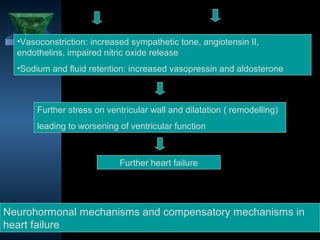
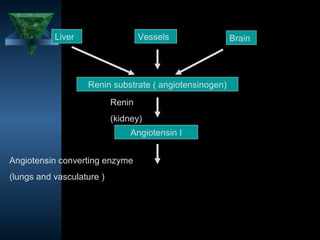
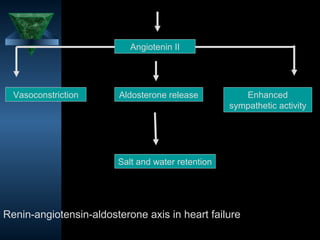
1. Heart failure occurs when the heart cannot pump enough blood to meet the body's needs or can only do so with increased filling pressure.
2. Common causes of heart failure include coronary artery disease, hypertension, cardiomyopathy, valvular heart disease, and arrhythmias.
3. Symptoms of heart failure depend on whether it affects the left side, right side, or both ventricles, and include fatigue, breathlessness, leg swelling, and liver congestion.