Increased intracranial pressure
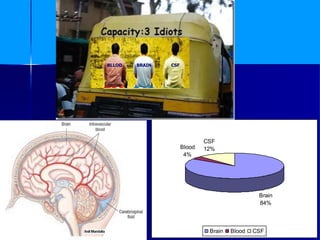
- 1. ANIL MANDALIA 1 Brain 84% Blood 4% CSF 12% Brain Blood CSF BLLOD BRAIN CSF
- 2. ANIL MANDALIA 2 INCREASED INTRACRANIAL PRESSURE (INTRACRANIAL HYPERTENSION) Our skull creates a hard casing in which our cranial contents rest and is protected from injury. The cranial contents consist of three components. Brain tissue or cells make up 84% of the cranial contents. Our cerebrospinal fluid 12% and cerebral blood volume is 4%.
- 3. ANIL MANDALIA 3 Normal ICP Intracranial pressure is the pressure exerted in the cranium by its components: Brain, blood and CSF. Normal intracranial pressure is 5-15mm of Hg.
- 4. ANIL MANDALIA 4 Definition of Increase Intracranial Pressure( intracranial hypertension) Pressure greater than 20 mm Hg is considered to represent Increase intracranial pressure or intracranial hypertension.
- 5. ANIL MANDALIA 5 Etiology and Risk Factors Brain related causes Space occupying lesion (SOL) Head injury Brain tumor Cerebral Hemorrhage Brain surgery infarction with edema Generalized brain swelling can occur in ischemic- anoxia states, acute liver failure, hypertensive encephalopathy, pseudotumor cerebri, hypercarbia.
- 6. ANIL MANDALIA 6 Increase cerebral blood flow or increase in venous pressure : Venous sinus thrombosis, Heart failure, or obstruction of superior mediastinal or jugular veins. Systemic Hypertension.
- 7. ANIL MANDALIA 7 obstruction to CSF flow and/or absorption : Hydrocephalus (blockage in ventricles or subarachnoid space at base of brain, e.g., by Arnold-Chiari malformation). Extensive meningeal disease (e.g., infectious, carcinomatous, granulomatous, or hemorrhagic). Obstruction in cerebral convexities and superior sagittal sinus (decreased absorption).
- 8. ANIL MANDALIA 8 Pathophysiology Head Injury/ Intra cranial Mass/ Brain swelling/ brain edema Increase intracranial pressure due to increase in brain tissue size or pressure.
- 9. ANIL MANDALIA 9 Displacement of CSF in to the spinal canal ( Evident by altered level of consciousness ) Further increasing in Intracranial pressure.
- 10. ANIL MANDALIA 10 Decrease cerebral blood flow through vasoconstriction of cerebral blood vessels. ( Evident by changes in EEG, altered cerebral metabolism, cerebral acidosis, brain hypoxia and brain tissue ischemia)
- 11. ANIL MANDALIA 11 Further increasing in Intracranial pressure. Herniation of the brain tissue. ( Evident by vasomotor, respiratory and cardiovascular center actions)
- 13. ANIL MANDALIA 13 Clinical Manifestations : 1. Altered level of consiousness. 2. Changes in speech. 3. Cltered pupillary reactivity. 4. Changes motor and sensory activities. 5. Headache. 6. Vomiting with no or little nausea.
- 14. ANIL MANDALIA 14 Clinical Manifestations : 7. Blured or double vision 8. Papiiledema 9. Bradycardia 10.Cheyne-strokes respiration 11.Hyperthermia 12.Brain Death
- 15. ANIL MANDALIA 15 Diagnsotic Study : X- ray Skull. C.T. Scan of brain. MRI. Transcranial Doppler. EEG. Invasive ICP monitoring.
- 16. ANIL MANDALIA 16 Management of Increase intracranial pressure : ( A) Medical Management : The main goal of medical management are to maintain cerebral oxygenation, to decrease ICP, to maintain optimal neurological function, and to ready the patient for rehabilitation.
- 17. ANIL MANDALIA 17 Maintain cerebral Oxygenation : – Oxygen inhalation to keep the PaO2 between 90-100 mm of Hg. – Endotrachial intubation. – Steroid to reduce cerebral edema.
- 18. ANIL MANDALIA 18 Decrease Intracranial pressure : – Osmotic diuretics. – Hyperventilation. – Slight head elevation. – Drain CSF
- 19. ANIL MANDALIA 19 Maintain cerebral perfusion : – Limit intra vascular fluid. – Vasoactive medication. – Barbiturates.
- 20. ANIL MANDALIA 20 Reducing fever : – Antipyretic medication.
- 21. ANIL MANDALIA 21 B. Nursing Management : Assessment – LOC – Lethargy and change in LOC first signs; restlessness – Glasgow Coma Scale – Vital signs – Late sign – Headache
- 22. ANIL MANDALIA 22 – Pupillary changes – Check pupil reaction, size, conjugate (paired; working together) . – Vomiting. – Evaluation of motor and sensory functions. – Monitoring of ICP
- 23. ANIL MANDALIA 23 Ineffective airway clearance related to diminished protective reflexes (Cough, gag) Nursing Intervention: Maintaining a patent airway. – Frequent suction. (with caution) – 100% oxygen given before and after suctioning. – Prevent suctioning more than 15 sec. – Discourage coughing. – Auscultate lung field.. – Elevate head of the bed.
- 24. ANIL MANDALIA 24 Evaluation : Evident by patent airway, breath sound clear, breath regularly, attain oxygen saturation, no secretions.
- 25. ANIL MANDALIA 25 Ineffective breathing pattern related to neurological dysfunctions. Nursing Intervention : Achieving an adequate breathing pattern. – Monitored frequently for respiratory irregularity. – Monitored PaO2 and PaCO2.
- 26. ANIL MANDALIA 26 Evaluation : Evident by regular breathing, maintain oxygen saturation.
- 27. ANIL MANDALIA 27 Ineffective cerebral perfusion related to effect of ICP. Nursing Intervention : Optimizing cerebral tissue perfusion – Elevate Head end 30 degrees with head in neutral position. – Cervical collar if needed to keep head neutral. – Avoid extreme hip flexion. – Avoid Valsalva maneuvers – ask client to exhale when being moved or turned – Avoid isometric exercises that increase SBP. – Preoxygenate and hyperventilate prior to suctioning. – Space nursing interventions. – Avoid emotional distress and frequent arousal from sleep. – Note abdominal distension.
- 28. ANIL MANDALIA 28 Evaluation : Evident by Oriented to time, place and person, follow verbal commands, improve glasgow coma scale score.
- 29. ANIL MANDALIA 29 Deficient fluid volume related to fluid restriction. Nursing Intervention : Maintain Negative fluid balance. – Monitor skin turgor, mucous membranes, serum and urine osmolality – Monitor IVF carefully. – Observe for CHF and pulmonary edema. – Good oral hygiene, monitor I&O.
- 30. ANIL MANDALIA 30 Evaluation : Evident by Optimal urine output, demonstrate serum and urine osmolality value within acceptable range.
- 31. ANIL MANDALIA 31 Risk for infection related to ICP monitoring system. Nursing Intervention : Preventing infection. – Change sterile dressing aseptically. – Aseptic technique must be adapted when managing system and changing the ventricular drainage bag. – Check the drainage for cloudiness and blood. – Watch for sign of infection viz fever, chills, neck rigidity etc. – Administered prescribed antibiotics.
- 32. ANIL MANDALIA 32 Evaluation : Evident by No fever, No signs of infection at catheter site and no purulent discharge from intracranial monitoring devices.
- 33. ANIL MANDALIA 33 Complications : Herniation of brain. Diabetes insipidus. Death.
