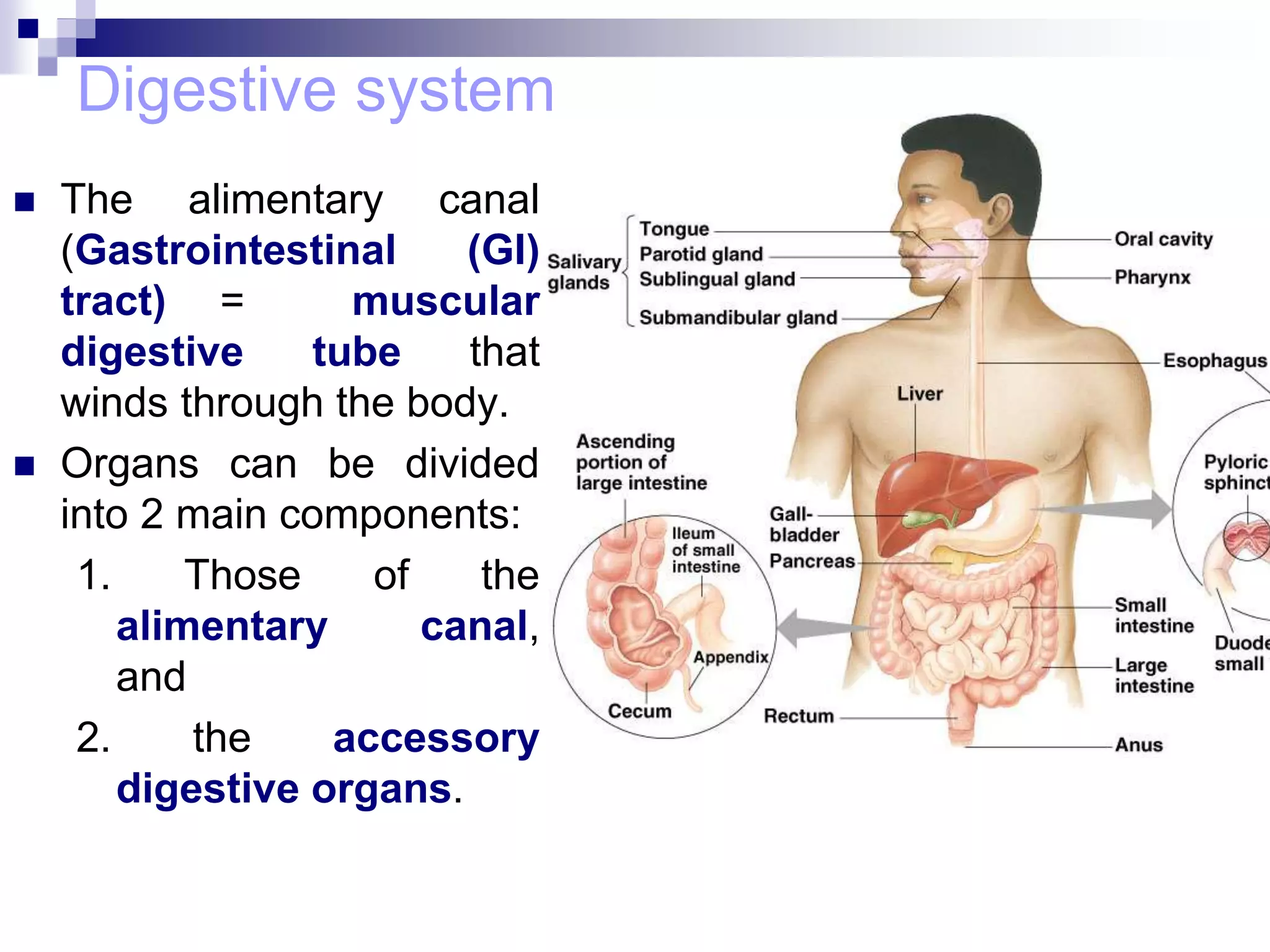
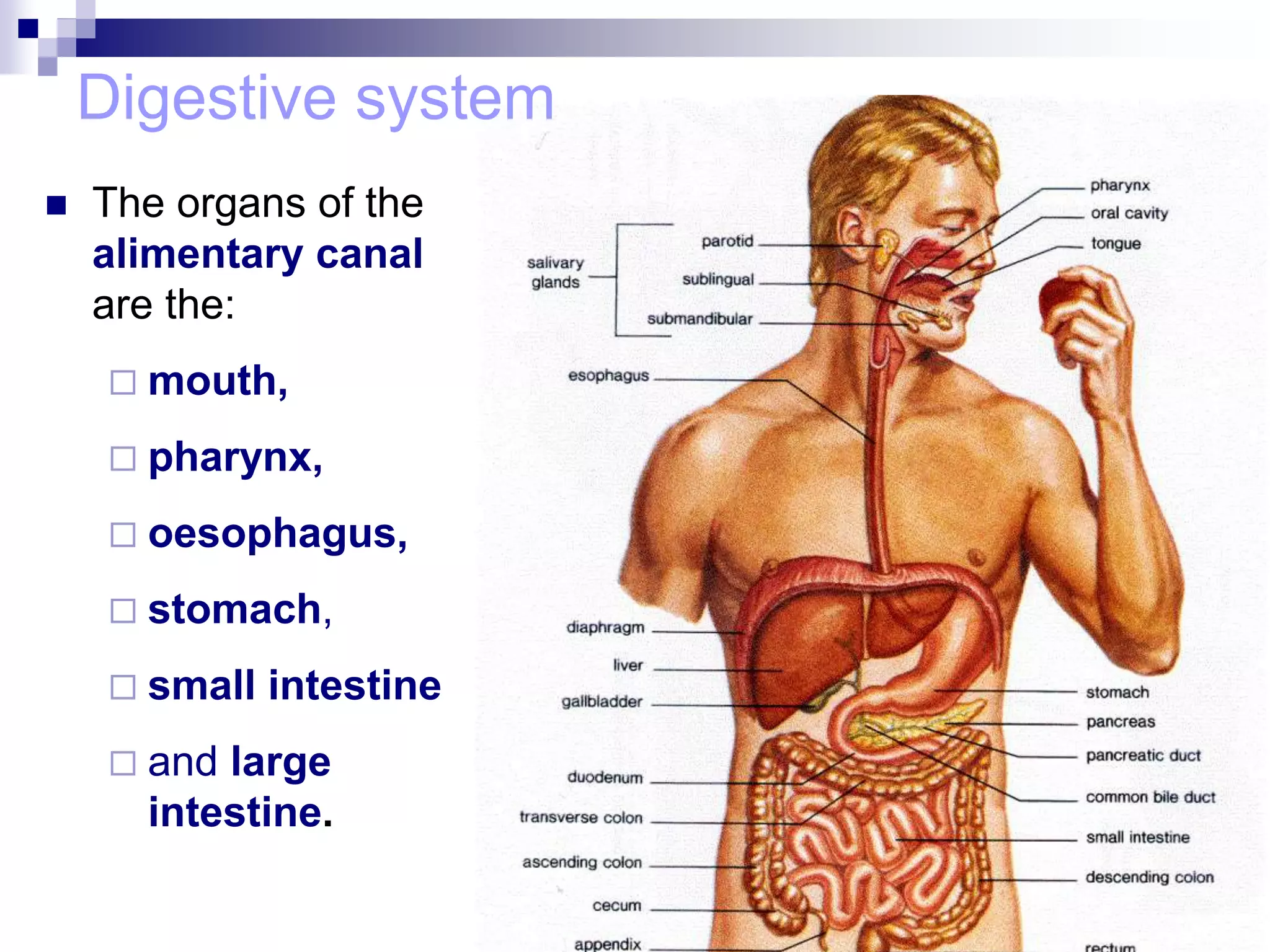
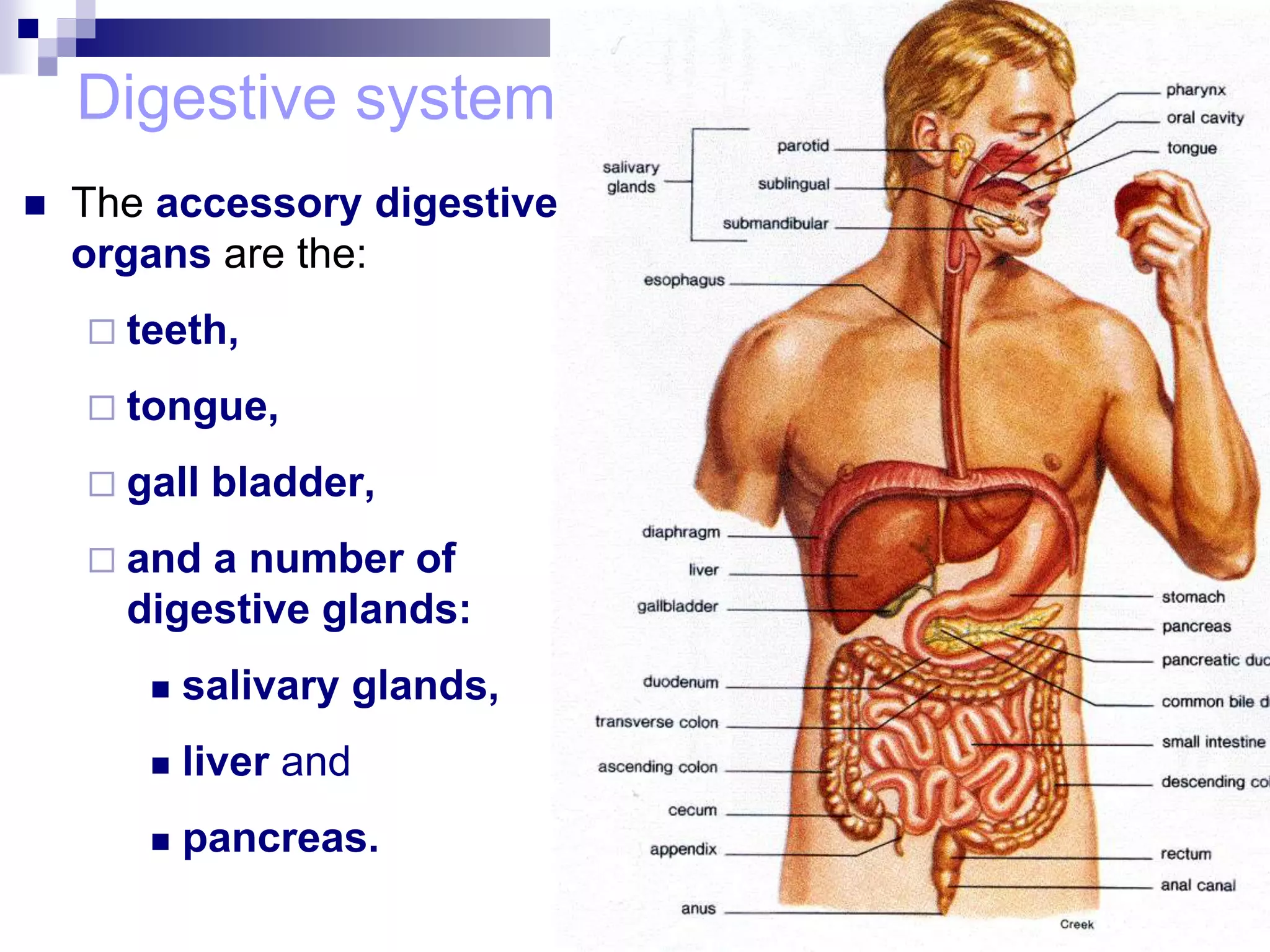
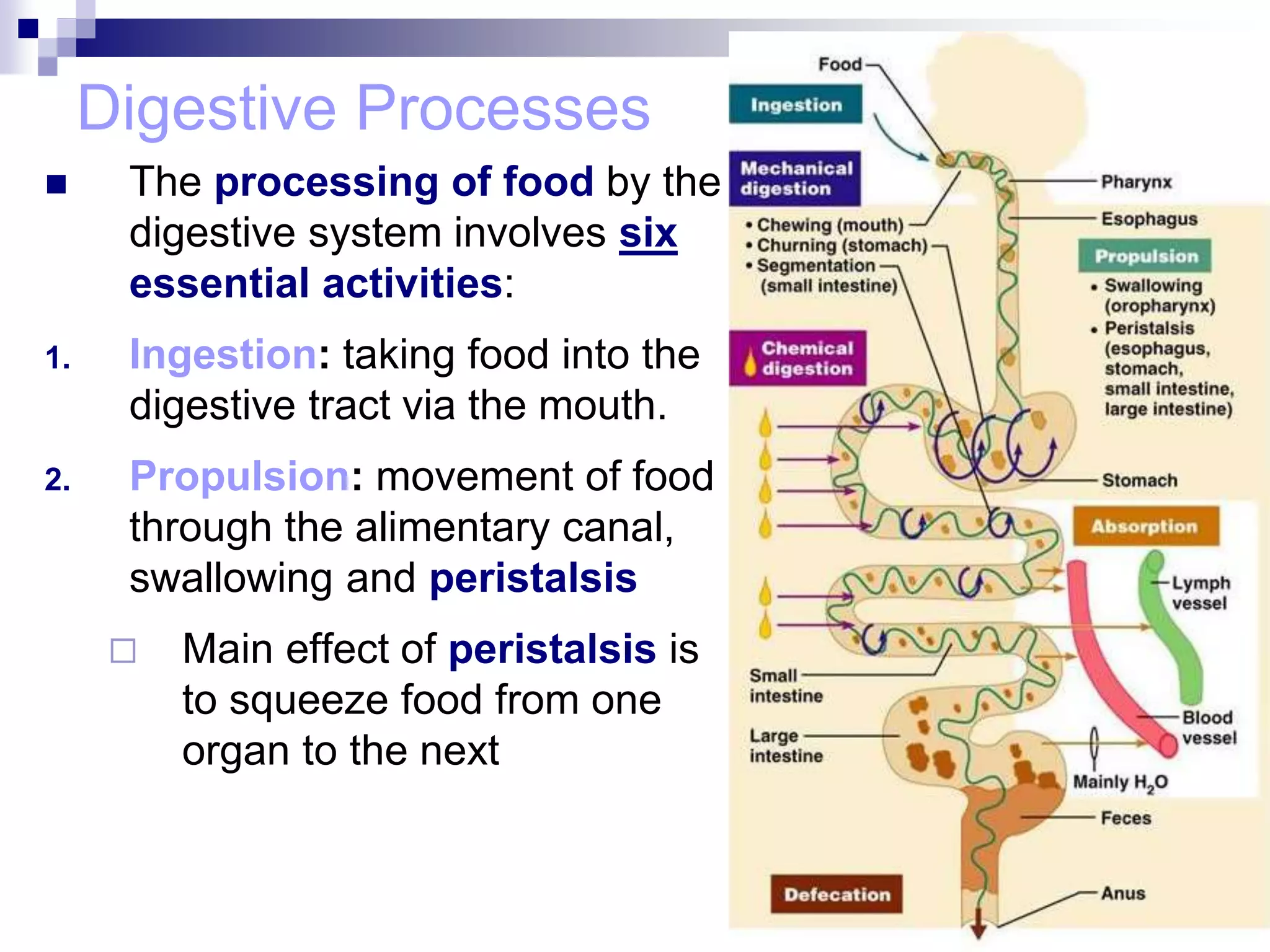
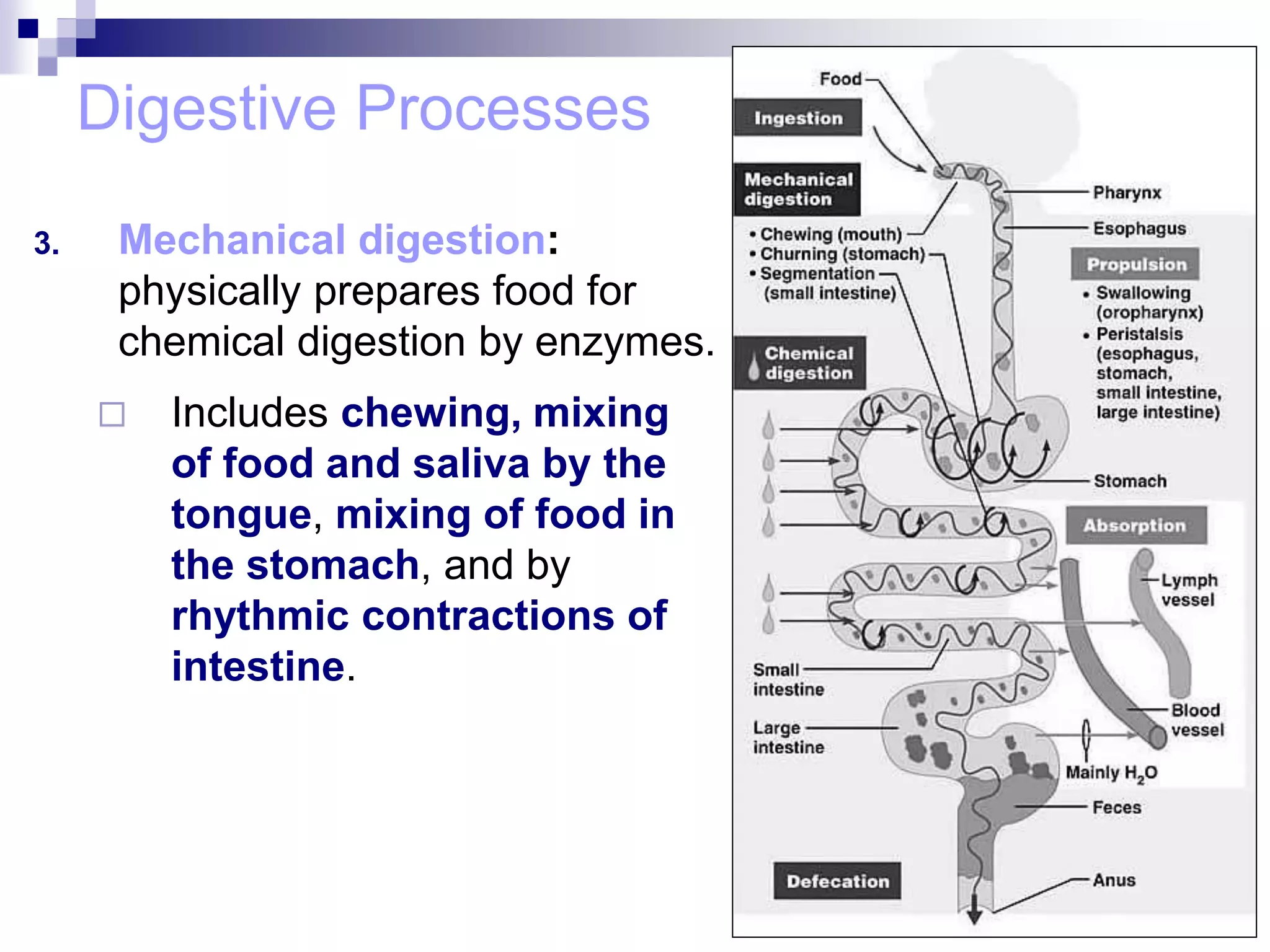
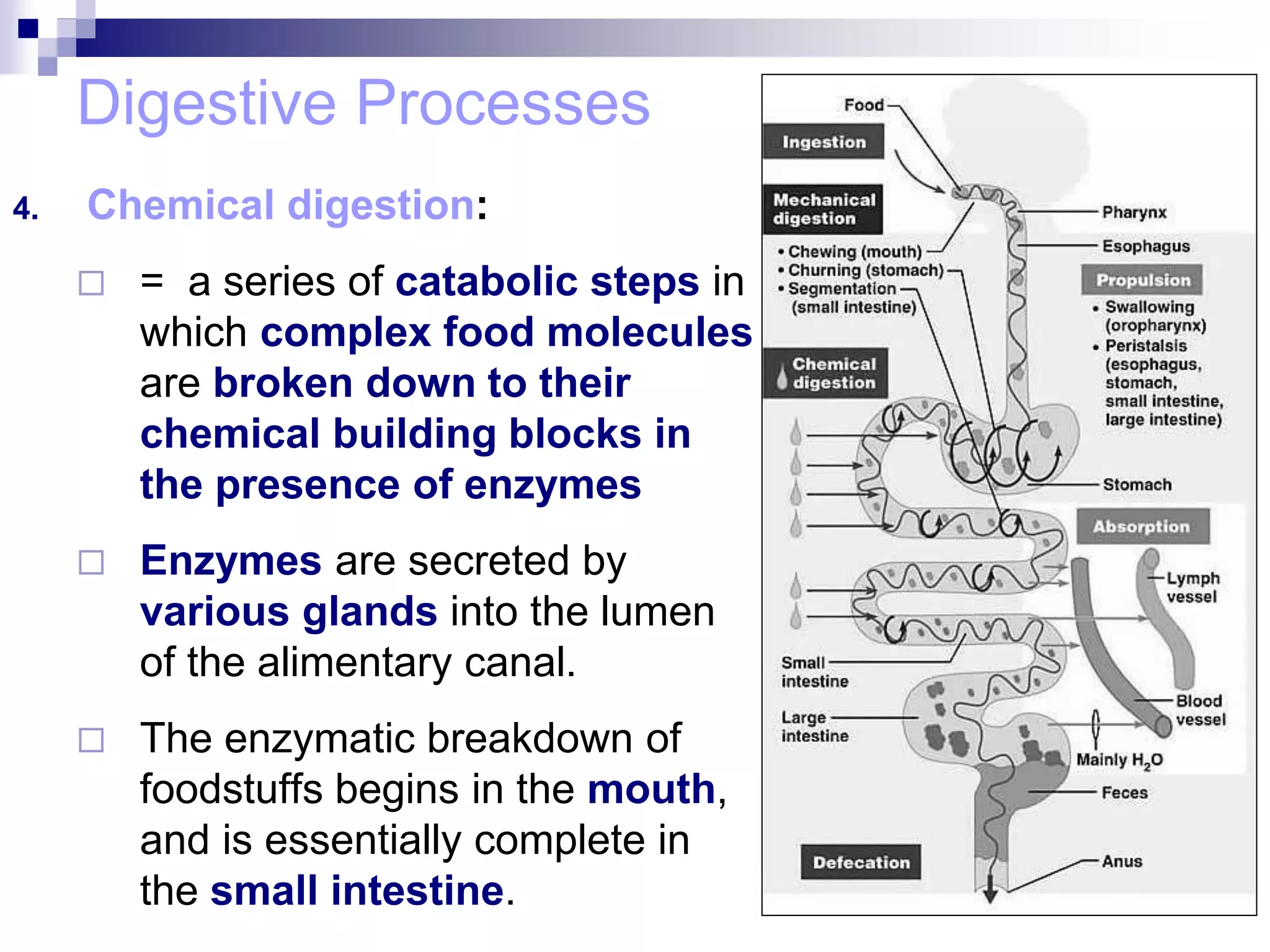
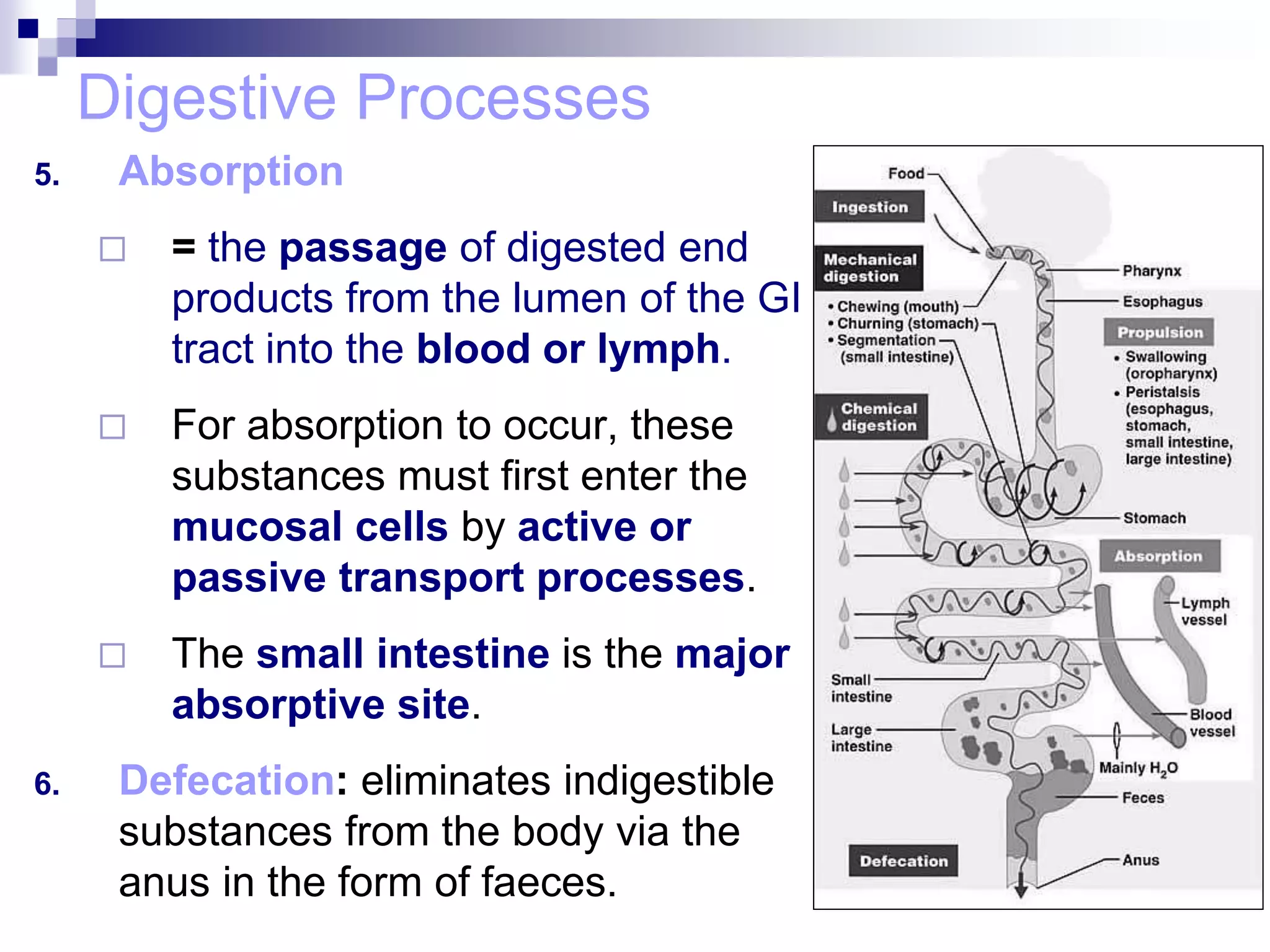
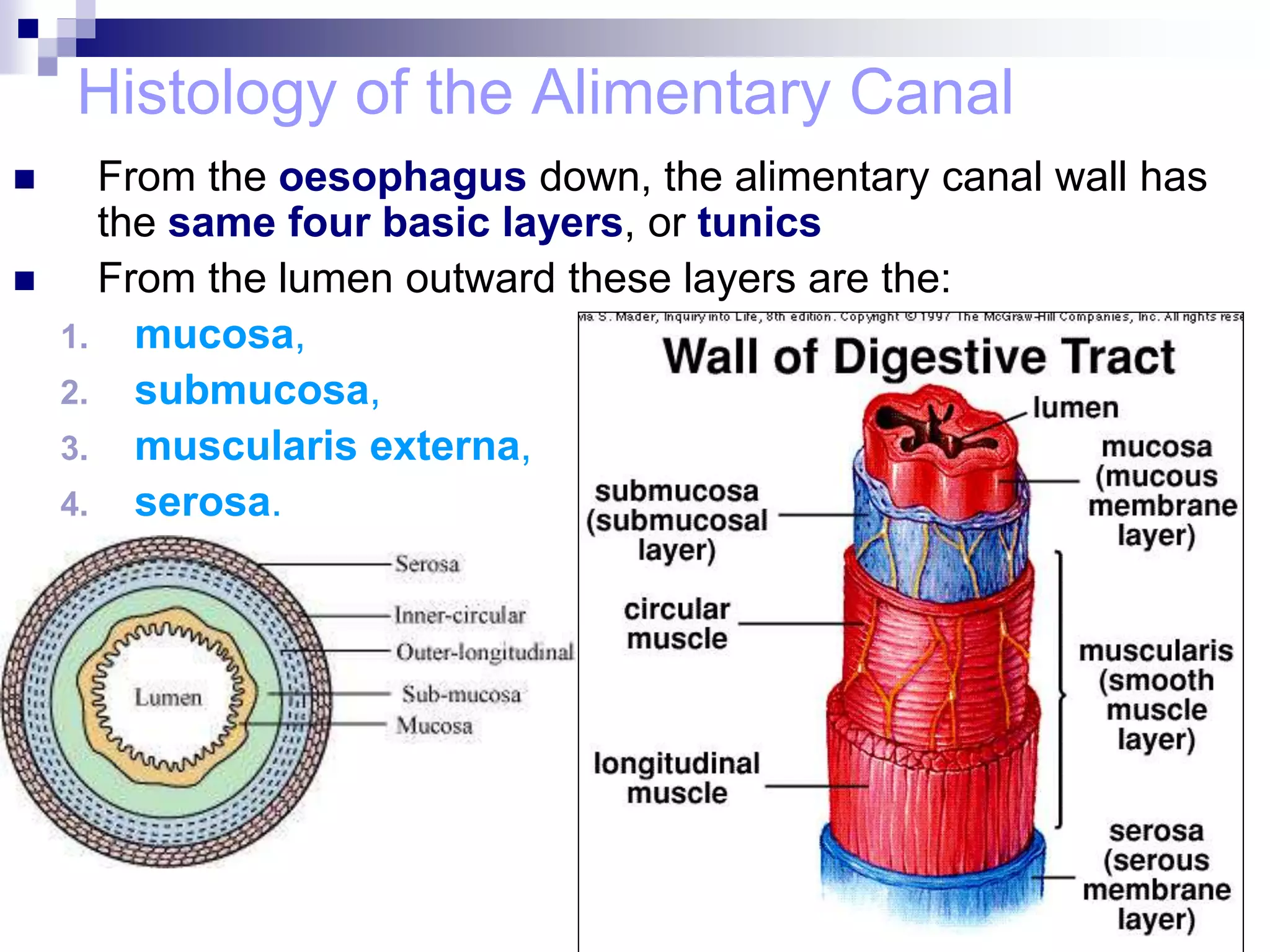
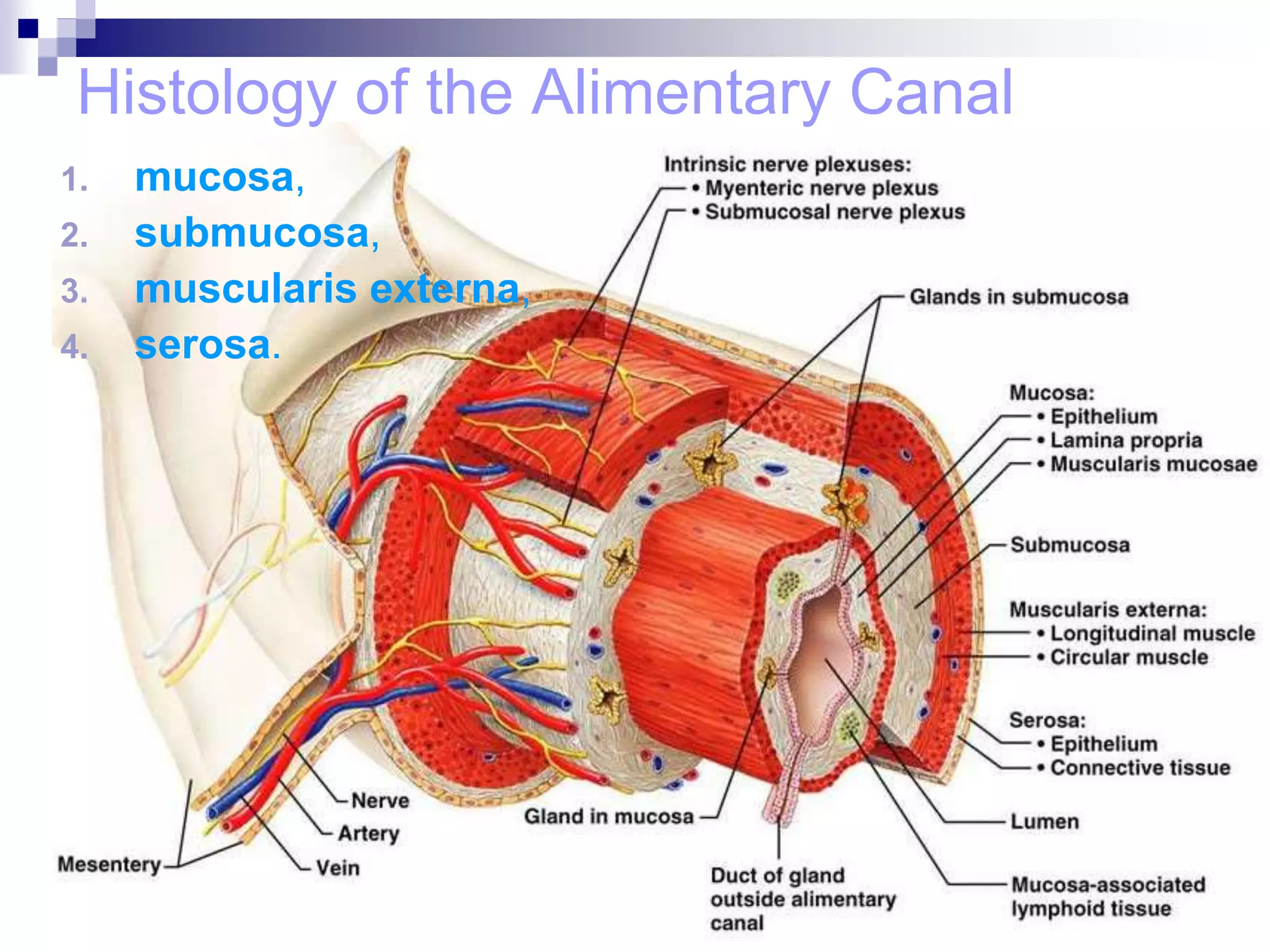
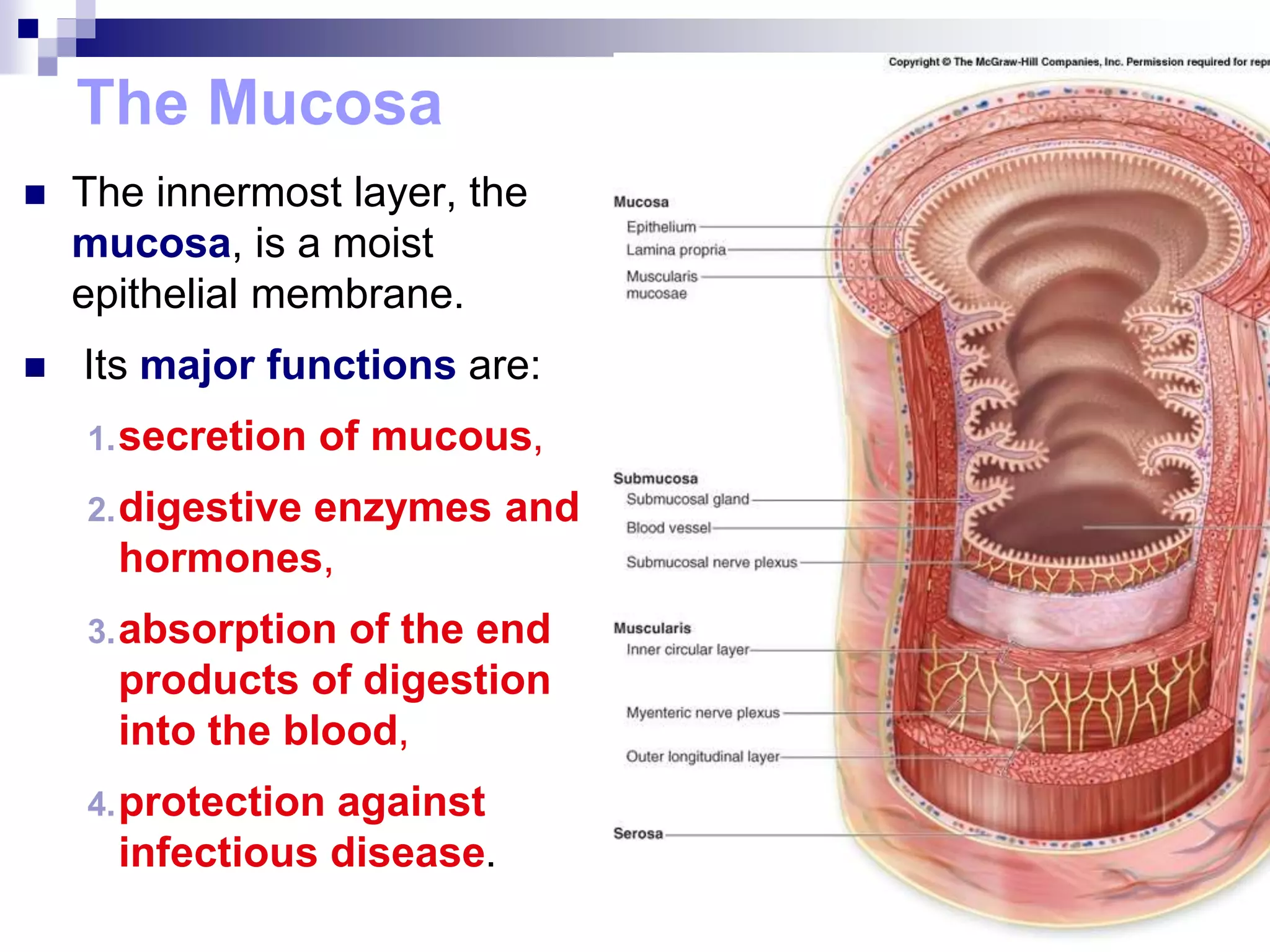
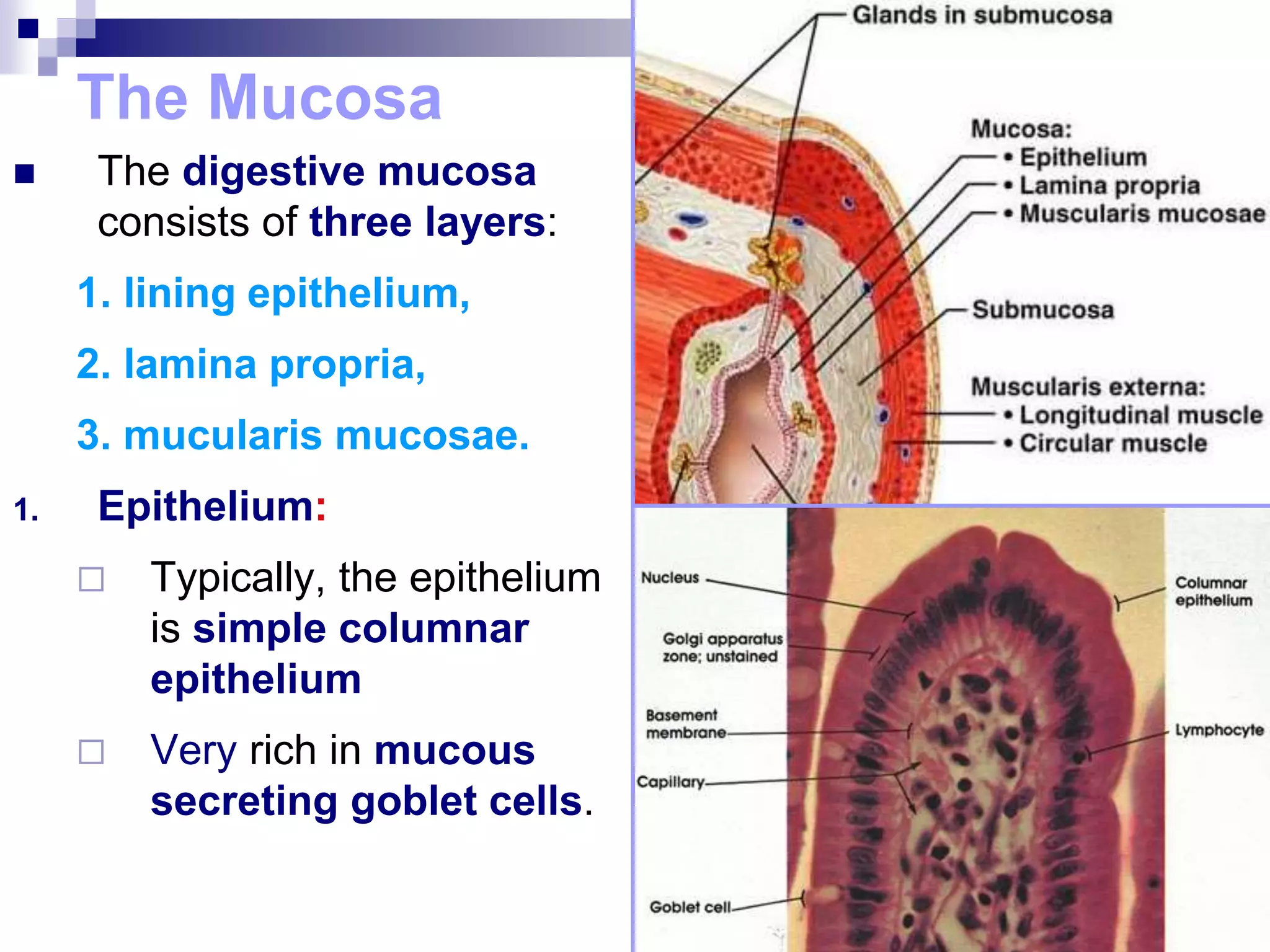
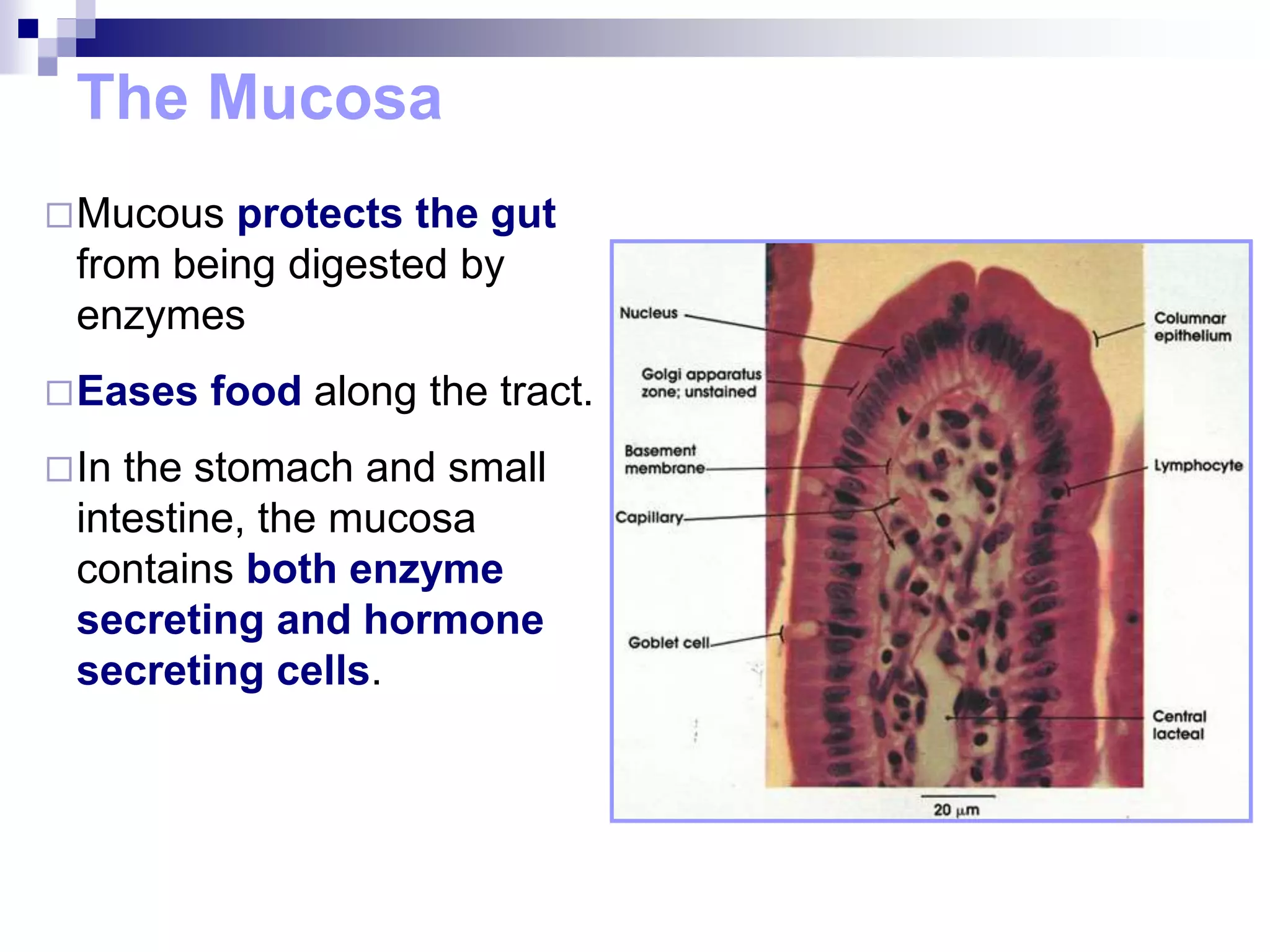
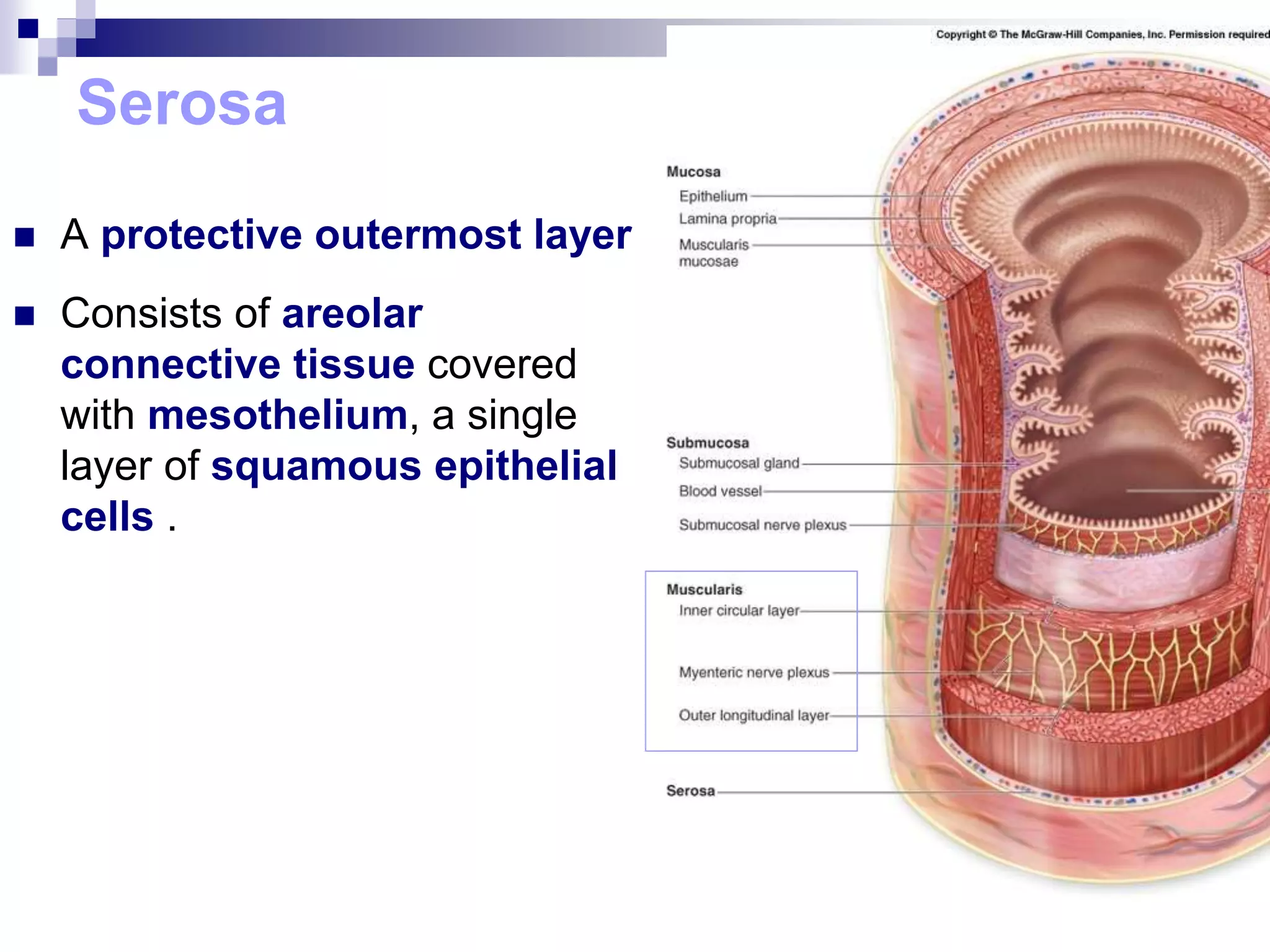
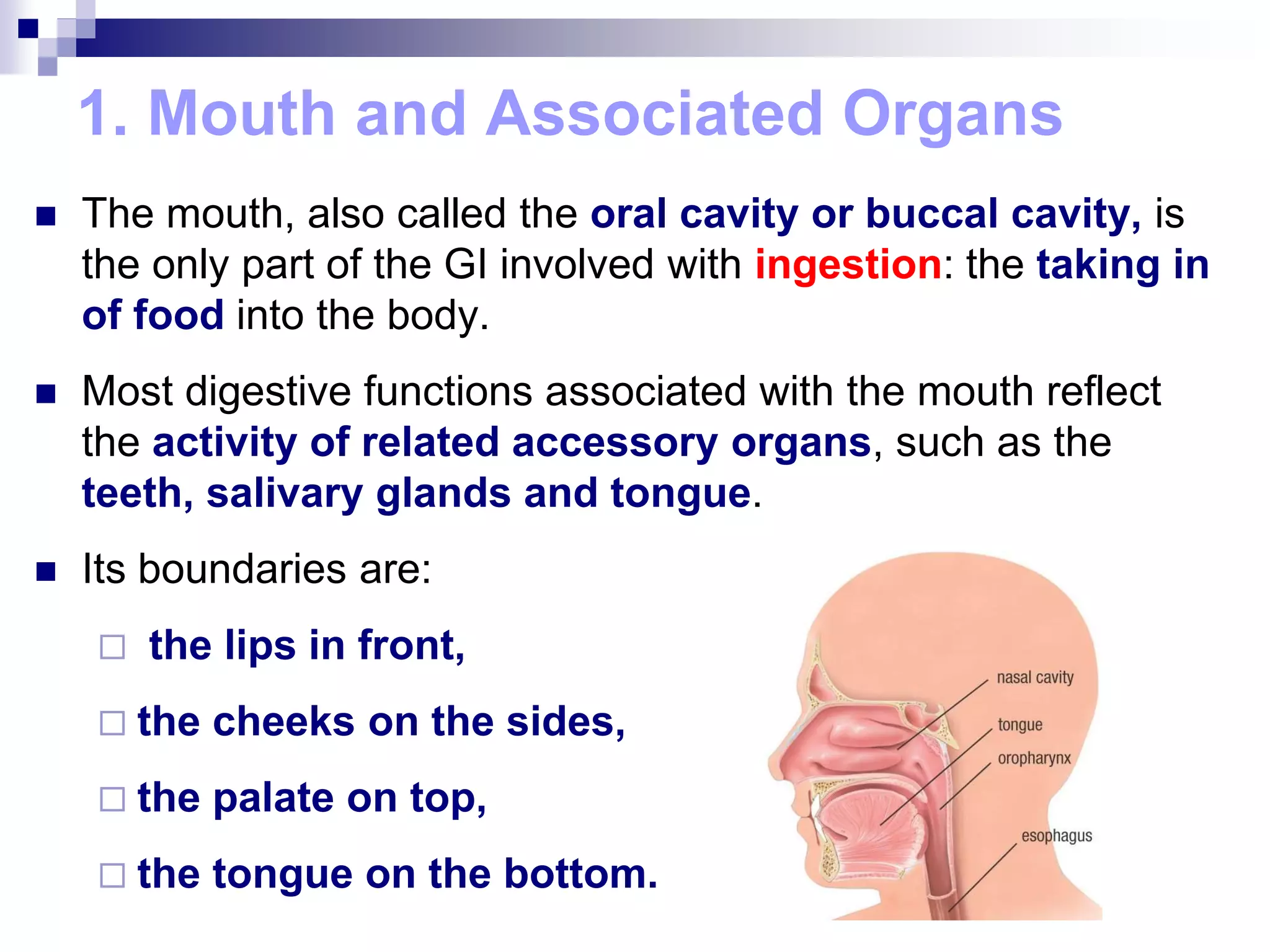
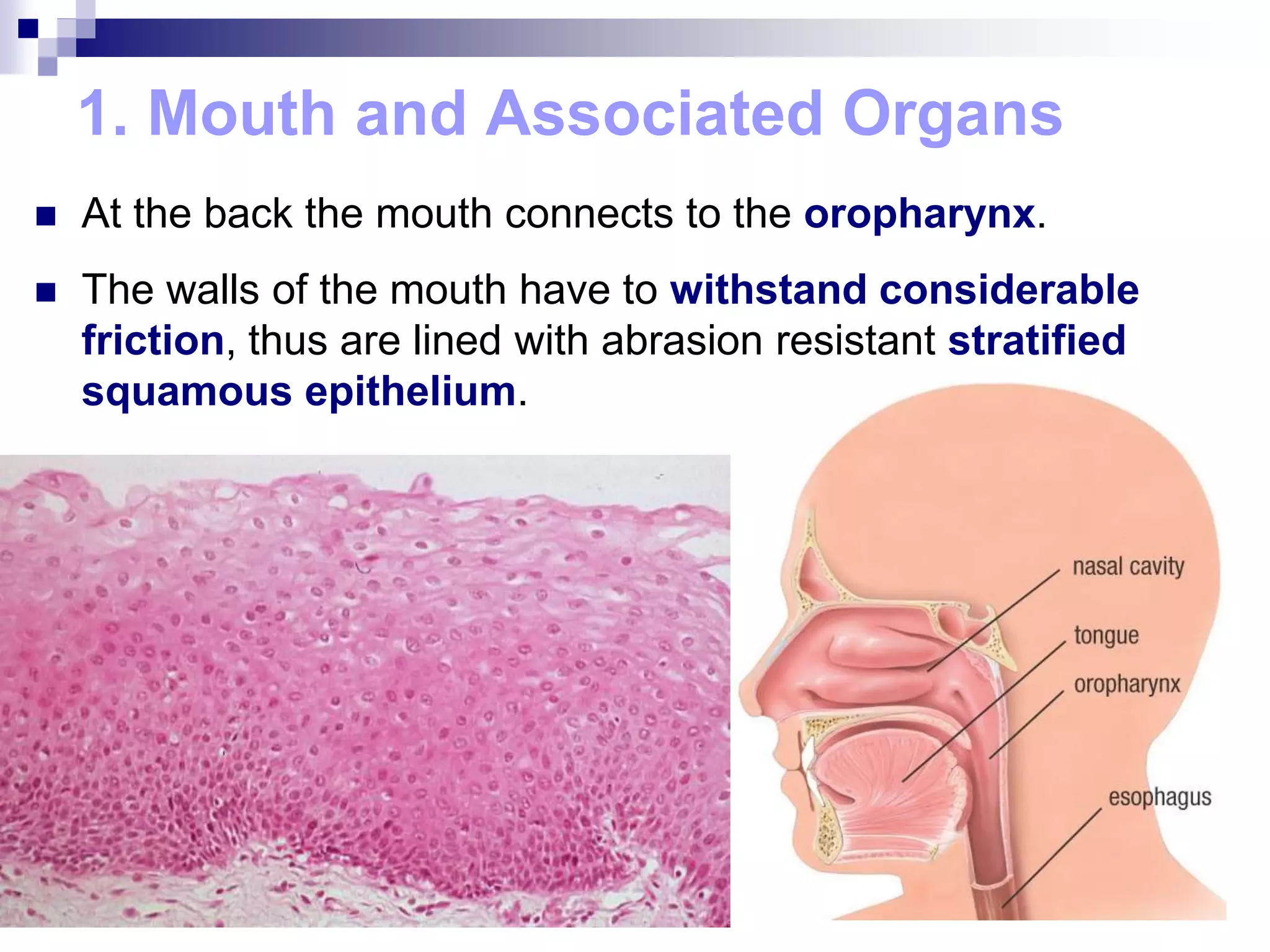
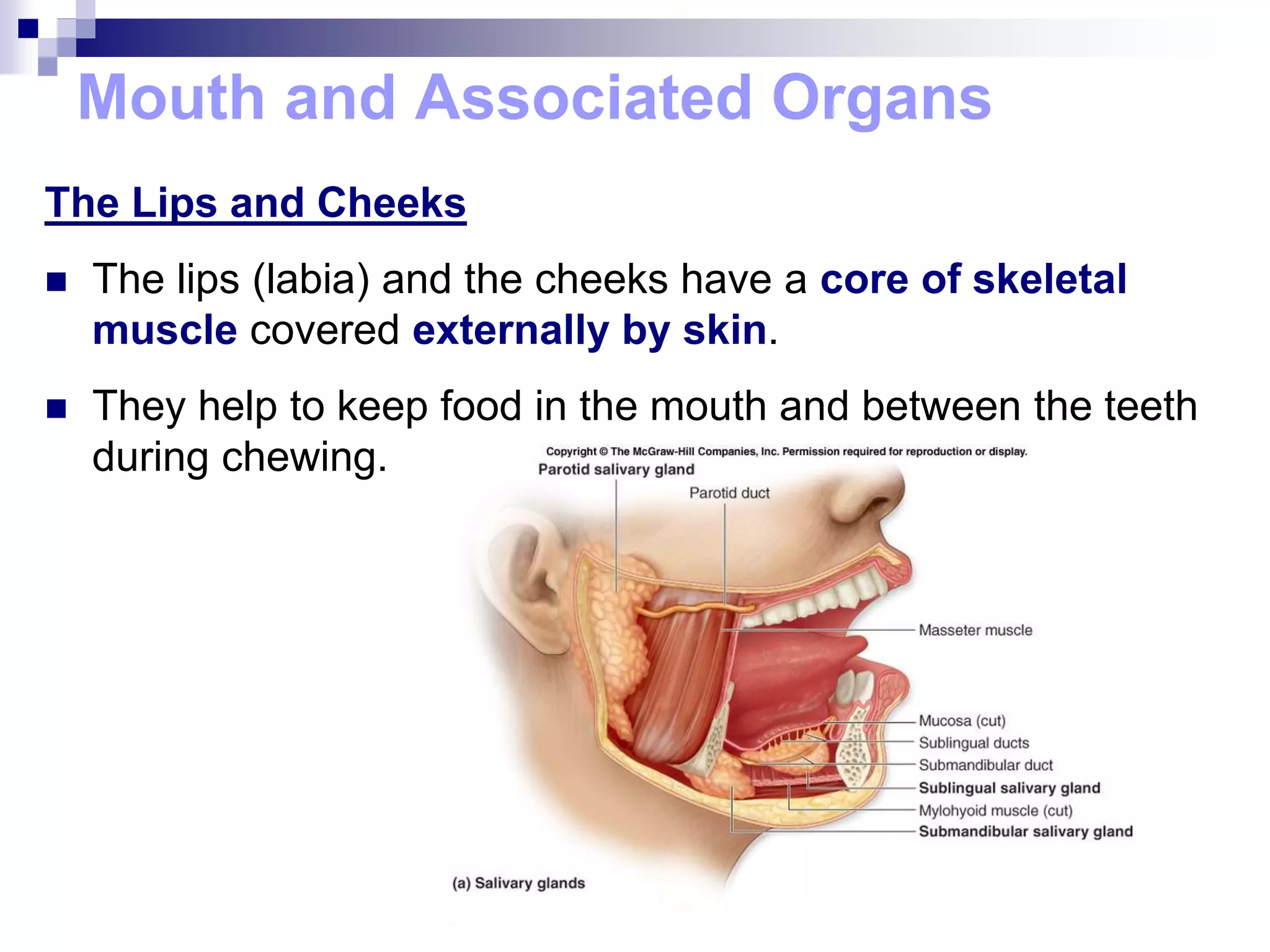
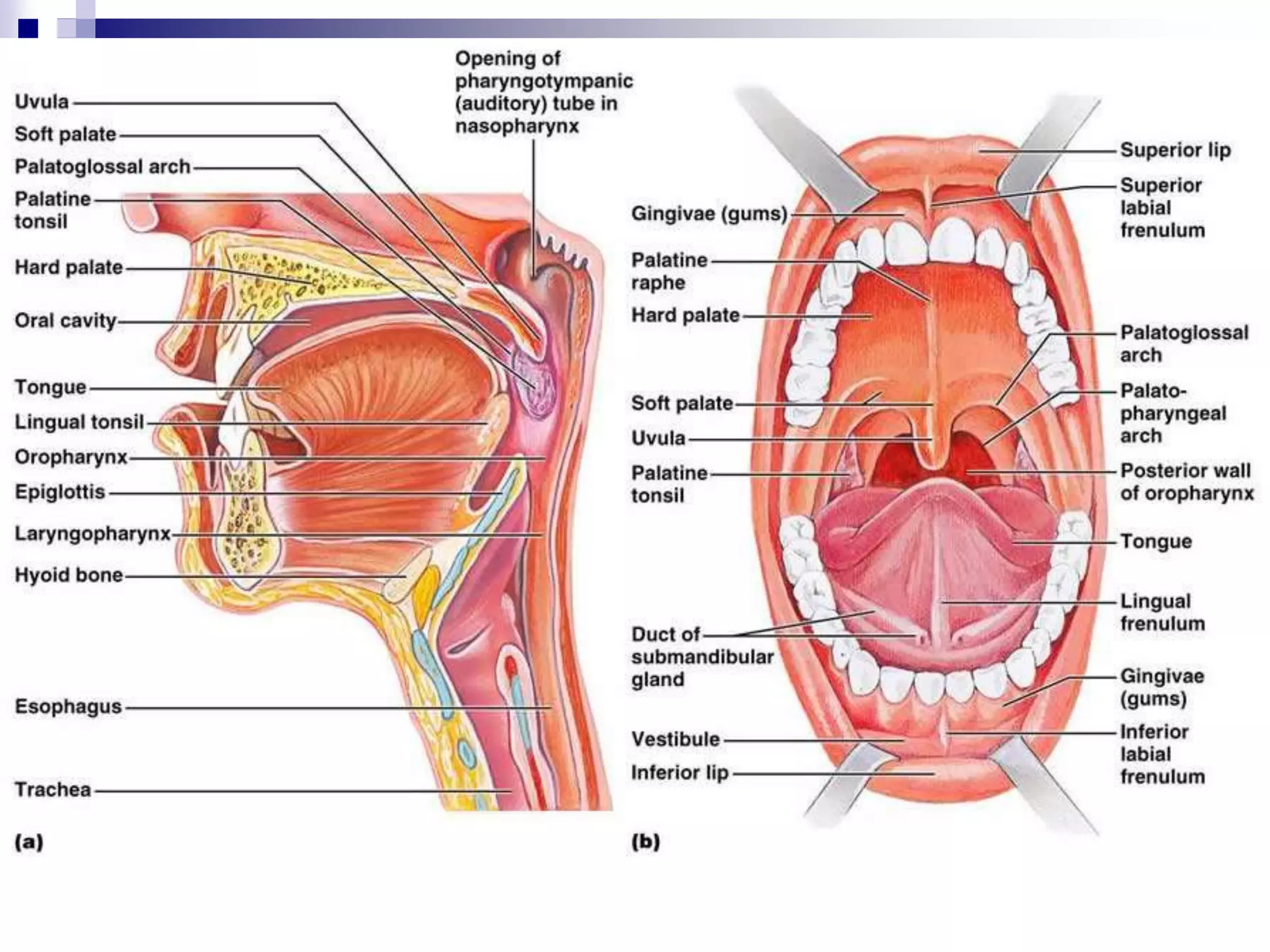
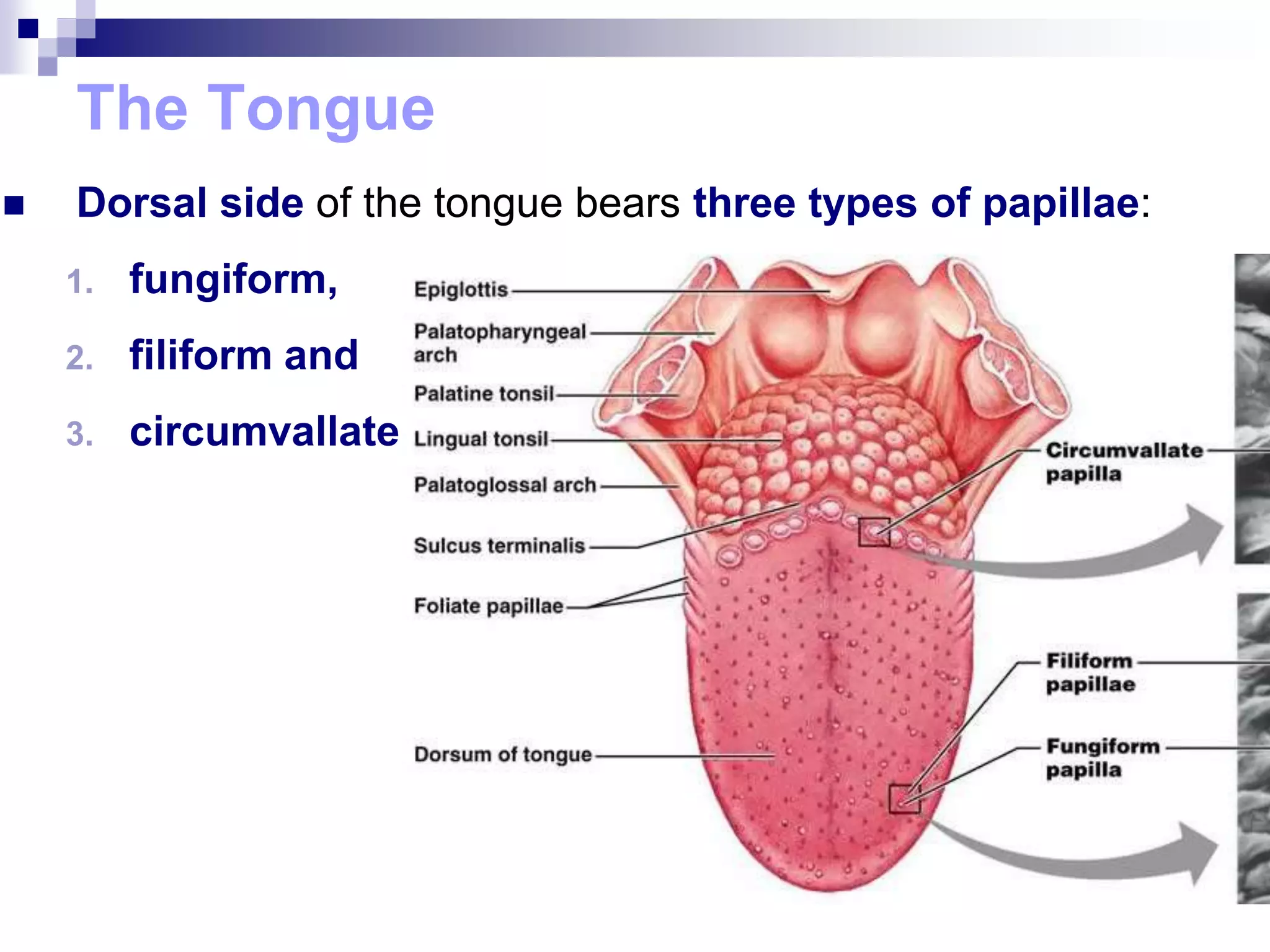
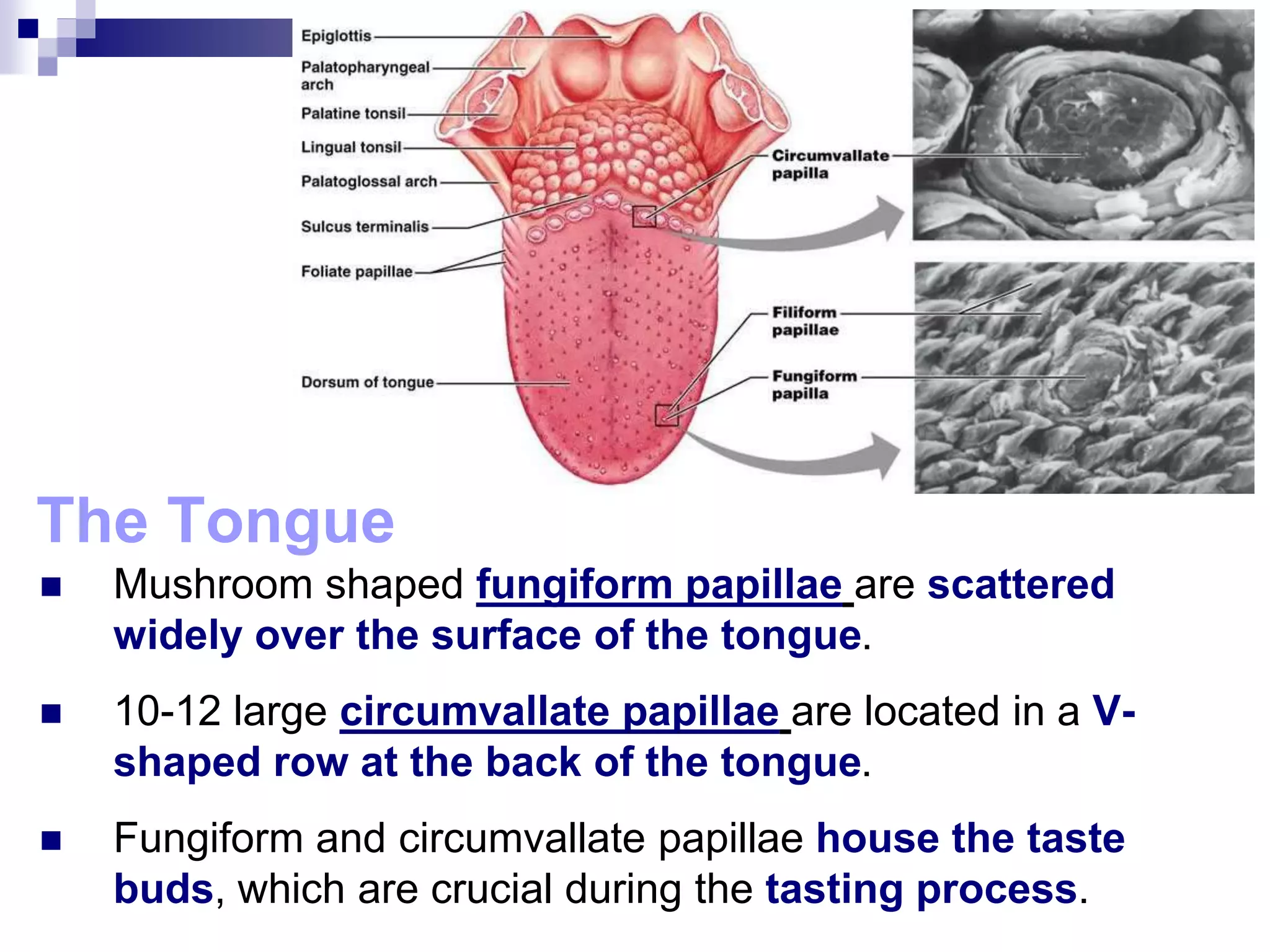
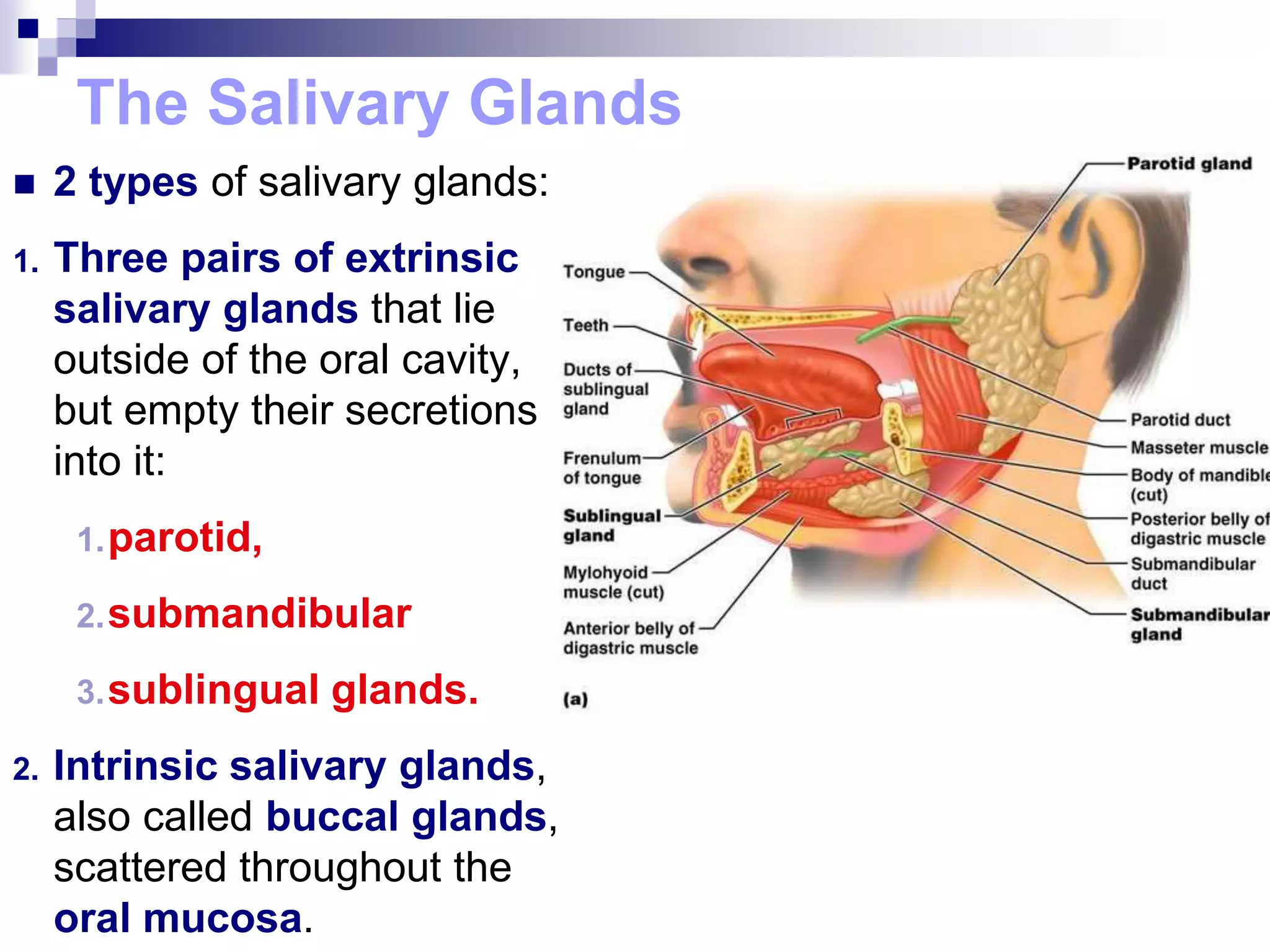
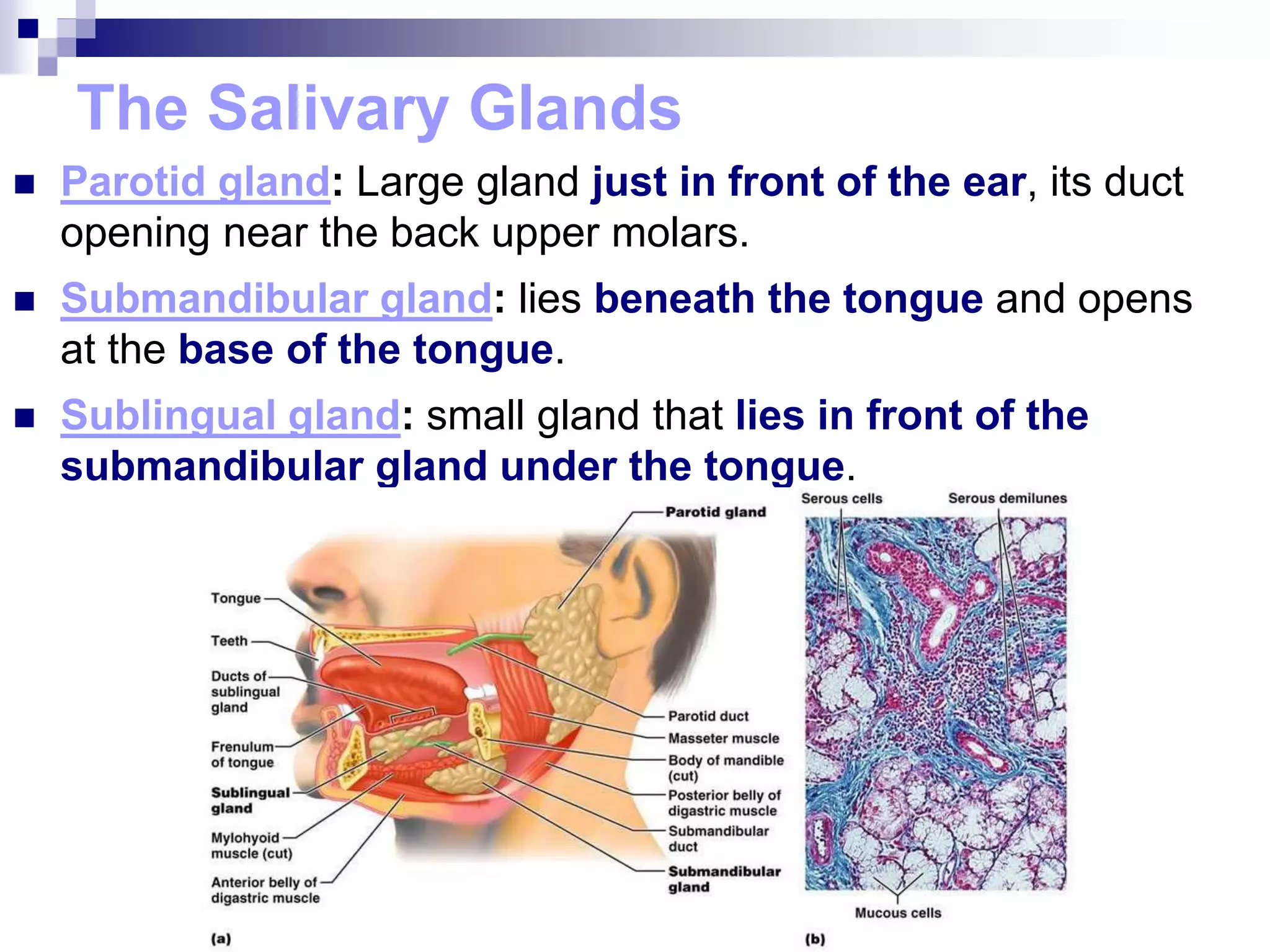
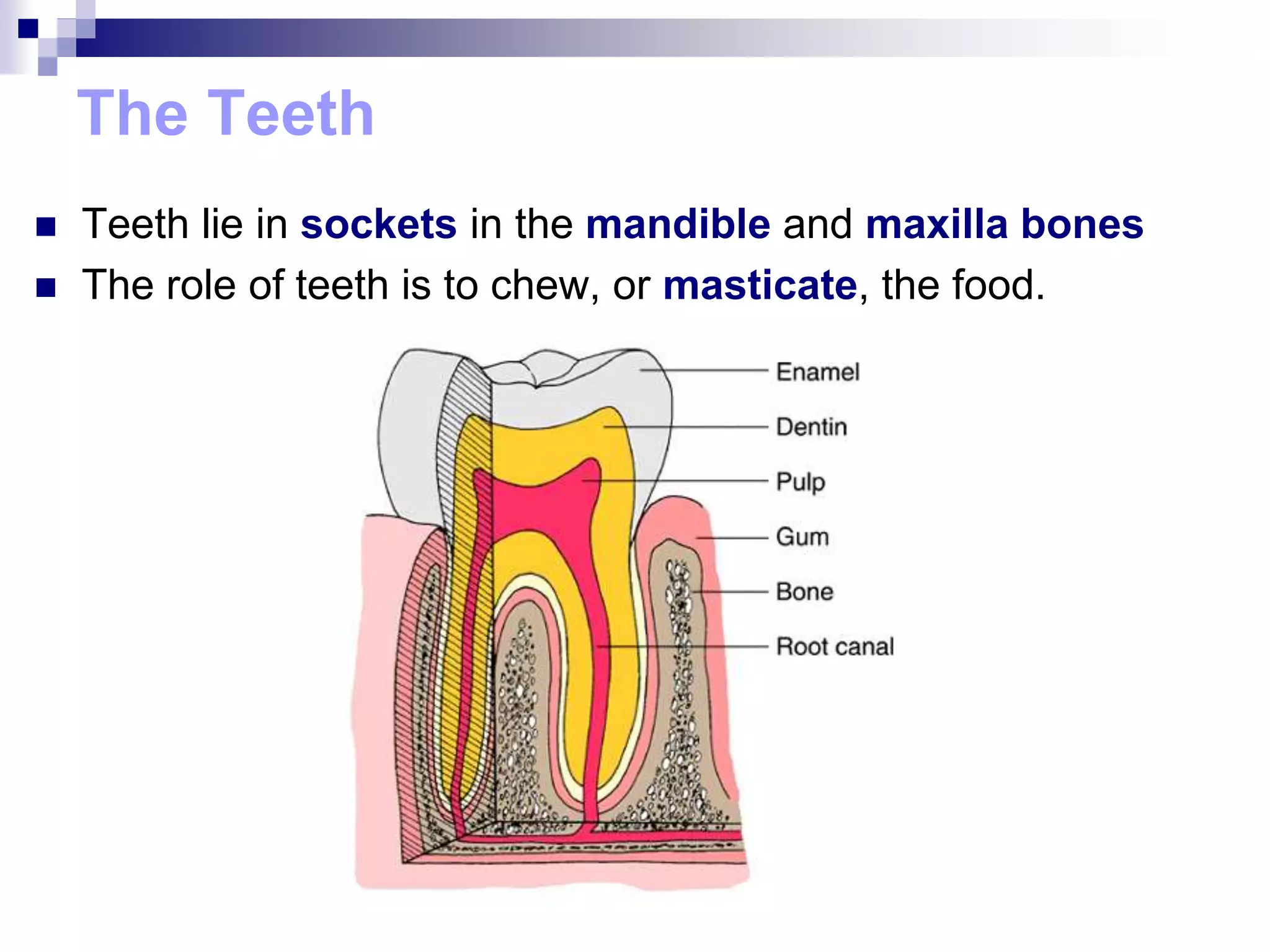
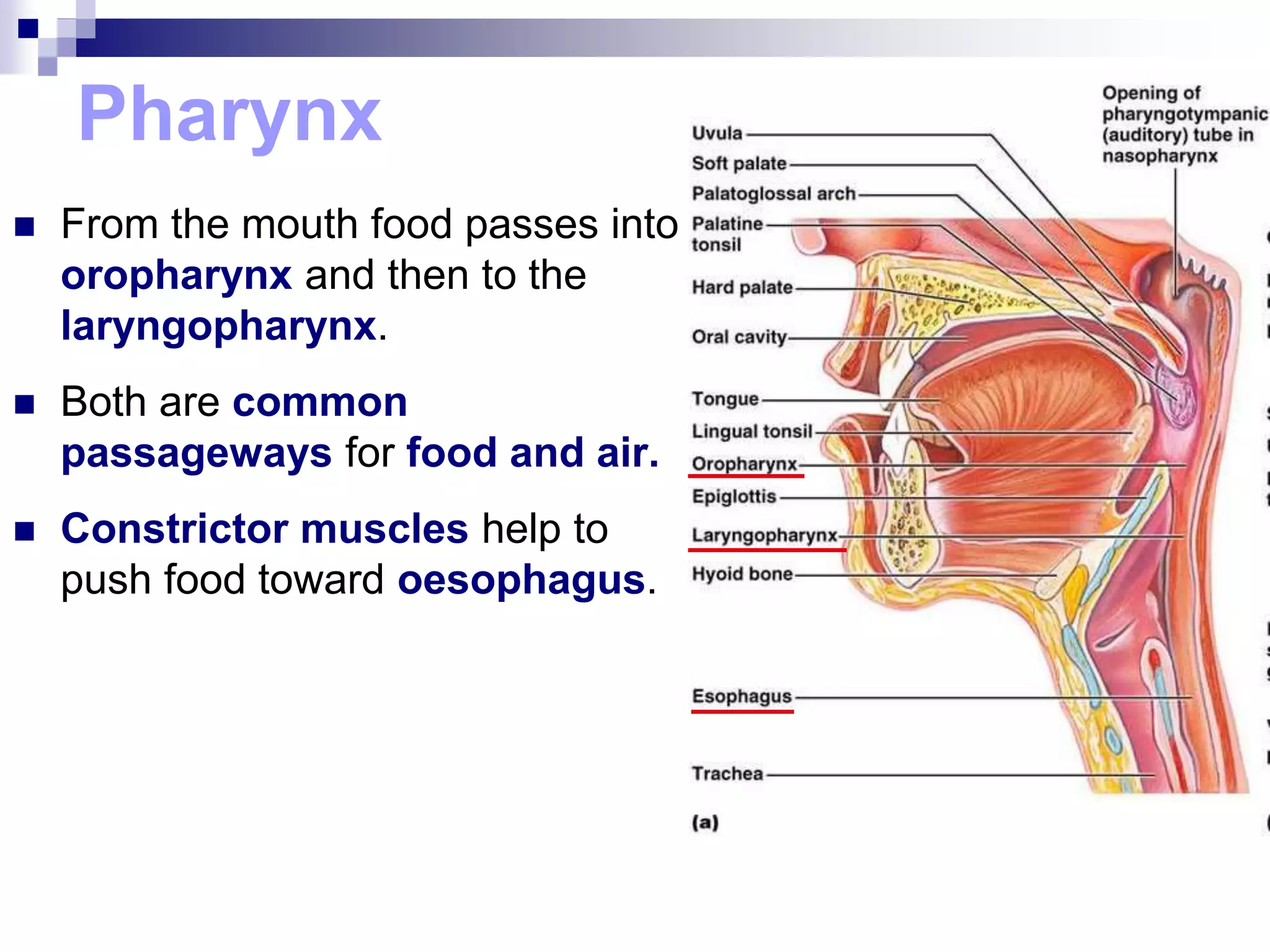
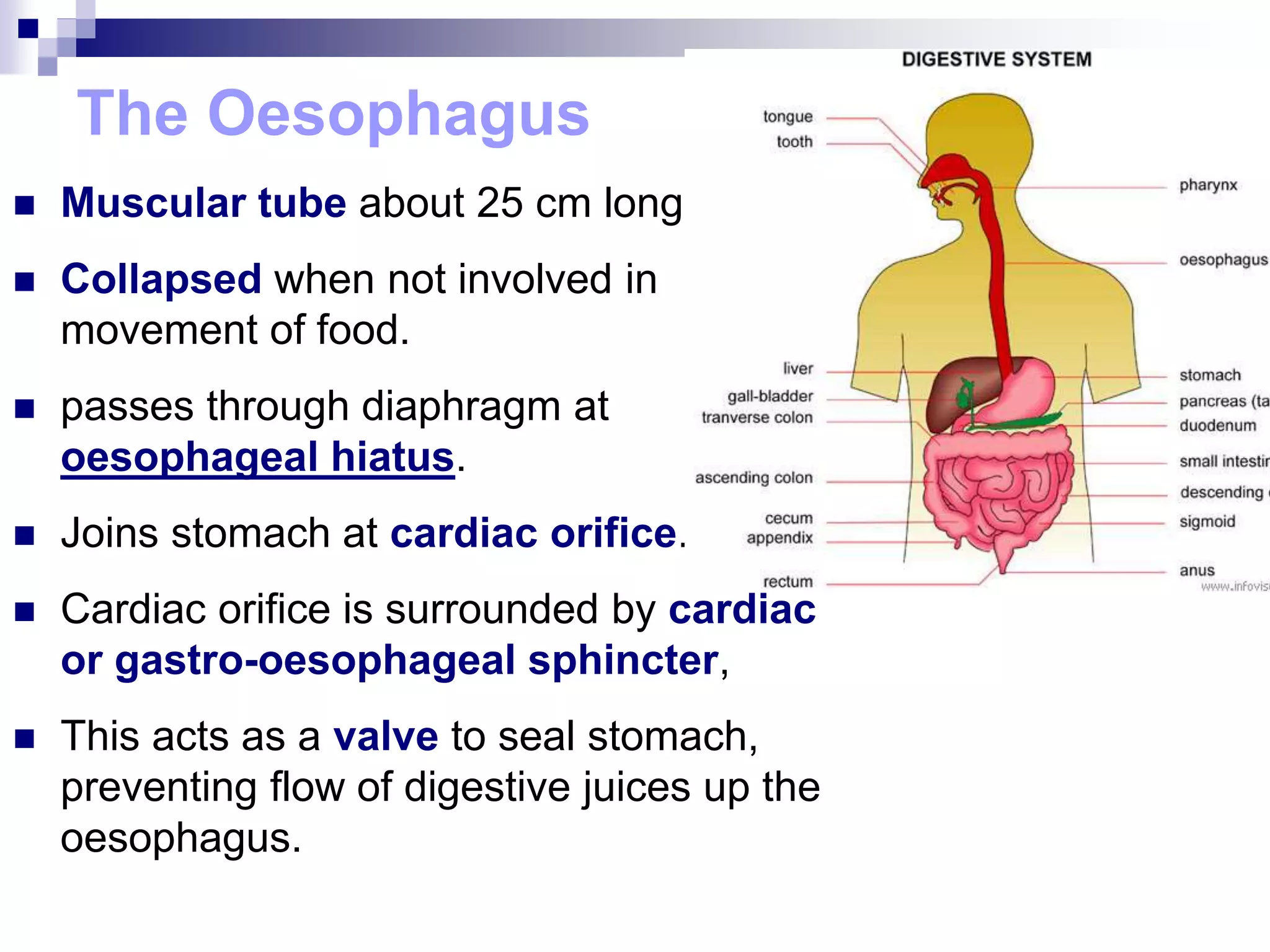
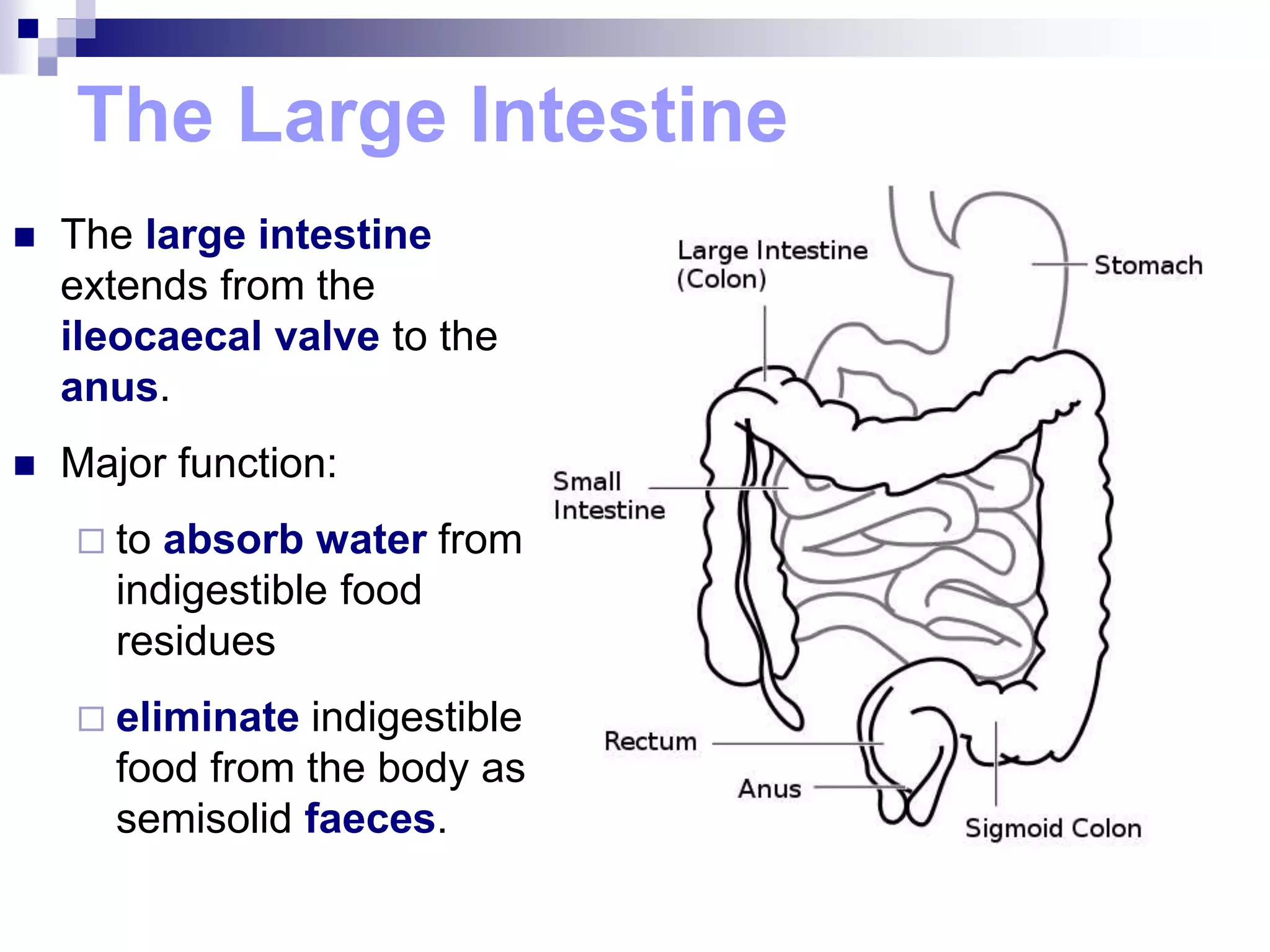
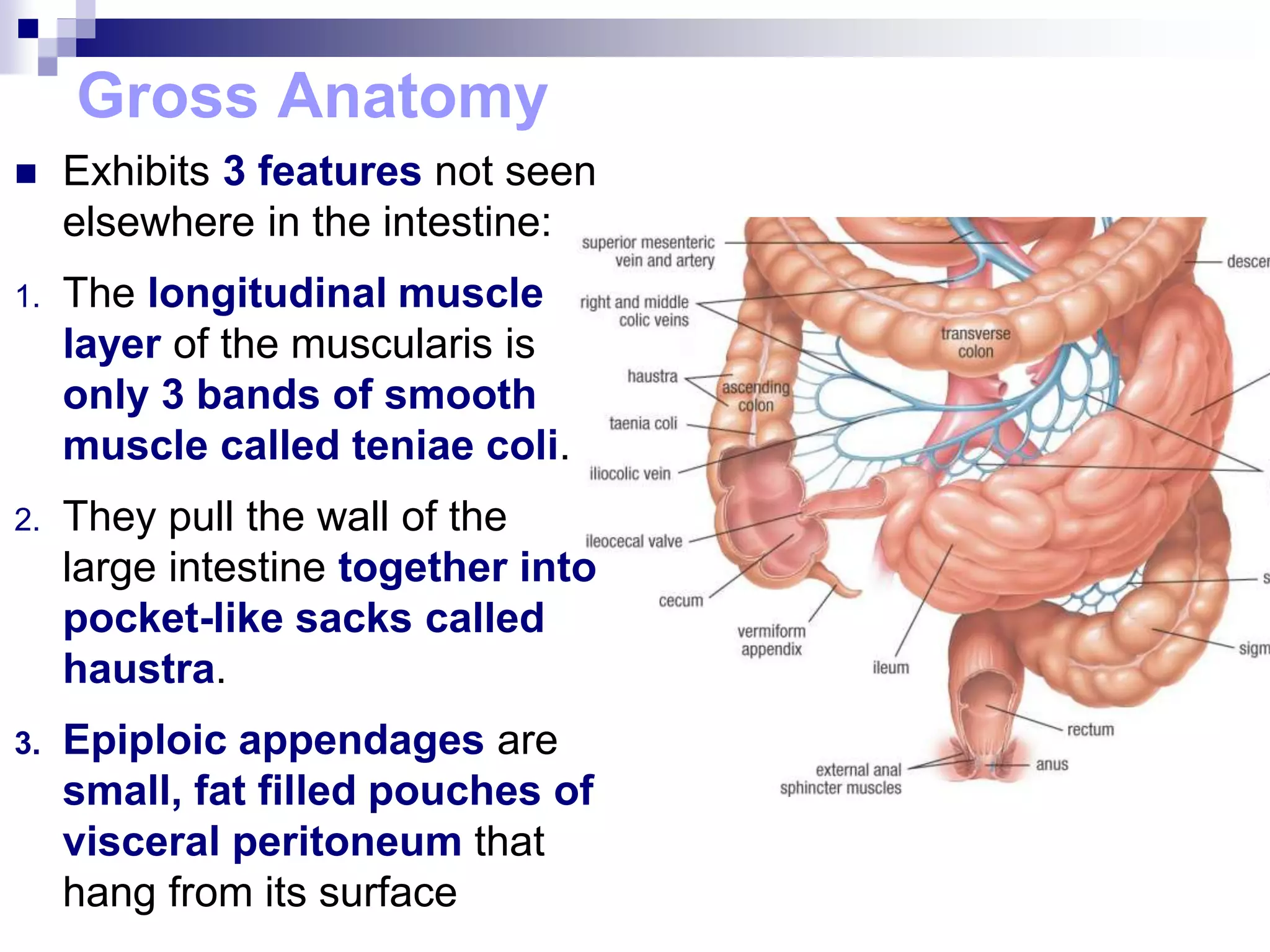
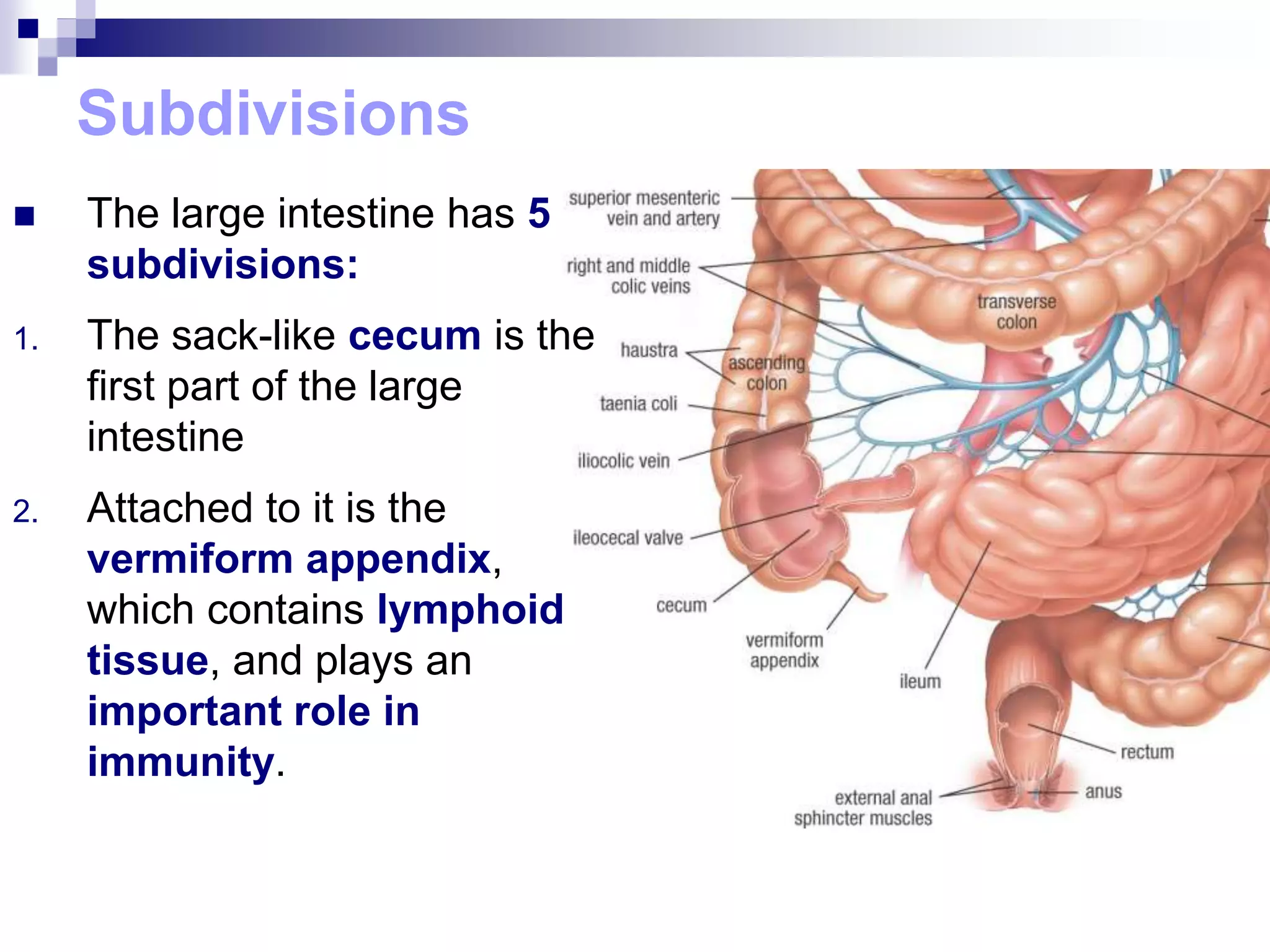
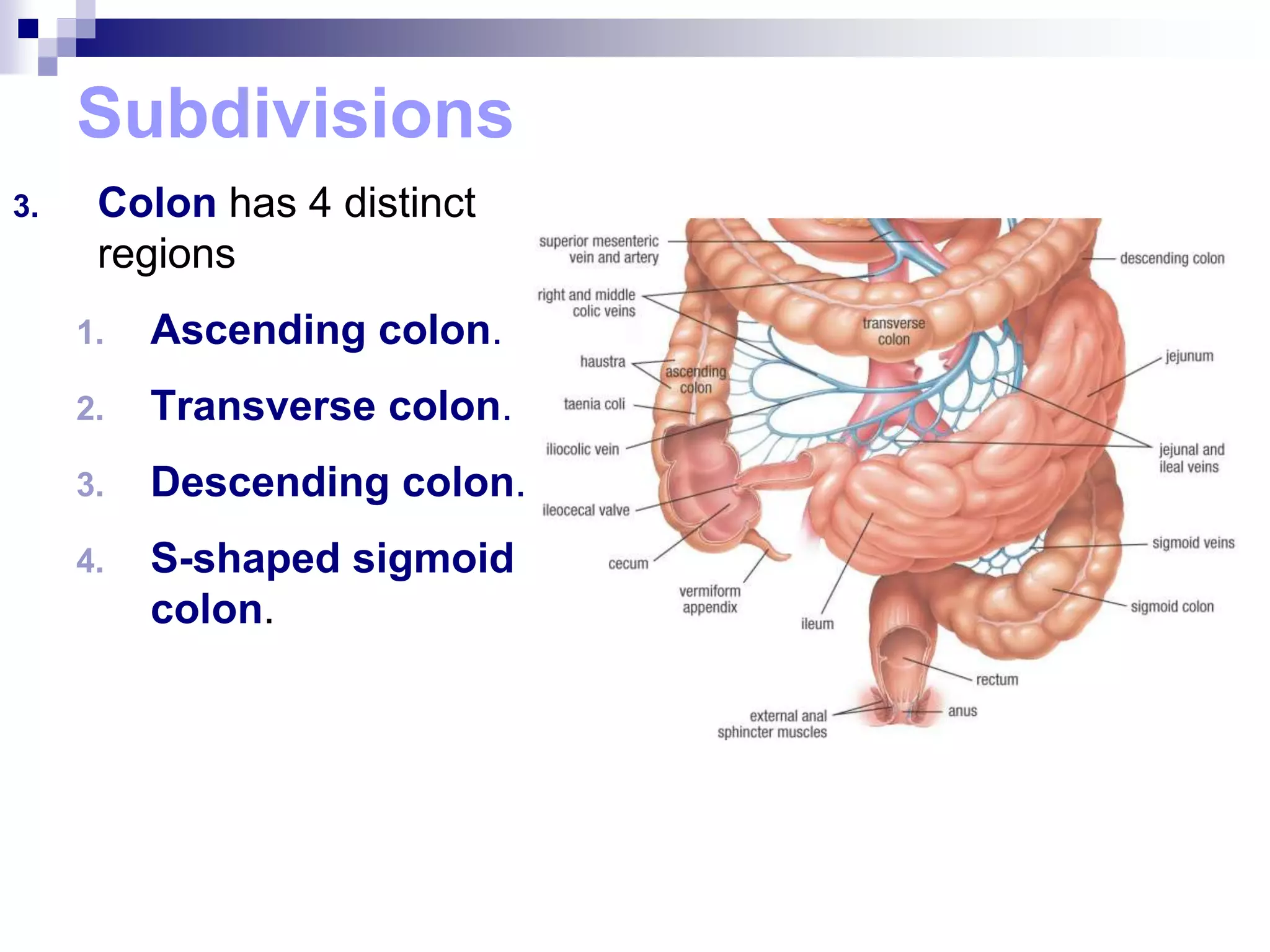
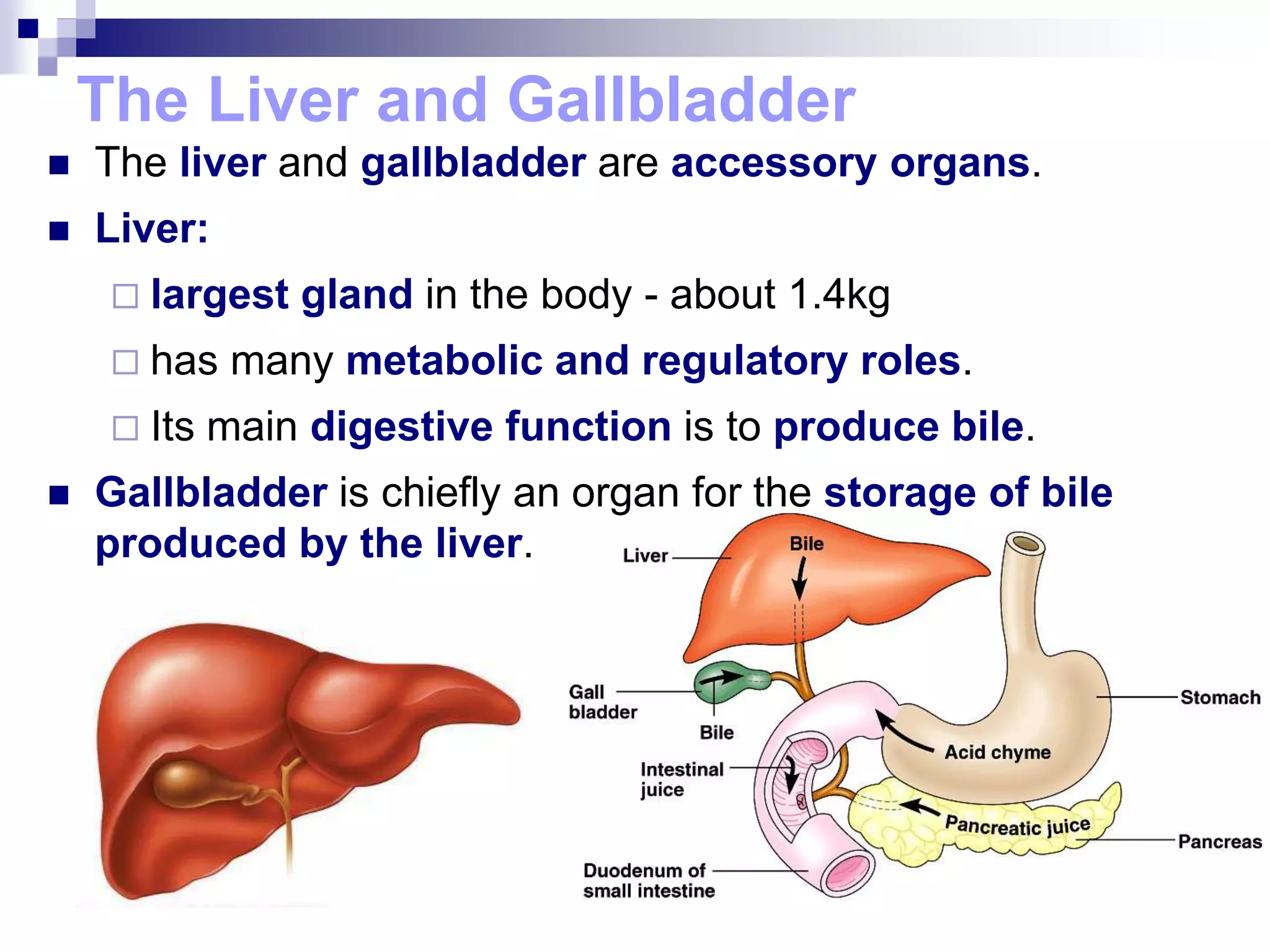
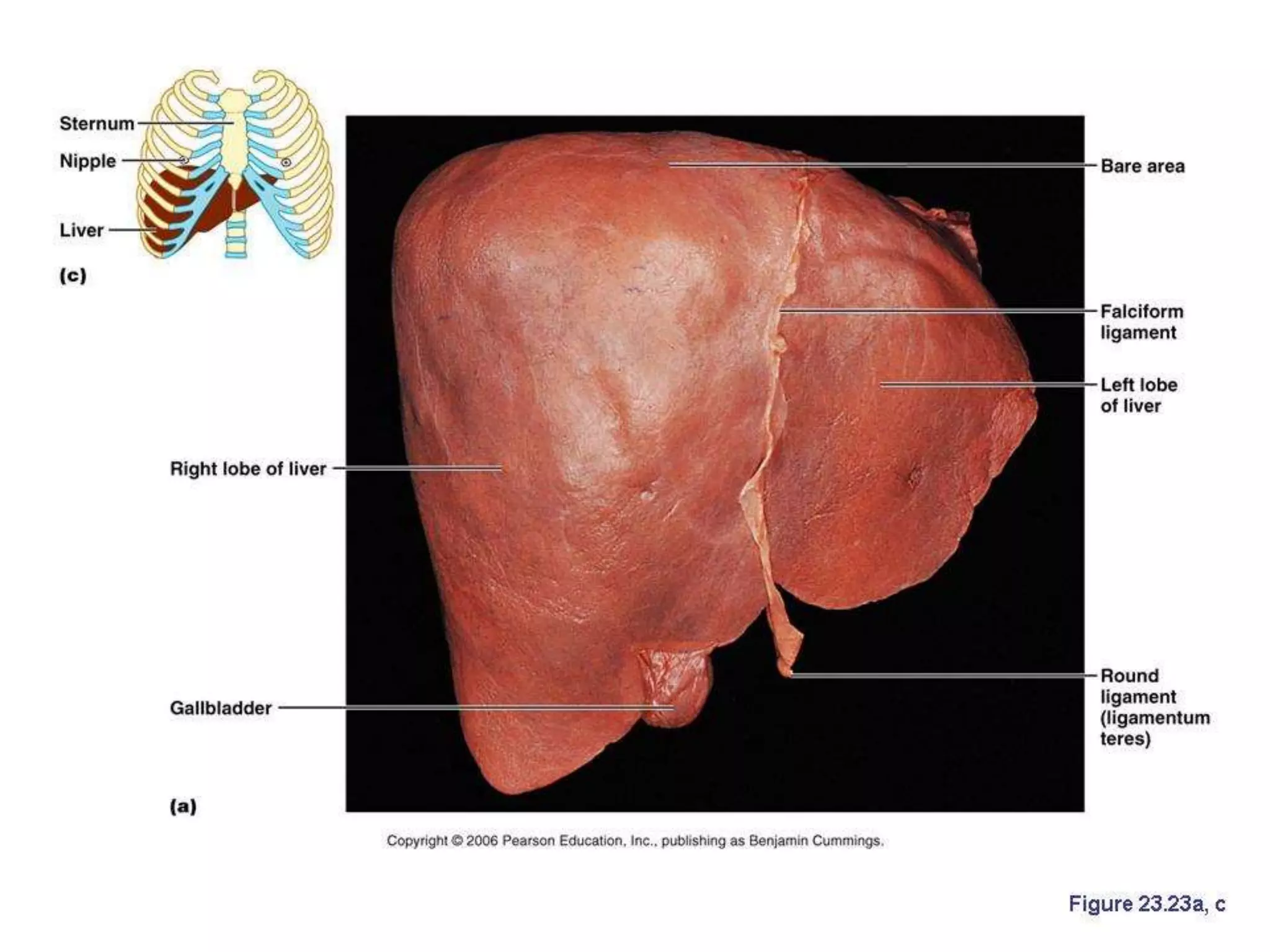
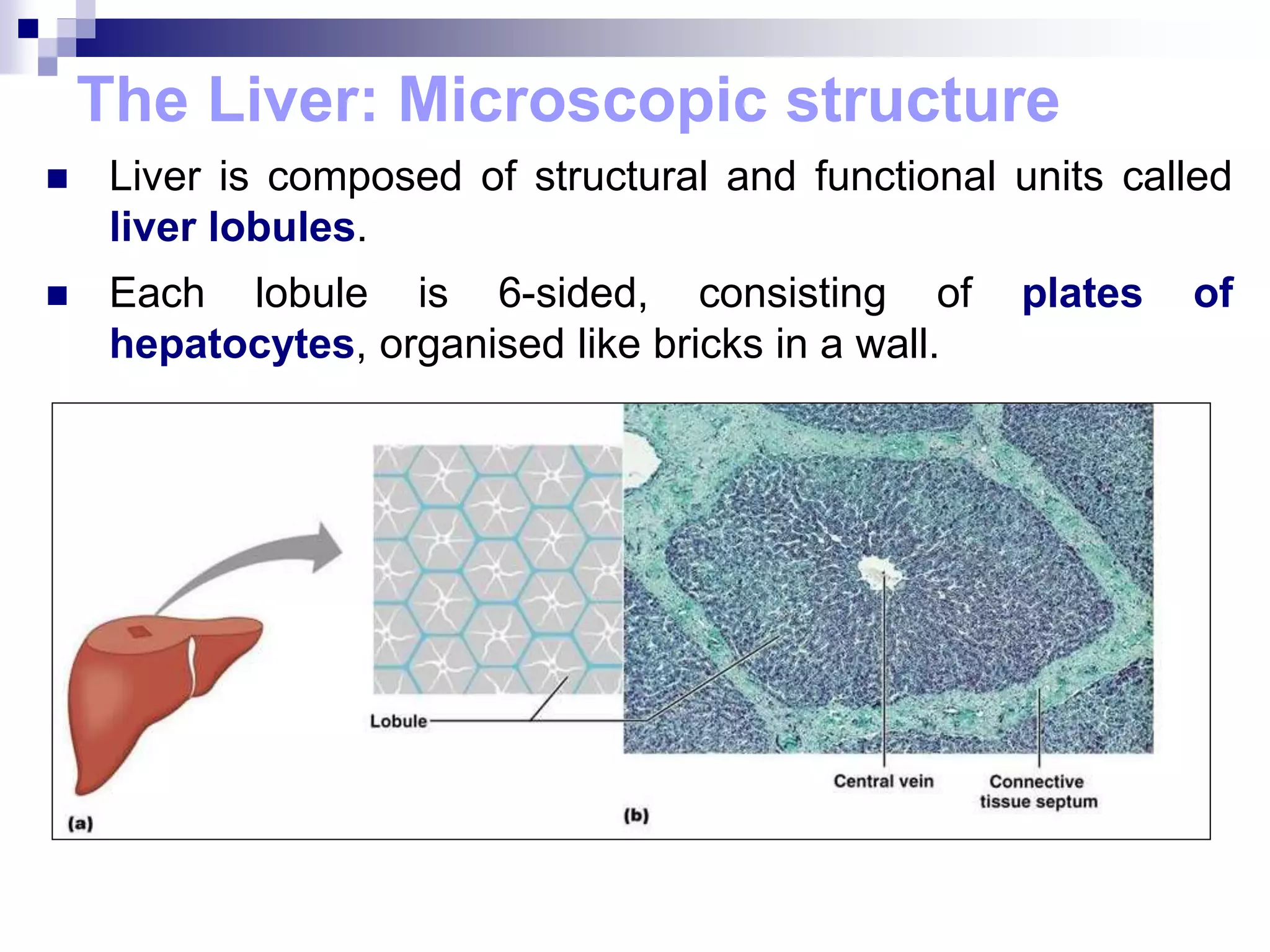
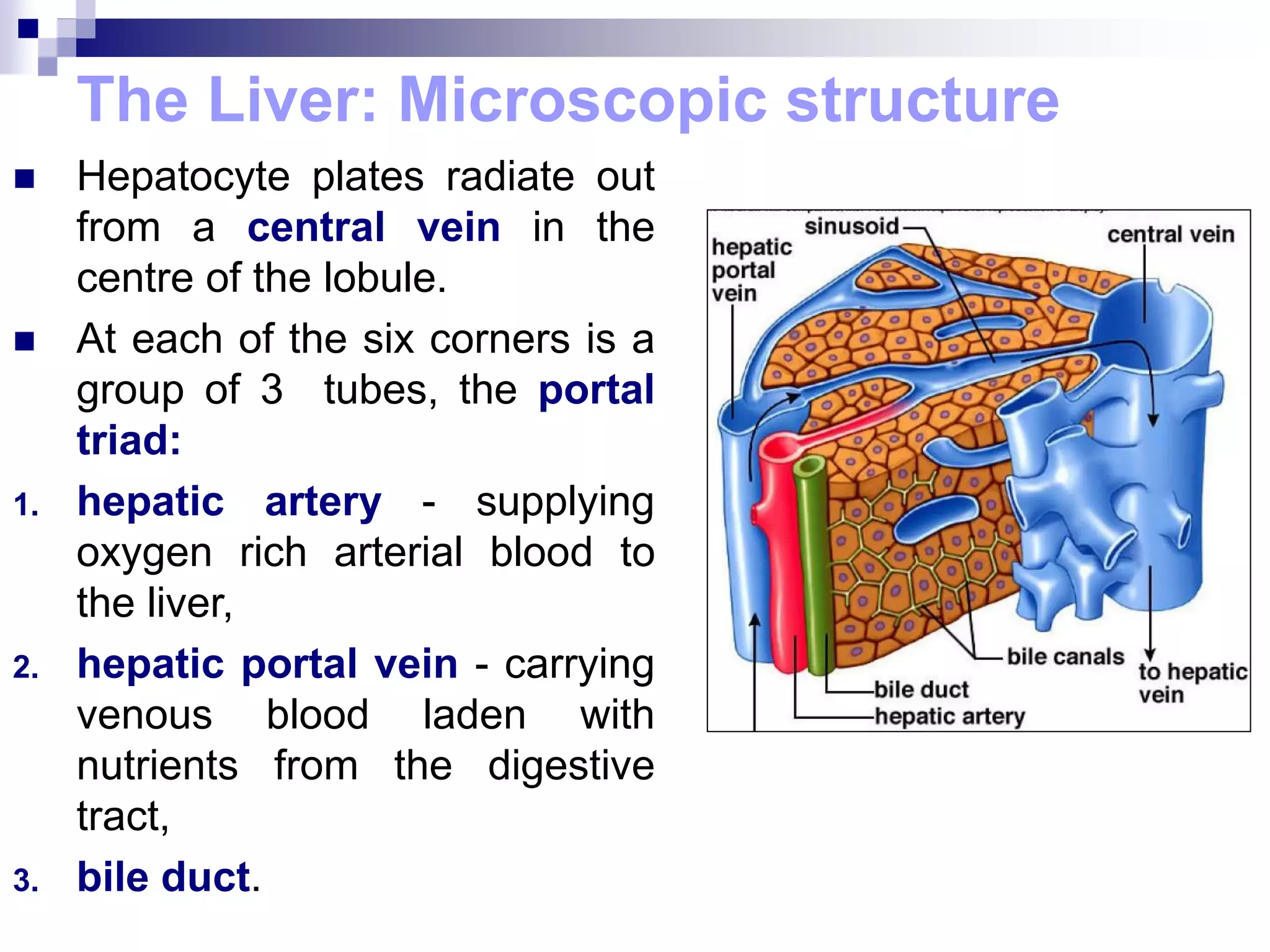
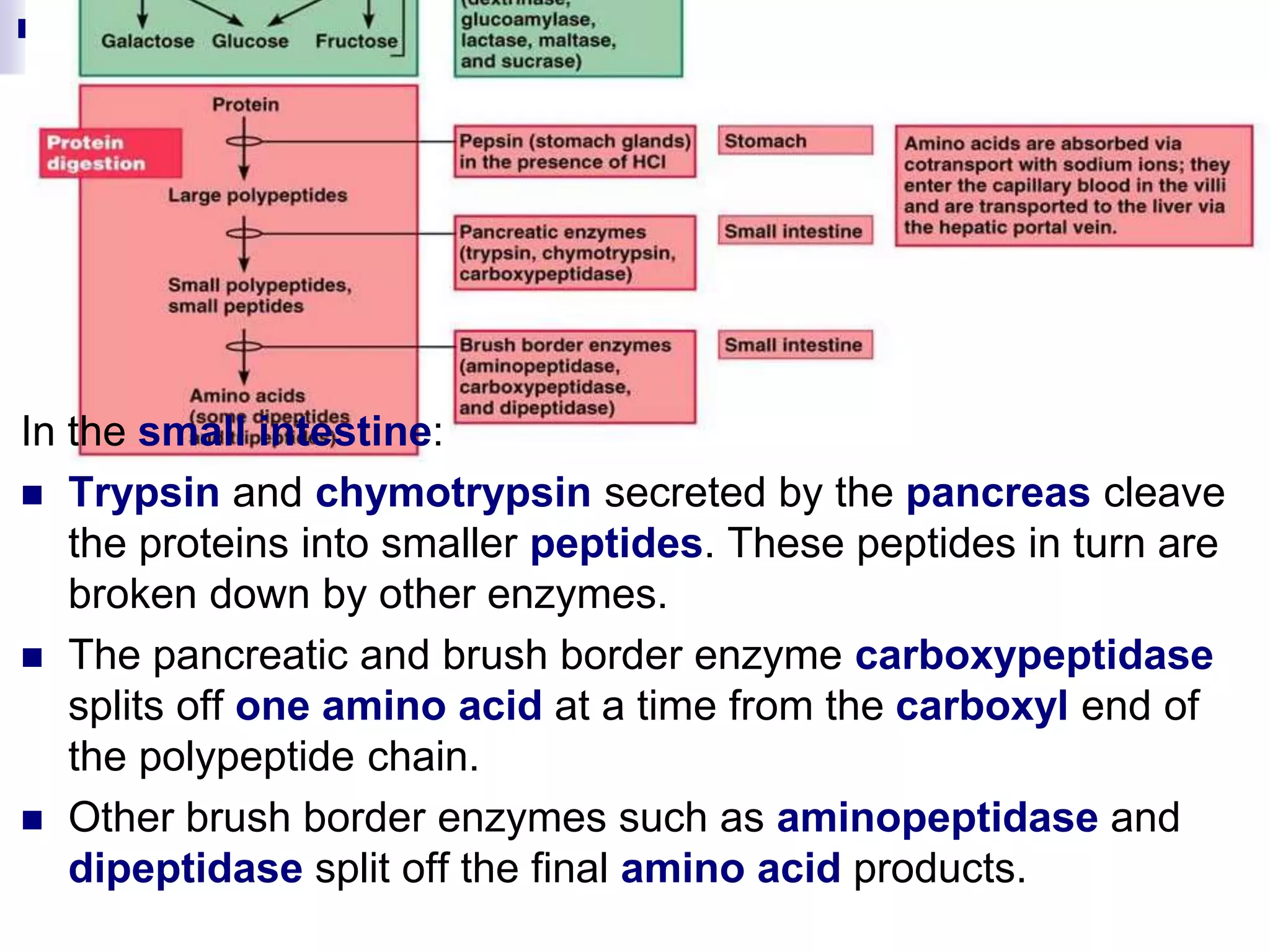
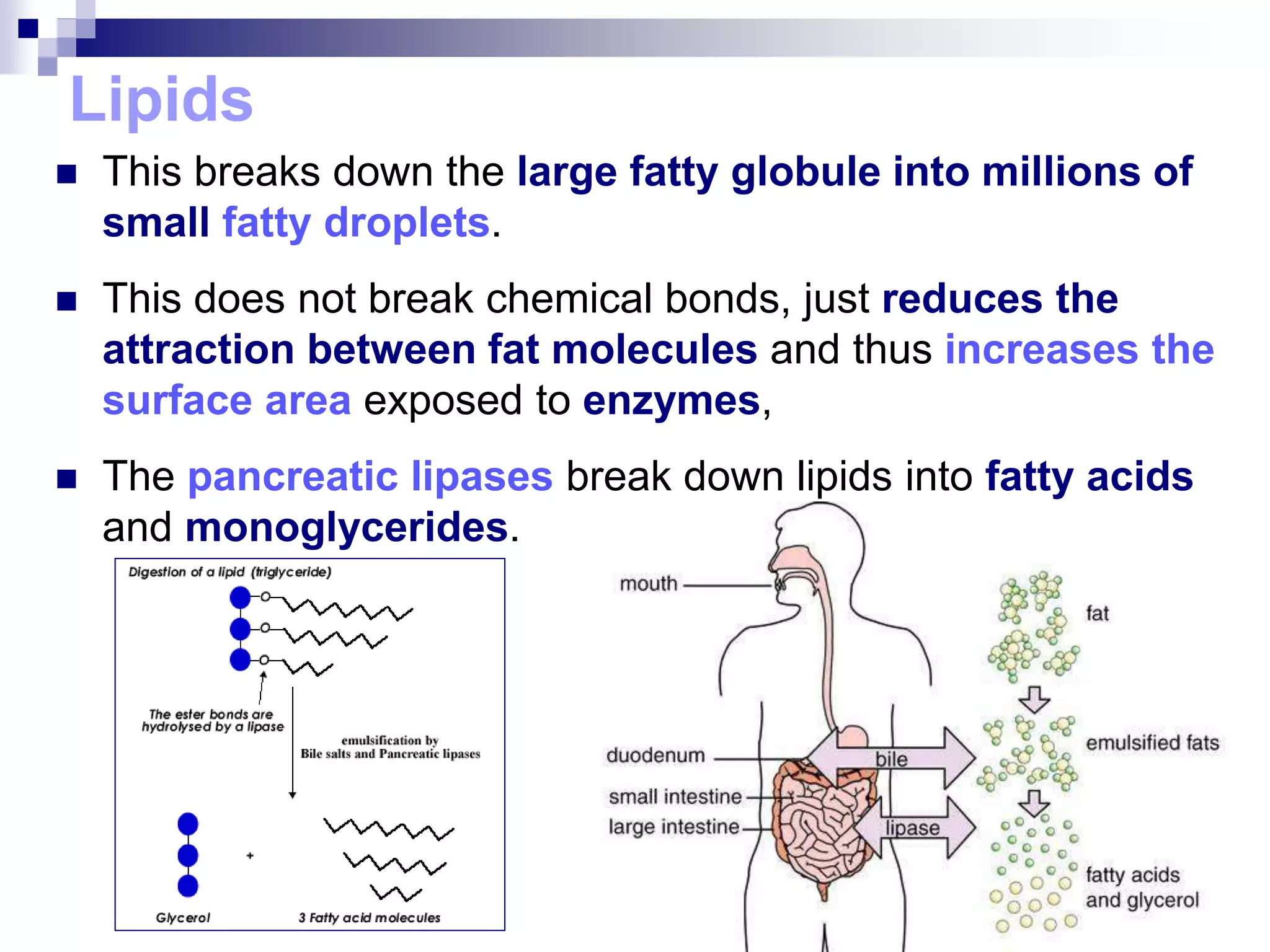
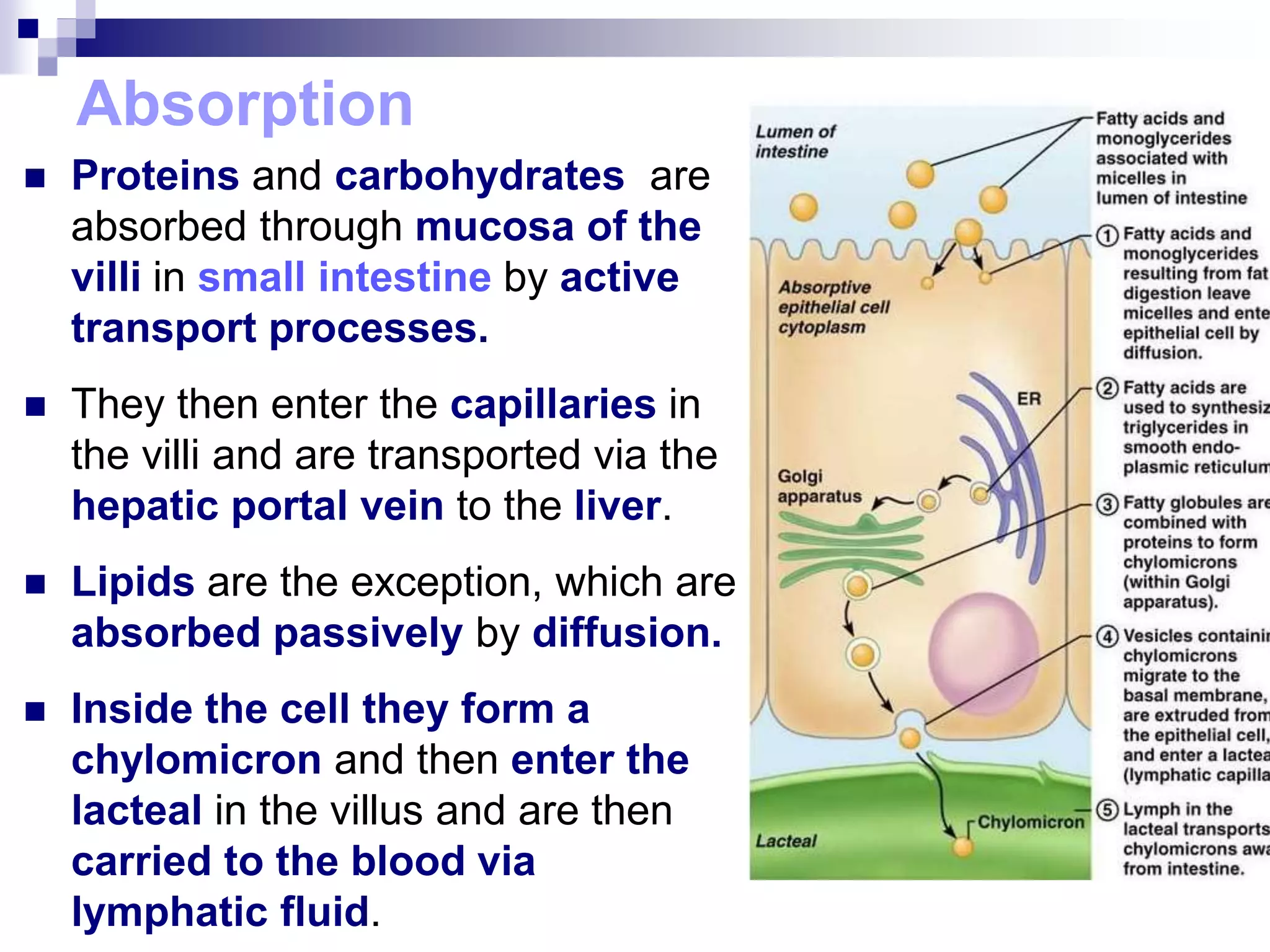
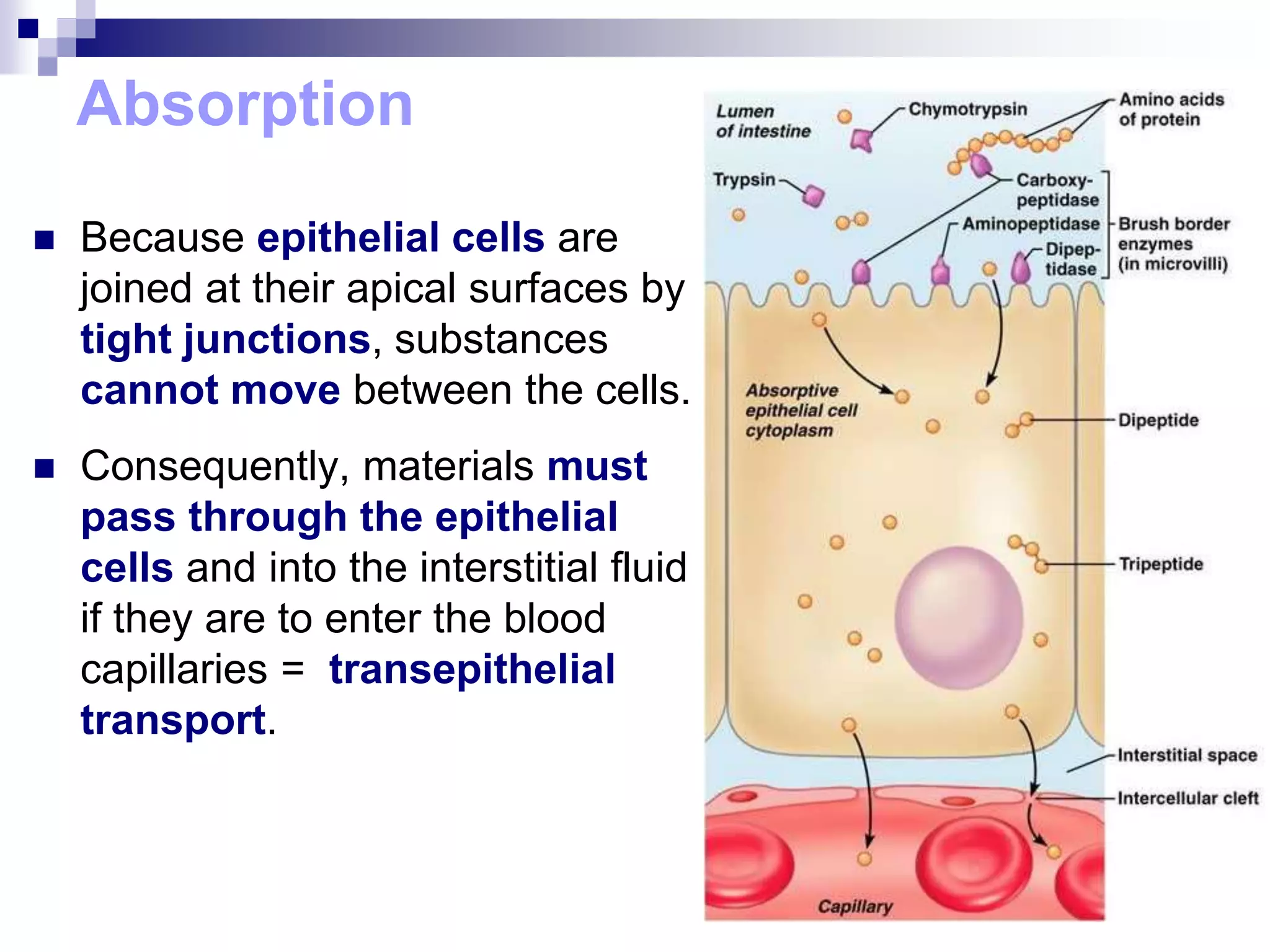
The digestive system consists of the alimentary canal and accessory organs. The alimentary canal includes the mouth, pharynx, esophagus, stomach, small intestine, and large intestine. Accessory organs include the teeth, tongue, liver, gallbladder, and pancreas. Food is ingested and moves through the digestive tract, where it undergoes mechanical and chemical digestion to break nutrients into smaller molecules that can be absorbed and used by the body. Enzymes produced in glands aid in digestion at different points along the tract.