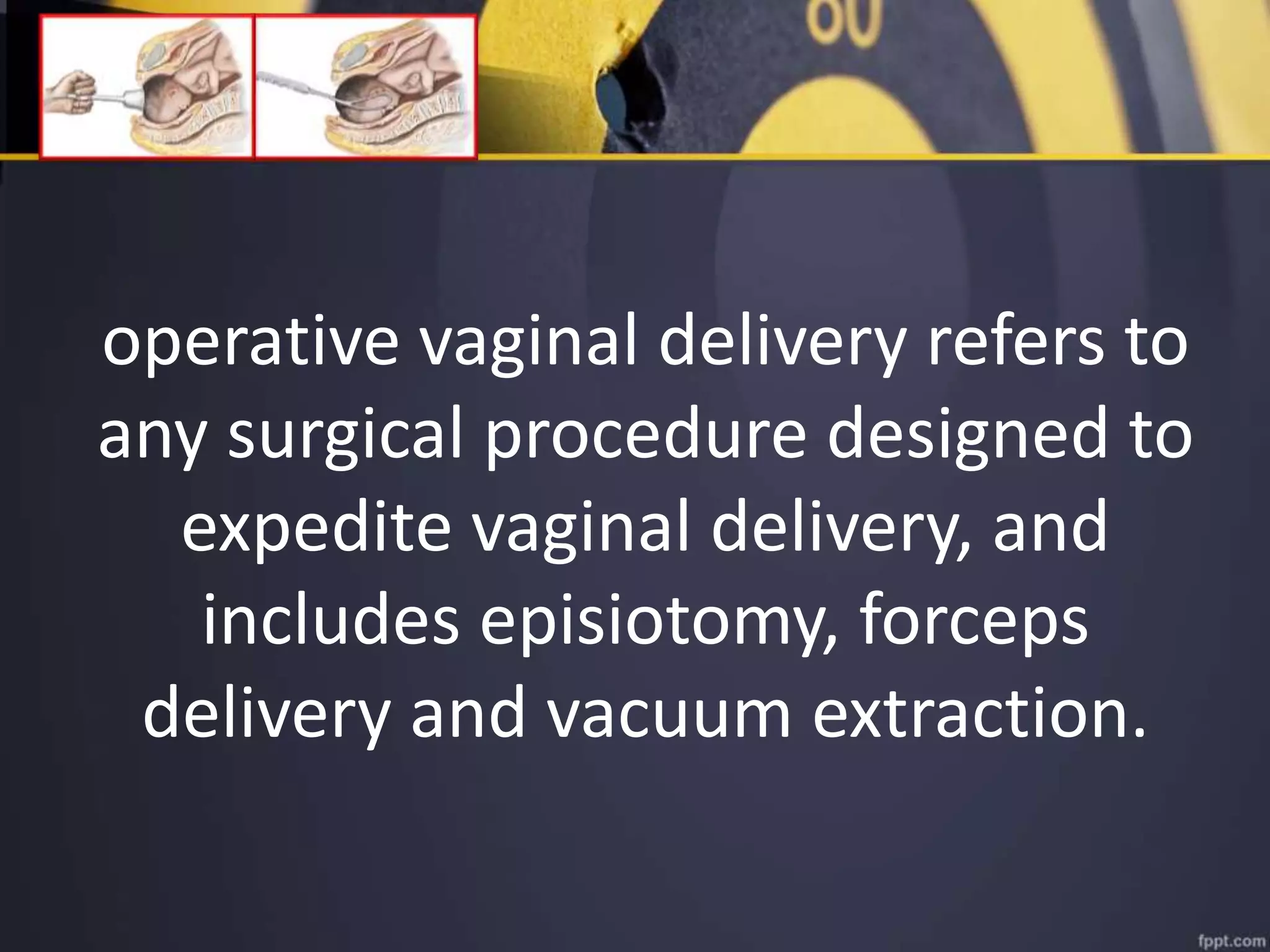
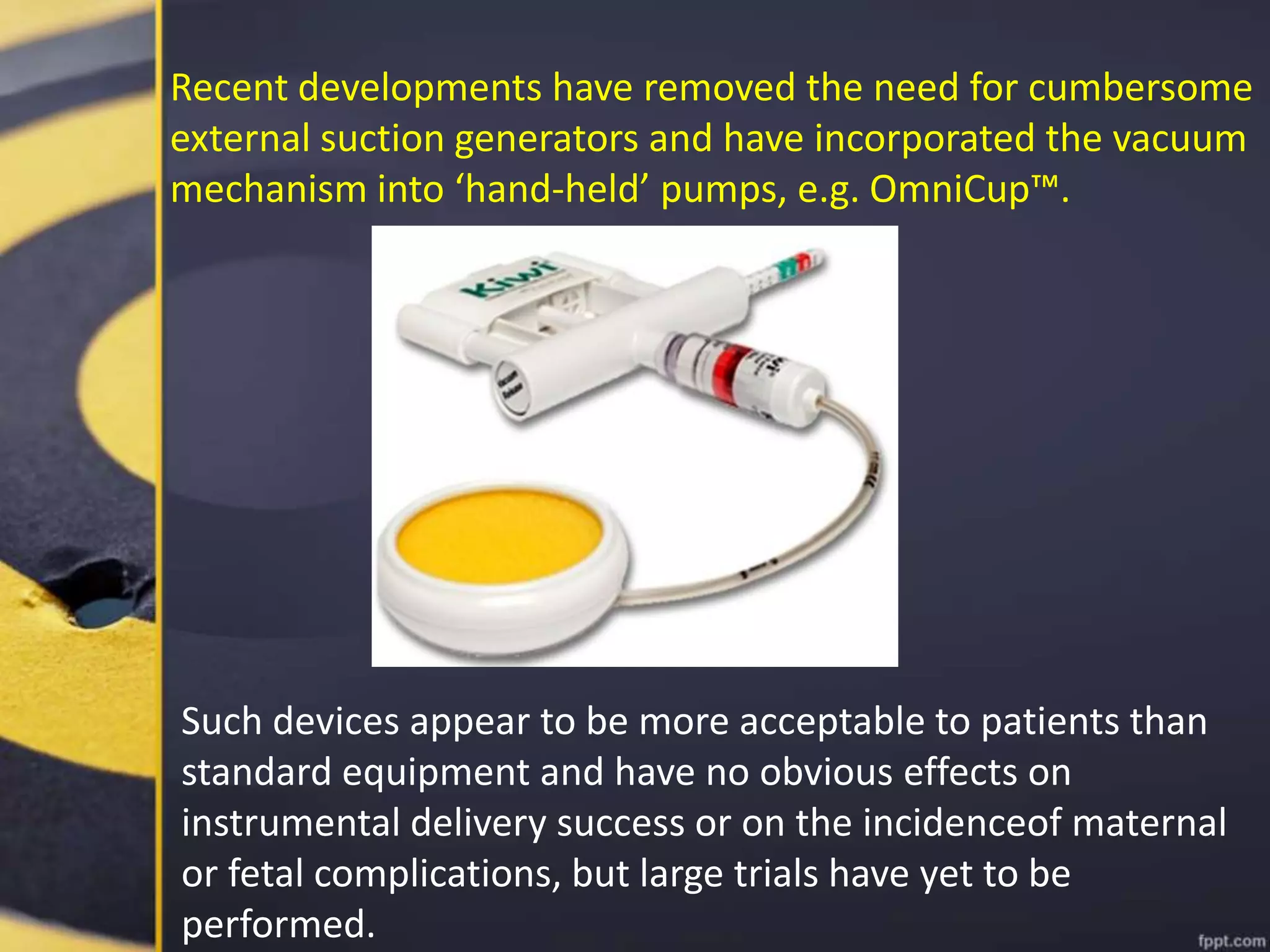
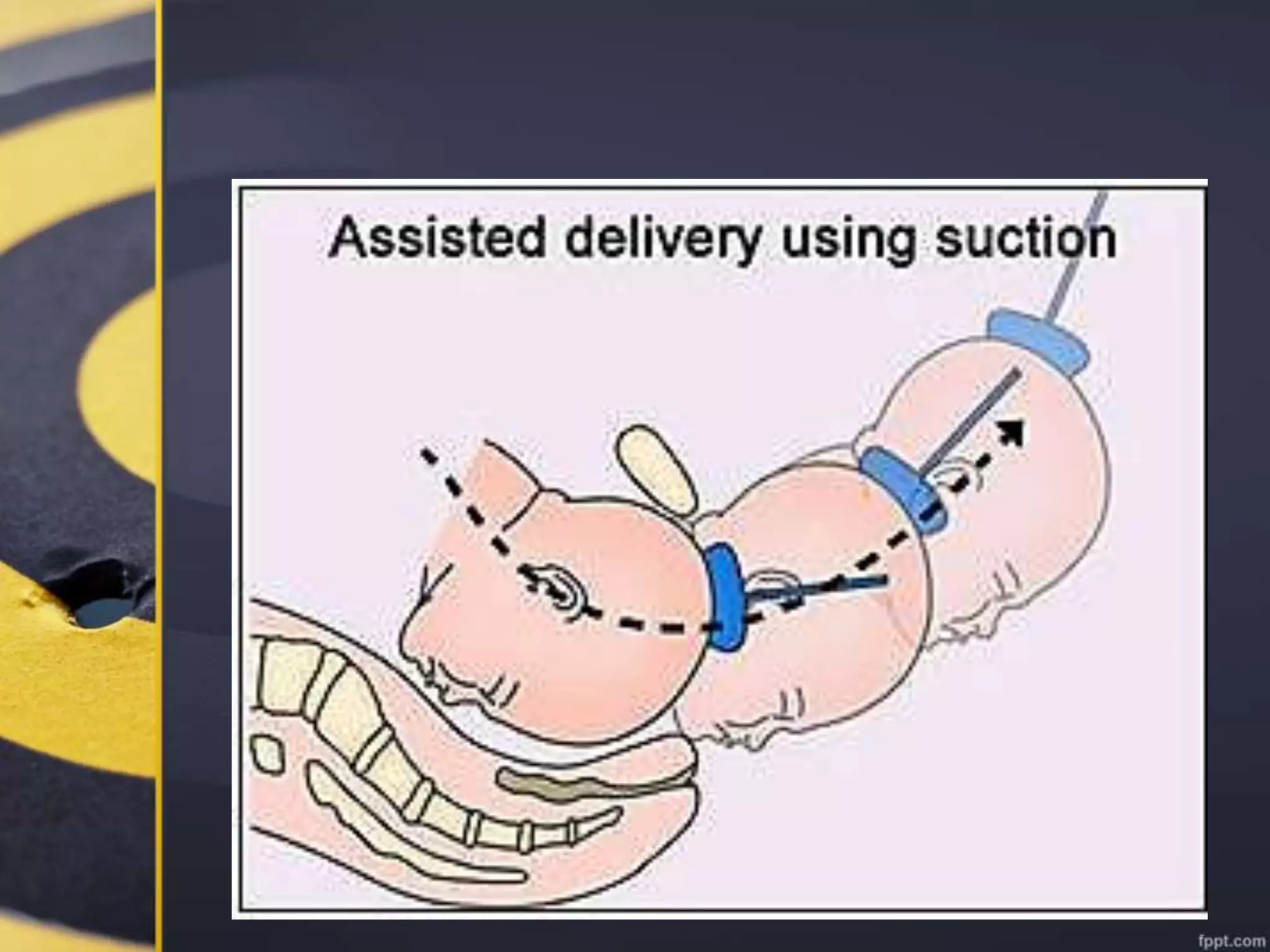
Operative vaginal delivery encompasses surgical procedures to expedite vaginal childbirth, such as forceps delivery and vacuum extraction, with varying incidence rates influenced by labor management practices. Maternal and fetal indications guide the need for these interventions, often highlighting risks like fetal heart rate irregularities and maternal exhaustion. Proper technique, prerequisites for delivery, and potential complications are critical considerations in the successful application of instruments in assisted births.