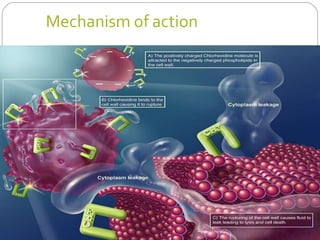
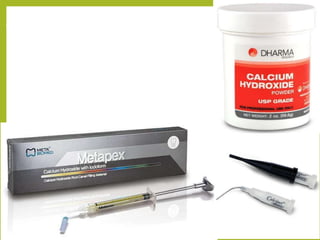
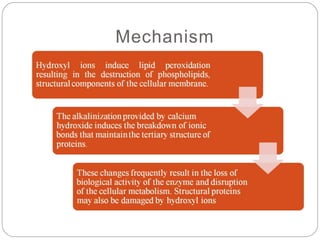
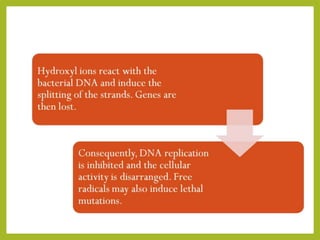
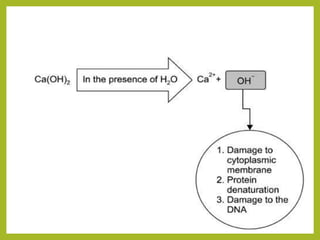
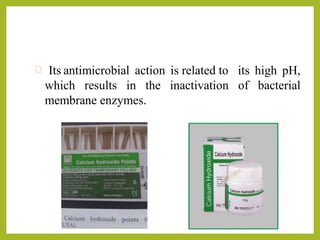
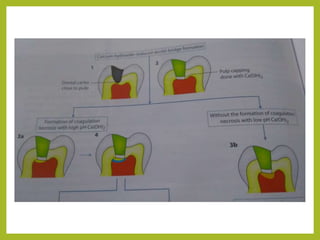
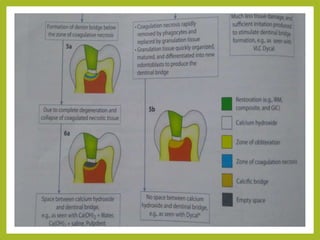
This document discusses intracanal medicaments used in endodontic treatment. It defines intracanal medicaments as temporary placement of biocompatible medications into root canals to inhibit bacterial invasion from the oral cavity. Common intracanal medicaments discussed include phenolics, halogens, non-phenolic biocides like chlorhexidine, calcium hydroxide, corticosteroids, antibiotics, and herbal alternatives. The document also examines the root canal flora, mechanisms of action, advantages and limitations of various intracanal medicaments.