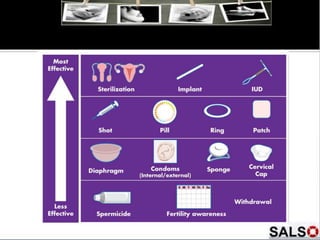
This document discusses various topics related to contraception, including epidemiological data on unintended pregnancies in the UK, types of contraception and their mechanisms of action, criteria for contraceptive use, and disease-specific contraceptive options. It provides details on natural family planning methods, barrier methods, hormonal contraceptives including combined oral contraceptives and progestogen-only methods, intrauterine devices, and sterilization procedures. Effectiveness, side effects, and other considerations are described for each contraceptive method.