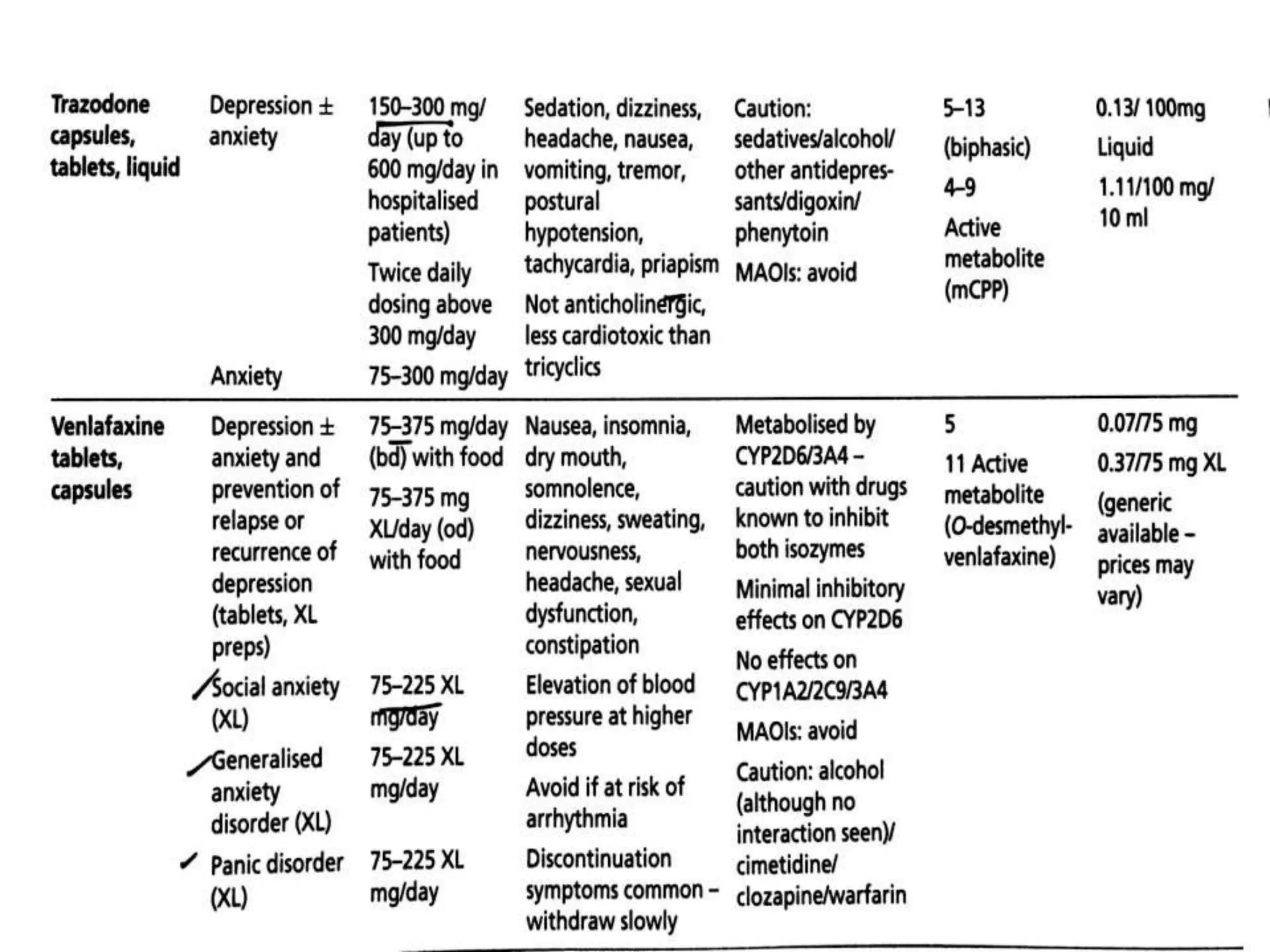
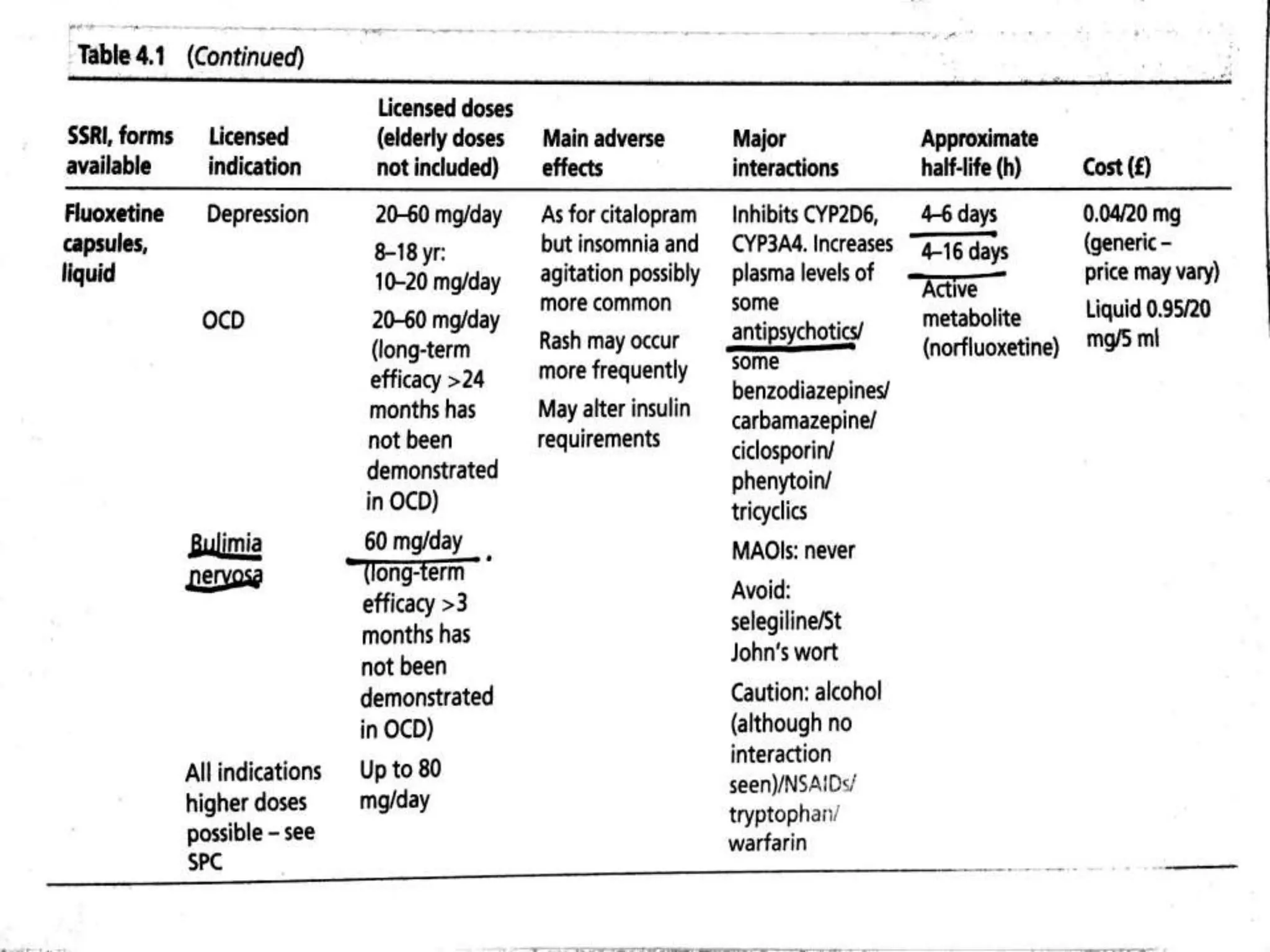
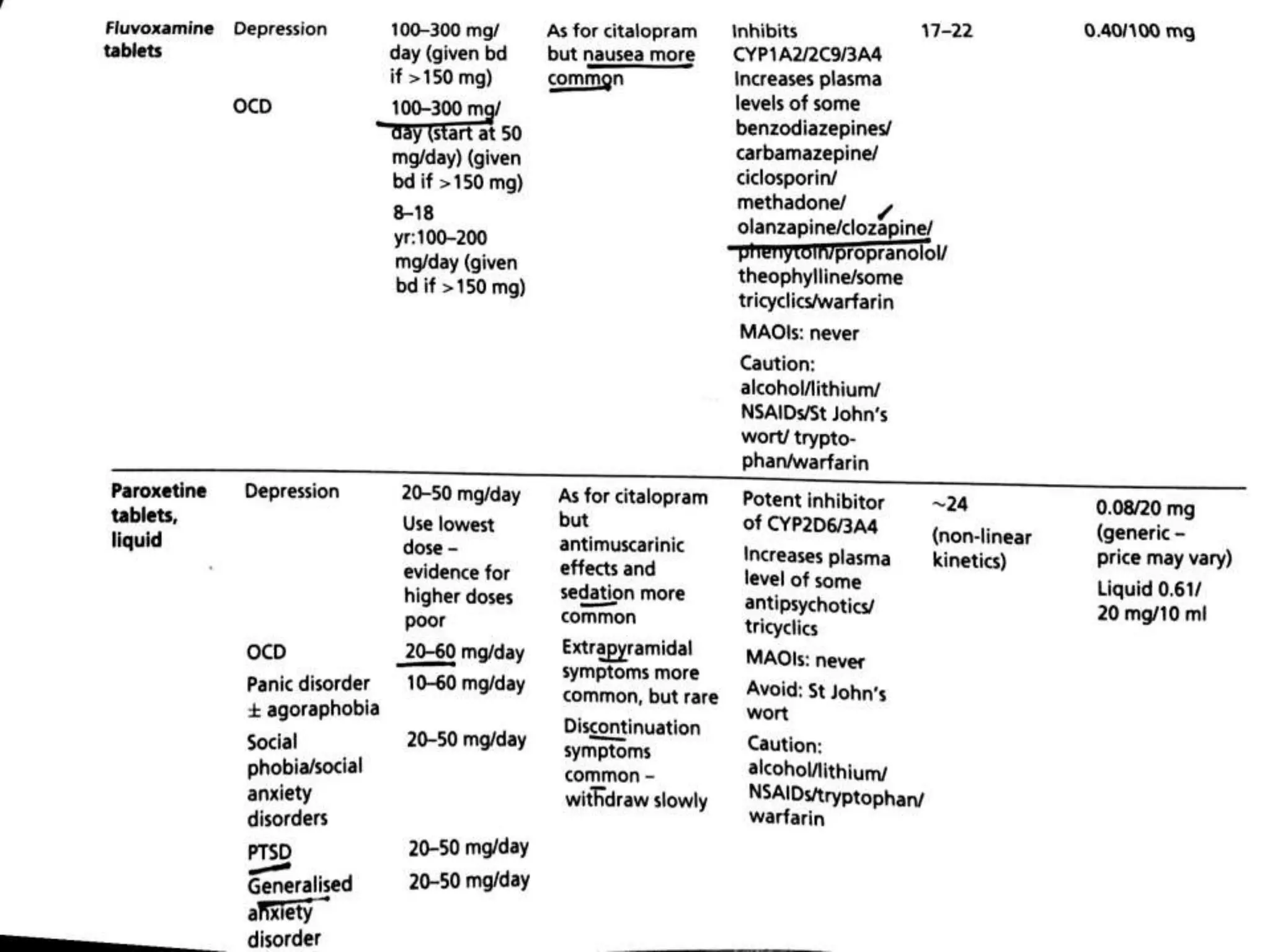
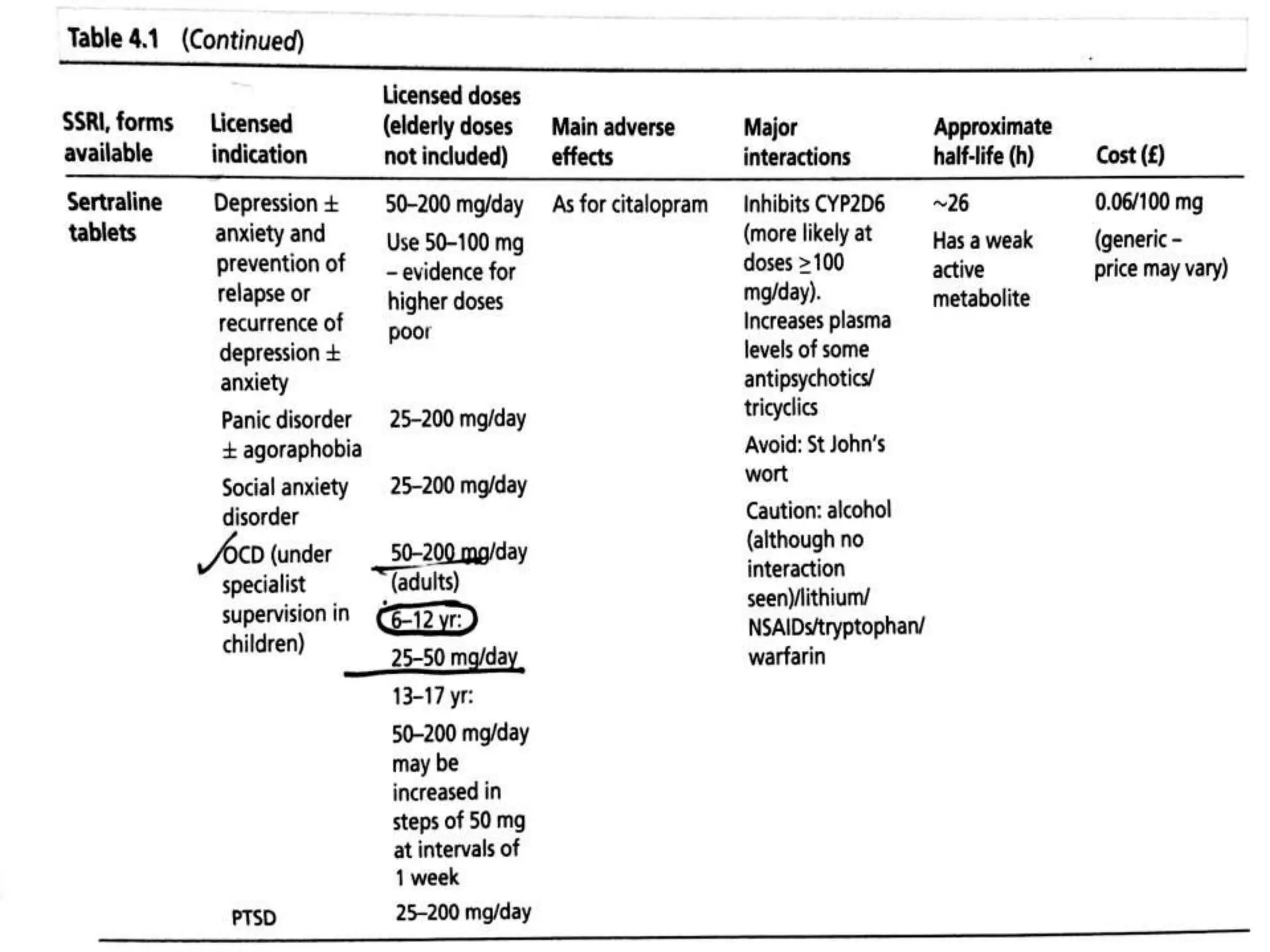
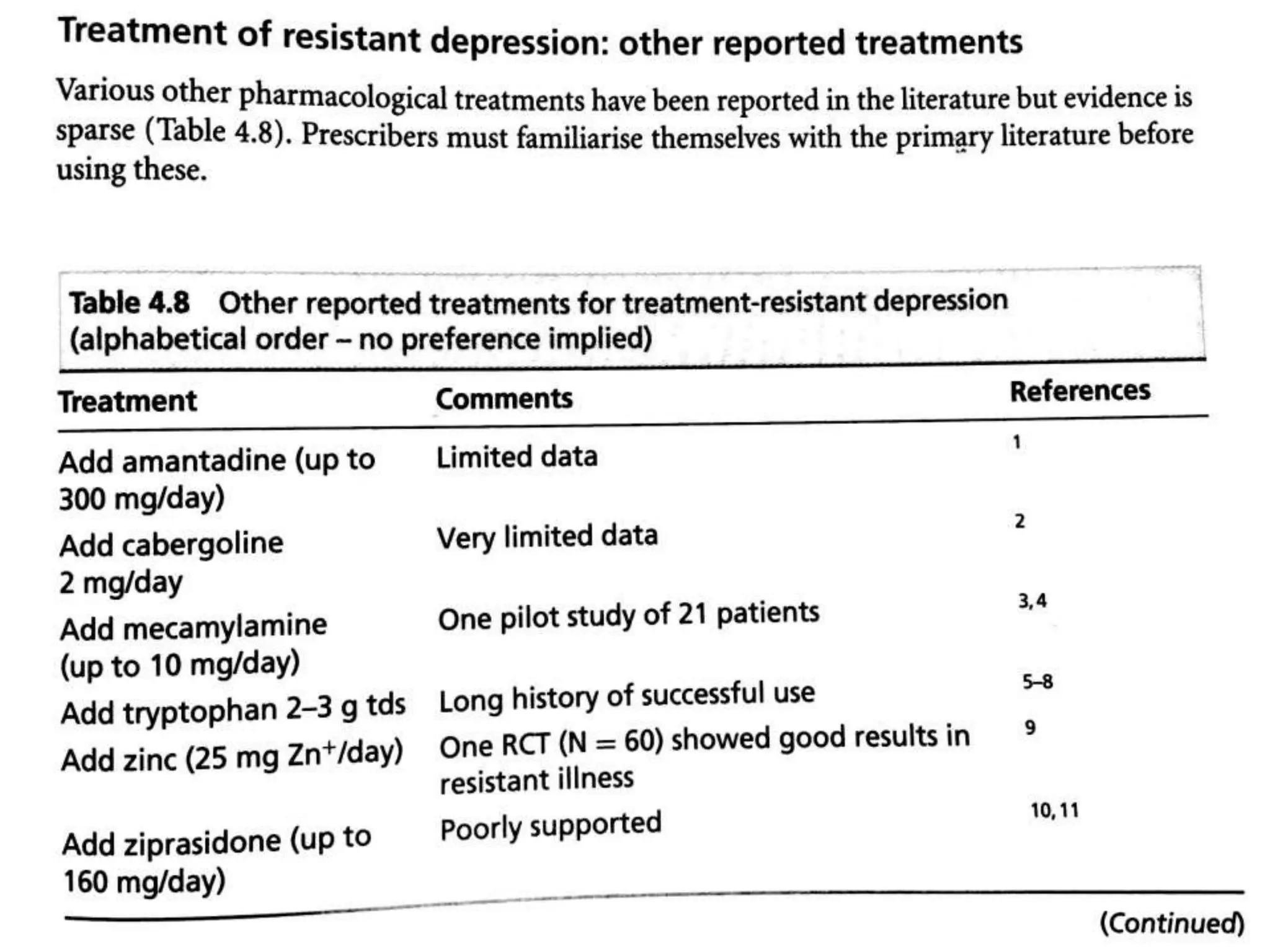
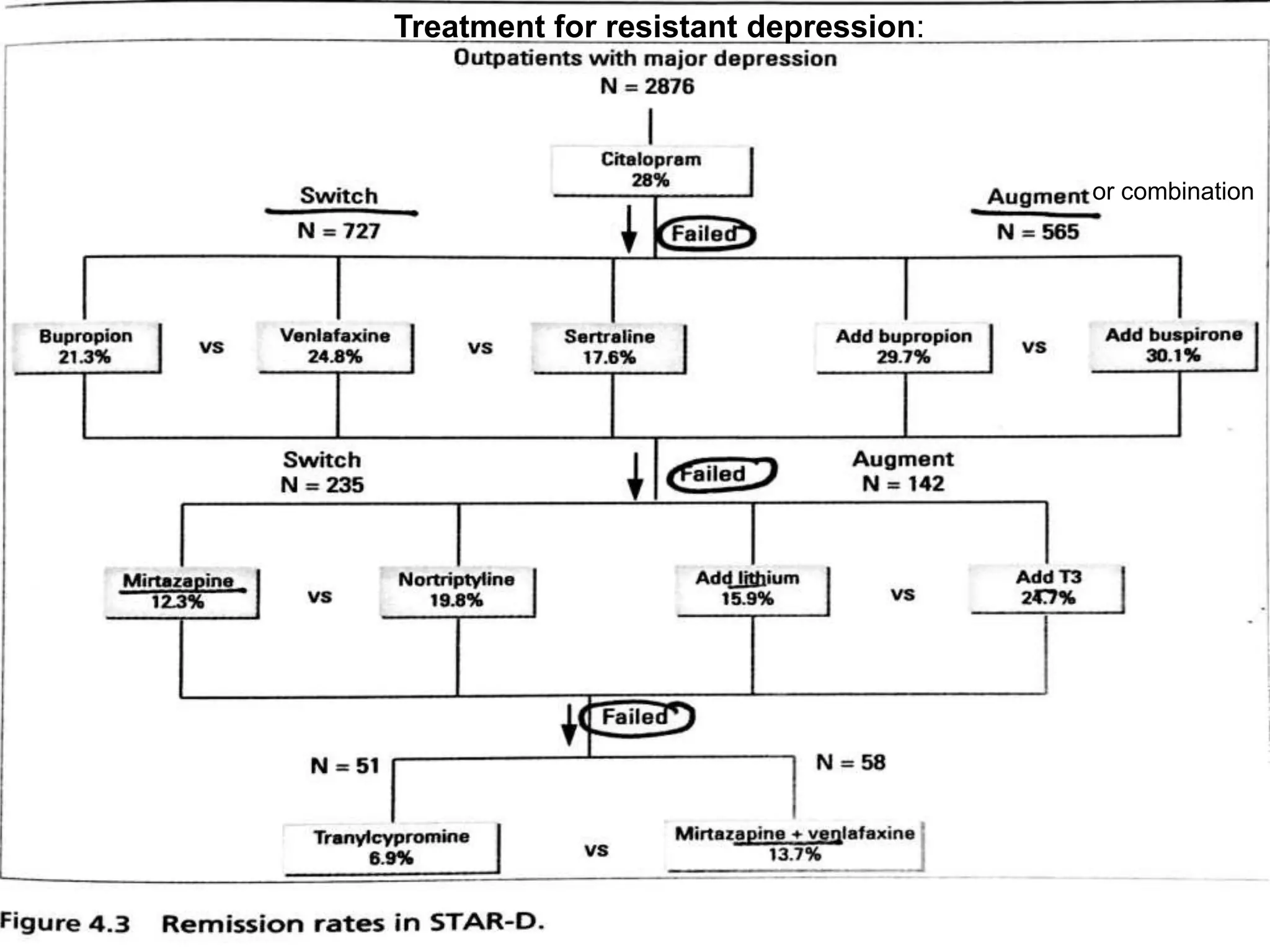
Depression is a common mental disorder characterized by depressed mood and loss of interest or pleasure. It is the leading cause of disability worldwide and has a high prevalence among women. Risk factors include genetics, brain chemistry, life stressors, and medical illnesses. Symptoms can range from mild to severe and include feelings of sadness, fatigue, changes in appetite, and suicidal thoughts in more severe cases. Treatment involves antidepressant medication, psychotherapy, or electroconvulsive therapy for severe or treatment-resistant cases. Antidepressants take 2-4 weeks to work and should be taken for at least 6-9 months after an initial episode or for 2 years for recurrent depression to prevent relapse.

































![Summary of NICE guidance:
recommendation regarding antidepressant prophylaxis
• Patient who have 2 or more episodes of depression in
the recent past, and who have experienced significant
functional impairment should be advised to continue
antidepressants for atleast 2 years.
• Patients on maintenance treatment should be re-
evaluated by age, co-morbid conditions, and other risk
factors in decision to continue maintenance treatment
beyond 2 years.
[NICE : National Institute for Health and Care Excellence]](https://image.slidesharecdn.com/depressionnuthn-171221130427/75/Depression-30-37-2048.jpg)










![REFERNCES:
• http://www.who.int/mental_health/manageme
nt/depression/who_paper_depression_wfmh
_2012.pdf
• Maudsley prescribing guidelines in
psychiatry[ 11th edition]](https://image.slidesharecdn.com/depressionnuthn-171221130427/75/Depression-30-49-2048.jpg)
