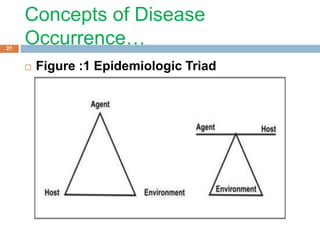
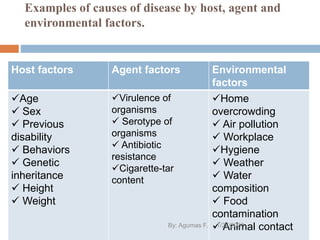
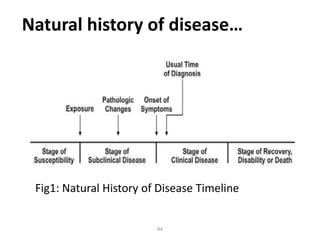
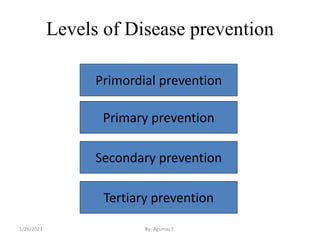
This document provides an overview of the natural history of disease and levels of disease prevention. It discusses the natural history of disease in four stages: susceptibility, pre-symptomatic disease, clinical disease, and disability/death. It also defines different levels of disease occurrence such as endemic, epidemic, outbreak, and pandemic. Finally, it outlines the four main levels of disease prevention: primordial, primary, secondary, and tertiary prevention. The goal of epidemiology is to understand disease causation and distribution in order to implement effective prevention and control measures at various levels.