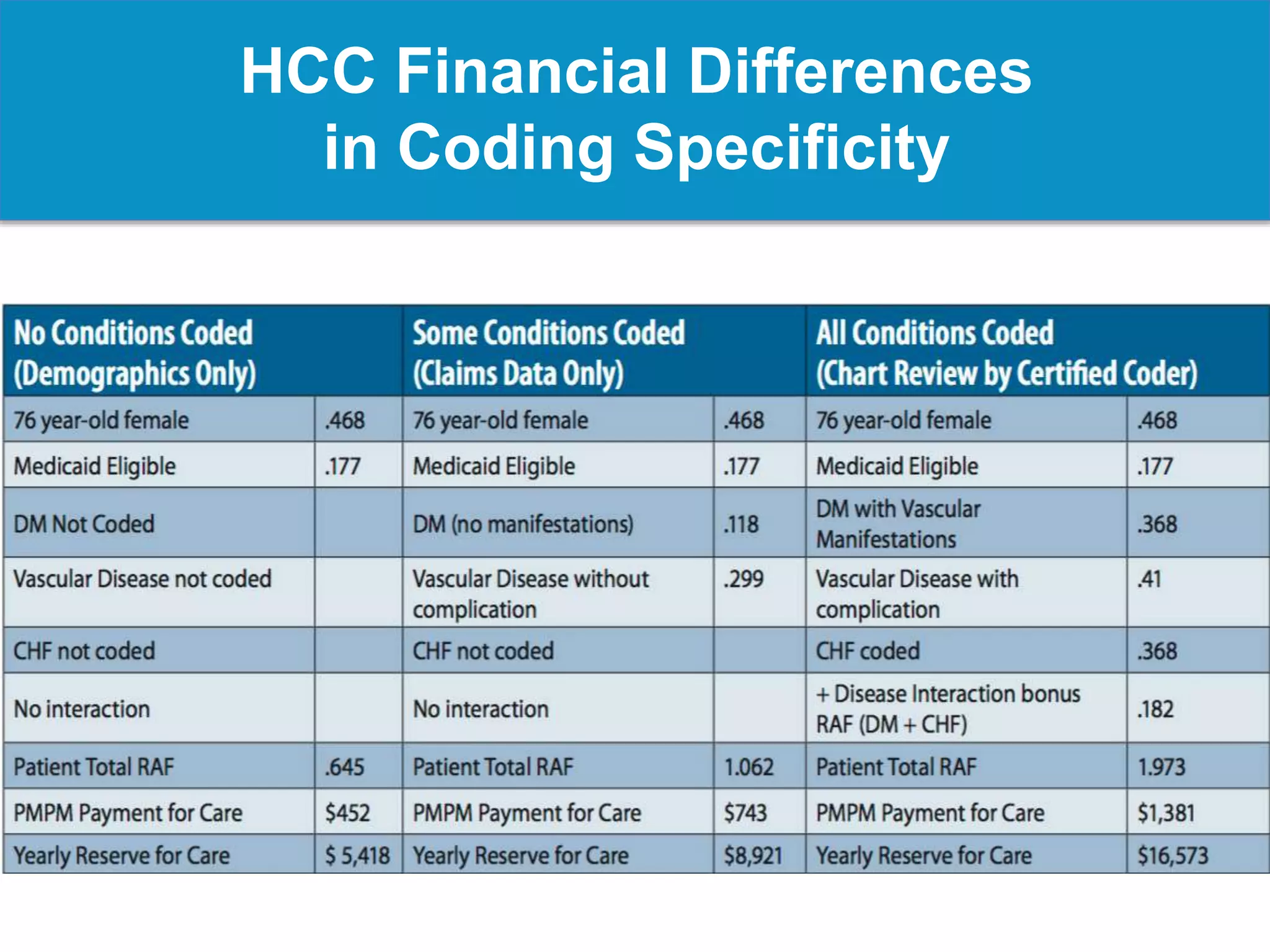
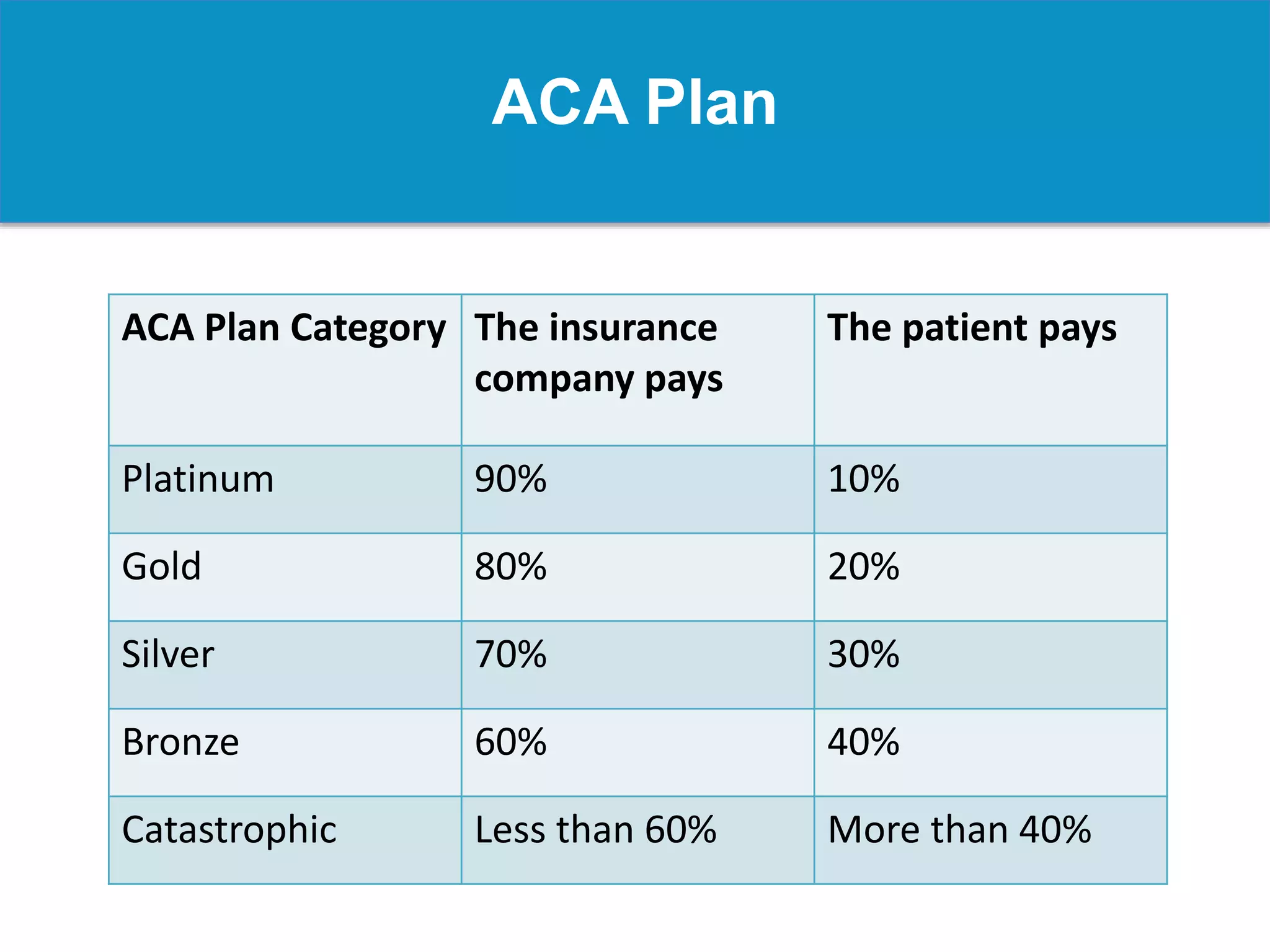
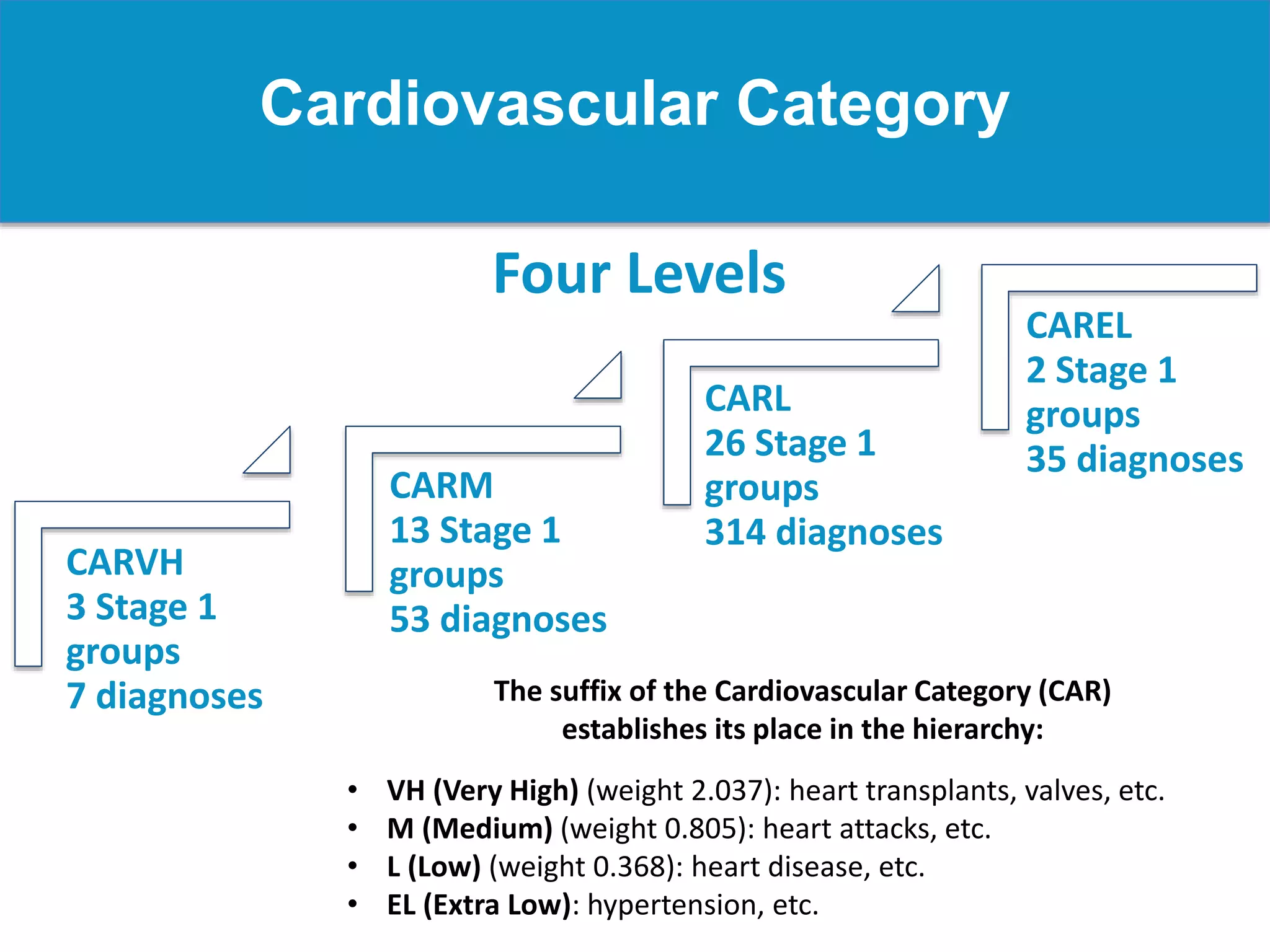
Risk adjustment is a methodology used to evaluate patient wellness by accounting for various health data elements, ensuring equitable comparisons among patients. It involves determining factors such as age, gender, socioeconomic status, and specific conditions to assess patient-level risks, influencing funding and reimbursement for healthcare providers. Accurate documentation and coding are crucial for reflecting patient acuity, which impacts the financial outcomes under risk adjustment systems, particularly for Medicare and Medicaid plans.