieving Lasting Benefits with Bispecific Antibodies &...

Striking Back at ALL: Achieving Lasting Benefits with Bispecific Antibodies &...
Specialty Training for the New Era in Alzheimer’s Disease: Building Skills fo...

Specialty Training for the New Era in Alzheimer’s Disease: Building Skills fo...
Specialty Training for the New Era in Alzheimer’s Disease: Building Skills fo...

Specialty Training for the New Era in Alzheimer’s Disease: Building Skills fo...
Ten Steps for Highly Successful Myeloma Care: Guidance on the Road to Remissi...

Ten Steps for Highly Successful Myeloma Care: Guidance on the Road to Remissi...
Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices...

Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices...
Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices...

Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices...
Modern Team-Based Therapeutic Management for Bladder Cancer Care: Expert Stra...

Modern Team-Based Therapeutic Management for Bladder Cancer Care: Expert Stra...
Nurses at the Forefront of Maximizing the Potential of TROP2-Targeted Therapy...

Nurses at the Forefront of Maximizing the Potential of TROP2-Targeted Therapy...
BTK Inhibition Transforming the Landscape of Chronic Spontaneous Urticaria Tr...

BTK Inhibition Transforming the Landscape of Chronic Spontaneous Urticaria Tr...
Recently uploaded
ANATOMY AND PHYSIOLOGY OF URINARY SYSTEM.pptx

Valuable Content of Human Anatomy and Physiology of Urinary system as per PCI Syllabus for Pharmacy and PharmD Students.
Physiology of Special Chemical Sensation of Taste

Title: Sense of Taste
Presenter: Dr. Faiza, Assistant Professor of Physiology
Qualifications:
MBBS (Best Graduate, AIMC Lahore)
FCPS Physiology
ICMT, CHPE, DHPE (STMU)
MPH (GC University, Faisalabad)
MBA (Virtual University of Pakistan)
Learning Objectives:
Describe the structure and function of taste buds.
Describe the relationship between the taste threshold and taste index of common substances.
Explain the chemical basis and signal transduction of taste perception for each type of primary taste sensation.
Recognize different abnormalities of taste perception and their causes.
Key Topics:
Significance of Taste Sensation:
Differentiation between pleasant and harmful food
Influence on behavior
Selection of food based on metabolic needs
Receptors of Taste:
Taste buds on the tongue
Influence of sense of smell, texture of food, and pain stimulation (e.g., by pepper)
Primary and Secondary Taste Sensations:
Primary taste sensations: Sweet, Sour, Salty, Bitter, Umami
Chemical basis and signal transduction mechanisms for each taste
Taste Threshold and Index:
Taste threshold values for Sweet (sucrose), Salty (NaCl), Sour (HCl), and Bitter (Quinine)
Taste index relationship: Inversely proportional to taste threshold
Taste Blindness:
Inability to taste certain substances, particularly thiourea compounds
Example: Phenylthiocarbamide
Structure and Function of Taste Buds:
Composition: Epithelial cells, Sustentacular/Supporting cells, Taste cells, Basal cells
Features: Taste pores, Taste hairs/microvilli, and Taste nerve fibers
Location of Taste Buds:
Found in papillae of the tongue (Fungiform, Circumvallate, Foliate)
Also present on the palate, tonsillar pillars, epiglottis, and proximal esophagus
Mechanism of Taste Stimulation:
Interaction of taste substances with receptors on microvilli
Signal transduction pathways for Umami, Sweet, Bitter, Sour, and Salty tastes
Taste Sensitivity and Adaptation:
Decrease in sensitivity with age
Rapid adaptation of taste sensation
Role of Saliva in Taste:
Dissolution of tastants to reach receptors
Washing away the stimulus
Taste Preferences and Aversions:
Mechanisms behind taste preference and aversion
Influence of receptors and neural pathways
Impact of Sensory Nerve Damage:
Degeneration of taste buds if the sensory nerve fiber is cut
Abnormalities of Taste Detection:
Conditions: Ageusia, Hypogeusia, Dysgeusia (parageusia)
Causes: Nerve damage, neurological disorders, infections, poor oral hygiene, adverse drug effects, deficiencies, aging, tobacco use, altered neurotransmitter levels
Neurotransmitters and Taste Threshold:
Effects of serotonin (5-HT) and norepinephrine (NE) on taste sensitivity
Supertasters:
25% of the population with heightened sensitivity to taste, especially bitterness
Increased number of fungiform papillae
The Normal Electrocardiogram - Part I of II

These lecture slides, by Dr Sidra Arshad, offer a quick overview of physiological basis of a normal electrocardiogram.
Learning objectives:
1. Define an electrocardiogram (ECG) and electrocardiography
2. Describe how dipoles generated by the heart produce the waveforms of the ECG
3. Describe the components of a normal electrocardiogram of a typical bipolar leads (limb II)
4. Differentiate between intervals and segments
5. Enlist some common indications for obtaining an ECG
Study Resources:
1. Chapter 11, Guyton and Hall Textbook of Medical Physiology, 14th edition
2. Chapter 9, Human Physiology - From Cells to Systems, Lauralee Sherwood, 9th edition
3. Chapter 29, Ganong’s Review of Medical Physiology, 26th edition
4. Electrocardiogram, StatPearls - https://www.ncbi.nlm.nih.gov/books/NBK549803/
5. ECG in Medical Practice by ABM Abdullah, 4th edition
6. ECG Basics, http://www.nataliescasebook.com/tag/e-c-g-basics
For Better Surat #ℂall #Girl Service ❤85270-49040❤ Surat #ℂall #Girls

For Better Surat #ℂall #Girl Service ❤85270-49040❤ Surat #ℂall #Girls
Ozempic: Preoperative Management of Patients on GLP-1 Receptor Agonists 

Preoperative Management of Patients on GLP-1 Receptor Agonists like Ozempic and Semiglutide
ASA GUIDELINE
NYSORA Guideline
2 Case Reports of Gastric Ultrasound
micro teaching on communication m.sc nursing.pdf

Microteaching is a unique model of practice teaching. It is a viable instrument for the. desired change in the teaching behavior or the behavior potential which, in specified types of real. classroom situations, tends to facilitate the achievement of specified types of objectives.
ARTIFICIAL INTELLIGENCE IN HEALTHCARE.pdf

Artificial intelligence (AI) refers to the simulation of human intelligence processes by machines, especially computer systems. It encompasses tasks such as learning, reasoning, problem-solving, perception, and language understanding. AI technologies are revolutionizing various fields, from healthcare to finance, by enabling machines to perform tasks that typically require human intelligence.
Ocular injury ppt Upendra pal optometrist upums saifai etawah

This ppt are composed by upendra pal to provide help future optometrist of india
Physiology of Chemical Sensation of smell.pdf

Title: Sense of Smell
Presenter: Dr. Faiza, Assistant Professor of Physiology
Qualifications:
MBBS (Best Graduate, AIMC Lahore)
FCPS Physiology
ICMT, CHPE, DHPE (STMU)
MPH (GC University, Faisalabad)
MBA (Virtual University of Pakistan)
Learning Objectives:
Describe the primary categories of smells and the concept of odor blindness.
Explain the structure and location of the olfactory membrane and mucosa, including the types and roles of cells involved in olfaction.
Describe the pathway and mechanisms of olfactory signal transmission from the olfactory receptors to the brain.
Illustrate the biochemical cascade triggered by odorant binding to olfactory receptors, including the role of G-proteins and second messengers in generating an action potential.
Identify different types of olfactory disorders such as anosmia, hyposmia, hyperosmia, and dysosmia, including their potential causes.
Key Topics:
Olfactory Genes:
3% of the human genome accounts for olfactory genes.
400 genes for odorant receptors.
Olfactory Membrane:
Located in the superior part of the nasal cavity.
Medially: Folds downward along the superior septum.
Laterally: Folds over the superior turbinate and upper surface of the middle turbinate.
Total surface area: 5-10 square centimeters.
Olfactory Mucosa:
Olfactory Cells: Bipolar nerve cells derived from the CNS (100 million), with 4-25 olfactory cilia per cell.
Sustentacular Cells: Produce mucus and maintain ionic and molecular environment.
Basal Cells: Replace worn-out olfactory cells with an average lifespan of 1-2 months.
Bowman’s Gland: Secretes mucus.
Stimulation of Olfactory Cells:
Odorant dissolves in mucus and attaches to receptors on olfactory cilia.
Involves a cascade effect through G-proteins and second messengers, leading to depolarization and action potential generation in the olfactory nerve.
Quality of a Good Odorant:
Small (3-20 Carbon atoms), volatile, water-soluble, and lipid-soluble.
Facilitated by odorant-binding proteins in mucus.
Membrane Potential and Action Potential:
Resting membrane potential: -55mV.
Action potential frequency in the olfactory nerve increases with odorant strength.
Adaptation Towards the Sense of Smell:
Rapid adaptation within the first second, with further slow adaptation.
Psychological adaptation greater than receptor adaptation, involving feedback inhibition from the central nervous system.
Primary Sensations of Smell:
Camphoraceous, Musky, Floral, Pepperminty, Ethereal, Pungent, Putrid.
Odor Detection Threshold:
Examples: Hydrogen sulfide (0.0005 ppm), Methyl-mercaptan (0.002 ppm).
Some toxic substances are odorless at lethal concentrations.
Characteristics of Smell:
Odor blindness for single substances due to lack of appropriate receptor protein.
Behavioral and emotional influences of smell.
Transmission of Olfactory Signals:
From olfactory cells to glomeruli in the olfactory bulb, involving lateral inhibition.
Primitive, less old, and new olfactory systems with different path
Non-respiratory Functions of the Lungs.pdf

These simplified slides by Dr. Sidra Arshad present an overview of the non-respiratory functions of the respiratory tract.
Learning objectives:
1. Enlist the non-respiratory functions of the respiratory tract
2. Briefly explain how these functions are carried out
3. Discuss the significance of dead space
4. Differentiate between minute ventilation and alveolar ventilation
5. Describe the cough and sneeze reflexes
Study Resources:
1. Chapter 39, Guyton and Hall Textbook of Medical Physiology, 14th edition
2. Chapter 34, Ganong’s Review of Medical Physiology, 26th edition
3. Chapter 17, Human Physiology by Lauralee Sherwood, 9th edition
4. Non-respiratory functions of the lungs https://academic.oup.com/bjaed/article/13/3/98/278874
263778731218 Abortion Clinic /Pills In Harare ,

263778731218 Abortion Clinic /Pills In Harare ,ABORTION WOMEN’S CLINIC +27730423979 IN women clinic we believe that every woman should be able to make choices in her pregnancy. Our job is to provide compassionate care, safety,affordable and confidential services. That’s why we have won the trust from all generations of women all over the world. we use non surgical method(Abortion pills) to terminate…Dr.LISA +27730423979women Clinic is committed to providing the highest quality of obstetrical and gynecological care to women of all ages. Our dedicated staff aim to treat each patient and her health concerns with compassion and respect.Our dedicated group ABORTION WOMEN’S CLINIC +27730423979 IN women clinic we believe that every woman should be able to make choices in her pregnancy. Our job is to provide compassionate care, safety,affordable and confidential services. That’s why we have won the trust from all generations of women all over the world. we use non surgical method(Abortion pills) to terminate…Dr.LISA +27730423979women Clinic is committed to providing the highest quality of obstetrical and gynecological care to women of all ages. Our dedicated staff aim to treat each patient and her health concerns with compassion and respect.Our dedicated group of receptionists, nurses, and physicians have worked together as a teamof receptionists, nurses, and physicians have worked together as a team wwww.lisywomensclinic.co.za/
NVBDCP.pptx Nation vector borne disease control program

NVBDCP was launched in 2003-2004 . Vector-Borne Disease: Disease that results from an infection transmitted to humans and other animals by blood-feeding arthropods, such as mosquitoes, ticks, and fleas. Examples of vector-borne diseases include Dengue fever, West Nile Virus, Lyme disease, and malaria.
Prix Galien International 2024 Forum Program

June 20, 2024, Prix Galien International and Jerusalem Ethics Forum in ROME. Detailed agenda including panels:
- ADVANCES IN CARDIOLOGY: A NEW PARADIGM IS COMING
- WOMEN’S HEALTH: FERTILITY PRESERVATION
- WHAT’S NEW IN THE TREATMENT OF INFECTIOUS,
ONCOLOGICAL AND INFLAMMATORY SKIN DISEASES?
- ARTIFICIAL INTELLIGENCE AND ETHICS
- GENE THERAPY
- BEYOND BORDERS: GLOBAL INITIATIVES FOR DEMOCRATIZING LIFE SCIENCE TECHNOLOGIES AND PROMOTING ACCESS TO HEALTHCARE
- ETHICAL CHALLENGES IN LIFE SCIENCES
- Prix Galien International Awards Ceremony
Report Back from SGO 2024: What’s the Latest in Cervical Cancer?

Are you curious about what’s new in cervical cancer research or unsure what the findings mean? Join Dr. Emily Ko, a gynecologic oncologist at Penn Medicine, to learn about the latest updates from the Society of Gynecologic Oncology (SGO) 2024 Annual Meeting on Women’s Cancer. Dr. Ko will discuss what the research presented at the conference means for you and answer your questions about the new developments.
KDIGO 2024 guidelines for diabetologists

KDIGO guidelines 2024 for evaluation and management of CKD, related to diabetes and management of diabetic kidney disease
How STIs Influence the Development of Pelvic Inflammatory Disease.pptx

STIs may cause PID. For the both disease, herbal medicine Fuyan Pill can be a solution.
Recently uploaded (20)
For Better Surat #ℂall #Girl Service ❤85270-49040❤ Surat #ℂall #Girls

For Better Surat #ℂall #Girl Service ❤85270-49040❤ Surat #ℂall #Girls
Maxilla, Mandible & Hyoid Bone & Clinical Correlations by Dr. RIG.pptx

Maxilla, Mandible & Hyoid Bone & Clinical Correlations by Dr. RIG.pptx
Ozempic: Preoperative Management of Patients on GLP-1 Receptor Agonists 

Ozempic: Preoperative Management of Patients on GLP-1 Receptor Agonists
Ocular injury ppt Upendra pal optometrist upums saifai etawah

Ocular injury ppt Upendra pal optometrist upums saifai etawah
NVBDCP.pptx Nation vector borne disease control program

NVBDCP.pptx Nation vector borne disease control program
Report Back from SGO 2024: What’s the Latest in Cervical Cancer?

Report Back from SGO 2024: What’s the Latest in Cervical Cancer?
How STIs Influence the Development of Pelvic Inflammatory Disease.pptx

How STIs Influence the Development of Pelvic Inflammatory Disease.pptx
New Options, Emerging Combinations in Advanced Hepatocellular Carcinoma: Are Management Approaches Poised For Transformation?
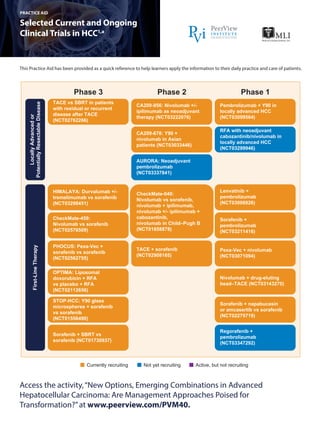
- 1. Selected Current and Ongoing Clinical Trials in HCC1,a PRACTICE AID This Practice Aid has been provided as a quick reference to help learners apply the information to their daily practice and care of patients. Access the activity,“New Options, Emerging Combinations in Advanced Hepatocellular Carcinoma: Are Management Approaches Poised for Transformation?”at www.peerview.com/PVM40. LocallyAdvancedor PotentiallyResectableDisease Phase 3 Phase 2 Phase 1 TACE vs SBRT in patients with residual or recurrent disease after TACE (NCT02762266) CA209-956: Nivolumab +/- ipilimumab as neoadjuvant therapy (NCT03222076) Pembrolizumab + Y90 in locally advanced HCC (NCT03099564) CA209-678: Y90 + nivolumab in Asian patients (NCT03033446) AURORA: Neoadjuvant pembrolizumab (NCT03337841) RFA with neoadjuvant cabozantinib/nivolumab in locally advanced HCC (NCT03299946) First-LineTherapy HIMALAYA: Durvalumab +/- tremelimumab vs sorafenib (NCT03298451) CheckMate-040: Nivolumab vs sorafenib, nivolumab + ipilimumab, nivolumab +/- ipilimumab + cabozantinib, nivolumab in Child–Pugh B (NCT01658878) Lenvatinib + pembrolizumab (NCT03006926) TACE + sorafenib (NCT02908165) CheckMate-459: Nivolumab vs sorafenib (NCT02576509) PHOCUS: Pexa-Vec + sorafenib vs sorafenib (NCT02562755) OPTIMA: Liposomal doxorubicin + RFA vs placebo + RFA (NCT02112656) STOP-HCC: Y90 glass microspheres + sorafenib vs sorafenib (NCT01556490) Sorafenib + SBRT vs sorafenib (NCT01730937) Sorafenib + pembrolizumab (NCT03211416) Pexa-Vec + nivolumab (NCT03071094) Nivolumab + drug-eluting bead–TACE (NCT03143270) Sorafenib + napabucasin or amcasertib vs sorafenib (NCT02279719) Regorafenib + pembrolizumab (NCT03347292) Currently recruiting Not yet recruiting Active, but not recruiting
- 2. Access the activity,“New Options, Emerging Combinations in Advanced Hepatocellular Carcinoma: Are Management Approaches Poised for Transformation?”at www.peerview.com/PVM40. Selected Current and Ongoing Clinical Trials in HCC1,a PRACTICE AID AFP: alpha-fetoprotein; BSC: best supportive care; HCC: hepatocellular carcinoma; HSP90: heat-shock protein 90; IDO: indoleamine 2,3-dioxygenase; RFA: radiofrequency ablation; SBRT: stereotactic body radiation therapy; TACE: transarterial chemoembolization; Y90: yttrium 90. 1. www.clinicaltrials.gov. Accessed December 21, 2017. a Recruitment status as of December 12, 2017. Second-LineTherapyorBeyond Phase 3 Phase 2 Phase 1 KEYNOTE-394: Pembrolizumab vs placebo in Asian patients (NCT03062358) TATE-PD-1: Transarterial tirapazamine embolization + PD-1 inhibitor (NCT03259867) SBRT followed by nivolumab +/- ipilimumab in unresectable HCC (NCT03203304) Tumor infiltrating lymphocytes + pembrolizumab (NCT01174121) Pembrolizumab monotherapy (NCT02658019) Durvalumab + tremelimumab with TACE, RFA, or cryotherapy (NCT02821754) Currently recruiting Not yet recruiting Active, but not recruiting Durvalumab, tremelimumab, or in combination (NCT02519348) Y90 glass microspheres + nivolumab in patients with no prior therapies (NCT02837029) KEYNOTE-037: Pembrolizumab + epacadostat [IDO inhibitor] (NCT02178722) Pembrolizumab + XL888 [HSP90 inhibitor] (NCT03095781) REACH-2: Ramucirumab vs placebo in patients with elevated AFP (NCT02435433) KEYNOTE-240: Pembrolizumab vs BSC (NCT02702401)
- 3. Immuno-Oncology in the Clinic: General Guidelines for Recognizing and Managing Immune-Mediated Adverse Reactions1-4 PRACTICE AID This Practice Aid has been provided as a quick reference to help learners apply the information to their daily practice and care of patients. Access the activity,“New Options, Emerging Combinations in Advanced Hepatocellular Carcinoma: Are Management Approaches Poised for Transformation?”at www.peerview.com/PVM40. How Do Checkpoint Inhibitors Work? Blocking negative regulatory signals activates the immune system Immune-Mediated Adverse Reactions More Common Pulmonary (pneumonitis) Dermatologic (rash, pruritus, blisters, ulcers, vitiligo) Gastrointestinal (diarrhea, enterocolitis, transaminitis, hepatitis, pancreatitis) Endocrine (thyroiditis, hypophysitis, adrenal insufficiency) Less Common Hematologic, cardiovascular, ocular, renal Lymphoid Tissue Anti–CTLA-4 antibodies Cytotoxic T cell Dendritic cell CD28 B7 B7 CTLA-4 Tumor Microenvironment Anti–PD-L1 antibodies Anti–PD-1 antibodies PD-L1 Tumor PD-1
- 4. Access the activity,“New Options, Emerging Combinations in Advanced Hepatocellular Carcinoma: Are Management Approaches Poised for Transformation?”at www.peerview.com/PVM40. Immuno-Oncology in the Clinic: General Guidelines for Recognizing and Managing Immune-Mediated Adverse Reactions1-4 PRACTICE AID CD: cluster of differentiation; CTLA-4: cytotoxic T-lymphocyte-associated protein 4; IMARs: immune-mediated adverse reactions; PD-1: programmed cell-death protein 1; PD-L1: programmed death-ligand 1. 1. Postow MA et al. http://www.uptodate.com/contents/toxicities-associated-with-checkpoint-inhibitor-immunotherapy. Accessed December 21, 2017. 2. Weber JS et al. J Clin Oncol. 2015;33:2092-2099. 3. Weber JS et al. Oncologist. 2016;21:1230-1240. 4. Puzanov I et al. J Immunother Cancer. 2017;5:95. IMARs: General Guidance for Diagnosis and Treatment IMARs: General Management Principles IMARs often diagnosed by exclusion; other causes should be ruled out, including AEs of other therapies used, but immunotherapy-related toxicity should always be included in the differential Management may require: • Corticosteroid or other immunosuppressive treatment • Interruption or discontinuation of therapy If appropriate, immunosuppressive treatment is used, and patients generally recover from IMARs Use of immunosuppressive therapy to manage IMARs does not impact response to immunotherapy Keys to Success Early recognition, evaluation, and treatment of IMARs plus patient education are essential for best outcomes If no improvement or progression, additional immunosuppressant treatment may be needed; if >4 wk of immunosuppressants needed, administer antimicrobial/antifungal prophylaxis to prevent opportunistic infections q Continue immunotherapy (or consider temporary delay) q Symptomatic therapy q Withhold immunotherapy q Corticosteroids, if symptoms do not resolve in 1 week (prednisone 0.5-1 mg/kg/d or equivalent) q Taper corticosteroids over ≥1 month to reduce recurrence q Re-dose if toxicity resolves to grade ≤1 q Discontinue immunotherapy q Hospitalization and multidisciplinary evaluation q High-dose corticosteroids (prednisone 1-2 mg/kg/d or equivalent) q Taper high-dose corticosteroids over ≥1 month until toxicity resolves to grade ≤1 Grade 1 (Minimal or no symptoms; diagnostic changes only) Grade 2 (Mild to moderate symptoms) Grade 3/4 (Severe or life-threatening symptoms)
- 5. A Guide to Management of Adverse Events Associated With Tyrosine Kinase Inhibitors PRACTICE AID This Practice Aid has been provided as a quick reference to help learners apply the information to their daily practice and care of patients. Access the activity,“New Options, Emerging Combinations in Advanced Hepatocellular Carcinoma: Are Management Approaches Poised for Transformation?”at www.peerview.com/PVM40. Diarrhea1,2 HFSR (alternative names: hand–foot syndrome, palmar–plantar erythrodysesthesia, acral erythema) is an acute-onset symptom complex Incidence of HFSR (all grades) with sorafenib in patients with hepatocellular carcinoma was 21% in the SHARP trial3 ; incidence of HFSR with regorafenib was 12.6% in the RESORCE trial4 Appropriate methods of prophylaxis and management of HFSR are necessary to ensure proper administration of the drugs and to improve the health-related QOL of patients Symptoms • Frequent, watery, bloody, or nocturnal stools General management • Monitor bowel habits and report any increase in activity above normal • Avoid spicy or fatty foods; plain, simple foods are best • Avoid fruit and caffeine • Maintain adequate fluid intake to avoid dehydration • Monitor/manage electrolytes Medical interventions • Loperamide is usually effective • If loperamide is ineffective, consider diphenoxylate/atropine Patient education • Direct patient to notify medical team of diarrhea or abdominal distress Maintain activity • Stay as active as possible, because that will help regulate sleep Establish routine • Maintain normal work and social schedule Take breaks • Take breaks as needed Always communicate • Tell your medical team if activity is intolerable or fatigue worsens Hand–Foot Skin Reaction Fatigue1,2
- 6. Access the activity,“New Options, Emerging Combinations in Advanced Hepatocellular Carcinoma: Are Management Approaches Poised for Transformation?”at www.peerview.com/PVM40. A Guide to Management of Adverse Events Associated With Tyrosine Kinase Inhibitors PRACTICE AID HFSR: hand–foot skin reaction; QOL: quality of life. Photos provided courtesy of Elizabeth Manchen, RN, MS, OCN. 1. Brose MS et al. Semin Oncol. 2014;41:S1-S16. 2. Walko CM et al. Semin Oncol. 2014;41:S17-S28. 3. Llovet JM et al. N Engl J Med. 2008;24:359-390. 4. Bruix J et al. Lancet. 2017;389:56-66. 5. https://ctep.cancer.gov/protocolDevelopment/electronic_applications/ctc.htm#ctc_v40. Accessed December 21, 2017. 6. Lacouture ME et al. Oncologist. 2008;13:1001-1011. 7. McLellannB et al. Ann Oncol. 2015;26:2017-2026. Grade 1 General tips: • Educate patients about HFSR, engage them in the monitoring and treatment plan • Encourage patients to report possible symptoms early, to take digital photos of their hands and feet, and to email them to the treatment team regularly to monitor for development and progression of HFSR Hand–Foot Skin Reaction (Cont'd)4-7 Grade 2 Grade 3 Symptoms Tingling, numbness, accompanied by minimal skin changes or dermatitis, such as erythema, edema, or hyperkeratosis of the hands and/or feet without pain; does not disrupt normal activities Symptoms Skin changes of the hands and/or feet may include peeling, blisters, bleeding, edema, or hyperkeratosis with pain; discomfort affecting the patient's normal activities Symptoms Severe skin changes of the hands and/or feet may include peeling, blisters, bleeding, edema, or hyperkeratosis with pain and/or severe discomfort that causes the patient to be unable to work or perform activities of daily living Management Avoid hot water Wear thick socks Wear cotton gloves/socks at night Use moisturizing creams Use keratolytics (urea 20% to 40%; salicylic acid 5% to 10%) No dose reduction needed Follow up within 2 weeks Management Employ grade 1 strategies Consider clobetasol 0.05% ointment twice daily for erythematous areas Use topical analgesic Use systemic analgesics if no contraindications (bleeding or kidney dysfunction) Consider 50% dose reduction for 7-28 days until HFSR is grade 1/0 → full dose Management Employ grade 1/2 strategies Treatment interruption for ≥7 days until HFSR is grade 1/0 → 50% of full dose → escalation if possible Resume treatment at lower dose as recommended in package insert Dose may be escalated if reaction does not reoccur
