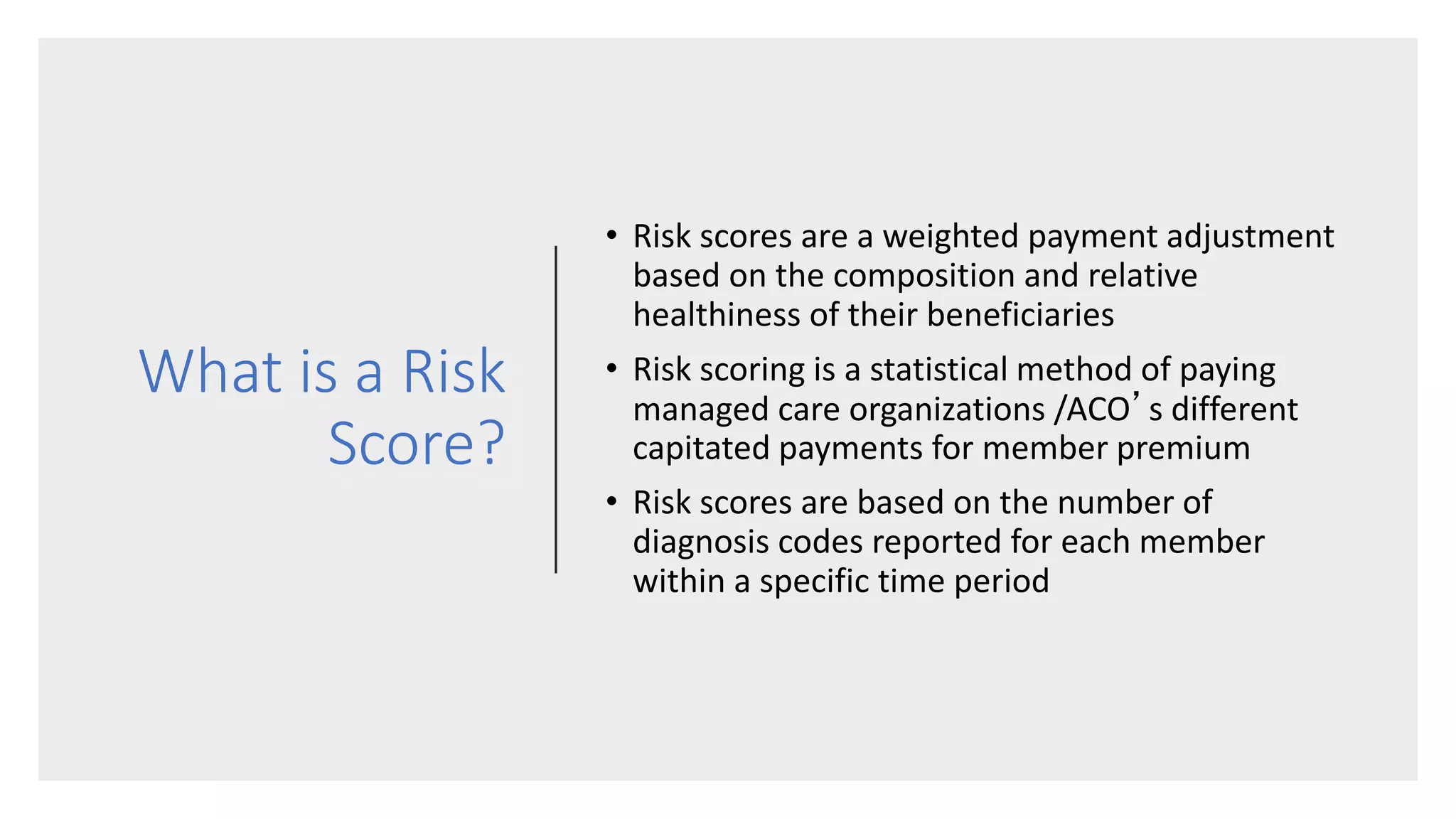
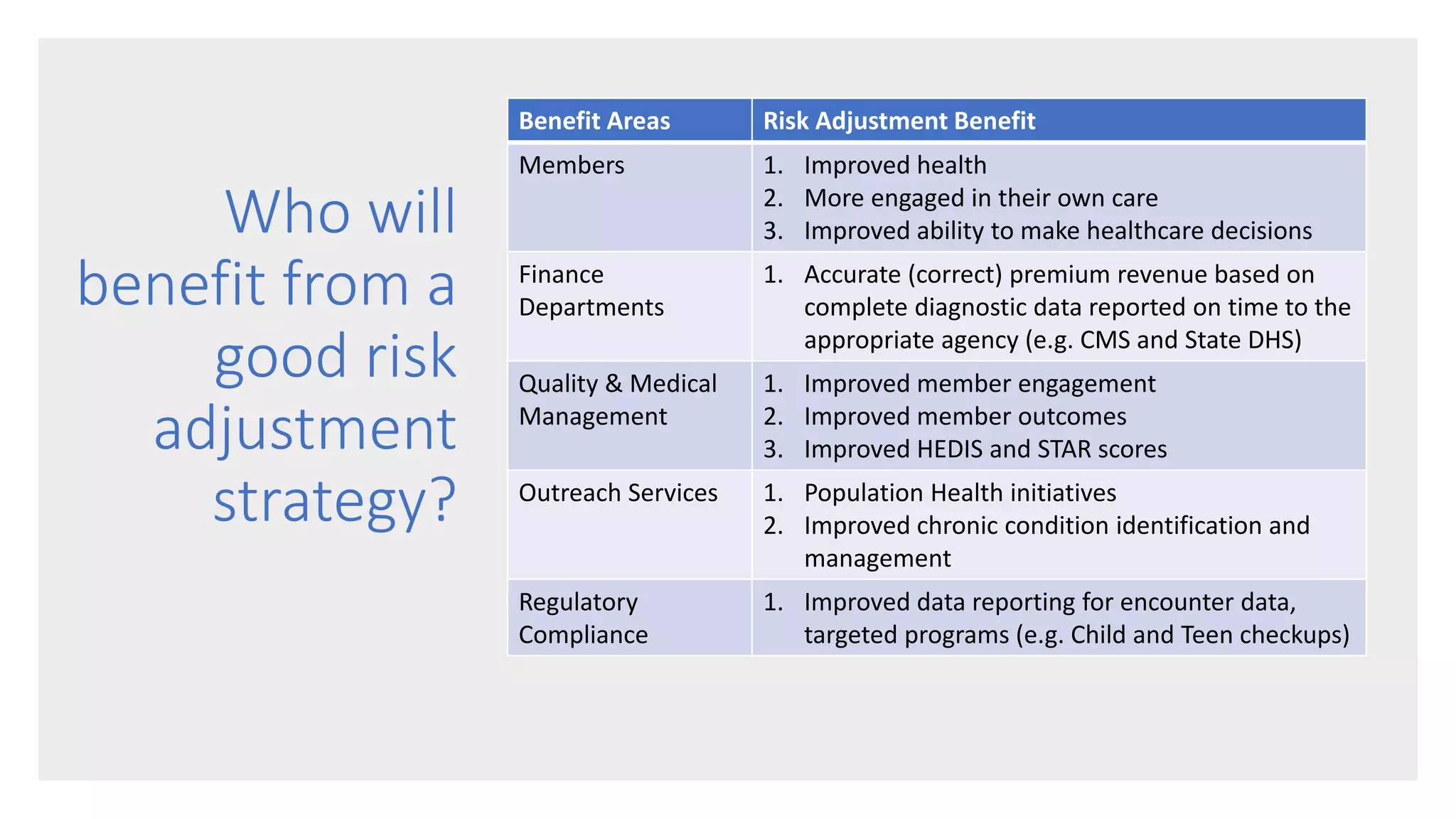
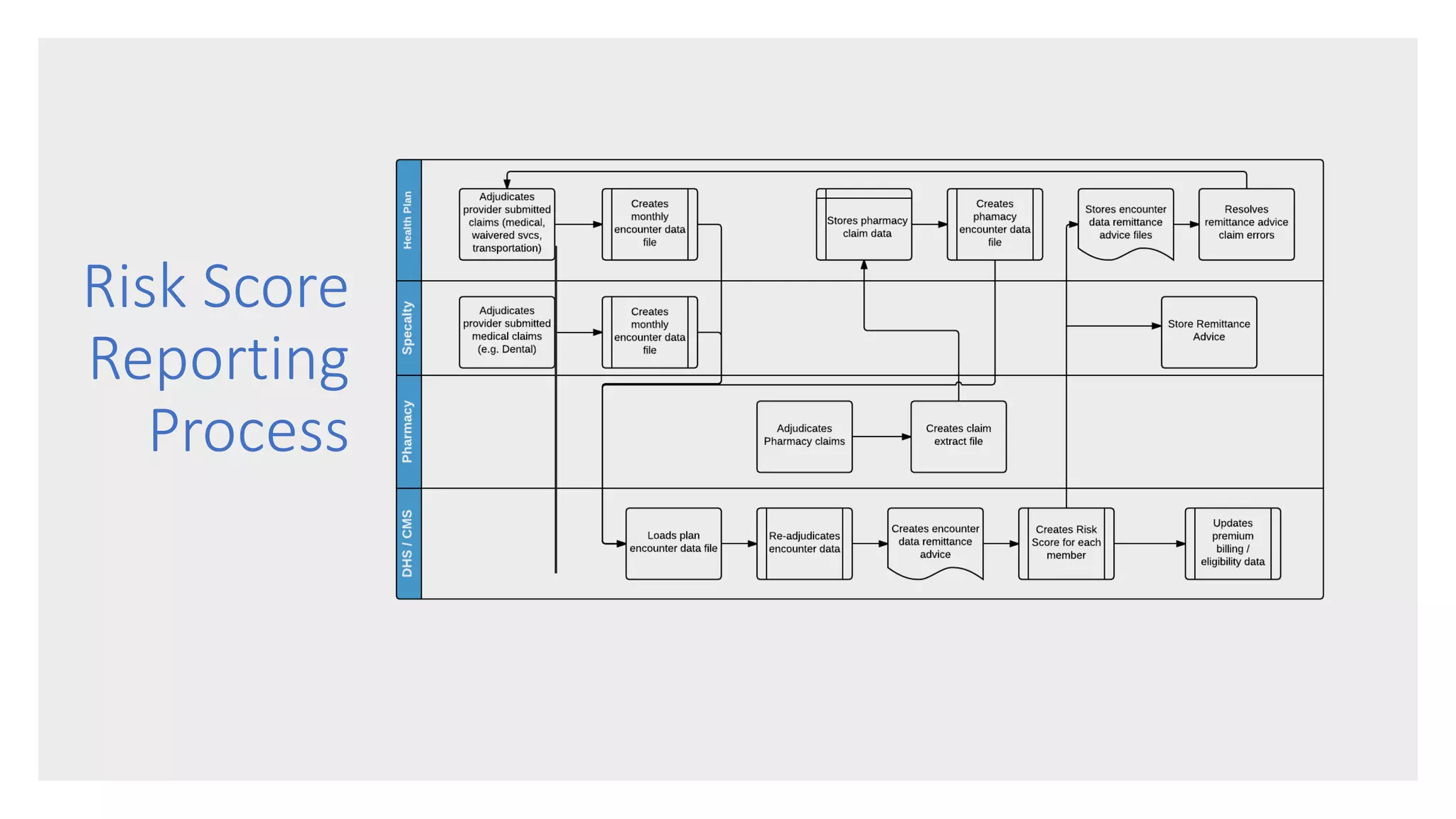
Implementing an effective risk adjustment strategy is important for health plans under the Affordable Care Act. Risk scores are used to determine adjusted capitated payments to plans based on the health status of their members. Risk scores are calculated using diagnosis codes from member encounters and can be positively or negatively affected by how well those codes capture members' health conditions. To maximize risk scores, plans should engage members in their health, provide coding education to providers, conduct chart reviews, and do targeted outreach to ensure all relevant diagnoses are reported for each member annually. This helps ensure accurate revenue for the plan while also improving members' health outcomes and engagement in their care.