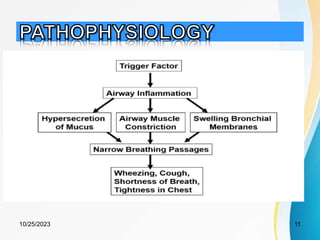
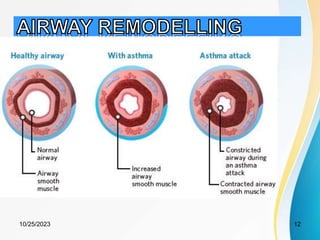
This document discusses acute severe asthma, an exacerbation of asthma characterized by persistent dyspnea that does not resolve with usual bronchodilator therapy. It covers the epidemiology, pathophysiology, clinical presentation, management, and differentials of acute severe asthma. Management involves relieving airflow obstruction with oxygen, bronchodilators, and corticosteroids. Patients not improving or deteriorating require intensive care admission for close monitoring. Acute severe asthma is a medical emergency but has a good outcome with prompt treatment.