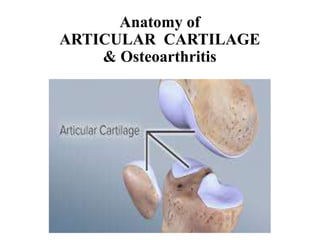
Anatomy of articular cartilage & Osteoarthritis
- 1. Anatomy of ARTICULAR CARTILAGE & Osteoarthritis
- 2. Articular cartilage • Highly specialized connective tissue covering bone epiphyses in synovial joints • Found at articulating ends of bones within joints of body • Hyaline cartilage and is 2 to 4 mm thick • Function Load-bearing material of the joints Provide excellent lubrication & great wear characteristic • Limited capacity for intrinsic healing and repair Limited potential of chondrocytes for replication Devoid of blood vessels, lymphatics, nerve (Nutrition ?)
- 3. Structure of articular cartilage 4 zones of articular cartilage Superficial zone Middle zone Deep zone Calcified zone Within each zone, 3 regions can be identified Pericellular region Territorial region Interterritorial region
- 9. Take home questions • How is microanatomy of articular cartilage damaged in OA ? • Why more in older age group ? • Is Osteoarthritis only a disease of articular cartilage ? • Why gender differences in OA ? • Immobilization Vs OA
- 10. Why OA ? • Most common chronic musculoskeletal disorder • Most prevalent cartilage degenerative disease • Substantial economic burden • Leading cause of activity limitation & absenteeism among working-age adults • Significant decline in function among older individuals.
- 11. Age related changes • Dissipation of chondrocytes in the superficial region, followed by an increase in number of chondrocytes in the deep layers. • Decrease in the proteoglycan aggregate numbers within the ECM. May be a result of Proteolytic damage to link protein & glycosaminoglycan chains Increase in partially degraded hyaluronan without newly synthesized molecules • Increased mechanical forces exerted on the tissue further lead to subchondral tissue calcification
- 12. Pathogenesis of OA • Trauma causes a microfracture or inflammation • Slight increase in enzymatic activity which allow formation of “ wear” particles, engulfed by resident macrophages. • Production of “wear” particles overwhelms ability of system to eliminate & they become mediators of inflammation, stimulating chondrocyte to release degradative enzymes • Molecules from breakdown of collagen & proteoglycan, also taken up by synovial macrophages, cause release of proinflammatory cytokines, like TNFα, IL-1 and IL-6. • These cytokines bind to chondrocyte receptors leading to further release of metalloproteinases & inhibition of type II collagen production, thus increasing cartilage degradation • Increased water content & decreased proteoglycan content of ECM, weakening of the collagen network due to decreased synthesis of type II collagen & increased breakdown of pre- existing collagen
- 13. Females Vs OA • Anatomical factor Decrease articular cartilage volume than male • Previous history of trauma Women more cartilage wear, increase ACL injury • Hormonal factor Estrogen beneficial effect in articular cartilage Increase proteoglycan in cartilage • Social factors Present for t/t in more advanced stages of OA, so more pain & disability HCW more likely to recommend total joint arthroplasty for male patient
- 14. Is Osteoarthritis only a disease of articular cartilage ? • Initially, osteoarthritis considered disease of articular cartilage • Recent research indicate involvement of entire joint • subchondral bone • synovium • menisci • ligaments, periarticular muscles and nerves
- 15. Subchondral bone • Concomitant increase in levels of cartilage oligomeric matrix protein (COMP) & bone sialoprotein (BSP) in people with early osteoarthritis • progressive increase in subchondral bone plate thickness • formation of new bone at the joint margins – osteophytes • In osteoarthritic bone tissue, ratio of α1 & α2 chains of type I collagen varied between 4:1 & 17:1, and this appears to be responsible for abnormal mineralization pattern In normal bone, type I collagen consist of heterotrimer of α1 & α2 chains at an average ratio of 2.4:1.
- 16. • Synovial membrane of osteoarthritic joints commonly exhibits hyperplasia of lining cell layer occasionally accompanied by focal infiltration of lymphocytes & monocytes in sublining layers • Meniscal degeneration : menisci appear torn, fissured, fragmented, macerated or completely destroyed
- 17. • The loss of articular cartilage thought to be primary change, but a combination of cellular changes & biomechanical stresses causes several secondary changes, including subchondral bone remodeling, formation of osteophytes development of bone marrow lesions change in the synovium, joint capsule, ligaments & periarticular muscles meniscal tears and extrusion
- 18. Immobility Vs OA • Mechanical load necessary for cartilage homeostasis. • Induces fluid movement between cartilage & synovial fluid, that helps in diffusion of molecules across cartilage thus facilitating its nutrition • Decrease protease (MMP-3, ADAMTS-5) expression in human chondrocytes • Increases proteoglycan (aggrecan) • Inhibits IL-1 & TNF-α induced inflammatory & catabolic responses • immobilization leads to joint damage
- 20. Normoxia Vs hyoxia • Since cartilage is an avascular tissue, chondrocytes live in a hypoxic environment • Hypoxia displays a protective effect on cartilage • Lower basal synthesis & release of MMP-1, MMP-13 • Lower generation of type II collagen cleavage fragments • HIF-1α promote chondrocyte function and survival • Gene encoding HIF-1α, Epas1 expressed in cartilage • Deletion of Epas1 gene in cartilaginous growth plate associated with chondrocyte apoptosis • Inhibitor of HIF-1,intraarticular injection promote cartilage degradation & osteophyte formation
- 21. References • Sophia Fox AJ, Bedi A, Rodeo SA. The basic science of articular cartilage: structure, composition, and function. Sports Health. 2009;1(6):461-468. • Houard X, Goldring MB, Berenbaum F. Homeostatic mechanisms in articular cartilage and role of inflammation in osteoarthritis. Curr Rheumatol Rep. 2013;15(11):375.
- 22. THANK YOU
