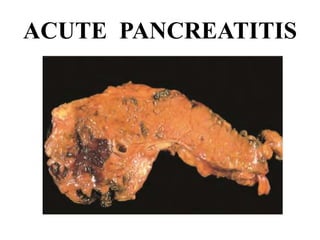
Management of Acute Pancreatitis
•Download as PPTX, PDF•
0 likes•471 views
Let's learn the management of acute pancreatitis.
Report
Share
Report
Share
Recommended
Recommended
More Related Content
What's hot
What's hot (20)
Similar to Management of Acute Pancreatitis
Similar to Management of Acute Pancreatitis (20)
CHOs Gastrointestinal Disease presentation z 2.ppt

CHOs Gastrointestinal Disease presentation z 2.ppt
Acute pancreatitis nursing care plan & management

Acute pancreatitis nursing care plan & management
Recent management of gerd from consensus to clinical application dr taulin ag...

Recent management of gerd from consensus to clinical application dr taulin ag...
More from Manoj Khadka
More from Manoj Khadka (20)
NORMAL TENSION GLAUCOMA "An exception in the glaucoma family"

NORMAL TENSION GLAUCOMA "An exception in the glaucoma family"
Recently uploaded
PEMESANAN OBAT ASLI : +6287776558899
Cara Menggugurkan Kandungan usia 1 , 2 , bulan - obat penggugur janin - cara aborsi kandungan - obat penggugur kandungan 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 bulan - bagaimana cara menggugurkan kandungan - tips Cara aborsi kandungan - trik Cara menggugurkan janin - Cara aman bagi ibu menyusui menggugurkan kandungan - klinik apotek jual obat penggugur kandungan - jamu PENGGUGUR KANDUNGAN - WAJIB TAU CARA ABORSI JANIN - GUGURKAN KANDUNGAN AMAN TANPA KURET - CARA Menggugurkan Kandungan tanpa efek samping - rekomendasi dokter obat herbal penggugur kandungan - ABORSI JANIN - aborsi kandungan - jamu herbal Penggugur kandungan - cara Menggugurkan Kandungan yang cacat - tata cara Menggugurkan Kandungan - obat penggugur kandungan di apotik kimia Farma - obat telat datang bulan - obat penggugur kandungan tuntas - obat penggugur kandungan alami - klinik aborsi janin gugurkan kandungan - ©Cytotec ™misoprostol BPOM - OBAT PENGGUGUR KANDUNGAN ®CYTOTEC - aborsi janin dengan pil ©Cytotec - ®Cytotec misoprostol® BPOM 100% - penjual obat penggugur kandungan asli - klinik jual obat aborsi janin - obat penggugur kandungan di klinik k-24 || obat penggugur ™Cytotec di apotek umum || ®CYTOTEC ASLI || obat ©Cytotec yang asli 200mcg || obat penggugur ASLI || pil Cytotec© tablet || cara gugurin kandungan || jual ®Cytotec 200mcg || dokter gugurkan kandungan || cara menggugurkan kandungan dengan cepat selesai dalam 24 jam secara alami buah buahan || usia kandungan 1_2 3_4 5_6 7_8 bulan masih bisa di gugurkan || obat penggugur kandungan ®cytotec dan gastrul || cara gugurkan pembuahan janin secara alami dan cepat || gugurkan kandungan || gugurin janin || cara Menggugurkan janin di luar nikah || contoh aborsi janin yang benar || contoh obat penggugur kandungan asli || contoh cara Menggugurkan Kandungan yang benar || telat haid || obat telat haid || Cara Alami gugurkan kehamilan || obat telat menstruasi || cara Menggugurkan janin anak haram || cara aborsi menggugurkan janin yang tidak berkembang || gugurkan kandungan dengan obat ©Cytotec || obat penggugur kandungan ™Cytotec 100% original || HARGA obat penggugur kandungan || obat telat haid 1 bulan || obat telat menstruasi 1-2 3-4 5-6 7-8 BULAN || obat telat datang bulan || cara Menggugurkan janin 1 bulan || cara Menggugurkan Kandungan yang masih 2 bulan || cara Menggugurkan Kandungan yang masih hitungan Minggu || cara Menggugurkan Kandungan yang masih usia 3 bulan || cara Menggugurkan usia kandungan 4 bulan || cara Menggugurkan janin usia 5 bulan || cara Menggugurkan kehamilan 6 Bulan
________&&&_________&&&_____________&&&_________&&&&____________
Cara Menggugurkan Kandungan Usia Janin 1 | 7 | 8 Bulan Dengan Cepat Dalam Hitungan Jam Secara Alami, Kami Siap Meneriman Pesanan Ke Seluruh Indonesia, Melputi: Ambon, Banda Aceh, Bandung, Banjarbaru, Batam, Bau-Bau, Bengkulu, Binjai, Blitar, Bontang, Cilegon, Cirebon, Depok, Gorontalo, Jakarta, Jayapura, Kendari, Kota Mobagu, Kupang, LhokseumaweCara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...

Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...Cara Menggugurkan Kandungan 087776558899
Recently uploaded (20)
👉Chandigarh Call Girl Service📲Niamh 8868886958 📲Book 24hours Now📲👉Sexy Call G...

👉Chandigarh Call Girl Service📲Niamh 8868886958 📲Book 24hours Now📲👉Sexy Call G...
👉 Amritsar Call Girls 👉📞 8725944379 👉📞 Just📲 Call Ruhi Call Girl Near Me Amri...

👉 Amritsar Call Girls 👉📞 8725944379 👉📞 Just📲 Call Ruhi Call Girl Near Me Amri...
Bandra East [ best call girls in Mumbai Get 50% Off On VIP Escorts Service 90...

Bandra East [ best call girls in Mumbai Get 50% Off On VIP Escorts Service 90...
VIP Hyderabad Call Girls KPHB 7877925207 ₹5000 To 25K With AC Room 💚😋

VIP Hyderabad Call Girls KPHB 7877925207 ₹5000 To 25K With AC Room 💚😋
Most Beautiful Call Girl in Chennai 7427069034 Contact on WhatsApp

Most Beautiful Call Girl in Chennai 7427069034 Contact on WhatsApp
7 steps How to prevent Thalassemia : Dr Sharda Jain & Vandana Gupta

7 steps How to prevent Thalassemia : Dr Sharda Jain & Vandana Gupta
Jual Obat Aborsi Di Dubai UAE Wa 0838-4800-7379 Obat Penggugur Kandungan Cytotec

Jual Obat Aborsi Di Dubai UAE Wa 0838-4800-7379 Obat Penggugur Kandungan Cytotec
🚺LEELA JOSHI WhatsApp Number +91-9930245274 ✔ Unsatisfied Bhabhi Call Girls T...

🚺LEELA JOSHI WhatsApp Number +91-9930245274 ✔ Unsatisfied Bhabhi Call Girls T...
Dehradun Call Girls Service {8854095900} ❤️VVIP ROCKY Call Girl in Dehradun U...

Dehradun Call Girls Service {8854095900} ❤️VVIP ROCKY Call Girl in Dehradun U...
❤️Call Girl Service In Chandigarh☎️9814379184☎️ Call Girl in Chandigarh☎️ Cha...

❤️Call Girl Service In Chandigarh☎️9814379184☎️ Call Girl in Chandigarh☎️ Cha...
💰Call Girl In Bangalore☎️63788-78445💰 Call Girl service in Bangalore☎️Bangalo...

💰Call Girl In Bangalore☎️63788-78445💰 Call Girl service in Bangalore☎️Bangalo...
Gastric Cancer: Сlinical Implementation of Artificial Intelligence, Synergeti...

Gastric Cancer: Сlinical Implementation of Artificial Intelligence, Synergeti...
Bhawanipatna Call Girls 📞9332606886 Call Girls in Bhawanipatna Escorts servic...

Bhawanipatna Call Girls 📞9332606886 Call Girls in Bhawanipatna Escorts servic...
💚Chandigarh Call Girls Service 💯Piya 📲🔝8868886958🔝Call Girls In Chandigarh No...

💚Chandigarh Call Girls Service 💯Piya 📲🔝8868886958🔝Call Girls In Chandigarh No...
Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...

Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...
💚Call Girls In Amritsar 💯Anvi 📲🔝8725944379🔝Amritsar Call Girl No💰Advance Cash...

💚Call Girls In Amritsar 💯Anvi 📲🔝8725944379🔝Amritsar Call Girl No💰Advance Cash...
👉 Chennai Sexy Aunty’s WhatsApp Number 👉📞 7427069034 👉📞 Just📲 Call Ruhi Colle...

👉 Chennai Sexy Aunty’s WhatsApp Number 👉📞 7427069034 👉📞 Just📲 Call Ruhi Colle...
Call Girls Shahdol Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Shahdol Just Call 8250077686 Top Class Call Girl Service Available
Circulatory Shock, types and stages, compensatory mechanisms

Circulatory Shock, types and stages, compensatory mechanisms
Management of Acute Pancreatitis
- 2. LEARNING OBJECTIVES To explain principles of management of acute pancreatitis. To discuss the drug therapy in acute pancreatitis.
- 3. MANAGEMENT OF ACUTE PANCREATITIS Establishing the diagnosis and stratifying disease Management of pain Management of fluid losses Role of prophylactic antibiotics Nutritional support Management of complications Management of underlying cause
- 4. Management of pain Pethidine (Meperidine), Tramadol preferred No Morphine - Morphine can induce spasm of sphincter of Oddi and worsen biliary pancreatitis Management of fluid losses Fluid loss is both externally and internally Managed by normal saline and / or colloids
- 5. Role of prophylactic antibiotics Not indicated in mild acute pancreatitis Often used in severe acute pancreatitis - Broad spectrum intravenous antibiotics like imipenem with cilastatin and cefuroxime Nutritional support ‘Nil by mouth’ Enteral (nasogastric) feeding -Reduces incidence of pancreatic infections
- 6. Management of complications Complications Management Hyperglycemia Using insulin Hypocalcemia IV calcium if tetany occurs ARDS Oxygen therapy Acute renal failure Hemodialysis / peritoneal dialysis Acute pseudocyst Urgent drainage into stomach / duodenum if pseudocyst > 6cm Pancreatic necrosis Necrosectomy
- 7. Management of underlying cause Gallstones • Cholecystectomy (same admission) Role of ERCP in acute pancreatitis • To diagnose choledocholithiasis • To manage choledocholithiasis by biliary sphincterotomy
- 8. REFERENCES Bailey & Love’s SHORT PRACTICE OF SURGERY ; 26th EDITION; 2013; (Page no. 1127-1133) Davidson’s Principles & Practice of Medicine ; 21st EDITION; 2010; (Page no. 889-891) HARRISON’S PRINCIPLES OF INTERNAL MEDICINE ; 18th EDITION; VOLUME 2; 2012 ; ( Page no. 2635-2643)
- 9. “THANK YOU”
