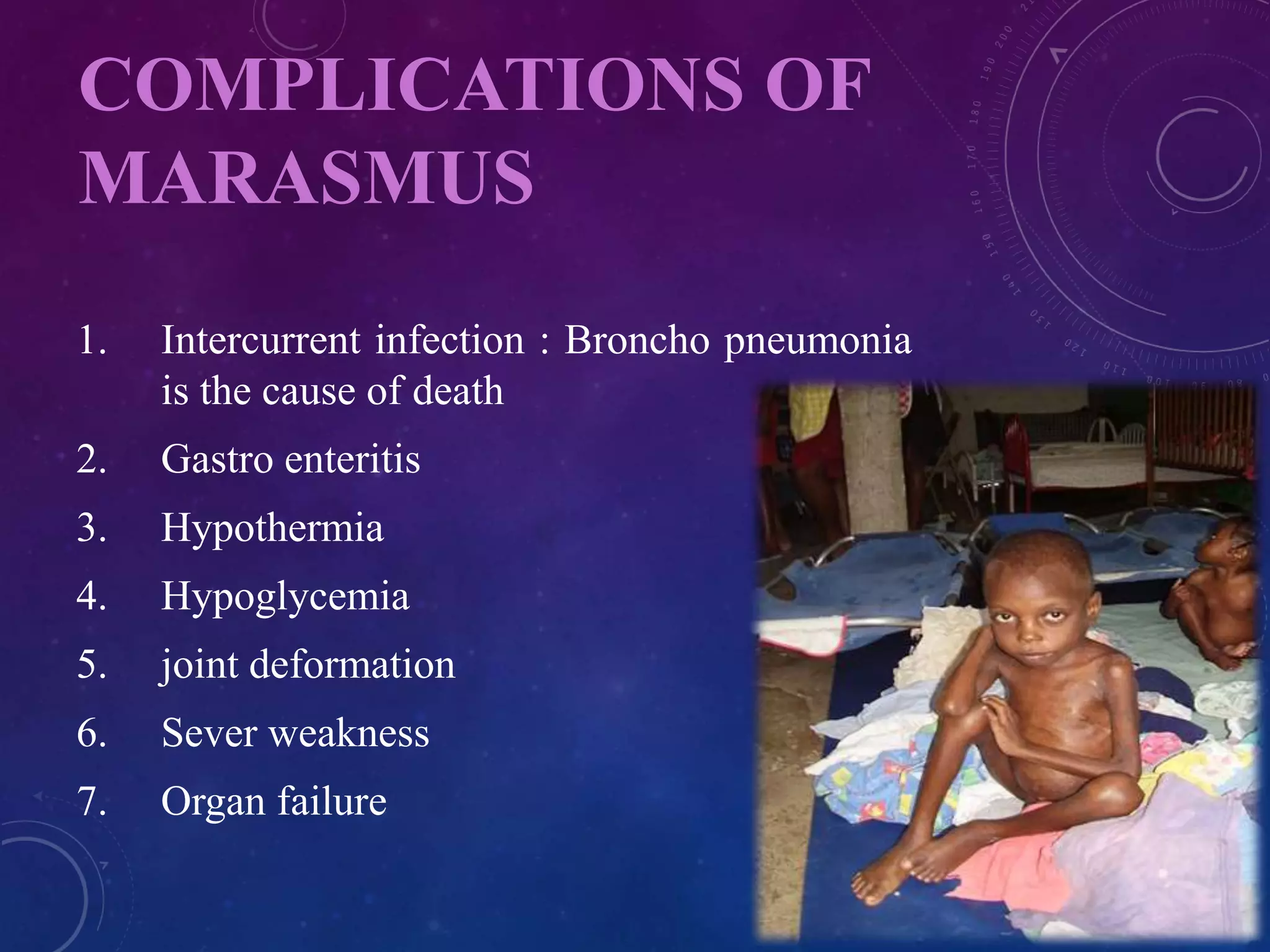
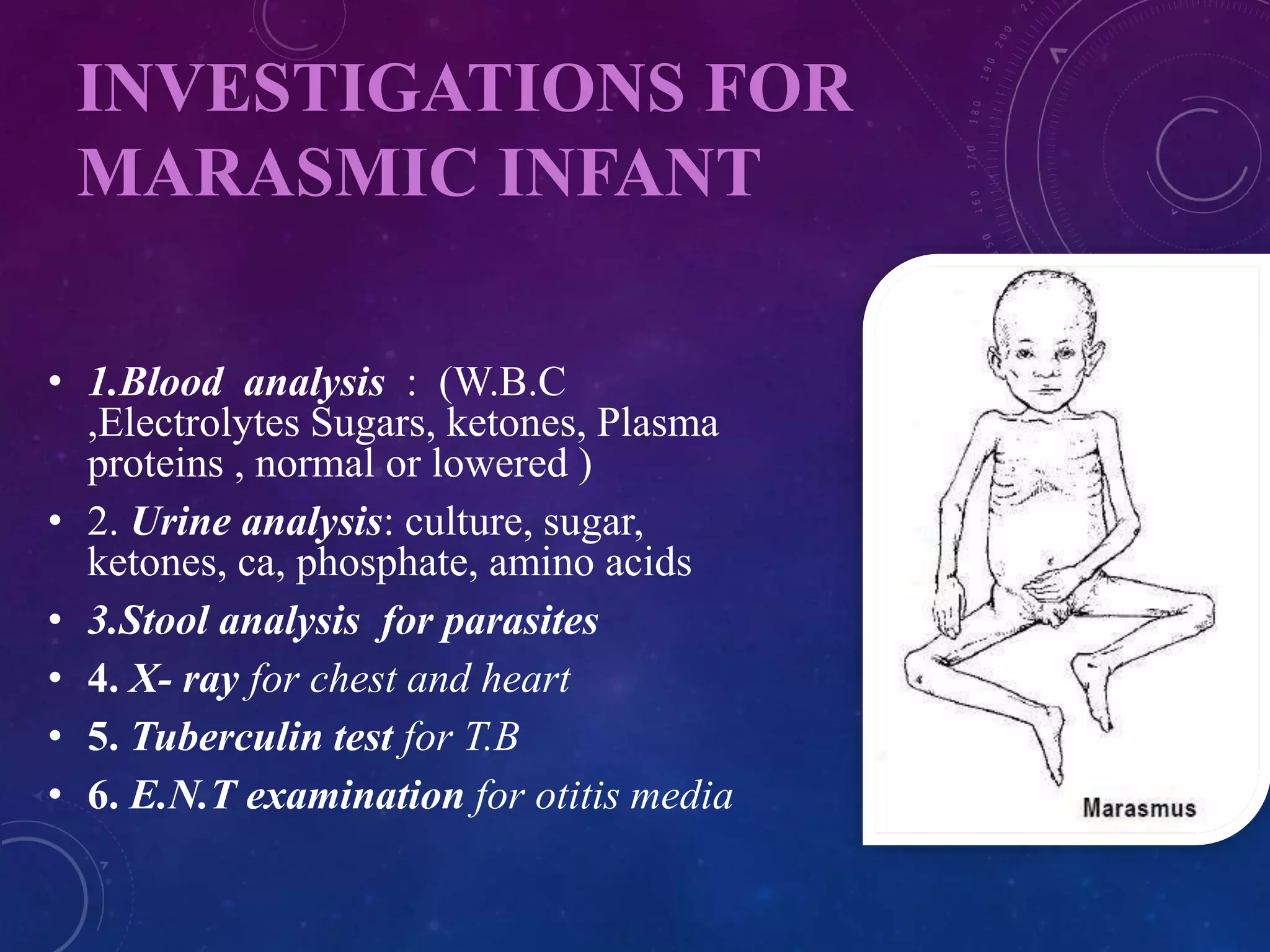
Marasmus is a form of severe protein-energy malnutrition resulting from inadequate calorie intake. It is characterized by muscle wasting and loss of subcutaneous fat. Complications include infection, hypothermia, and organ failure. Treatment involves dietary management with balanced, energy-dense feedings through nasogastric tubes if needed. Nursing care focuses on providing nutrition, maintaining temperature, preventing infection, and educating families on proper nutrition.