Glycolysis and Gluconeogenesis and PFK-2/FBPase-2 enzyme and Pentose Phosphate Pathway
- 1. 1 Glycolysis
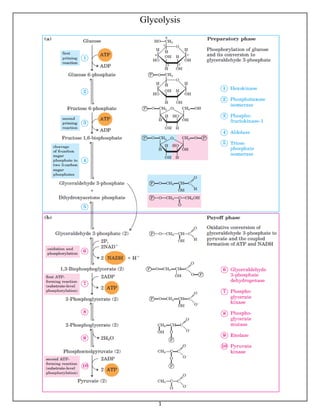
- 2. 2 • Glycolysis can be defined as the sequence of reactions for the breakdown of Glucose (6-carbon molecule) to two molecules of pyruvic acid (3-carbon molecule) under aerobic conditions; or lactate under anaerobic conditions along with the production of small amount of energy. • In organisms that perform cellular respiration, glycolysis is the first stage of this process. • However, glycolysis doesn’t require oxygen, and many anaerobic organisms that do not use oxygen—also have this pathway. • When animal tissues cannot be supplied with sufficient oxygen to support aerobic oxidation of the pyruvate and NADH produced in glycolysis, NAD+ is regenerated from NADH by the reduction of pyruvate to lactate. - Some tissues and cell types (such as erythrocytes, which have no mitochondria and thus cannot oxidize pyruvate to CO2) produce lactate from glucose even under aerobic conditions. - The reduction of pyruvate is catalyzed by lactate dehydrogenase. • Glycolysis takes place in the cytosol of a cell (cytoplasm). Steps in Details: https://laboratoryinfo.com/glycolysis-steps-diagram-energy-yield-and- significance/ 1. ○ Most of the reactions of the glycolytic pathway are reversible, which are also used for gluconeogenesis. ♦There are two types of glycolysis. ♣Aerobic Glycolysis: It occurs when oxygen is plentiful. - Final product is pyruvate along with the production of Eight ATP molecules. ♣Anaerobic Glycolysis: It occurs when oxygen is scarce. - Final product is lactate along with the production of two ATP molecules.
- 3. 3 Gluconeogenesis • Gluconeogenesis (abbreviated GNG) is a metabolic pathway that results in the generation of glucose from non-carbohydrate carbon substrates such as lactate, glycerol, and glucogenic amino acids. • It is one of the two main mechanisms humans and many other animals use to keep blood glucose levels from dropping too low (hypoglycemia). • The other means of maintaining blood glucose levels is through the degradation of glycogen (glycogenolysis). • Gluconeogenesis is a ubiquitous process, present in plants, animals, fungi, bacteria, and other microorganisms. • In animals, gluconeogenesis takes place mainly in the liver and, to a lesser extent, in the cortex of kidneys. • This process occurs during periods of fasting, starvation, low- carbohydrate diets, or intense exercise and is highly endergonic. • Gluconeogenesis is the reverse process of glycolysis.
- 4. 4 • The net production of glucose via gluconeogenesis involves the orchestrated activities of several key enzymes (pyruvate carboxylase, PEPCK(Phosphoenolpyruvate carboxykinase), aldolase, fructose-1,6-diphosphatase, and glucose-6-phosphatase) • Alanine and lactate are Precursors for Gluconeogenesis. • lactate by lactate dehydrogenase form pyruvate. • glycogen by glucokinase or hexokinase it form glucose-6-phosphate and then converted to glucose-1-phosphate by phosphoglucomutase . - glucose-1-phosphate by a reverse reaction (by phosphoglucomutase) can form glucose-6- phosphate and enter Gluconeogenesis process . • Triglyceride by lipolysis turn to glycerol and fatty acids , then glycerol by glycerol kinase form glycerol -3-phosphate the converted to DHAP and enter Gluconeogenesis process. • Pyruvate can convert to Oxaloacetate through Kreb’s cycle, or directly by pyruvate carboxylase , Then OAA by PEPCK (Phosphoenolpyruvate carboxykinase) it converted to PEP (Phosphoenolpyruvate) then enter Gluconeogenesis process. اول4زياده صفحجدا مهمين بسمنين جه جاي اللي كل نفهم عشانقالهم الدكتور منهم وفي
- 5. 5 Carbohydrate Metabolism: Gluconeogenesis, Reciprocal Regulation The dual function enzyme PFK-2/FBPase-2 (Key enzyme responsible for gluconeogenesis and glycolysis) controls flux through gluconeogenesis and glycolysis by controlling levels of F-2,6-BP in the cell Key Concepts: Gluconeogenesis • The importance of gluconeogenesis is to provide glucose for cells from non-carbohydrate precursors. • Three steps in glycolysis must be bypassed by gluconeogenic enzymes in order to overcome large G differences. • Reciprocal regulation at the PFK-1 (glycolysis) and F-1,6-BPase (gluconeogenesis) is controlled by the allosteric regulator F-2,6- bisphosphate, as well as, energy charge (ATP/AMP), and citrate levels. • The Cori Cycle recycles lactate produced in anaerobic muscle cells during exercise by exporting it to the liver where it is converted to pyruvate and used to synthesize glucose by gluconeogenesis.
- 6. 6 ◘Gluconeogenesis and glycolysis are opposing pathways: • Two of the bypass enzymes in gluconeogenesis, fructose- 1,6-bisphosphatase-1 (FBPase-1) and glucose-6- phosphatase, simply reverse the reaction However, 4 extra ATP/GTP, and pyruvate carboxylase and phosphoenolypyruvate carboxykinase (PEPCK), are required to catalyze the bypass reaction that converts pyruvate to PEP. How do you come up with the 4 extra ATP/GTP for gluconeogenesis compared to glycolysis?
- 7. 7 ♦ Reciprocal regulation of PFK-1 and FBPase-1 The activities of PFK-1 and FBPase-1 are regulated by the allosteric effectors AMP, citrate, and fructose-2,6-bisphosphate (F-2,6-BP), but in a reciprocal manner. ال ان عارفين احنا ما زيPFK-1ال هو الليPhospho-fructo Kinase-1ال بيحولي Fructose-6-pلFructose 1,6-bispوالglycolysisالجلوكوز تكسر عشان طريقها في بتمشي ال انزيم عندي والعكسFBPaseهو الليFructose 1,6-bisphosphataseال ال بيحوليFructose 1,6-bispلFructose-6-p ال وعمليهgluconeogenesisجلوكوز تكونلي عشان بتتم عار احنا ما زي طيبال عمليه ان فينglycolysisصح طاقه عنها بينتج..عندي بيبقي يعنيATPكتير!!. ال ان عارفها اكون معلومه في طيبATPل بتتكسرAMPو2Pال تركيز ما كل يعنيAMPال ان ذلك معني يزيدATPوقلت استهلكت.. عندي يكون لما يعنيAMPال اكون عايز طاقه عايز كدا اناATPال اكون عشان الجلوكوز اكسر وعايزATPال عمليه اعمل عايز يعني glycolysis؟ صح ال كدا يبقيAMPعمل زاد لما تركيزهstimulationللPFK-1لل طريقه في يكمل عشانglycolysis عندي انا لو طيبCitrateال في اتكون هو اللي كتيرKreb’s cycleال بعد بتحصل الليglycolysisعملت انا كدا يبقيkreb’s cycle طاقه وعنديATPاعمل اني محتاج فمش كتيرglycolysisال تركيز فبالتالي الجلوكوز في واكسرcitrateيعملInhibitionللPFK-1 ال عمليه في هنعكسه دا الكالم وطبعاgluconeogenesisعندي لو انAMPكتيرعندي انا يبقيATPمحتاج مش انا ساعتها يبقي قليل ال فبالتالي بيه هحتفظ انا ال الجلوكوز في اكسرAMPهيعمل هناInhibitionللFBPase-1وهيبقيstimulateللPFK-1ال لو اما Citrateالجلوكوز في اكسر محتاج مش انا يبقي كتير عندي..ال هعمل فبالتاليgluconeogenesisال في اكسره ما بدل الجلوكوز في وهكون glycolysis ال ان عارفها اكون معلومه وفيfructose-2,6-bisphosphateبيعمل بيتكون لماInhibitionللFructose 1,6-bisphosphataseودا بعدين عنه هنتكلم What is the metabolic logic of reciprocal regulation by citrate?
- 8. 8 • In muscle during exercise, AMP levels are high due to consumption of ATP, so muscle need more ATP by glycolysis. - High amount of AMP stimulate PFK-1 that stimulate glycolysis. • When ATP & Citrate are high - Cells don’t need ATP, so no need for glycolysis. - High amount of citrate indicate that adequate amount of substrate enter TCA cycle, so gluconeogenesis is activated Levels of F-2,6-BP in the cell are controlled by a dual function enzyme called PFK-2/FBPase-2 • The amount of F-2,6-BP in the cell is controlled by the activity of a dual function enzyme containing two catalytic activities, 1) a kinase activity called phosphofructokinase-2 (PFK-2) that phosphorylates fructose-6P to form F- 2,6-BP, and 2) a phosphatase activity called fructose-2,6- bisphosphatase (FBPase-2) that dephosphorylates F-2,6-BP to form fructose-6P. ال كميهF-2,6-BPبتعمل انها كدا قبل قولت الليInhibitionللFructose 1,6- bisphosphataseال عمليه بتوقفلي يعنيgluconeogenesisاصال امتي انا طب ال اعمل بحتاجgluconeogenesisصح اكسره مش جلوكوووز اكون عايز ارفعه عايز وانا الدم في منخفض يكون السكر لما ؟؟ ايه لما..؟؟.. صح..معاك دي المعلومه خلي تمام.. اسمه واحد جزئين من متكون انزيم في الوقتيPFK-2اسمه وواحدFBPase-2.. الPFK-2ال بيحوليfructose-6PلF-2,6-BPال اتكون ما وبعدF-2,6-BPال هو اللي االنزيم من التاني الجزء يجيFBPase-2يحولي الF-2,6-BPلfructose-6P ؟ كدا حلو ال تركيز كدا يعنيF-2,6-BPعاملInhibitionللFructose 1,6-bisphosphataseال ومانعgluconeogenesisدا كدا بس مش عامل كمانStimulationللPFK-1ال عمليه في هيساعد الليglycolysis. عمليه واعمل الدم في السكر مستوي ارفع عايز يعني اكسره مش جلوكوز اكون وعايز عندي انخفض والسكر مشكله عندي لو الوقتي انا طب gluconeogenesis...؟ بقي هيتم اللي ايه.. ال هرمون تفرزلي البنكرياس ان مثال زي دي العمليه هتحفز كتير حاجات فيglucagonال مثال زي تتفرز تانيه هرمونات اوEpinephrine والNor-epinephrine..ال االخر في وتكونلي بقي بتاعها بالميكانيزم تشتغل الهرمونات وبعدهاProtein kinase Aال هو الليPKA
- 9. 9 • During Fasting, Glucagon level increase work on liver cell receptors, then stimulate formation of cAMP that activate formation of Protein Kinase A هيعملي بقي ايه هيعملPhosphorylationجزئين من بيتكون اللي االنزيم علي(PFK-2/FBPase-2)هيحصل فيهم واحد وكلحاجه ه.. ال هو اللي االوالنيPFK-2هيحصلهInhibitionال كميه وبالتاليF-2,6-BPعملتلي قلت لما وبالتالي هتقلstimulateللFructose 1,6-bisphosphataseال حدوث حفزت يعنيgluconeogenesisعملت قلت لما كمان دا كدا بس مشInhibitionللPFK-1عشان ال يوقفglycolysisالجلوكوز تكسير ويوقف. الثاني االنزيم اماFBPase-2بيحصلهstimulationعادي وظيفته ويعمل عاديال ويستهلكF-2,6-BPل ويحولهfructose-6Pفبالتالي ال كميهF-2,6-BPتقل عماله. • In Fed state increase blood glucose stimulate secretion of insulin; that activate protein phosphatase; these enzyme activate net dephophorylation. • When the PFK-2/FBPase-2 dual function enzyme is unphosphorylated, then the PFK-2 activity in the enzyme is stimulated resulting in the net phosphorylation of fructose-6P to produce more F-2,6-BP which stimulates glycolytic flux. يحصله ما قبل بيقولك هناPhosphorylationيعني(dephophorylation)ال كانPFK-2ال بيحولي fructose-6PلF-2,6-BP..ال بيتكون لما الليF-2,6-BPكميته ويزيدبيعملstimulateللPFK-1ال وبالتالي glycolysisهتشتغل. • In contrast, when PFK-2/FBPase-2 is phosphorylated, the activity of FBPase-2 is stimulated, leading to less F-2,6-BP, and reduced flux through glycolysis, with a concomitant increase in flux through gluconeogenesis. ال بقي هناPKAعملهمPhosphorylationفحصلstimulationللFBPase-2ال فكميهF-2,6-BPقلت فلما قلت عملتStimulationللgluconeogenesisوInhibitionللglycolysis
- 10. 10 • Activation of the glucagon receptor in liver cells results in stimulation of protein kinase A signaling, leading to an increase in gluconeogenesis, whereas, insulin signaling stimulates protein phosphatase-1, leading to an increase in glycolysis
- 11. 11 Pentose Phosphate Pathway • We will cover three primary pathways related to carbohydrate metabolism in non-photosynthetic organisms: 1. Pentose phosphate pathway 2. Gluconeogenesis 3. Glycogen metabolism • Metabolism of ribose sugars in the pentose phosphate pathway is used to generate NADPH and to provide the carbohydrate component of nucleotides. • The major sources of carbon in gluconeogenesis are amino acids and glycerol in animals, and glyceraldehyde-3-phosphate (GAP) in plants.
- 12. 12 Key Concepts: The Pentose Phosphate Pathway • The pentose phosphate pathway takes place entirely within the cytoplasm and is also known as the hexose monophosphate shunt or phosphogluconate pathway. • The most important function of the pentose phosphate pathway is to reduce two molecules of NADP+ to NADPH (nicotinamide adenine dinucleotide phosphate) for each glucose-6-phosphate that is oxidatively decarboxylated to ribulose-5-phosphate. • NADPH is functionally similar to NAD+ however, NADPH is the primary reductant in the cell, whereas, NAD+ is the primer oxidant. NADPH is critical to maintaining reduced glutathione levels in cells which is required to minimized damage from reactive oxygen species. • The pentose phosphate pathway is also responsible for producing ribose-5-phosphate which provides the ribose sugar backbone that anchors the nucleotide base to DNA and RNA polymers.
- 13. 13 ♣ There are two distinct phases in the pathway. • The first is the oxidative phase, in which NADPH is generated, and the second is the non- oxidative synthesis of 5-carbon sugars. • The NADPH molecules are important reductant agents that are used in fatty acid biosynthesis, nucleotide biosynthesis, cholesterol biosynthesis, neurotransmitter biosynthesis and various detoxification processes. • When needed, the ribose 5-phosphate can be used to create DNA, RNA and nucleotide-bases molecules such as ATP, NADH, FAD and CoA. Three enzymatic reactions in the oxidative phase • G6PD is the commitment step in the Pentose Phosphate Pathway because 6-Phosphogluconon- d-lactone has no other metabolic fate except to be converted to 6-phosphogluconate.
- 14. 14 The non-oxidative phase of the Pentose Phosphate Pathway (PPP) • The carbon shuffle reactions of the nonoxidative phase are used to regenerate glucose-6P using the same transketolase and transaldolase enzyme reactions as the Calvin Cycle.
- 15. 15 • Six glucose-6P (36 carbons) are metabolized to regenerate five glucose-6P (30 carbons). What happened to the six carbons?
- 16. 16 ♦ Metabolic flux through the Pentose Phosphate Pathway is tightly-regulated: • If increased NADPH is required for biosynthetic pathways. لوعندينقصفيالNADPHالليبحتاجهفيbiosynthetic pathwaysبضطراعملالPPP • If cells need to replenish nucleotide pools. لومحتاجاكونDNAاوRNAهحتاجاكونالRibose-5-p • If ATP levels in the cell are low. لوعندينقصفيالATPهحتاجاكونالGlucose-6-pعشانتدخلالglycolysisوانتجطاقه
- 17. 17 ◘ Regulation of the G6PD activity controls flux through the glycolytic pathway and pentose phosphate pathways: - When NADPH decrease, and NADP+ increase that activate G6PD (Glucose -6-phophate dehydrogenase ) to oxidate glucose, by making Pentose phosphate pathway - When NADPH increase and accumulate it makes feedback inhibition for G6PD so is activate glycolysis. Glucose-6P dehydrogenase deficiency in humans • The pentose phosphate pathway is responsible for maintaining high levels of NADPH in red blood cells (erythrocytes) for use as a reductant in the glutathione reductase reaction. • Glutathione is a tripeptide that has a free sulfhydryl group which functions as an electron donor in a variety of coupled redox reactions in the cell.
- 18. 18 ◘ Glucose-6P dehydrogenase deficiency in humans: • When erythrocytes are exposed to chemicals that generate high levels of superoxide radicals, GSH is required to reduce these damaging compounds. • The pentose phosphate pathway in erythrocytes normally provides sufficient levels of NADPH to maintain the GSH:GSSG ratio at about 500:1. • Primaquine inhibits growth of the malaria parasite in red blood cells by creating a hostile environment. - The biochemical basis for this drug-induced illness was found to be lower than normal levels of NADPH due to a G6PD deficiency. • The acute hemolytic anemia seen in individuals with G6PD who are treated with primaquine explains the symptoms of favism. - One of the compounds in fava beans is vicine, a toxic glycoside that induces oxidative stress in erythrocytes.
- 19. 19 HEXOSE MONOPHOSPHATE PATHWAY (HMP- PATHWAY) • The pentose phosphate pathway (also called the phosphogluconate pathway and the hexose monophosphate shunt) ♦ Definition: • HMP pathway is an alternative pathway for glucose oxidation involving the formation of pentose phosphates as intermediates. ♦ Site: • It is very active in the cytosol of certain tissues: 1. Liver 2. Lactating mammary gland 3. RBCs 4. Adipose tissue 5. Adrenal cortex 6. Eye (retina, cornea & lens) 7. Testis - Ovaries - Placenta ♦ IMPORTANCE of HMP I. Formation of Ribose-5-P (Active ribose phosphate): • Ribose-5-P is important for synthesis nucleotides & nucleic acids (DNA & RNA). • N.B. Dietary Ribose CAN NOT be utilized by our tissues and are excreted in urine because there is NO Ribokinase enzyme to convert it to Ribose-5- phosphate.
- 20. 20 II. Formation of NADPH (reduced NADP): • NADPH is important for many enzymes and reductive synthetic pathways: e.g. 1. Synthesis of Fatty Acids (Lipogenesis). - This occurs mainly in adipose tissue, liver and lactating mammary glands. NADPH is coenzyme for certain reductases. 2. Synthesis of cholesterol. - NADPH is coenzyme for b-hydroxy, b-methyl glutaryl-CoA Reductase (HMG- CoA Reductase) the key enzyme in cholesterol biosynthesis. 3. Synthesis of steroid hormones. - This occurs mainly in adrenal cortex, testis, ovaries and placenta. - NADPH is coenzyme for certain hydroxylases. 4. Keeps glutathione in the reduced state (G-SH). ♣ Reduced glutathione (G-SH) functions as : A. Coenzyme for the enzyme G-SH peroxidase which protect RBCs against H2O2. B. Coenzyme for the enzyme met-hemoglobin reductase which keeps the iron of Hb in the ferrous state (Fe2+ ) thus preserving its capacity to carry oxygen. C. Stabilizer to the proteins of cell membranes, particularly in RBCs. H2O2 2 G-SH G-S-S-G2 H2O NADP + NADPH H + + Glutathione peroxidase Glutathione Reductase HMP- Shunt Se
- 21. 21 STEPS of HMP- PATHWAY • Glucose-6-P is dehydrogenated to 6-phospho-gluconic acid. - The hydrogen carrier is NADP that is reduced to NADPH. - The reaction is catalyzed by glucose-6-phosphate dehydrogenase (G-6-PD). • 6-phosphogluconate is dehydrogenated and decarboxylated to ribulose-5-Phosphate. - NADP is reduced to NADPH. - The reaction is catalyzed by 6-phospho gluconate dehydrogenase (6-P gluconate DH). • The 2 dehydrogenases of HMP: G-6-PD and 6-P gluconate DH use NADP as hydrogen carrier. - NADPH is formed. -كملباقي الsteps Xylulose-5-P Ribose-5-P Xylulose-5-P Sedoheptulose-7-PGlyceraldehyde-3-P Erythrose-4-PFructose-6-P Glucose-6-P Transketolase TPP Transaldolase Fructose-6-P Glyceraldehyde-3-P Transketolase TPP +NADPH H+ NADP+ P C C C C C CH2O OH OH HO H H H H O O PP O C C C C C CH2O OH OH HO H H H H OHH H H H H HO OH OH CH2O C C C C OH COOH H2O Glucose-6-phosphate Dehydrogenase Hydrolase Glucose-6-phosphate 6-phospho-gluconolactone 6-phospho-gluconic acid H H H OH OH CH2O C C C C OH COOH O PP NADP+ NADPH H++ 6-phospho-gluconate dehydrogenase H H OH CH2O C C C OH O CH2OH CO2 3-keto-6-phospho- gluconic acid Ribulose-5-phosphate H CH2O C C C OH O CH2OH HO H H H OH CH2O C C OH C CHO OHH P P 3-epimerase isomerase Xylulose-5-P Ribose-5-P Mn++ Hexose Monophosphate Shunt ( HMP-shunt) Isomerase
- 22. 22 ◘ Regulation of HMP pathway: • The key enzymes of HMP is the 2 dehydrogenases: G-6-PD and 6-P gluconate DH. • CHO feeding stimulates insulin secretion; insulin induces the synthesis of G-6- PD and 6-P gluconate DH and HMP is activated. • Fasting inhibits insulin secretion; and stimulates glucagons secretion that represses the synthesis of G-6-PD and 6-P gluconate DH and HMP is inhibited. • CHO feeding blood glucose insulin HMP. • Fasting blood glucose glucagon HMP. FAVISM • Favism is an inborn error of metabolism caused by congenital deficiency of G-6- PD enzyme due to DNA mutation of the G-6-PD gene. • Favism is a genetically inherited disease characterized by increased fragility of RBCs and hemolysis that occurs after intake of fava beans or after the intake of some drugs (e.g. anti-malarial drugs). • The congenital deficiency of G-6-PD decreases the activity of HMP pathway in RBCs leading to decrease in reduced NADP (NADPH). • Fava beans and certain drugs [anti-malarial drugs (primaquinone), sulfa drugs (sulfonamides), phenacetin, nitrofurans, salicylates..] cause the increased production of oxidizing agents and H2O2. • No enough NADPH for reduction of oxidized glutathione (G-S-S-G) to reduced glutathione (G-SH). • The oxidizing agents and H2O2 attack the plasma membrane of the RBCs causing its destruction. • This leads to marked hemolysis and hemolytic anemia.
- 23. 23 • Diagnosis: Favism is diagnosed by measuring the activity of G-6-PD in RBCs. G-6-PD activity is markedly decreased in favism. • Treatment: ♣ No specific treatment but we can: • Blood transfusion after the hemolytic crisis. • Avoid the intake of fava beans and oxidizing drugs. Main differences between glycolysis and HMP GALACTOSE METABOLISM • The main source of galactose in food is lactose of milk. • Lactose by intestinal lactase gives glucose and galactose which is absorbed from the intestine and goes via portal blood to the liver. • In the liver: Galactose is converted to Glucose with the help of three enzymes: galactokinase; galactose-1-P uridyl transferase or UDP-Gal 4-epimerase.
- 24. 24 GALACTOSEMIA • Galactosemia is a congenital disease caused by deficiency of galactokinase; galactose-1-P uridyl transferase or UDP-Gal 4-epimerase. ♣ Galactosemia is characterized by: 1)- Galactosemia: increased blood galactose 2)- Galactosuria: excretion of large amounts of galactose in urine. 3)- Cataract : Opacity in eye lens that looks white in color 4)- Mental retardation ( problem in the brain ) 5)- Liver cell failure • Treatment: - It must be started early in life. - The baby must feed lactose-free milk formula and galactose-free diet.
- 25. 25 FRUCTOSE METABOLISM • Sources of fructose: Diet; Sucrose (table sugar) and fruits. • In the liver, fructose is either converted to glucose or oxidized through the glycolysis pathway to pyruvic acid. • Excess fructose in liver is converted to glucose. • The enzymes are: Fructokinase and Aldoalse-B. • Fructose is secreted in semen in a high concentration, its level in seminal fluid is 200 – 600 mg/dl. • Spermatozoa utilize fructose rather than glucose as a source of energy. Inborn Errors of Fructose Metabolism 1- Essential Fructosuria: • Inborn error of fructose metabolism caused by deficiency of Fructokinase in liver. - Fructose is not converted to glucose in liver, its level is increased in blood (Fructosemia) and excreted in large amount in urine (Fructosuria). - It is a harmless condition. 2- Hereditary Fructose Intolerance: • Inborn error of fructose metabolism caused by congenital deficiency of Aldolase B in liver cells. - Ingestion of fructose or sucrose by these patients leads to fasting hypoglycemia that might lead to coma and even death. - Liver cell failure. - So, Hereditary fructose intolerance is more dangerous than essential fructosuria. • Treatment: Sucrose and fructose-free diet. ايdiagramاوصورةمتحددهباطاراسودغامقيبقيعليناغيركدايبقيللتوضيح.
