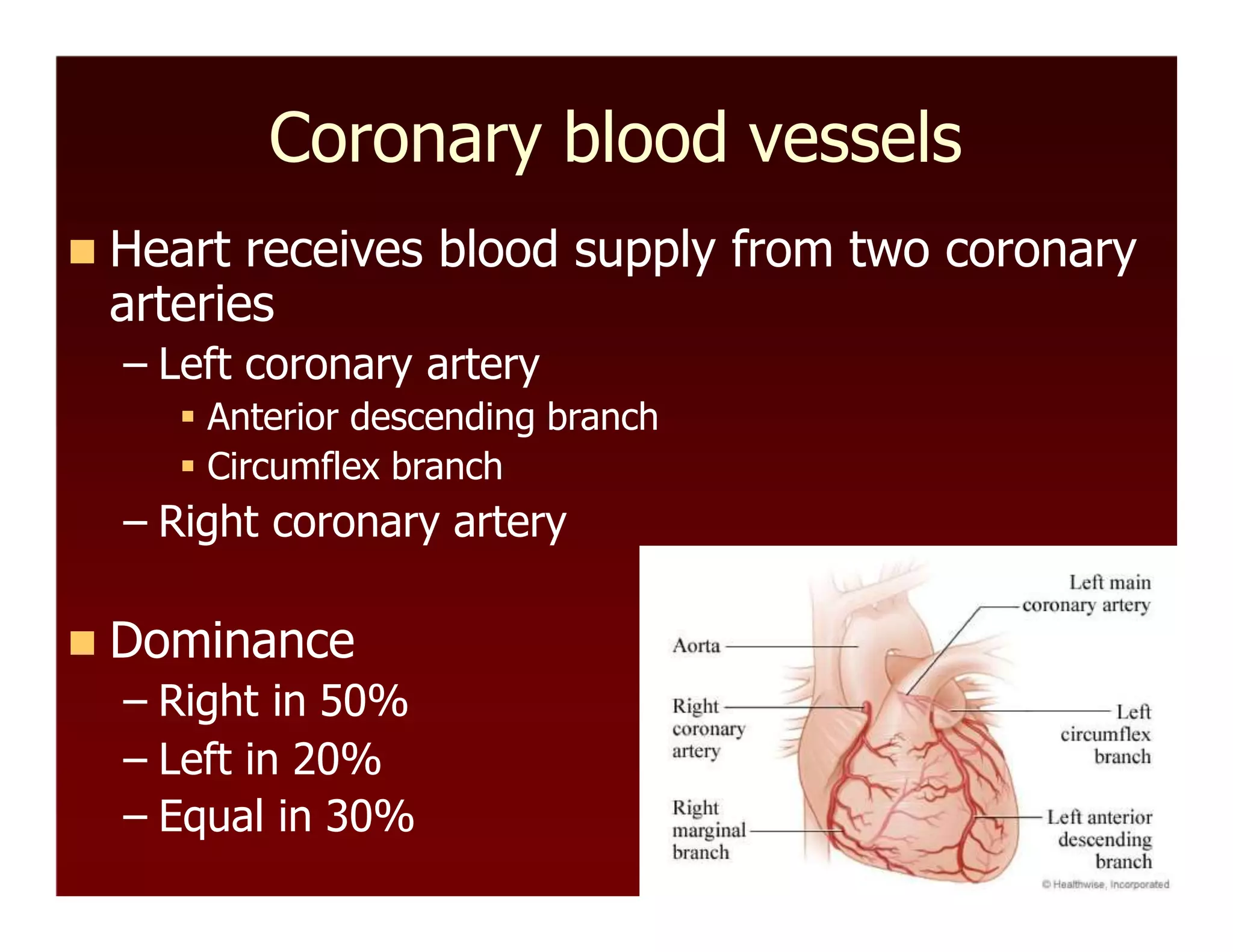
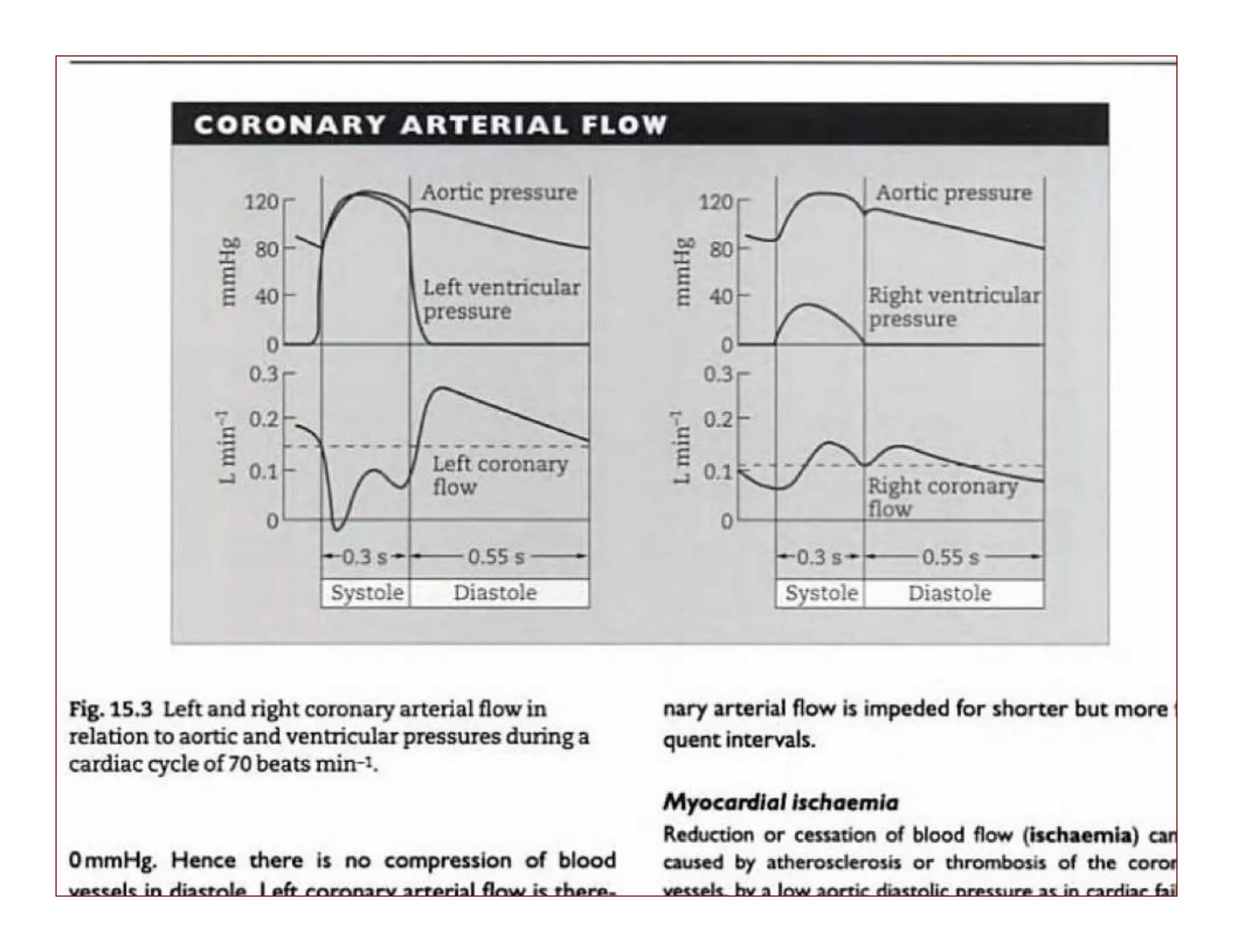
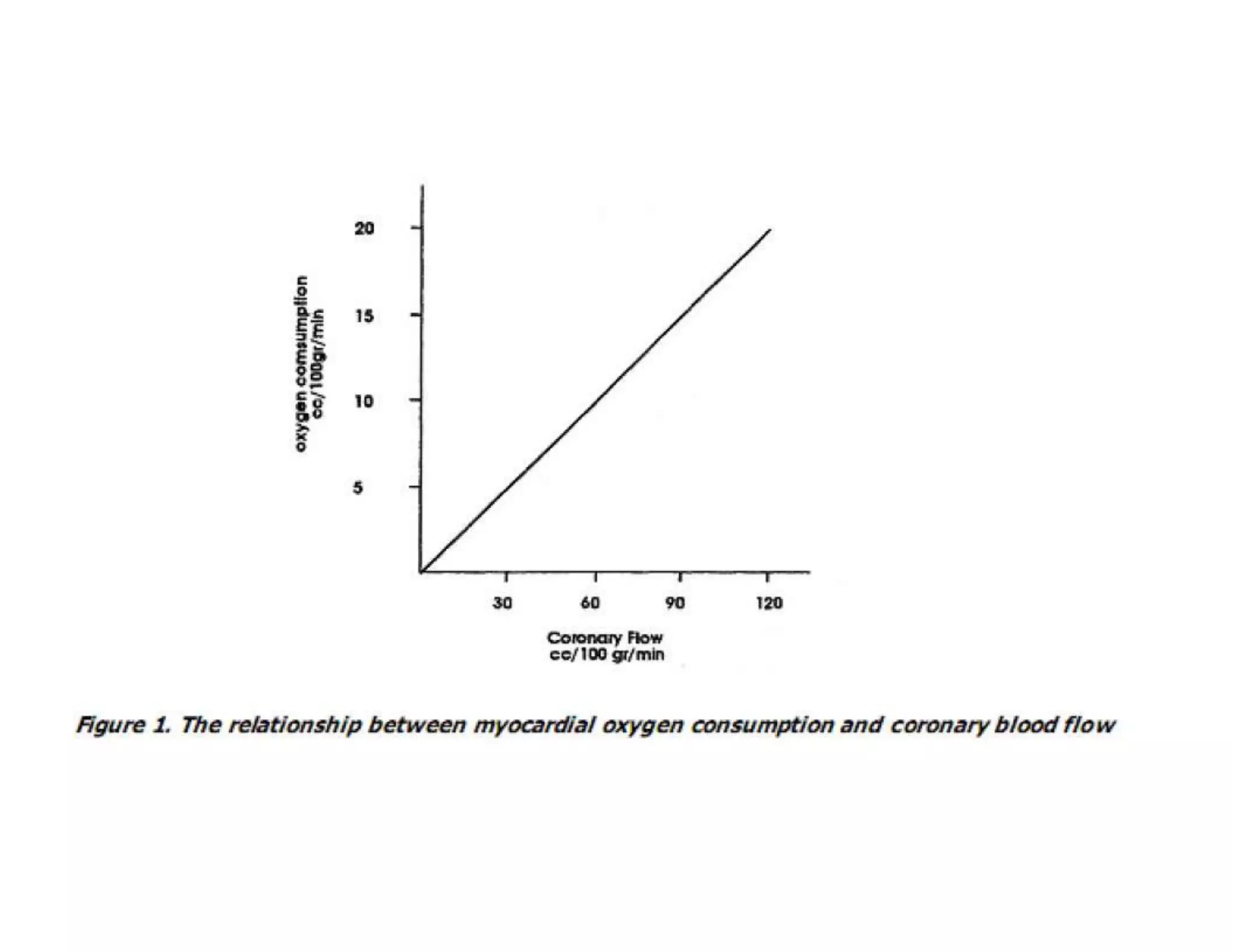
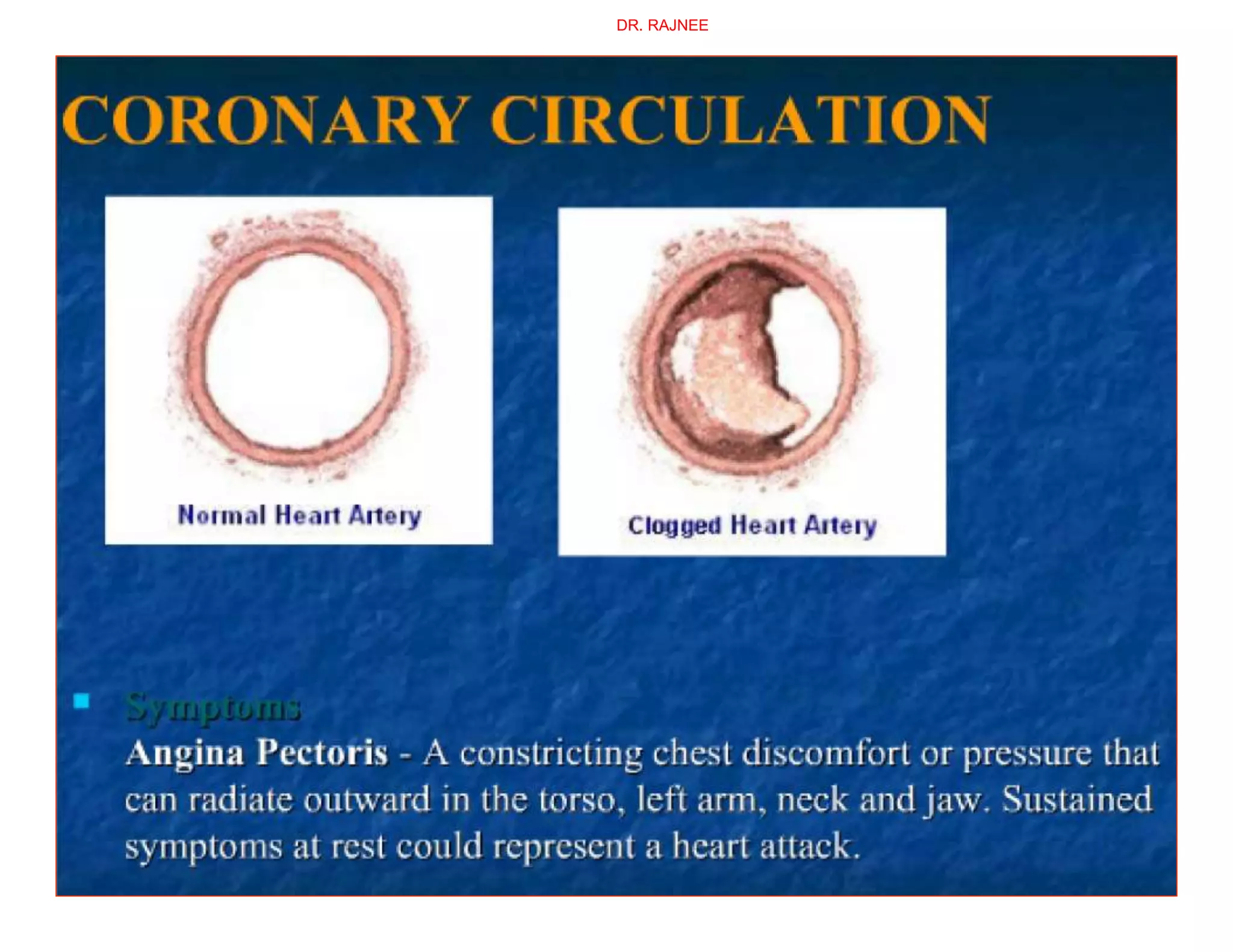
The document discusses regional circulations, focusing on coronary, cerebral, and cutaneous circulation. It provides details on the anatomy, blood supply, regulation, and clinical implications of each circulation. For coronary circulation, it describes the blood vessels that supply the heart muscle and how blood flow is regulated to meet myocardial oxygen demands. For cerebral circulation, it outlines the unique anatomical features of the brain's blood supply and factors that control blood flow. For cutaneous circulation, it explains the role of arteriovenous anastomoses and arterioles in regulating heat transfer and sympathetic nervous system control of cutaneous blood flow.




























![Chemical
Arterial PCO2 (normal, 35-45 mmHg)
– hypercapnia (↑PCO2 ) → dilatation → ↑blood flow
– hypocapnia (↓PCO2 ) → constriction →↓blood flow
– CO2 diffuses from blood into brain ECF
– CO2+H2O → H2CO3 → H++HCO3
– ↑ [H+] → vasodilatation
– blocks Ca2+ entry
– hyperpolarizes the membrane
– ↑NOS activity
DR. RAJNEE](https://image.slidesharecdn.com/regionalcirculationsbyrajnee-200528123828/75/Regional-circulations-by-rajnee-35-2048.jpg)





























![Metabolism (functional hyperemia)
Mediators of Vasodilation
– increased interstitial [K+] →stimulates
Na+/K+ATPase → hyperpolarizes membrane
– interstitial acidosis/hypoxia → hyperpolarizes
membrane
– interstitial hyperosmolarity
– adenosine?
DR. RAJNEE](https://image.slidesharecdn.com/regionalcirculationsbyrajnee-200528123828/75/Regional-circulations-by-rajnee-70-2048.jpg)