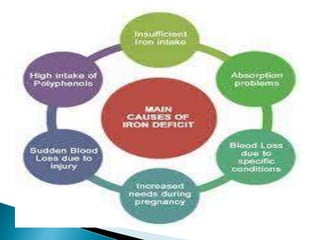
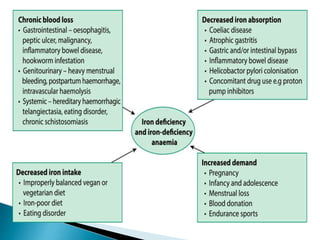
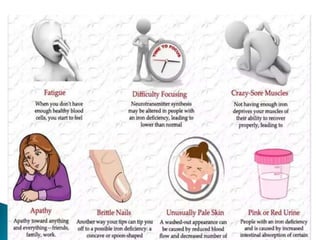
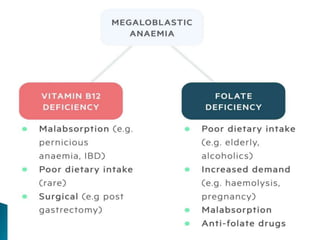
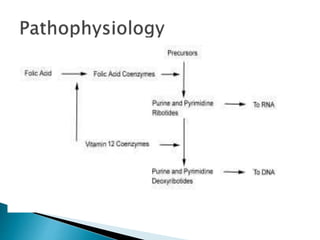
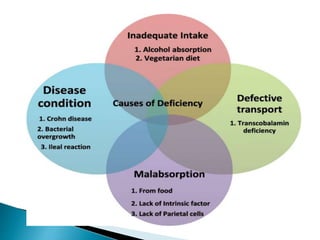
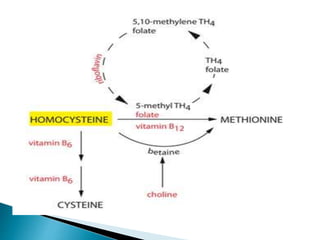
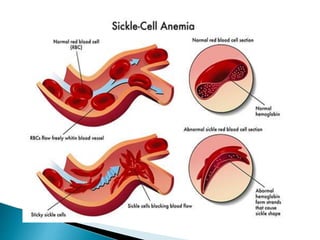
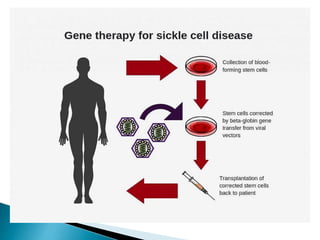
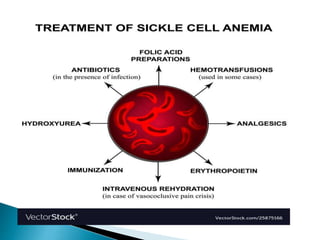
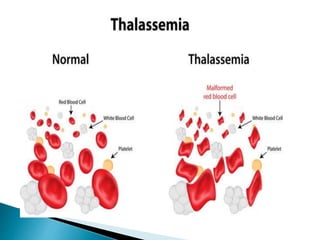
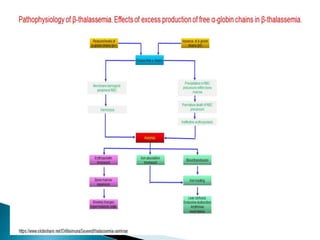
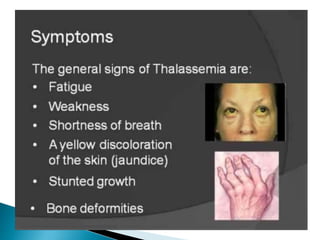
This document discusses different types of anemia. It describes iron deficiency anemia, vitamin B12 and folate deficiency anemias, sickle cell anemia, and thalassemia. Iron deficiency anemia is the most common type and results from not enough dietary iron intake or too much blood loss. Vitamin B12 and folate deficiencies can cause large red blood cell size due to impaired DNA synthesis. Sickle cell anemia is a genetic disorder where red blood cells become sickle shaped and clog blood vessels. Thalassemia is also genetic and causes low hemoglobin levels due to alpha or beta chain mutations.