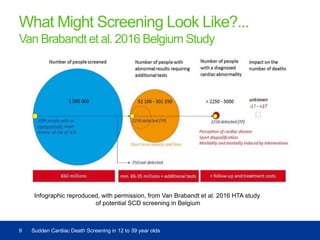
The UK National Screening Committee has reviewed sudden cardiac death screening for individuals aged 12 to 39, highlighting the lack of high-quality evidence supporting its effectiveness in reducing incidence. Their findings noted significant uncertainties about the condition and test performance, leading to a recommendation against a systematic screening program. The consultation revealed differing opinions among stakeholders regarding the management of risk factors and the implications of current screening strategies.