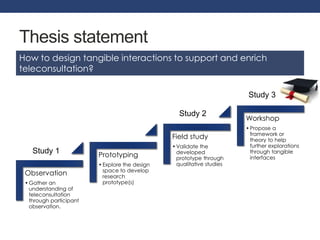
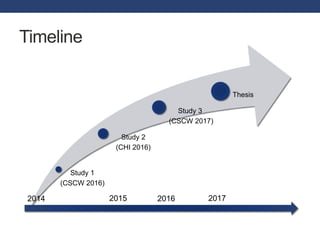
The document discusses how to enhance teleconsultation in rural areas using tangible interfaces to address challenges in physical diagnosis and user interactions. It outlines a research plan involving participant observation, prototyping, and qualitative studies to develop and validate a framework for supporting teleconsultation. The author, Deepti Aggarwal, highlights the importance of understanding user experiences and technical communication in the design process.