British Society of Gastroenterology_Association of Coloproctology of Great Britain and Ireland_Public Health England post-polypectomy and post-colorectal cancer resection surveillance guidelines.pdf
•
0 likes•8 views
Guidelines for polyp screening
Report
Share
Report
Share
Download to read offline
Recommended
Recommended
Endoscopy in Gastrointestinal Oncology - Slide 17 - D. Fisher - Post-polypect...

Endoscopy in Gastrointestinal Oncology - Slide 17 - D. Fisher - Post-polypect...European School of Oncology
Chair and Presenter, Marianne Davies, DNP, ACNP, AOCNP, FAAN, Matthew A. Gubens, MD, MS, and Elizabeth S. Waxman, BSN, MSN, APN-BC, prepared useful Practice Aids pertaining to NSCLC for this CME/NCPD/ILNA/IPCE activity titled “Nurses at the Forefront of the Continuing Success Story of Immunotherapy in NSCLC: Best Practices for Guiding and Supporting Patients Through Treatment and Survivorship.” For the full presentation, downloadable Practice Aids, and complete CME/NCPD/ILNA/IPCE information, and to apply for credit, please visit us at https://bit.ly/3FvAeOR. CME/NCPD/ILNA/IPCE credit will be available until May 27, 2024.Nurses at the Forefront of the Continuing Success Story of Immunotherapy in N...

Nurses at the Forefront of the Continuing Success Story of Immunotherapy in N...PVI, PeerView Institute for Medical Education
Though a recent study found repeat colonoscopy is good for certain patients, accurate documentation is still a crucial factor to determine whether it is appropriate.How Accurate Clinical Documentation Is Crucial for Repeat Colonoscopy

How Accurate Clinical Documentation Is Crucial for Repeat ColonoscopyMedical Transcription Service Company
Endoscopy in Gastrointestinal Oncology - Slide 15 - D. Fisher - Colorectal ca...

Endoscopy in Gastrointestinal Oncology - Slide 15 - D. Fisher - Colorectal ca...European School of Oncology
More Related Content
Similar to British Society of Gastroenterology_Association of Coloproctology of Great Britain and Ireland_Public Health England post-polypectomy and post-colorectal cancer resection surveillance guidelines.pdf
Endoscopy in Gastrointestinal Oncology - Slide 17 - D. Fisher - Post-polypect...

Endoscopy in Gastrointestinal Oncology - Slide 17 - D. Fisher - Post-polypect...European School of Oncology
Chair and Presenter, Marianne Davies, DNP, ACNP, AOCNP, FAAN, Matthew A. Gubens, MD, MS, and Elizabeth S. Waxman, BSN, MSN, APN-BC, prepared useful Practice Aids pertaining to NSCLC for this CME/NCPD/ILNA/IPCE activity titled “Nurses at the Forefront of the Continuing Success Story of Immunotherapy in NSCLC: Best Practices for Guiding and Supporting Patients Through Treatment and Survivorship.” For the full presentation, downloadable Practice Aids, and complete CME/NCPD/ILNA/IPCE information, and to apply for credit, please visit us at https://bit.ly/3FvAeOR. CME/NCPD/ILNA/IPCE credit will be available until May 27, 2024.Nurses at the Forefront of the Continuing Success Story of Immunotherapy in N...

Nurses at the Forefront of the Continuing Success Story of Immunotherapy in N...PVI, PeerView Institute for Medical Education
Though a recent study found repeat colonoscopy is good for certain patients, accurate documentation is still a crucial factor to determine whether it is appropriate.How Accurate Clinical Documentation Is Crucial for Repeat Colonoscopy

How Accurate Clinical Documentation Is Crucial for Repeat ColonoscopyMedical Transcription Service Company
Endoscopy in Gastrointestinal Oncology - Slide 15 - D. Fisher - Colorectal ca...

Endoscopy in Gastrointestinal Oncology - Slide 15 - D. Fisher - Colorectal ca...European School of Oncology
Similar to British Society of Gastroenterology_Association of Coloproctology of Great Britain and Ireland_Public Health England post-polypectomy and post-colorectal cancer resection surveillance guidelines.pdf (20)
Endoscopy in Gastrointestinal Oncology - Slide 17 - D. Fisher - Post-polypect...

Endoscopy in Gastrointestinal Oncology - Slide 17 - D. Fisher - Post-polypect...
Nurses at the Forefront of the Continuing Success Story of Immunotherapy in N...

Nurses at the Forefront of the Continuing Success Story of Immunotherapy in N...
How Accurate Clinical Documentation Is Crucial for Repeat Colonoscopy

How Accurate Clinical Documentation Is Crucial for Repeat Colonoscopy
Letter: Is the Stupp Protocol an expensive and unsustainable standard of care...

Letter: Is the Stupp Protocol an expensive and unsustainable standard of care...
Microbiome Diagnostics Platform for Microbiome Health and Colon Cancer Preven...

Microbiome Diagnostics Platform for Microbiome Health and Colon Cancer Preven...
Endoscopy in Gastrointestinal Oncology - Slide 15 - D. Fisher - Colorectal ca...

Endoscopy in Gastrointestinal Oncology - Slide 15 - D. Fisher - Colorectal ca...
Clinical Practice Guideline on management of patients with diabetes and chron...

Clinical Practice Guideline on management of patients with diabetes and chron...
Review of Diagnostic Procedures and Progress in the Management of Acute Chole...

Review of Diagnostic Procedures and Progress in the Management of Acute Chole...
Review of Diagnostic Procedures and Progress in the Management of Acute Chole...

Review of Diagnostic Procedures and Progress in the Management of Acute Chole...
Recently uploaded
Holistic Approaches to Depression, Mental Well-Being, Mind Health, and Stress Treatment.Unlocking Holistic Wellness: Addressing Depression, Mental Well-Being, and St...

Unlocking Holistic Wellness: Addressing Depression, Mental Well-Being, and St...Health Kinesiology Natural Bioenergetics
A rare case of double-diverticulae of the Gallbladder found during a routine elective cholecystectomy is presented including intra operative and specimen images.Gallbladder Double-Diverticular: A Case Report المرارة مزدوجة التج: تقرير حالة

Gallbladder Double-Diverticular: A Case Report المرارة مزدوجة التج: تقرير حالةMohamad محمد Al-Gailani الكيلاني
Recently uploaded (20)
Hemodialysis: Chapter 1, Physiological Principles of Hemodialysis - Dr.Gawad

Hemodialysis: Chapter 1, Physiological Principles of Hemodialysis - Dr.Gawad
SEMESTER-V CHILD HEALTH NURSING-UNIT-1-INTRODUCTION.pdf

SEMESTER-V CHILD HEALTH NURSING-UNIT-1-INTRODUCTION.pdf
Failure to thrive in neonates and infants + pediatric case.pptx

Failure to thrive in neonates and infants + pediatric case.pptx
Unlocking Holistic Wellness: Addressing Depression, Mental Well-Being, and St...

Unlocking Holistic Wellness: Addressing Depression, Mental Well-Being, and St...
Treatment Choices for Slip Disc at Gokuldas Hospital

Treatment Choices for Slip Disc at Gokuldas Hospital
Creeping Stroke - Venous thrombosis presenting with pc-stroke.pptx

Creeping Stroke - Venous thrombosis presenting with pc-stroke.pptx
Hi Fi * Surat ℂall Girls Surat Dumas Road 8527049040 WhatsApp AnyTime Best Su...

Hi Fi * Surat ℂall Girls Surat Dumas Road 8527049040 WhatsApp AnyTime Best Su...
Top 15 Sexiest Pakistani Pornstars with Images & Videos

Top 15 Sexiest Pakistani Pornstars with Images & Videos
Unveiling Pharyngitis: Causes, Symptoms, Diagnosis, and Treatment Strategies.pdf

Unveiling Pharyngitis: Causes, Symptoms, Diagnosis, and Treatment Strategies.pdf
VIII.1 Nursing Interventions to Promote Healthy Psychological responses, SELF...

VIII.1 Nursing Interventions to Promote Healthy Psychological responses, SELF...
Bangalore whatsapp Number Just VIP Brookefield 100% Genuine at your Door Step

Bangalore whatsapp Number Just VIP Brookefield 100% Genuine at your Door Step
Gallbladder Double-Diverticular: A Case Report المرارة مزدوجة التج: تقرير حالة

Gallbladder Double-Diverticular: A Case Report المرارة مزدوجة التج: تقرير حالة
British Society of Gastroenterology_Association of Coloproctology of Great Britain and Ireland_Public Health England post-polypectomy and post-colorectal cancer resection surveillance guidelines.pdf
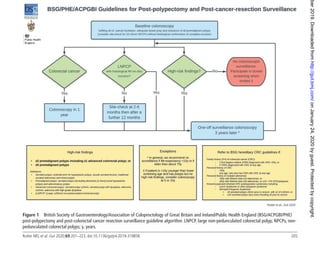
- 1. 205 Rutter MD, et al. Gut 2020;69:201–223. doi:10.1136/gutjnl-2019-319858 Guidelines Figure 1 British Society of Gastroenterology/Association of Coloproctology of Great Britain and Ireland/Public Health England (BSG/ACPGBI/PHE) post- polypectomy and post- colorectal cancer resection surveillance guideline algorithm. LNPCP, large non- pedunculated colorectal polyp; NPCPs, non- pedunculated colorectal polyps; y, years. involved in the decision- making process and improved safety and better clinical outcomes. However, there is a paucity of evidence regarding patient views on, and experiences of, surveillance. This is consistent with the lack of research regarding patient views and experiences of endoscopy, and is an area that requires significant research.27 28 Patients should have the evidence for surveillance explained to them and risks and benefits of different strategies explained. The principles of shared decision- making and informed choice should be applied. Patients should also be made aware of any alternative strategy available, and a discussion should take place regarding risks and benefits. Patient needs and expectations should be kept in mind and addressed where possible. Patients should be made aware of other evidence- based interven- tions that could reduce their risk of CRC and/or polyp recurrence. These could include lifestyle and behavioural modifications (eg, stopping smoking and reducing red meat consumption) as well as medications (eg, aspirin). Information should be conveyed in a manner and language that is understandable, allowing patients to make informed choices. Information should be provided in clear written form and with clear verbal explanation and opportunity for reflection and discus- sion. Patients should be made aware of whom they can contact in the event of any subsequent questions about surveillance. Surveillance guidelines recommendations The following recommendations have been developed by the GDG, based on the predetermined surveillance principles, the underlying evidence and following detailed discussion and consensus voting. These recommendation are summarised in figure 1. We recommend that the high- risk criteria for future CRC comprise either: ► ► two or more premalignant polyps including at least one advanced colorectal polyp (defined as a serrated polyp of at least 10mm in size or containing any grade of dysplasia, or an adenoma of at least 10mm in size or containing high- grade dysplasia); or ► ► five or more premalignant polyps. GRADE of evidence: See later evidence section Strength of recommendation: Strong The guidelines incorporate surveillance of patients following resection of either adenomatous or serrated polyps, aiming to simplify risk stratification of patients who may have both types of polyp. Surveillance following resection of CRC and LNPCPs have also been incorporated into the same algorithm in order to standardise surveillance across these broad cohorts of patients. on January 24, 2020 by guest. Protected by copyright. http://gut.bmj.com/ Gut: first published as 10.1136/gutjnl-2019-319858 on 27 November 2019. Downloaded from