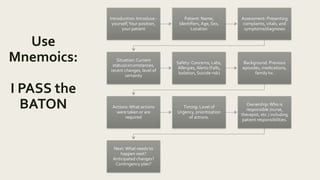
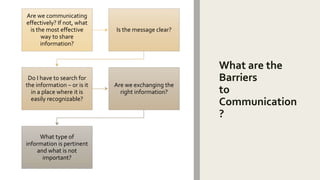
This document discusses the importance of standardizing communication processes during transitions of care in behavioral health to improve patient safety. It provides tips for effective handoff communication between providers and departments, such as using a standardized format like I PASS the BATON to exchange relevant patient information verbally. The document also addresses how to improve discharge planning and transitions between levels of care through coordinated treatment planning, engaging social supports, and orienting patients to upcoming care. Overlapping and blending levels of care can help facilitate continuity of care.