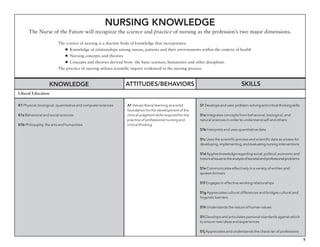
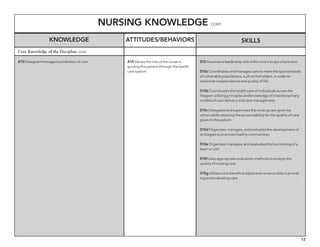
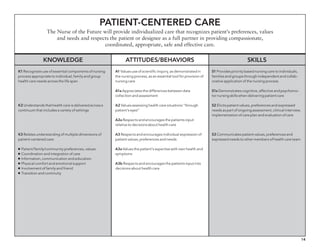
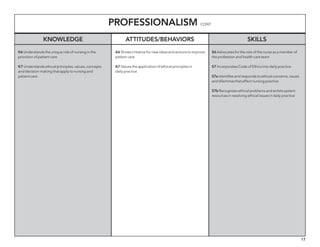
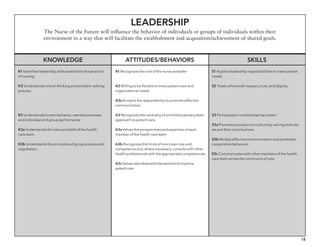
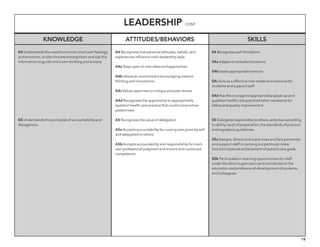
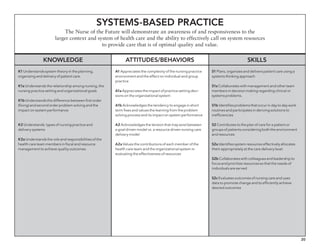
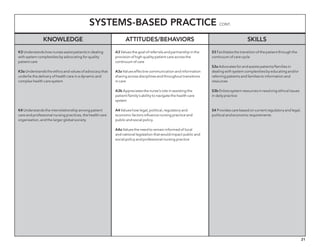
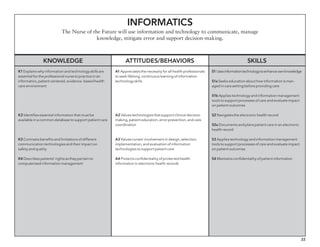
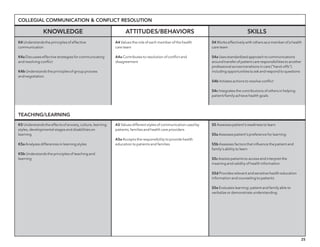
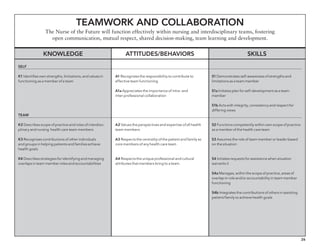
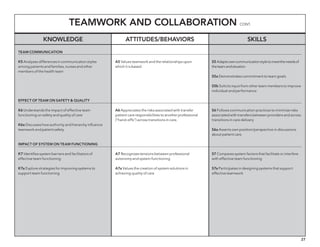
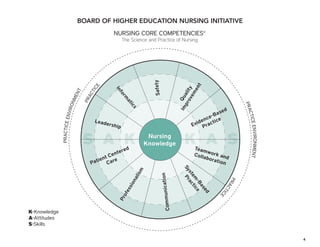
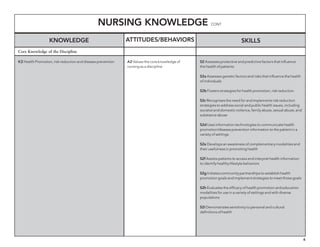
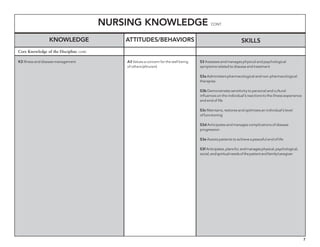
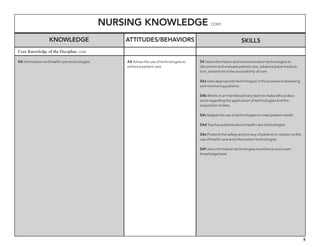
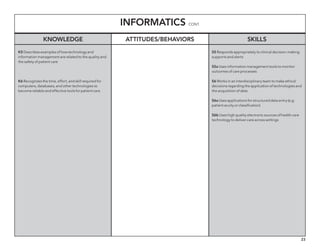
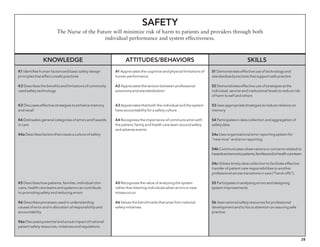
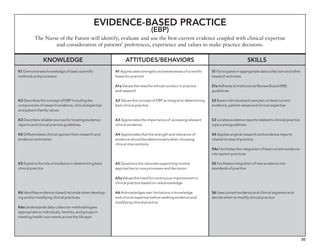
The document outlines the development of core nursing competencies in Massachusetts to establish a seamless progression through all levels of nursing education and transition nurses into practice settings. A working group composed of nursing educators and leaders developed competencies based on a review of other state and national standards. The competencies are intended to serve as a framework for a competency-based nursing education model. Feedback is being sought from nursing faculty and practitioners to refine the competencies.