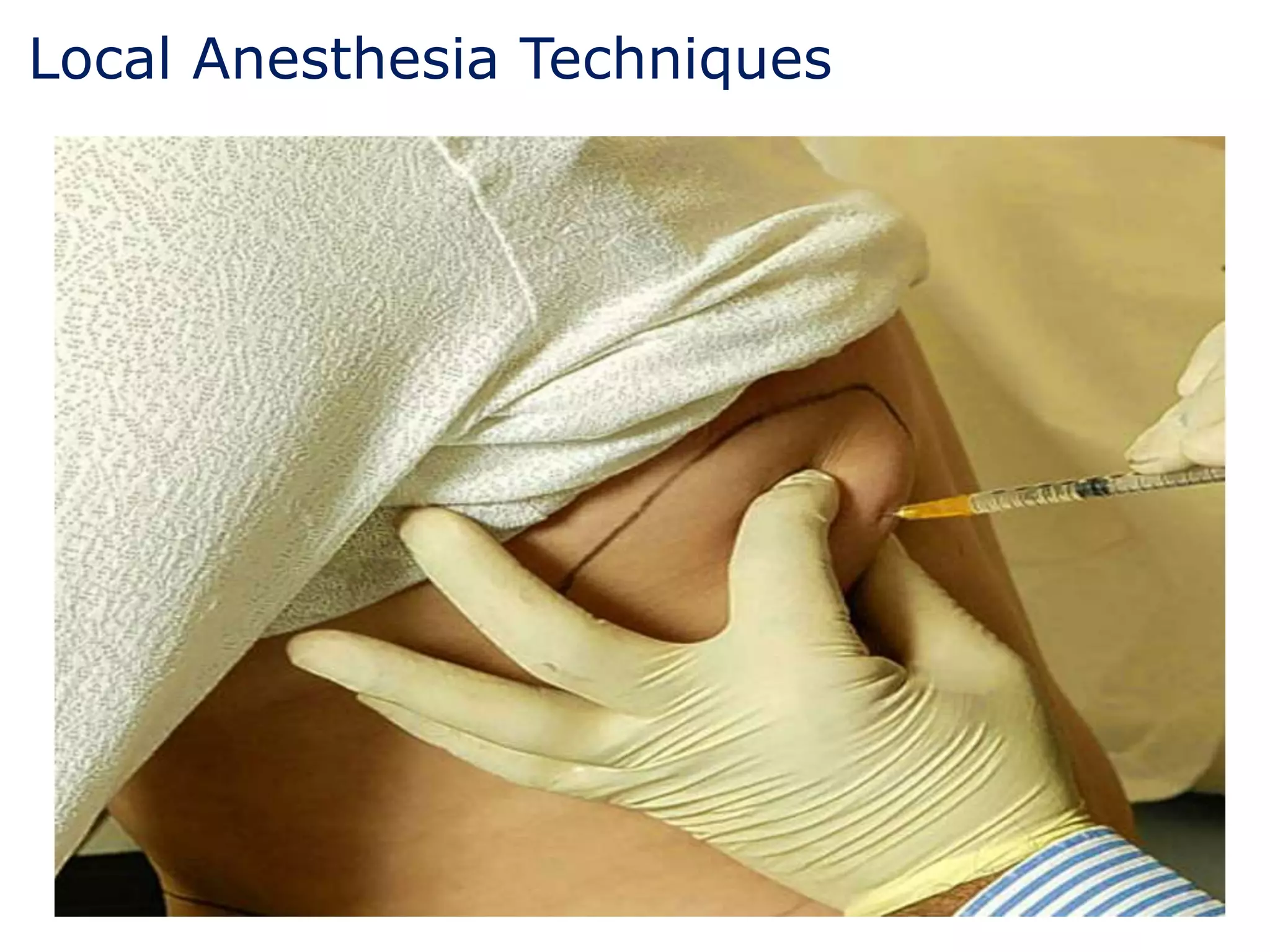
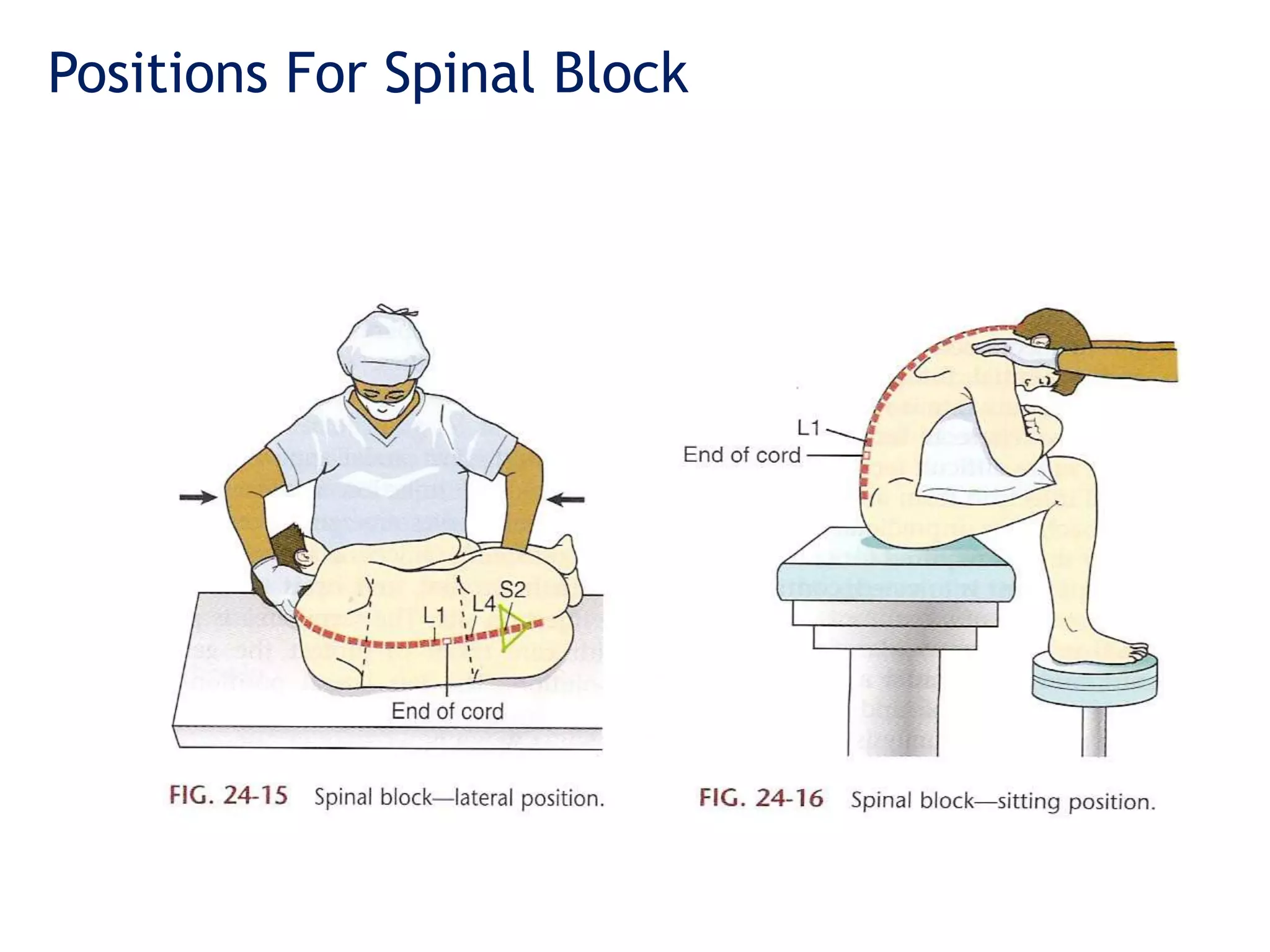
This document discusses different types of anesthesia including local, regional, and general anesthesia. It provides details on common regional anesthesia techniques like spinal blocks, epidurals, and caudal blocks. It also describes local anesthesia techniques such as infiltration, nerve blocks, and intravenous regional anesthesia. The document discusses the mechanisms of local anesthetics and some potential complications as well as benefits of local and regional anesthesia compared to general anesthesia.