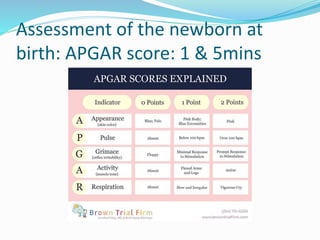
This document outlines the key steps in neonatal resuscitation for newborns requiring assistance to begin breathing or transition to life outside the womb. It discusses factors that may increase the need for resuscitation, important equipment, assessing the newborn using the APGAR score, and the steps of providing warmth, clearing the airway, breathing support, and circulation support like chest compressions and medications if needed. Effective resuscitation in the critical first minute after birth can prevent many newborn deaths from asphyxia globally each year.