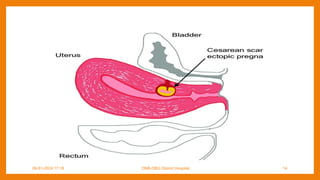
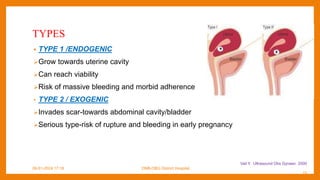
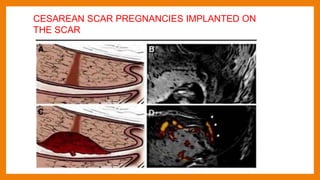
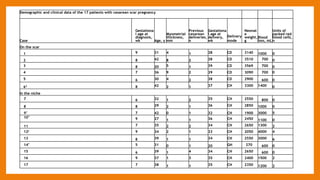
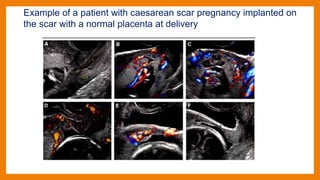
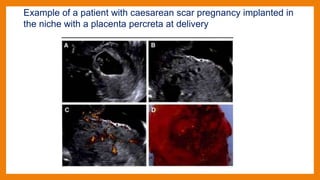
This study compared outcomes of cesarean scar pregnancies (CSP) implanted on the scar versus in the niche. Of 17 CSP cases, 6 were implanted on the scar and 11 in the niche. Those implanted on the scar had better outcomes: they did not develop morbidly adherent placenta and 5/6 delivered via c-section. Those implanted in the niche all developed morbidly adherent placenta and required hysterectomy, with 10/11 having placenta increta/percreta. CSP implanted in the niche may have worse outcomes than those implanted directly on the scar.