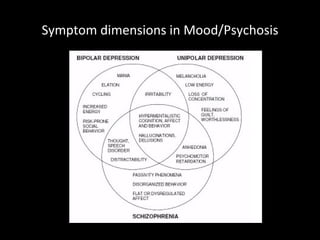
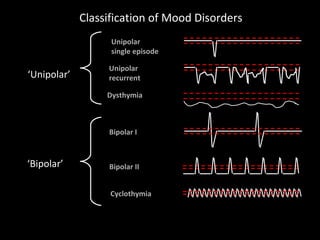
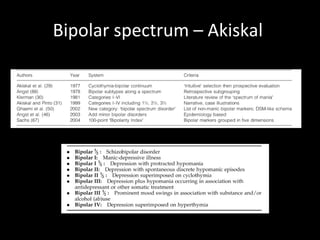
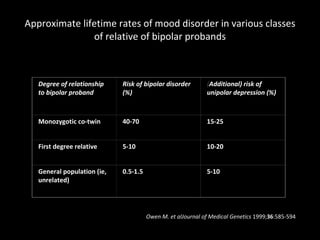
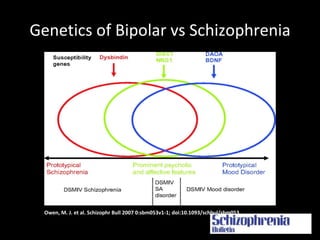
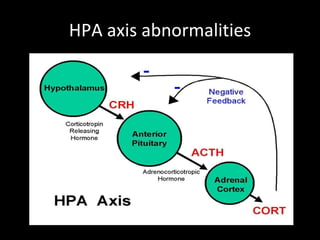
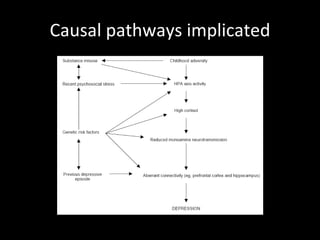
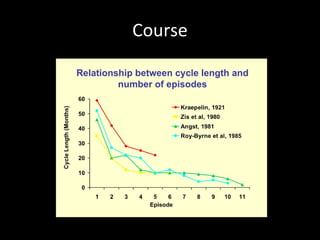
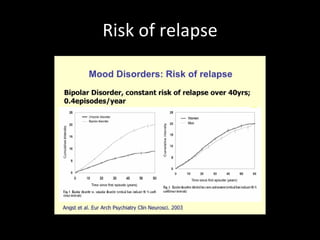
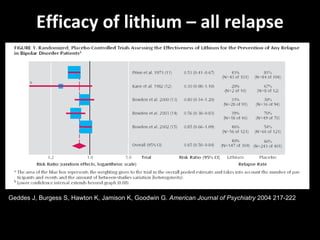
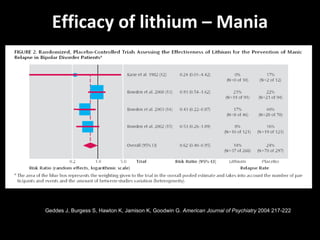
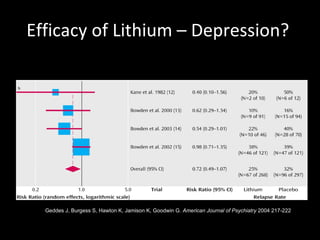
The document provides an overview of bipolar disorder, including its prevalence, symptoms, diagnosis, course, treatment guidelines, and monitoring recommendations. It discusses the symptomatology and classification of bipolar I and II disorders. It also outlines the etiology, neurobiology, and risk of relapse associated with bipolar disorder. Treatment guidelines from NICE focus on acute stabilization and long-term management using lithium, anticonvulsants, or antipsychotics.