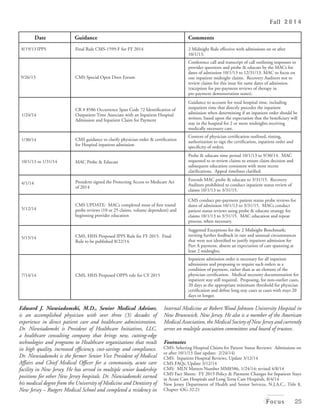
The document discusses the '2-midnight rule' implemented by CMS on October 1, 2013, which clarifies the criteria for determining hospital inpatient admissions, emphasizing the necessity for documentation by physicians that anticipates a stay exceeding two midnights. It also highlights New Jersey's regulations that are stricter than CMS guidelines, the importance of collaborative efforts among healthcare teams, and ongoing education for physicians regarding inpatient admission processes. Lastly, it outlines exceptions to the 2-midnight rule and the evolving regulatory landscape affecting hospital billing and compliance.