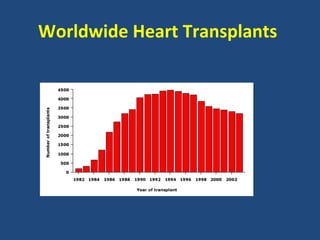
This document summarizes a symposium on heart failure held on January 23rd, 2013 sponsored by Servier Laboratories. The full-day programme consisted of two sessions with multiple speakers covering topics such as the epidemiology, diagnosis, and management of acute and chronic heart failure. New diagnostic tools and treatments discussed include biomarkers like galectin-3 and BNP, cardiac imaging modalities, device therapies, and novel drugs in development. Prognostic factors and approaches to integrated end-of-life care in heart failure were also addressed.

























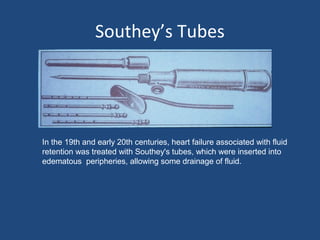

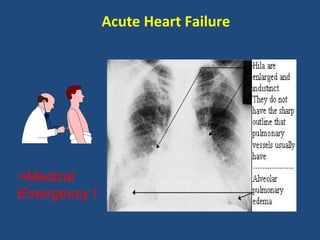




![Annual Mortality Reduction With
Successful Therapies
11.25%-beta blocker Carvedilol [COPERNICUS]
16% ACEI Enalapril [SOLVD]
13% - ARB : Valsartan [Val-HeFT]
• 17.5%- Aldactone -[RALES]
• 24% CRT [COMPANION]
• 36% CRT+D [COMPANION]](https://image.slidesharecdn.com/heartfailuresymposium-130129135324-phpapp01/85/Heart-failure-symposium-40-320.jpg)