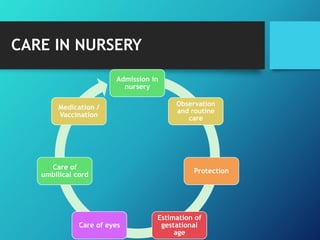
The document outlines essential newborn care practices emphasizing the role of maternal involvement and early bonding between mother and baby. It addresses the crucial first 24 hours of a newborn's life, detailing immediate care procedures, monitoring for congenital issues, and ensuring proper nutrition and infection control. It also incorporates guidelines for managing newborns during the COVID-19 pandemic, highlighting infection prevention, neonatal resuscitation, and vaccination protocols.