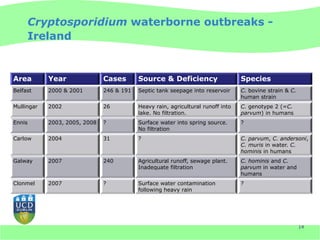
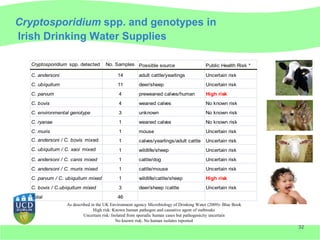
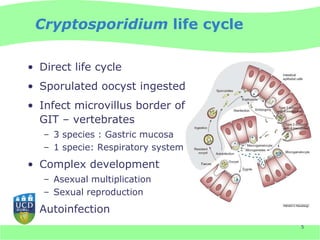
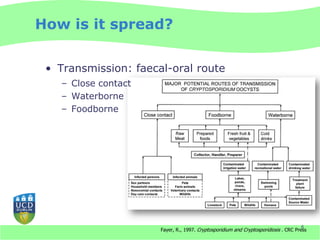
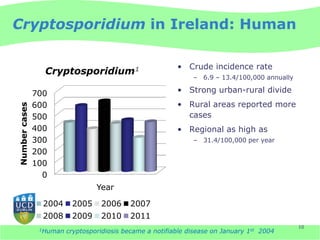
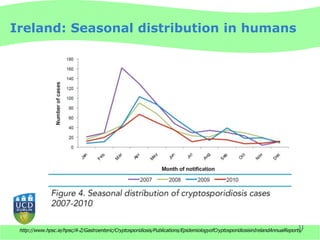
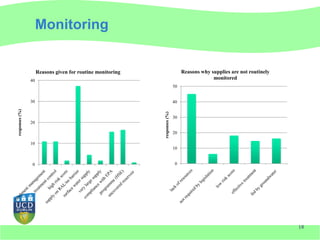
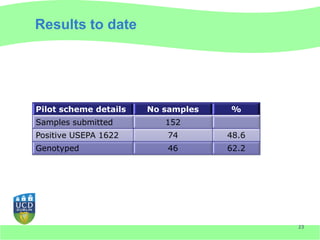
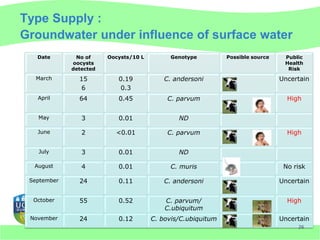
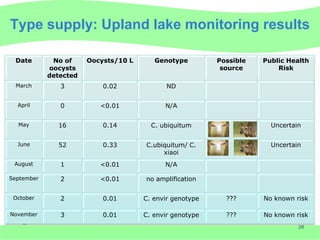
This document discusses Cryptosporidium monitoring of surface waters in Ireland. It provides background on Cryptosporidium, including what it is, how it spreads, and impacts on humans and surface waters. It notes several waterborne outbreaks in Ireland linked to Cryptosporidium in untreated surface waters. It also discusses the development of a national reference laboratory in Ireland for Cryptosporidium monitoring of public water supplies to improve detection and risk assessment.