GERD
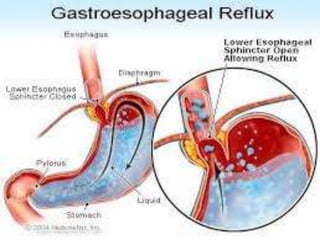
- 2. Definition • Gastro esophageal reflux disease is a chronic and relapsing condition in which prolonged reflux of hydrochloric acid, pepsin and bile salts in esophagus, oral cavity and respiratory system occurs that leads to esophagitis
- 4. Excessive intake of junk foods, coffee, chocolate
- 5. Excessive intake of onion, tomato, and beverages
- 6. • Heavy exercise Alcoholic and smoking
- 7. Medications
- 11. • Heart burn • Discomport • Chest pain • Difficulty in respiration • Aspiration pneumonia
- 12. After endoscopy the lesions are graded for severity using the Savary Miller grading system; • Grade 1: single or multiple erosions on a single fold. • Grade 2: multiple erosions affecting multiple folds. Erosions may be confluent. • Grade 3: multiple circumferential or rounded erosions. • Grade 4: ulcer, stenosis or esophageal shortening. • Grade 5: Barrett's epithelium. Columnar metaplasia (cellular changes on the miscroscopic level) in the form of circular or non-circular (islands or tongues) extensions.
- 13. Pathophysiology GERD Inflammation of esophagus Esophageal irritation and erosion of mucus lining The acidic gastric secretion reflux up into esophagus Increased the pressure in the abdomen Decreased gastric emptying, hyper secretion of stomach content Due to etiological factors
- 15. Management
- 16. • Antacids : An antacid is a substance which neutralizes stomach acidity, used to relieve heartburn, indigestion or an upset stomach (ex: Rantac, Zantac) • H2receptor antagonist: H2 antagonists block histamine-induced gastric acid secretion from the parietal cells of the gastric mucosa. They include cimetidine, famotidine, nizatidine
- 17. • Photon Pump Inhibitors: Proton pump inhibitors (PPIs) reduce the production of acid by blocking the enzyme in the wall of the stomach that produces acid (Omeprazole, Rabeprazole, pantaprazole) • Cholinergic drugs:Cholinergic drug, any of various drugs that inhibit, enhance, or mimic the action of the neurotransmitter (acetylcholine, carbachol, methacholine)
- 18. • Cytoprotective drugs: is a process by which chemical compounds provide protection to cells against harmful agents (carbenoxolone, sucralfate, misoprostol) • Prokinetic drugs: prokinetic, is a type of drug which enhances gastrointestinal motility by increasing the frequency of contractions in the small intestine or making them stronger, but without disrupting their rhythm. (Benzamide, Cisapride, Domperidone).
- 20. Endoscopic intraluminal valvuloplasty • Gastric tissue is utilised to increase the integrity of LES By creating a valve like structure.
- 23. A Nissen fundoplication, or laparoscopic Nissen fundoplication when performed via laparoscopic surgery, is a surgical procedure to treat gastroesophageal reflux disease (GERD) and hiatal hernia.
- 25. • Gastric bypass surgery makes the stomach smaller and allows food to bypass part of the small intestine.
- 27. Nursing management • ACUTE PAIN AT EPIGASTRIC REGION RELATED TO REFLUX OF THE GASTRIC CONTENTS INTO THE ESOPHAGUS • NAUSEA RELATED TO GLOBUS SENSATION, REGURGITATION, DELAYED ESOPHAGEAL EMPTYING. • IMBALANCED NUTRITION: LESS THAN BODY REQUIREMENT RELATED TO NAUSEA, INABILITY TO INTAKE FOOD ADEQUATELY SECONDARY TO GLOBUS SENSATION IN THROAT, PYROSIS.
- 28. • HEMORRHAGE RELATED TO ERODED MUCOSAL TISSUE OF ESOPHAGUS. • INEFFECTIVE THERAPEUTIC REGIMEN RELATED TO LACK OF KNOWLEDGE OF LONG-TERM MANAGEMENT OF GERD, LIFESTYLE MODIFICATION, APPROAPRIATE DIET THERAPY
- 29. Complication • Chronic erosive Oesophagitis: It is responsible for 40-60% of GERD symptoms. • Esophageal stricture: It is the result of healing of erosive esophagitis. • Barrett’s esophagus: It accounts for 8-15% of all GERD cases.
- 30. Esophageal stricture • Benign esophageal stricture describes a narrowing or tightening of the esophagus. The esophagus is the tube that brings food and liquids from your mouth to your stomach. “Benign” means it’s not cancerous. • Benign esophageal stricture typically occurs when stomach acid and other irritants damage the lining of the esophagus over time. This leads to inflammation (esophagitis) and scar tissue, which causes the esophagus to narrow.
- 31. Clinical manifestation • Difficult or painful swallowing • Unintended weight loss • Regurgitation of food or liquids • Sensation of something stuck in the chest After you eat • Frequent burping or hiccups • Heartburn
- 32. Management • Esophageal dilation • Esophageal dilation, or stretching, is the preferred option in most cases. Esophageal dilation can cause some discomfort, so you’ll be under general or moderate sedation during the procedure.
- 33. • Esophageal stent placement • The insertion of esophageal stents can provide relief from esophageal stricture. A stent is a thin tube made of plastic, expandable metal, or a flexible mesh material. Esophageal stents can help keep a blocked esophagus open so you can swallow food and liquids.
- 34. • Diet & lifestyle • Making certain adjustments to your diet and lifestyle can effectively manage GERD, which is the primary cause of benign esophageal stricture.
- 35. Barrette's esophagus Barrett’s esophagus is a condition in which the lining of the esophageal mucosa is altered. It typically occurs in association with GERD; indeed, longstanding untreated GERD may lead to Barrett’s esophagus. Reflux eventually causes changes in the cells lining the lower esophagus. The cells that are laid to cover the exposed area are no longer squamous in origin. These precancerous cells initiate the healing process and can be a precursor to esophageal cancer.
- 36. Management • Monitoring varies depending on the extent of cell changes. Follow-up endoscopy is performed within 6 months if there are minor cell changes. Treatment is individualized for each patient. The options include intensive surveillance with • Biopsies, • Endoscopic ablation therapy (eg, photodynamic therapy), • Esophagectomy
