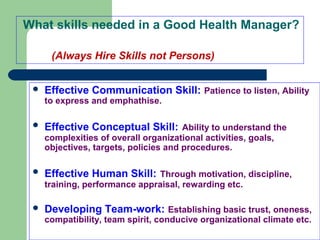
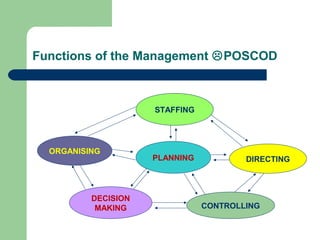
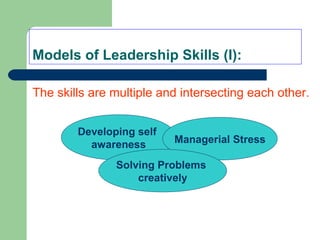
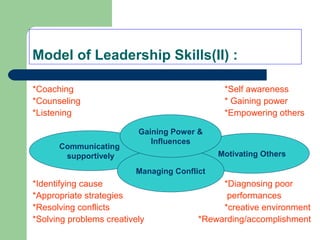
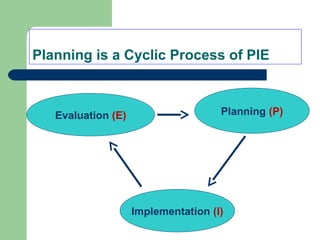
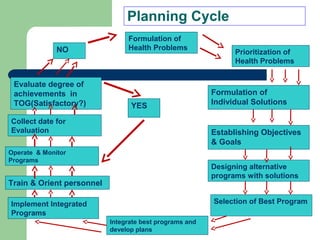
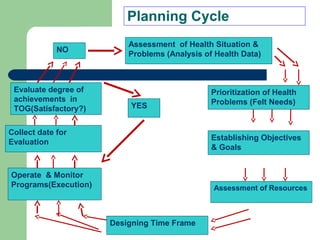
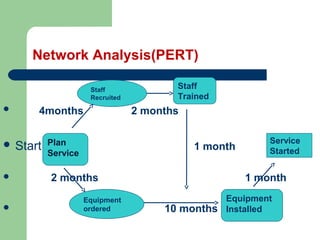
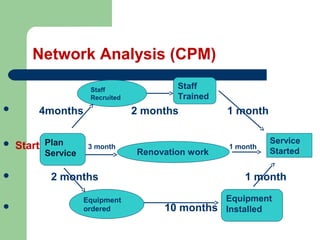
The document outlines the principles and methods of health system management, emphasizing the coordination and efficient use of resources to achieve healthcare objectives. It details the planning process involved in health management, including setting goals, assessing resources, and evaluating outcomes, alongside various qualitative and quantitative management methods. Effective health managers are characterized by strong communication, leadership, and technical skills, essential for implementing and evaluating health programs effectively.