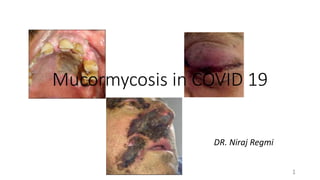
Mucormycosis
- 1. Mucormycosis in COVID 19 1 DR. Niraj Regmi
- 2. Contents • Introduction • Clinical manifestation • Radiographic manifestation • Methods of diagnosis • Management 2
- 3. Introduction • Coronavirus disease 2019 (COVID-19) caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has been associated with a wide range of opportunistic bacterial and fungal infections like aspergillosis and candidiasis, • Recently, several cases of mucormycosis in people with COVID19 have been increasingly reported world-wide, in particular from India • The Ministry of Health and Population of Nepal has confirmed 10 instances of black fungus infection or mucormycosis in the country till dated 3rd June 3
- 4. • On 4th June 65-year-old man was reported dead and was being treated at the intensive care unit at a hospital in western Nepal after being diagnosed with temporal lobe encephalitis. • "He died on 3 June 2021... after a nasal swab test showed fungal hyphae and a biopsy test of nose and lips showed mucor," said a statement by the Seti Provincial Hospital on 4th June 2021. • The man had however tested negative for coronavirus according to the official statement 4
- 5. • Mucormycosis is an uncommon but a fatal fungal infection that usually affects patients with altered immunity • Mucormycosis is an angioinvasive disease caused by mold fungi of the genus Rhizopus, Mucor, Rhizomucor, Cunninghamella and Absidia of Order- Mucorales, Class- Zygomycetes • It is worldwide in distribution and the organisms normally occur in soil, manure, fruits, and in decaying matter • The Rhizopus Oryzae is the most common type and responsible for nearly 60% of mucormycosis cases in humans and also accounts for 90% of the Rhino-orbital-cerebral (ROCM) form. 5 Eucker J, Sezer O, Graf B, Possinger K. Mucormycoses. Mycoses. 2001 Oct;44(7‐8):253-60.
- 6. • These organisms are present in the nasal passages and oral cavities of normal persons. 6 Branscomb R. An overview of mucormycosis. Laboratory Medicine. 2002 Jun 1;33(6):453-5.
- 7. 7 Singh AK, Singh R, Joshi SR, Misra A. Mucormycosis in COVID-19: a systematic review of cases reported worldwide and in India. Diabetes & Metabolic Syndrome: Clinical Research & Reviews. 2021 May 21.
- 8. Association • DM has been the most common risk factor linked with mucormycosis in India, although hematological malignancies and organ transplant takes the lead in Europe and the USA • a secondary occurrence in cancer patients, especially those with any of the malignant lymphomas and in patients having renal failure, organ transplant, AIDS, and cirrhosis • Immunosuppressed patients are prone to develop this infection as well as patients with burns or open wounds. • A cumulative prednisone dose of greater than 600 mg or a total methyl prednisone dose of 2-7 g given during the month before, predisposes immunocompromised people to mucormycosis • There are few case reports of mucormycosis resulting from even a short course (5–14 days) of steroid therapy, especially in people with DM 8 Lionakis MS, Kontoyiannis DP. Glucocorticoids and invasive fungal infections. Lancet 2003, 362, 1828–1838. Hoang K, Abdo T, Reinersman JM, Lu R, Higuita NIA. A case of invasive pulmonary mucormycosis resulting from short courses of corticosteroids in a wellcontrolled diabetic patient. Med Mycol Case Rep. 2020;29(1):22-24.
- 9. • There has been a steep rise in case reports/series of mucormycosis in people with COVID-19 especially in India • Among 101 cases of mucormycosis in patients with COVID-19 have been reported of which 82 cases belong to India. • Diabetes was present in 80% of cases, while corticosteroid treatment was given for COVID-19 in 76.3% cases. 9 Singh AK, Singh R, Joshi SR, Misra A. Mucormycosis in COVID-19: a systematic review of cases reported worldwide and in India. Diabetes & Metabolic Syndrome: Clinical Research & Reviews. 2021 May 21.
- 10. 10
- 11. Risk factors 1.COVID-19 infection (Active or Post COVID) 2. Steroid therapy: High dose and early initiation of therapy in treatment of COVID 3. Uncontrolled Diabetes 4. Irrational use of broad-spectrum antibiotics 5. Chronic Kidney Disease 6. Immunodeficiency conditions: Neutropenia, hematological malignancies, stem cell transplants, and organ transplant patients on immunosuppressants. 7. Elevated free iron levels 8. Inappropriate use of immunosuppressants like Tocilizumab 9. Living in dusty and damp area, stagnant area without proper ventilation 10.Dehydration 11
- 12. PRESENTATION • Any age or sex but commonly middle-aged people • Usually 2-4 weeks of COVID-19 symptom onset. • However, can appear at 10- 60 days or during active COVID infection 12
- 13. 13
- 14. In COVID 19 patients • Mucorales spores to germinate in people with COVID-19 is an ideal environment of low oxygen (hypoxia), high glucose (diabetes, new- onset hyperglycemia, steroid-induced hyperglycemia), acidic medium (metabolic acidosis, diabetic ketoacidosis [DKA]), high iron levels (increased ferritins) and decreased phagocytic activity of white blood cells (WBC) due to immunosuppression (SARS-CoV-2 mediated, steroid-mediated or background comorbidities) coupled with several other shared risk factors including prolonged hospitalization with or without mechanical ventilators. 14 Singh AK, Singh R, Joshi SR, Misra A. Mucormycosis in COVID-19: a systematic review of cases reported worldwide and in India. Diabetes & Metabolic Syndrome: Clinical Research & Reviews. 2021 May 21.
- 15. Types • 1) superficial and (2) visceral, although it is sometimes also classified as localized and disseminated. • The superficial infection(cutaneous) includes involvement of the external ear, the fingernails, and the skin. • The visceral forms of phycomycosis are of three main types: (a) pulmonary, (b) gastrointestinal, and (c) rhinocerebral 15
- 16. 16 Skiada A, Lass-Floerl C, Klimko N, Ibrahim A, Roilides E, Petrikkos G. Challenges in the diagnosis and treatment of mucormycosis. Medical mycology. 2018 Apr 1;56(suppl_1):S93-101.
- 17. SYMPTOMS AND SIGN (A)Rhino-orbito-cerebral Mucormycosis Common Early Symptoms Unilateral facial pain; Focal in cheek, retro- orbital pain Swelling, redness around the eyes and nose: progressive anesthesia felt over cheek region or nasal mucosa Nasal congestion Bloody/black nasal discharge Blurring of vision, double vision Fever, malaise Dental pain or loosening of teeth 17
- 18. Symptoms in later stage : Facial swelling Ptosis (closure of eyelids) Proptosis (swelling of the eyeballs) Diplopia, Restricted eye movements Chemosis Facial skin discolouration Palatal blackish discolouration or ulcer Other neurological symptoms, Seizure, altered sensorium , Hemiplegia (Contralateral) 18
- 19. 19 Cornely OA, Alastruey-Izquierdo A, Arenz D, Chen SC, Dannaoui E, Hochhegger B, Hoenigl M, Jensen HE, Lagrou K, Lewis RE, Mellinghoff SC. Global guideline for the diagnosis and management of mucormycosis: an initiative of the European Confederation of Medical Mycology in cooperation with the Mycoses Study Group Education and Research Consortium. The Lancet infectious diseases. 2019 Dec 1;19(12):e405-21.
- 20. (B) Pulmonary mucormycosis Refractory fever non-productive cough, progressive dyspnea, pleuritic chest pain. 20
- 21. (C) Gastro-intestinal mucormycosis Fever, Bleeding per rectum, mass like lesion, perforation (late stage) 21
- 22. (D) Cutaneous and soft tissue Erythema, induration, then black eschar, muscle pain with deeper involvement 22
- 23. (E) Disseminated mucormycosis: Symptoms vary as per site of involvement, mostly associated with pneumonia 23 . Sugar AM. Mucormycosis. Clin Infect Dis 1992;14:S126-9
- 24. • Infections of the head by these organisms are characterized by the classical syndrome of uncontrolled diabetes, cellulitis, ophthalmoplegia and meningoencephalitis. • The infection apparently enters the tissues through the nasal mucosa and extends to the paranasal sinuses, pharynx, palate, orbit, and brain • One early clinical manifestation of the disease is the appearance of a reddish-black nasal turbinate and septum with a nasal discharge. • The necrosis may extend to the paranasal sinuses and orbital cavity, with the development of sinus tracts and sloughing of tissue. 24
- 25. • Cases of Mucormycosi involving the maxillary sinus may present clinically as a mass in the maxilla, resembling carcinoma of the antrum, and radiographs may support the latter diagnosis • Involvement may occur at any age, cases having been reported in infants as well as adults. 25
- 26. Suspect • Sinusitis: nasal blockade or congestion, nasal discharge (blackish/bloody), local pain on cheek bone. • One sided facial pain, numbness or swelling. • Blackish discoloration over bridge of nose or palate. • Toothache, loosening of teeth, jaw involvement, swollen gums • Blurred or double vision with pain; fever, skin lesion; ptosis; thrombosis and necrosis (eschar) or loss of vision (early or late feature) • Chest pain, pleural effusion, hemoptysis, worsening of respiratory symptoms. • Seizures, stroke – in cases of cerebral involvement 26
- 27. Warning signs • Pain and redness around eyes and/or nose • Fever – usually mild • Epistaxis • Headache • Cough • Shortness of breath • Bloody vomiting • Altered mental status 27
- 28. 28
- 29. Diagnostic criteria The 1950 Smith and Krichner criteria for the clinical diagnosis of mucormycosis; (i) Black, necrotic turbinate’s easily mistaken for dried, crusted blood, (ii) Blood-tinged nasal discharge and facial pain, both on the same side, (iii) Soft peri-orbital or peri-nasal swelling with discoloration and induration (iv) Ptosis of the eyelid, proptosis of the eyeball and complete ophthalmoplegia and (v) Multiple cranial nerve palsies unrelated to documented lesions. 29
- 30. 30 Cornely OA, Alastruey-Izquierdo A, Arenz D, Chen SC, Dannaoui E, Hochhegger B, Hoenigl M, Jensen HE, Lagrou K, Lewis RE, Mellinghoff SC. Global guideline for the diagnosis and management of mucormycosis: an initiative of the European Confederation of Medical Mycology in cooperation with the Mycoses Study Group Education and Research Consortium. The Lancet infectious diseases. 2019 Dec 1;19(12):e405-21.
- 31. Investigations • Histopathology (In 10%Formalin) – for presence of fungus • KOH mount (in Normal Saline) – for presence of fungus • Fungal culture (in Normal Saline) – for type of fungus • All Mucorales grow rapidly (3–5 days) on most fungal culture media, such as Sabouraud agar and potato dextrose agar incubated at 25–30°C • Microbiological identification of the hyphae based on diameter, presence or absence of septa, branching angle (right or acute branching), and pigmentation, differentiates it from other fungal infections • No laboratory tests are specifically suggestive of diagnosis beyond cultures from likely infected sites in an “appropriate host” for mucormycosis or histopathology from infected tissue that is consistent with Mucorales infection (gold standard). 31
- 32. • Direct microscopy of clinical specimens, preferably using optical brighteners in clinical specimens, allows a rapid presumptive diagnosis of mucormycosis. • Blankophor and Calcofluor White bind to chitin and fluoresce in ultraviolet light • Hyphae of Mucorales have a variable width (6–25 μm), are nonseptate or sparsely septate. • The angle of branching is variable and includes wide-angle (90°) bifurcations 32 Branscomb R. An overview of mucormycosis. Laboratory Medicine. 2002 Jun 1;33(6):453-5.
- 33. 33
- 34. 34
- 35. • Histological sections show acute suppurative inflammation with focal areas of granulomatous inflammation. • There are aseptate hyphae 6 to 50 µm in diameter, branching at 90°. • The hyphae invade the adjacent blood vessel walls, producing thrombosis and infarction, but rarely disseminate through the vessels. • Staining with Grocott-Gomori methenamine silver is best, though periodic acid-Schiff and hematoxylin & eosin (H&E) stains can be used. • Diagnosis is frequently made from tissue sections 35 . Koneman E, Allen S. Diagnostic Microbiology. Philadelphia, PA: JB Lippincott. 1992:812-814.
- 36. Radiographic presentation • Multiple (>10) nodules by CT scan and pleural effusion • Reverse halo sign (ground glass attenuation inside a ring of hemorrhage) • Pulmonary infection suggestive of infection crossing tissue planes (i.e., chest wall cellulitis adjacent to a lung infarct) 36
- 37. 37
- 38. Mucormycosis of the oral cavity 38 Rai S, Misra D, Misra A, Jain A, Jain P, Dhawan A. Palatal mucormycosis masquerading as bacterial and fungal osteomy A rare case report. Contemporary clinical dentistry. 2018 Apr;9(2):309.
- 39. 39 Kumar JA, Babu P, Prabu K, Kumar P. Mucormycosis in maxilla: Rehabilitation of facial defects using interim
- 40. Mortality • the intracranial involvement of mucormycosis increases the fatality rate to as high as 90% • DM remains the leading risk factor associated with mucormycosis globally, with an overall mortality of 46% 40 Deutsch PG, Whittaker J, Prasad S. Invasive and non-invasive fungal rhinosinusitis—a review and update of the evidence, Medicina (2019) 1–14.
- 41. • The current survival rate for rhinocerebral disease in patients with no systemic disease is about 75%; with diabetes, about 60%; and with other underlying diseases, about 20%. • Pulmonary disease is almost uniformly fatal. Sivapathasundharam B. Shafer's Textbook of Oral Pathology E-book. Elsevier Health Sciences; 2020 Jul 15. 41
- 42. Differential diagnosis • Aspergillosis • Fusariosis • Pseudallescheria complex • Phaeohyphomycosis (i.e., brown-black molds) • Cryptococcus • Advanced (extensive) Pneumocystis jirovecii infection • Tuberculosis • Pseudomonas aeruginosa, Staphylococcus aureus 42
- 43. Tests useful for establishing differential diagnosis: • Serum or BAL galactomannan or beta-D glucan (to aid diagnosis of pulmonary aspergillosis) • Serum cryptococcal antigen • Urine and serum antigen assays for histoplasmosis, blastomycosis, and coccidiodomycosis (if history is suggestive of endemic fungal infection) • Pneumocystis DFA or polymerase chain reaction (PCR) from BAL • Quantiferon TB test (however, most experts say this should not be used for diagnosis) 43
- 44. Management Key principles of therapy: • Early diagnosis • Reversal or tapering of underlying immunosuppression • Systemic antifungal therapy • Surgical resection or debulking of infected necrotic lesions if feasible • Adjunctive therapies 44
- 45. • Patients should be started on a lipid amphotericin B formulation (possibly with the addition of an echinocandin) at first suspicion of mucormycosis. • While patient is on Ampho-B treatment, daily monitoring of RFT and Serum Electrolytes to check for hypokalemia is mandatory • Currently, only four systemic antifungal agents are available for the treatment of mucormycosis: amphotericin B, lipid amphotericin B, posaconazole, isavuconazole and occasionally echinocandins (some will use in combination with lipid amphotericin B formulations) 45
- 46. 46 Swaminathan S. Mycoses in Transplant. InClinical Practice of Medical Mycology in Asia 2020 (pp. 101-117). Springer, Singapore.
- 47. • Induction with LIPOSOMAL AMPHOTERICIN-B (L-AMB) 5-10 mg/kg/day for 2 weeks • Deoxycholate formulation of Amphotericin-B: 0.7 - 1.0 mg/kg daily (this is more toxic) OR • Dual therapy: L-AMB + Oral Posaconazole (300 mg BD on Day 1 f/b 300 mg OD for 2 weeks) • Oral POSACONAZOLE 300 mg BD for a further 2-4 weeks till clinical resolution and radiological stabilization. • Monitor patients clinically, with radio-imaging for response / disease progression & microbiologically • After 3-6 weeks of AMPHOTERICINE-B therapy, consolidation therapy (POSACONAZOLE/ISAVUCONAZOLE) for 3-6 months 47
- 48. • Control of hyperglycemia/ketoacidosis is critical to reverse physiological conditions that contribute to increase free iron in tissues (acidemia) as well as impair neutrophil function. • Reversal or tapering of immunosuppression (i.e., corticosteroids) improves patient responses to systemic antifungal therapy. 48
- 49. Surgical • Surgical debridement of infection tissue and/or debulking of necrotic lesions has been associated with improved survival in several case series; however, evidence in this this area is biased by that fact that surgery is more likely pursued in patients with better prognosis of their underlying disease. • Radical surgical resections combined with systemic antifungal have been lifesaving when performed early in the course of treatment, particularly in patients with sinus mucormycosis at risk for invasion of the brain. • Transcutaneous Retrobulbar Amphotericin B (TRAMB): 1 ml of 3.5 mg/ml • Orbital Exenteration : For patients with extensive orbital involvement. 49
- 50. Controversial or evolving therapies: • Hyperbaric oxygen therapy has been reported effective for cutaneous and sinus mucormycosis and is believed to speed wound healing following surgical resection • Iron chelation with newer agents that cannot be used as xenosiderophores by Mucorales (i.e., deferasirox) has been shown in animal models to exhibit direct antifungal effects through iron starvation and salutary immunostimulatory effects 50 Swaminathan S. Mycoses in Transplant. InClinical Practice of Medical Mycology in Asia 2020 (pp. 101-117). Springer, Singapore.
- 51. 51
- 52. Prevention • Antifungal prophylaxis with posaconazole in high risk populations 52 Swaminathan S. Mycoses in Transplant. InClinical Practice of Medical Mycology in Asia 2020 (pp. 101-117). Springer, Singapore.
- 53. 53
- 54. Summary • Mucormycosis post COVID 19 is a rapidly developing disease • Mainly caused by Rhizopus species • DM has been the most common risk factor linked, hematological malignancies and organ transplant ie patient who are immunocompromised and are infected with COVID 19 • Rhoncocerebral form is the most common presentation in dental setting • Early signs of tooth ache and loose teeth along with headache, pain in the eye can be early signs to look for oral physicians 54
- 55. • Suscpicion of mucormycosis should be followed by radiographic investigation and immediate referral to E.N.T department • Early treatment is of upmost importance in case of mucormycosis 55
- 56. Conclusion • As of recent events oral physicians or dentist may be the first one to recognize signs of mucormycosis se knowledge about every aspect of mucormycosis is important for dental health care provider. 56
- 58. Early sign of mucormycosis in a patient in dental setting may be? a. Sinusitis b. Eschar in face c. Loose teeth and dental pain d. Chest pain 58
- 59. Part of medical history of great significance in suspicion of Mucormycosis is a) Immunocompromised state and post COVID 19 b) Previous history of Tuberculosis c) History of Diabetes d) History of trauma 59
- 60. First treatment strategy for treatment of Mucormycosis is a. Surgical debridement b. Control of blood sugar level c. Start of Amphotericin d. Use of steroids 60
- 61. Thank you 61
- 62. References • Eucker J, Sezer O, Graf B, Possinger K. Mucormycoses. Mycoses. 2001 Oct;44(7‐8):253-60. • Branscomb R. An overview of mucormycosis. Laboratory Medicine. 2002 Jun 1;33(6):453-5 • Singh AK, Singh R, Joshi SR, Misra A. Mucormycosis in COVID-19: a systematic review of cases reported worldwide and in India. Diabetes & Metabolic Syndrome: Clinical Research & Reviews. 2021 May 21. • Hoang K, Abdo T, Reinersman JM, Lu R, Higuita NIA. A case of invasive pulmonary mucormycosis resulting from short courses of corticosteroids in a wellcontrolled diabetic patient. Med Mycol Case Rep. 2020;29(1):22-24. 62
- 63. • Lionakis MS, Kontoyiannis DP. Glucocorticoids and invasive fungal infections. Lancet 2003, 362, 1828–1838. • Singh AK, Singh R, Joshi SR, Misra A. Mucormycosis in COVID-19: a systematic review of cases reported worldwide and in India. Diabetes & Metabolic Syndrome: Clinical Research & Reviews. 2021 May 21. • Skiada A, Lass-Floerl C, Klimko N, Ibrahim A, Roilides E, Petrikkos G. Challenges in the diagnosis and treatment of mucormycosis. Medical mycology. 2018 Apr 1;56(suppl_1):S93-101. • Cornely OA, Alastruey-Izquierdo A, Arenz D, Chen SC, Dannaoui E, Hochhegger B, Hoenigl M, Jensen HE, Lagrou K, Lewis RE, Mellinghoff SC. Global guideline for the diagnosis and management of mucormycosis: an initiative of the European Confederation of Medical Mycology in cooperation with the Mycoses Study Group Education and Research Consortium. The Lancet infectious diseases. 2019 Dec 1;19(12):e405-21. 63
- 64. • Cornely OA, Alastruey-Izquierdo A, Arenz D, Chen SC, Dannaoui E, Hochhegger B, Hoenigl M, Jensen HE, Lagrou K, Lewis RE, Mellinghoff SC. Global guideline for the diagnosis and management of mucormycosis: an initiative of the European Confederation of Medical Mycology in cooperation with the Mycoses Study Group Education and Research Consortium. The Lancet infectious diseases. 2019 Dec 1;19(12):e405-21. • Swaminathan S. Mycoses in Transplant. InClinical Practice of Medical Mycology in Asia 2020 (pp. 101-117). Springer, Singapore. • Sivapathasundharam B. Shafer's Textbook of Oral Pathology E-book. Elsevier Health Sciences; 2020 Jul 15. • Sugar AM. Mucormycosis. Clin Infect Dis 1992;14:S126-9 • Deutsch PG, Whittaker J, Prasad S. Invasive and non-invasive fungal rhinosinusitis—a review and update of the evidence, Medicina 55 (2019) 1–14. • Rai S, Misra D, Misra A, Jain A, Jain P, Dhawan A. Palatal mucormycosis masquerading as bacterial and fungal osteomyelitis: A rare case report. Contemporary clinical dentistry. 2018 Apr;9(2):309. 64
