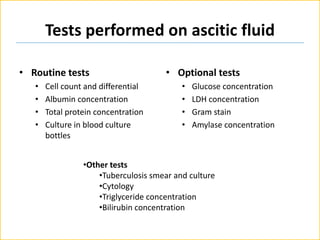
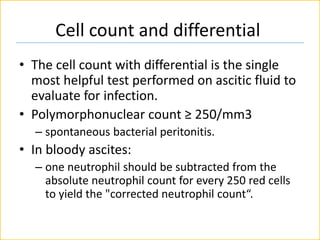
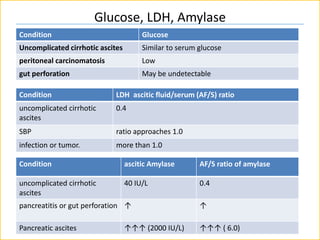
The document discusses ascites, its diagnosis, causes, and classification, with emphasis on the role of imaging tests and paracentesis in identifying fluid presence and its etiology. It outlines the grading system for ascites and the significance of laboratory tests performed on ascitic fluid, such as cell count, albumin gradient, and cultures. Additionally, the document highlights the differentiation between infections and other conditions causing ascites, including specific tests for tuberculosis peritonitis.