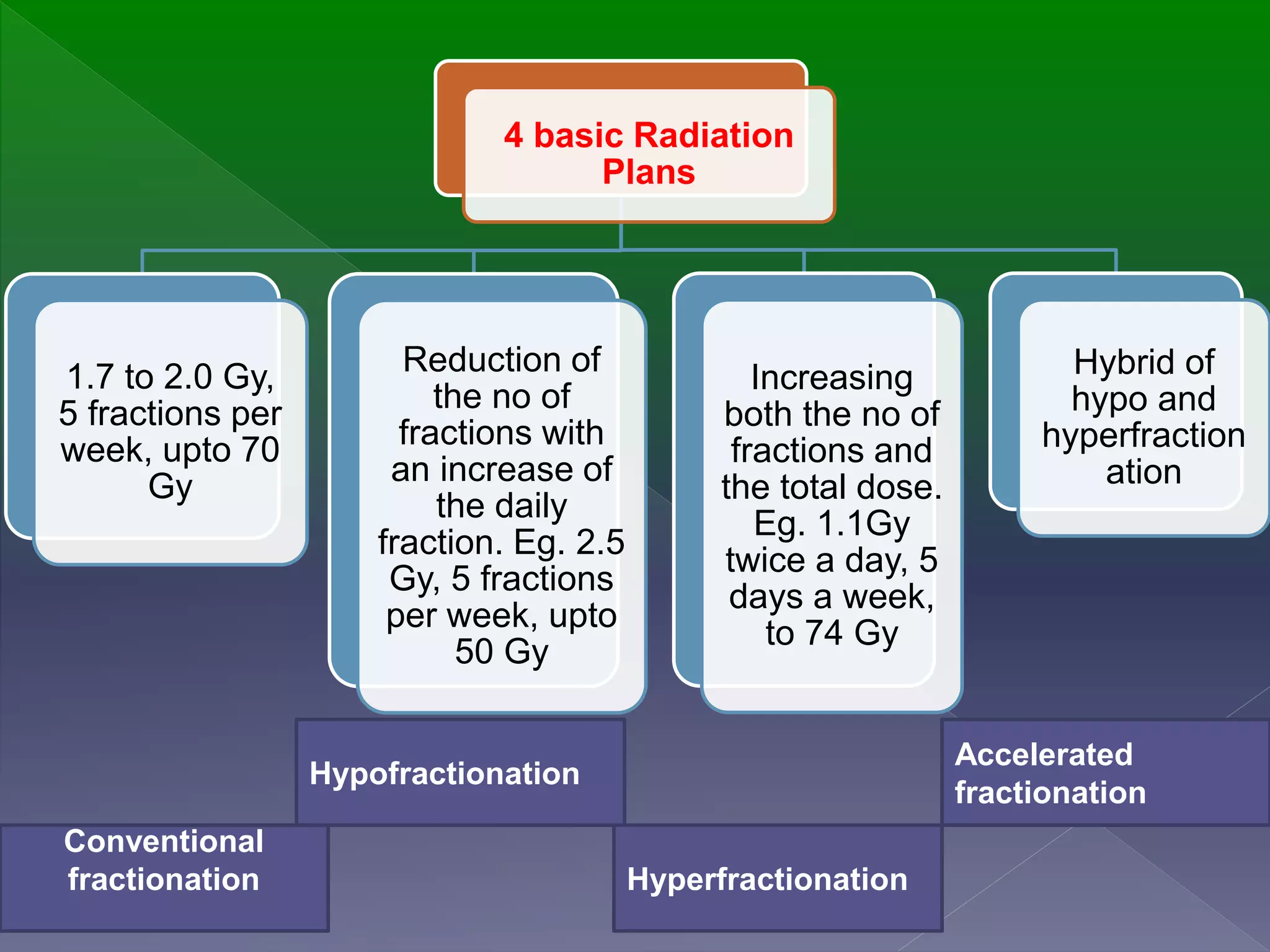
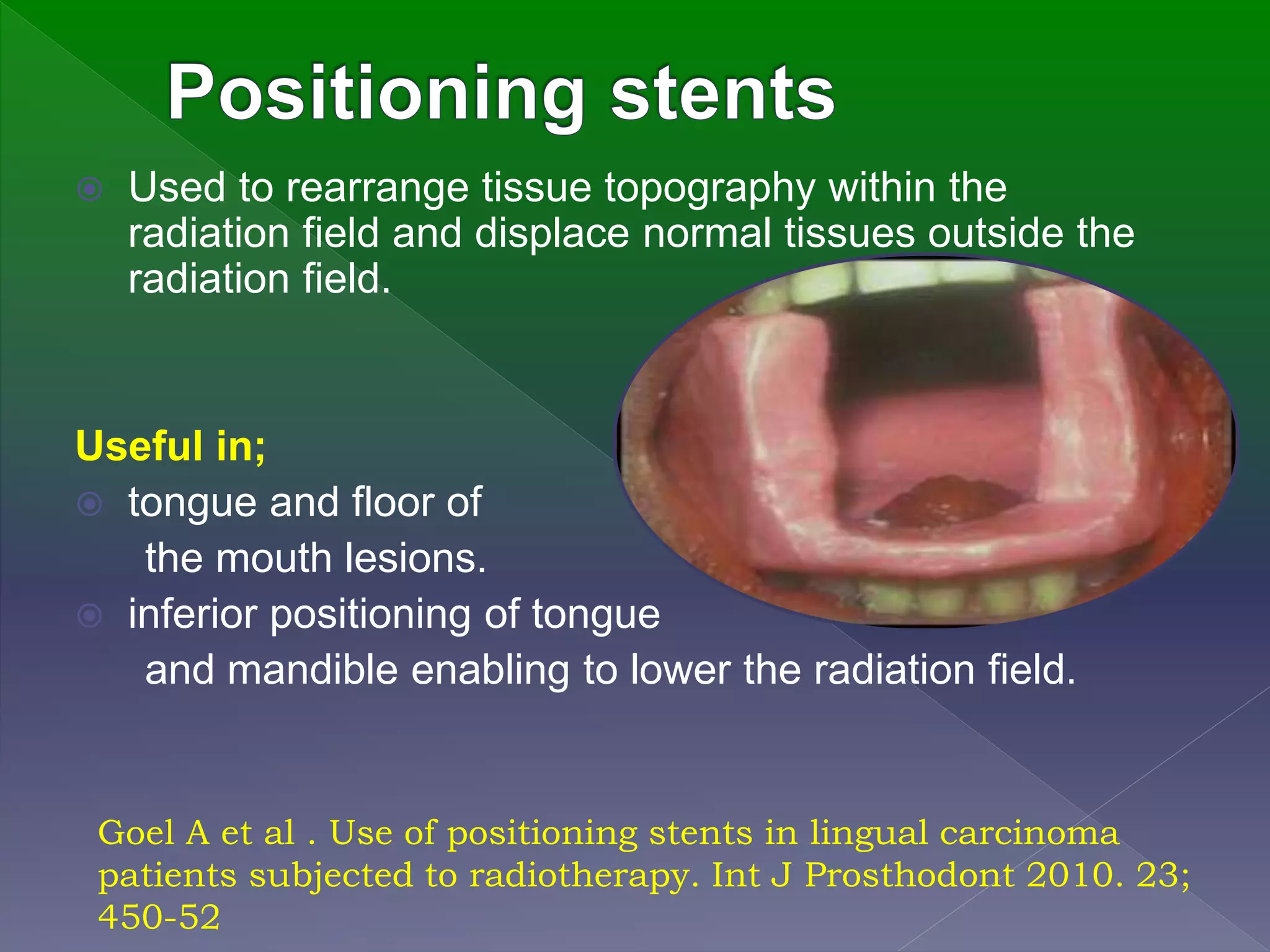
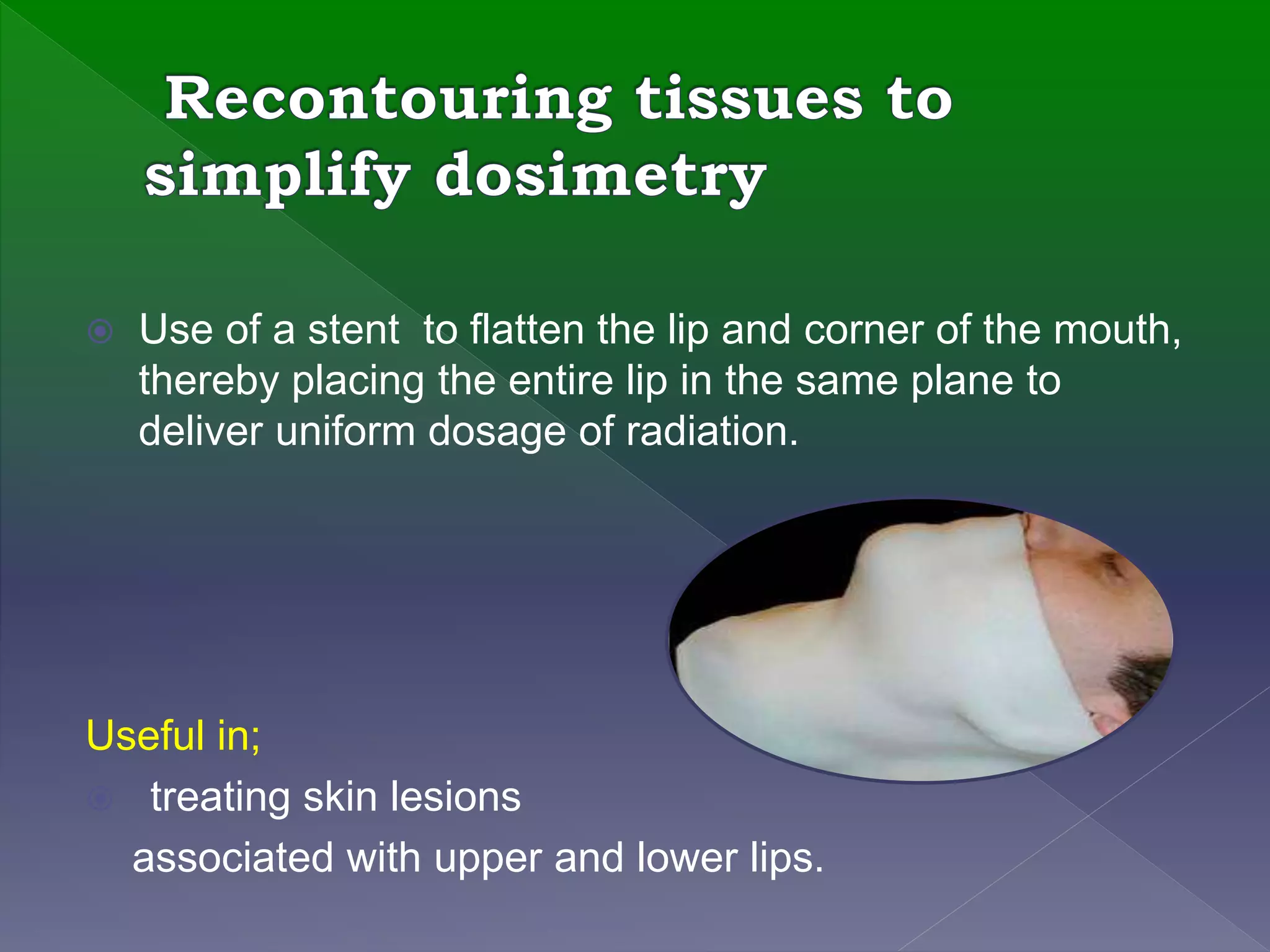
This document discusses the use of radiation therapy in the treatment of head and neck cancers. It notes that radiation therapy is often used alone or in combination with surgery and chemotherapy to treat cancers in areas like the nasopharynx, base of tongue, and soft palate. It also discusses how certain cancer types, like those of the salivary gland and alveolar ridge, are best treated with surgery followed by radiation. The document outlines the goals of radiation therapy and techniques like conventional fractionation, hypofractionation and brachytherapy. It also discusses the use of positioning devices and shields to optimize radiation delivery and reduce side effects.