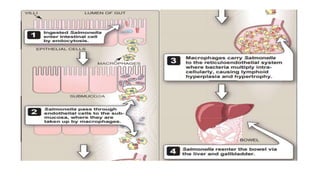
The document provides an overview of the Enterobacteriaceae family of Gram-negative bacteria. It discusses key characteristics such as being facultative anaerobes that ferment carbohydrates and possess complex antigenic structures. Major pathogens within Enterobacteriaceae like Escherichia coli, Salmonella, and Shigella are then described in more detail, outlining their classification, virulence factors, clinical diseases caused, and methods of transmission and prevention.