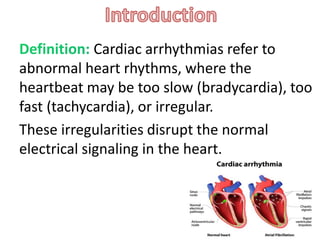
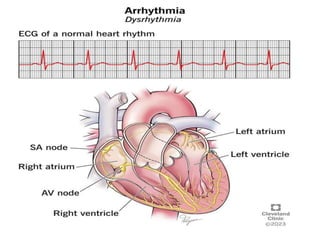
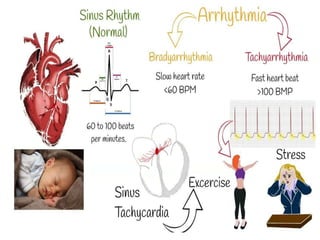
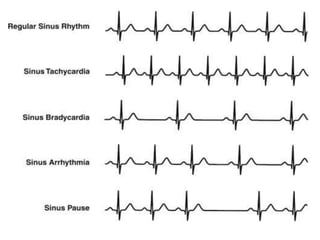
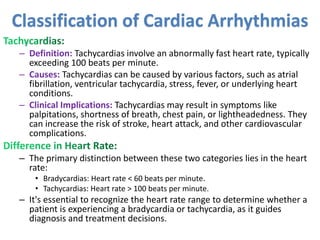
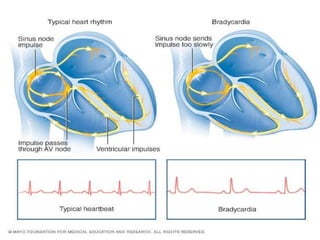
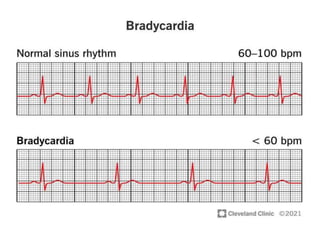
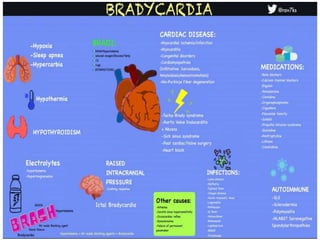
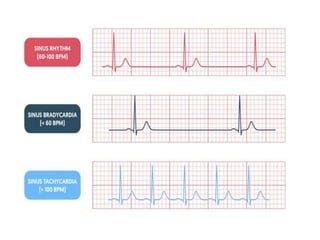
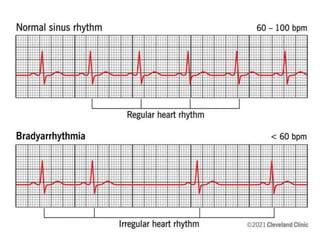
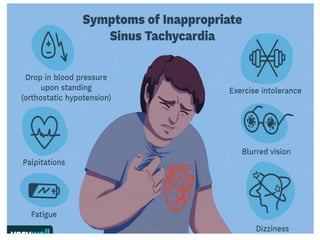
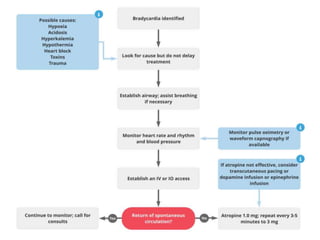
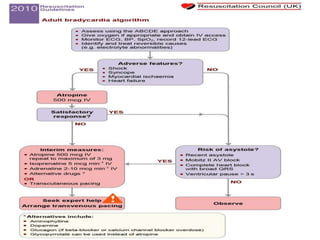
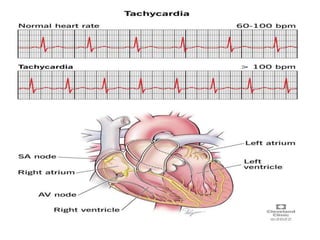
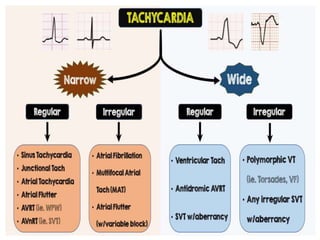
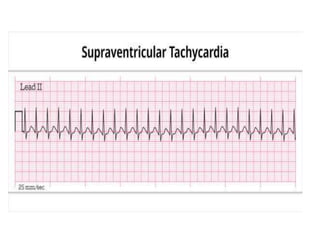
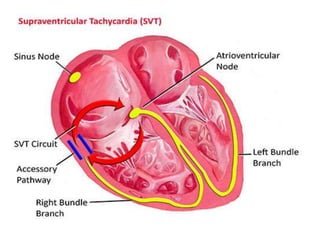
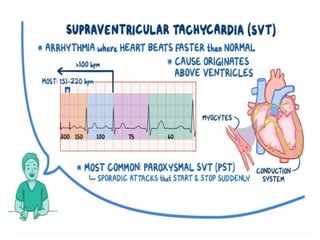
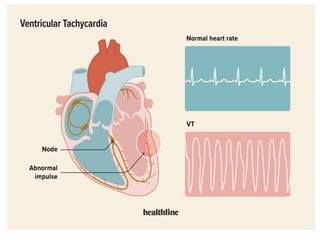
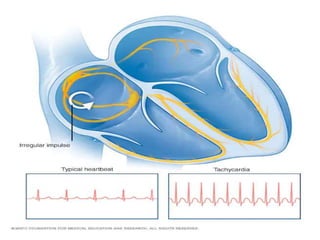
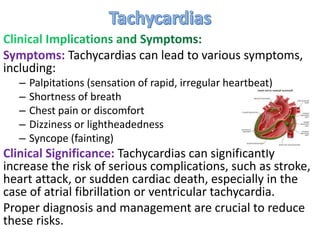
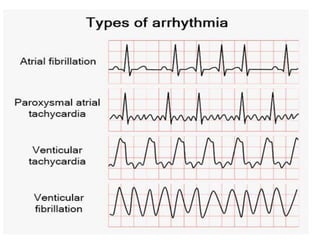
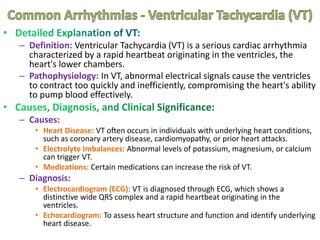
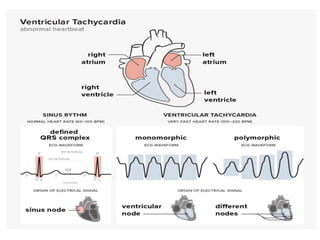
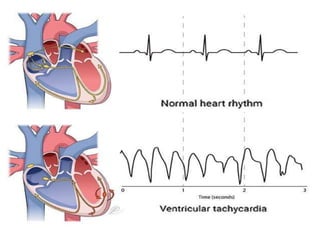
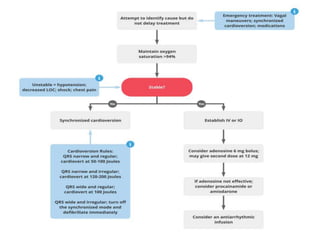
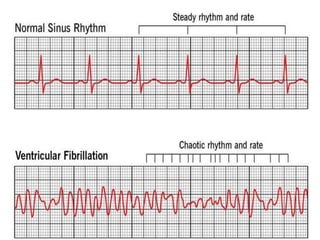
Cardiac arrhythmias are abnormal heart rhythms that can be categorized into bradycardias (slow heart rates) and tachycardias (fast heart rates), both leading to serious health complications. Accurate diagnosis and management by cardiologists are crucial, involving various diagnostic tools and treatment options, including medications, ablation, and lifestyle modifications. The document emphasizes the importance of understanding arrhythmias for effective treatment and improved patient outcomes.