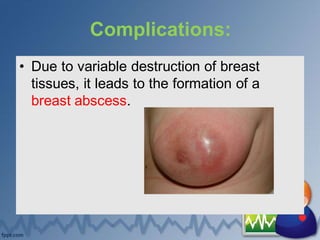
The document discusses common breast complications in the postpartum period including breast engorgement, cracked and retracted nipples, mastitis, breast abscess, and lactation failure. It provides details on causes, signs and symptoms, prevention, and treatment for each complication. Management involves ensuring proper breastfeeding technique, treating any infections, expressing milk to relieve engorgement, and using medications as needed to increase milk production or treat infections.