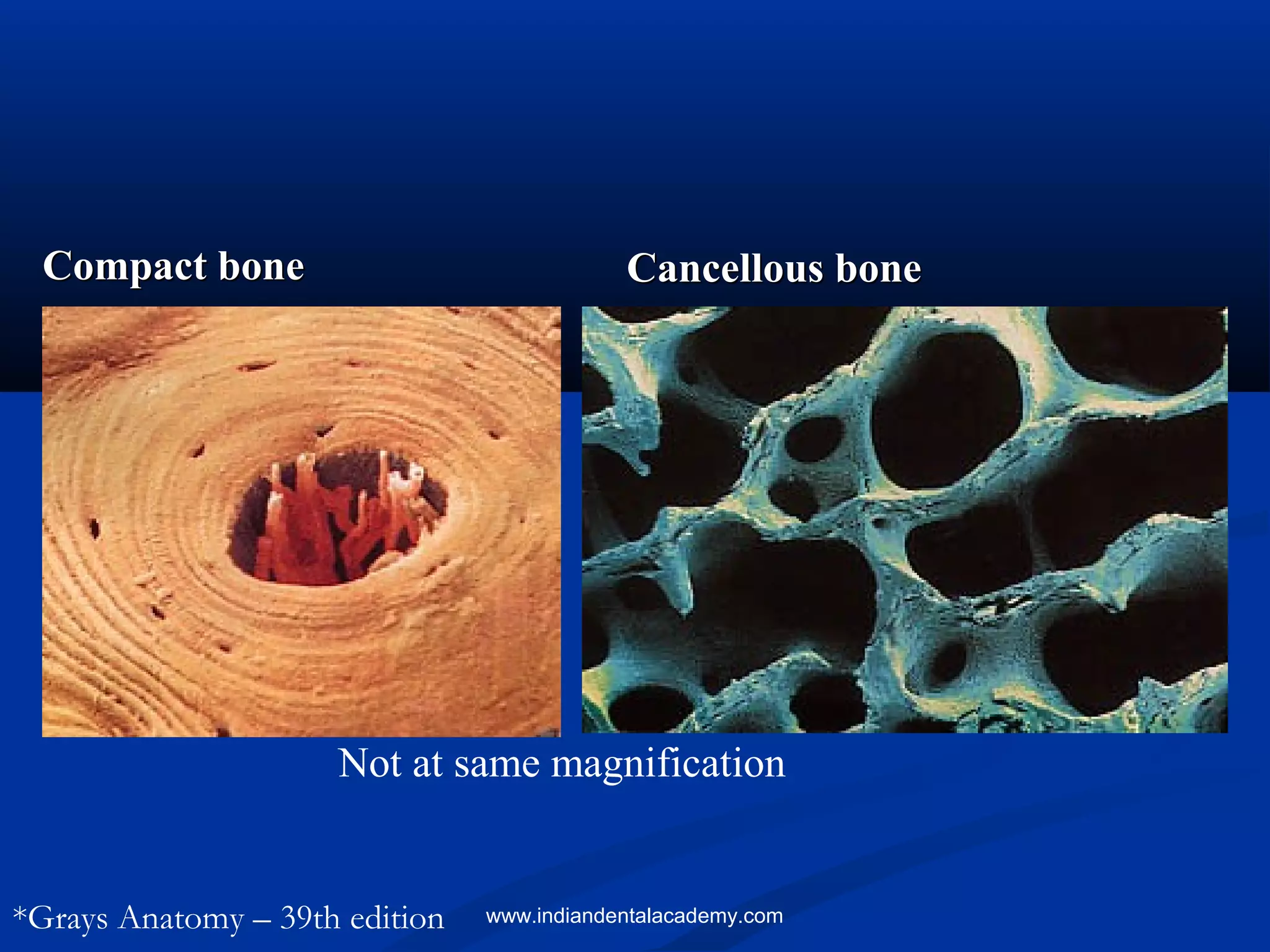
The document provides an extensive overview of bone physiology, including its classification, metabolism of calcium and phosphate, and the roles of various bone cells such as osteoblasts, osteocytes, and osteoclasts. Key components and mechanisms involved in bone formation, remodeling, and repair are discussed, along with the influence of hormones on bone functions. Additionally, the document addresses the importance of understanding craniofacial morphology in orthodontics and the effects of mechanical stresses on bone structure.