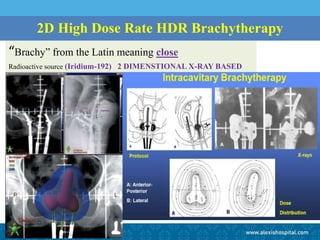
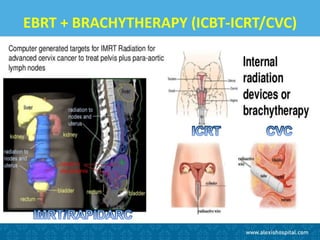
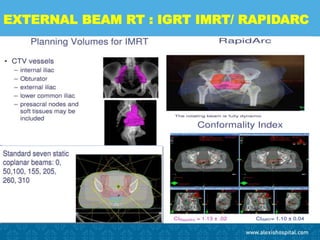
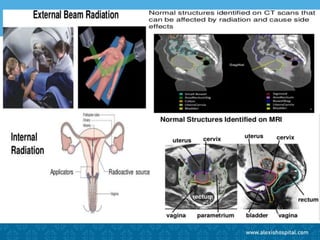
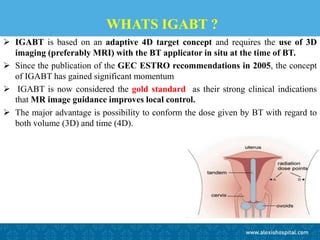
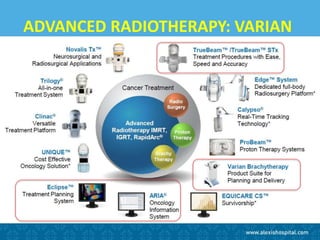
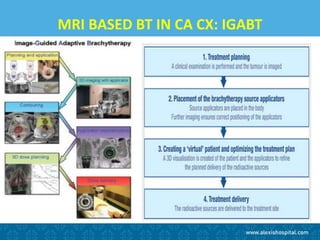
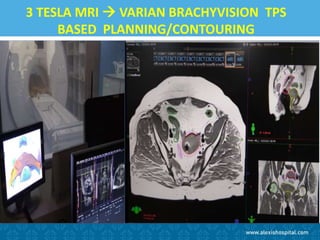
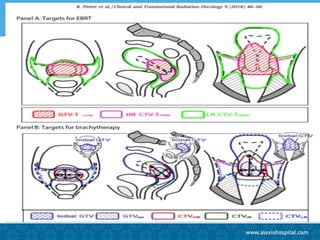
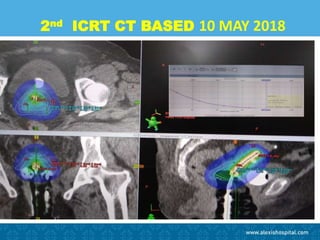
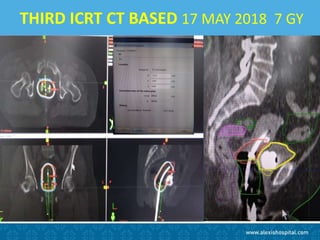
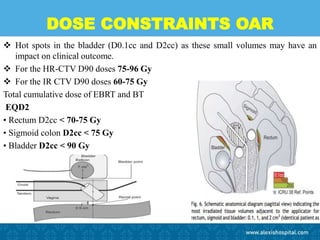
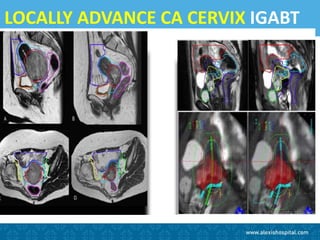
The document discusses the advancements and applications of image-guided adaptive brachytherapy (IGABT) in treating various cancers, notably cervical cancer, by utilizing precise imaging techniques like MRI to improve treatment efficacy and reduce side effects. It highlights the importance of dosimetry, advanced technology integration, and the rising global market for brachytherapy, which is expected to grow significantly by 2030. Emphasizing the standardization of IGABT, the document also presents clinical outcomes and ongoing studies validating its effectiveness compared to traditional methods.