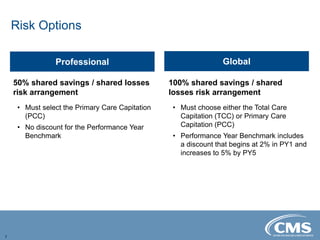
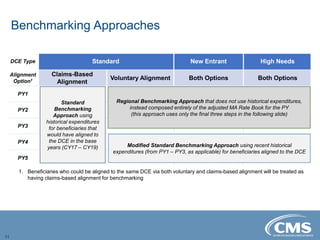
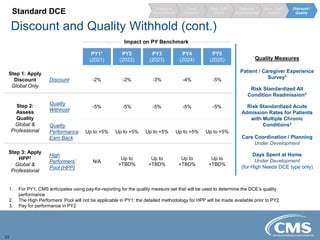
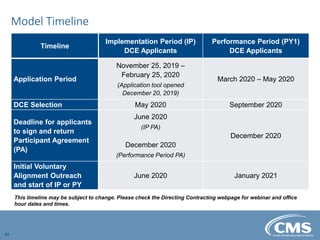
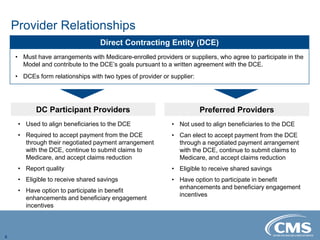
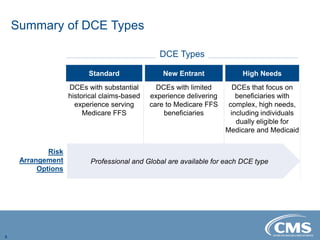
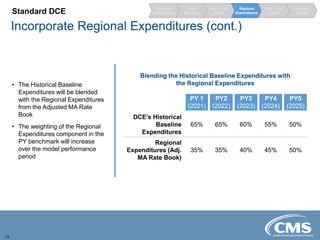
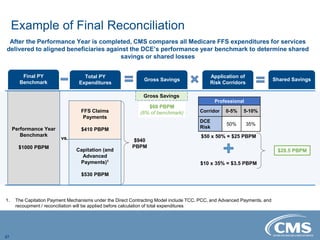
The document provides an overview of the Direct Contracting Model introduced by CMS, focused on enhancing risk-sharing arrangements in Medicare fee-for-service. It details various benchmarks, payment mechanisms, and the types of Direct Contracting Entities (DCEs), including new entrants and those serving high-needs populations. The financial methodologies for this model are still developing, and further information will be released by CMS as it becomes available.