CA Tongue and its management.pptx
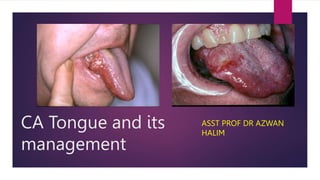
- 1. CA Tongue and its management ASST PROF DR AZWAN HALIM
- 2. Scenario 63yo Malay Male P/w right lateral border of tongue swelling in 5/12 Started as ulcer, claimed due to friction of right lower molar tooth against the tongue Painful associated with odynophagia and slurred speech Ulcer persist despite extraction of the right lower molar tooth +LOW (15kg in 3/12), +LOA No numbness over right lower jaw/lip No PMHX Non smoker and non alcoholic drinker
- 3. Examination Patient comfortable, not cachexic, pink no stridor Intra oral: No trismus, 4x2cm fungating mass at right lateral tongue, anteriorly confined to anterior 2/3 of tongue, not involving the tip, posteriorly involve the post 1/3 of tongue with anterior pillar involved, laterally involving the floor of the mouth, medially crossed midline Limited tongue movement seen, tongue deviated to the right on the tongue protrusion, no fasciculation seen Right retromolar trigone and gingivobuccal sulcus clear.
- 4. Examination Neck : 2x1cm right level 1b node palpable Flexible scope: Base of tongue, vallaculae, epiglottis clear, larynx normal Investigation Incisional biopsy: dorsum – well differentiated SCC, ventral moderated diff. SCC
- 5. An ulcerative squamous cell carcinoma of the undersurface of the tongue. Squamous cell carcinoma of the tongue associated with hyperkeratosis.
- 6. History taking When did the ulcer or growth started Is the size increasing Is it painful – is it local or radiating Is it affecting the speech – slurred Mobility of the tongue Is it affecting oral intake- dysphagia/ odynophagia Bleeding from the ulcer? Any neck lump Any sign of distant metastasis
- 7. History taking We need to established history of smoking, tobacco chewing, vaping, Alcohol drinking Betel nut chewing Dietary deficiency. Eg Plummer Vinson syndrome( due to iron deficiency) increased the risk of oral cancer Dental problem – jagged sharp teeth and ill fitting dentures
- 8. examination Thorough ENT examination has to be done. Otalgia suggests perineural or deep invasion Oral cavity examination must include bimanual examination Look for leukoplakia and erythroplakia Size of the tumor, location of the tumor- ventral/base of tongue or lateral, mobility of the tongue. Endophytic or exophytic lesion Deviation of tongue suggests deep infiltration of muscularity of the tongue. Examination of the teeth and alveolus Trismus present/- Neck examination-To palpate for cervical lymph node metastasis.
- 9. Examination Endophytic lesion ( above) This lesion tend to metastasis more due to deeper and more infiltrating nature Exophytic lesion ( Below)
- 11. Differential diagnosis Benign tumor Solid Cystic Premalignant lesion Malignant lesion Carcinoma Non squamous malignant lesion
- 12. Benign tumor Hemangioma of the tongue Lymphagioma of the tongue
- 13. premalignant Erythroplakia of the lateral border of tongue Leukoplakia of the lateral border of the tongue
- 14. Malignant Melanoma of tongue Leiomyosarcoma of tongue Liposarcoma of tongue
- 15. DIAGNOSIS All ulcerated lesions of the tongue and floor of mouth that last for longer than two to three weeks require an incisional biopsy to confirm the underlying diagnosis All areas of leukoplakia and erythroplakia require a biopsy Excisional biopsy will leave a risk of having positive margin at the deep margin
- 16. imaging Ultrasound Lodder et al, US thus seems to be the optimal technique in patients with no limited mouth opening or base of tongue involvement. US measurement is more reliable than MRI for the measurement of tumour thickness, especially in superficial lesions. CT Scan Ong et al, It is used if there is suspicious of cortical bone involvement, notably the mandible which is able to be diagnosed with a higher level of certainty MRI Ong et al, Tumour invasion of the floor of the mouth is particularly well seen on coronal images. Sagittal images provide information on tongue base involvement and the extent of pharyngeal infiltration that cannot be seen on CT. MRI provides valuable information both within and without the tongue hence it is imaging modality of choice for evaluation of tongue carcinomas
- 17. OPG can be used to assess the state of dentitation and potential gross mandibular invasion Positron emission tomography (PET) is useful in improving the detection of head and neck cancer, especially recurrent disease, but lacks anatomical detail
- 19. Staging Oral cavity, lips, hypopharynx, major salivary gland Lip Oral cavity Hypopharynx clinical/ pathological Major salivary gland clinical/pathological Cutaneous TX Cannot assess Cannot assess Cannot assess Cannot assess Cannot assess Tis In situ In situ In situ In situ In situ T1 Size < 2cm DOI < 5mm Size < 2cm 1 subsite Size < 2cm No extraparenchymal extension Size < 2cm T2 2 < size < 4cm 5 < DOI < 10mm 2 < size < 4cm > 1 subsite 2 < size < 4cm No extraparenchymal extension 2 < size < 4cm T3 Size > 4cm DOI > 10mm Size > 4cm Hemilarynx fixation Esophagus Size > 4cm Extraparenchymal extension Size > 4cm Minor bone erosion Perineurial invasion Deep invasion T4 Moderately advanced/ very advanced Moderately advanced/ very advanced Moderately advanced/ very advanced a Bone Skin FOM Nerve Bone Sinus - maxillary Skin Neck soft tissue - central Cricoid cartilage Thyroid cartilage - outer cortex Hyoid bone Thyroid gland Skin Mandible EAC Nerve - facial Gross cortical/marrow infiltration b Pterygoid plate BOS Masticator Carotid artery - internal encased Prevertebral - invade Carotid artery - encased Mediastinal structure - invade Pterygoid plates Carotid artery BOS BOS & foramen
- 21. Depth of invasion Spiro, et al. : proposed that the increasing depth of tumor thickness, rather than tumor staging have the best correlation with treatment failure of survival Pentenero et al. tumour thickness was shown to be an important parameter for predicting nodal metastases and for surviva
- 22. Goal of treatment The goals of the treatment of cancer of the oral cavity are: 1. Cure of the cancer 2. Preservation or restoration of speech, mastication, swallowing, and external appearance; 3. Minimization of the sequelae of treatment such as dental decay, osteonecrosis of the mandible, and trismus.
- 23. Factors that influence the choice of surgical treatment for a primary tumor of the oral cavity are tumor factors such as: 1. Size and site of the primary tumor (i.e., anterior versus posterior location) 2. Its depth of infiltration 3. The proximity of the tumor to the mandible or maxilla, or involvement of mandible or maxilla. 4. Cervical nodes metastasis
- 24. Tumour thickness (mm) Recommended management >3 Partial glossectomy alone 4-9 Partial glossectomy +/- elective, ipsilateral level I –IV, selective neck dissection >9 Partial glossectomy, neck dissection and post operative radiotherapy to primary site and neck Management of cancer of the oral tongue according to tumour thickness
- 25. Types of glossectomy Partial glossectomy 1/3 or less of tongue Hemiglossectomy 1/3 to ½ of the tongue Near total glossectomy ½ to ¾ of the tongue Total glossectomy or greater of tongue
- 26. For T1/T2 lesion, a transoral partial glossectomy provided adequate margins of resection. This maintains articulation and swallowing function. However, even early stage cancer may be associated with rates of nodal metastasis of 30%. Also, an increase in loco-regional and disease free survival after elective neck dissections for clinically tumor negative necks mandates aggressive treatment.
- 27. For T3/T4 Partial to subtotal glossectomy: 1. modified radical neck dissection type III of N positive neck; 2. ipsilateral selective level I–IV for N0 neck; 3. postoperative radiotherapy of oral cavity and neck.
- 28. Total glossectomy This patient we will have to do a near total glossectomy with radical/modified neck dissection on the ipsilateral side with selective neck dissection on the contralateral side Post operatively radiotherapy should be given
- 29. Total glossectomy The surgical approach for total glossectomy with preservation of the larynx is selected after consideration of several factors: 1. The size and location of the tumor 2. Invasion of the mandible and the need for mandibulectomy 3. The need for neck dissection
- 30. Neck dissection Neck dissection should be done first prior to incision of the primary tumor For this case: A Modified radical neck dissection on the ipsilateral side A selective supraomohyoid neck dissection on the contra lateral side. Rationale for selective or elective neck dissection
- 31. COnsideration Bilateral neck dissections should be considered in tumours that extend to or beyond the midline. Elective neck dissection or elective neck radiotherapy should be considered for: 1. Tumours thicker than 3–4mm. 2. T2 or greater in dimension 3. T1 tumours that demonstrate poor histological features (poor differentiation, double DNA aneuploidy or degree of differentiation at the advancing front)
- 32. Modified radical neck dissection MRND is divided into 3 types: 1. Type 1 (Preservation of SAN) 1. Clinically obvious neck lymph nodes metastasis and SAN not involved by tumor. Usually is an intraoperatively decision 2. Type 2 (Preservation of SAN and IJV) 1. Intra operatively decision when tumor is found to be adherent to SCM but away from IJV and SAN 3. Type 3 (Preservation of SAN, IJV and SCM) 1. Indicated for N1 mobile nodes and not greater than 2.5 – 3.0 cm 2. Contra indicated in the presence of node fixation
- 33. Supra-omohyoid neck dissection En Block removal of cervical lymph node and fibrofatty tissue in regions of I to III, including submandibular gland Posterior limit is the cutaneous branches of the cervical plexus and posterior border of SCM Inferior limit is the superior belly of the omohyoid where it cross IJN
- 34. Surgical appoach Oral cavity tumours can be accessed via : 1. Transoral - T1 and small T2 without mandibular involvoment 2. Pull through technique - For more extensive anterior and lateral floor of mouth cancers without mandibular involvement 3. Mandibulotomy and mandibular swing
- 35. Transoral approach As long as the tumour is small and easily accessible, ( T1 – T2 lesions ) Patients with limited mouth opening, constriction of the oral commissure and previous radiotherapy causing fibrosis, may not be suitable .
- 36. Pull through technique Pull-through technique is indicated for large tumors of the BOT when the surgeon needs wide exposure but does not want to split the mandible or lip
- 37. Pull through
- 38. Visor flap. The superior flap is raised in the subplatysmal plane up to the submandibular level. Intraoral mucosal cuts are then performed transorally with cautery along the lingual surface of the mandible
- 40. MANDIBULOTOMY Mandibulotomy or mandibular osteotomy is an excellent mandible-sparing surgical approach designed to gain access to the oral cavity or oropharynx for resection of primary tumors otherwise not accessible through the open mouth approach. 3 types of mandibulotomy: 1. Lateral (through the body or angle of the mandible)- rarely do (posterior) 2. Midline (anterior) 3. Paramedian. (anterior)
- 41. Comparison of mandibulotomy Lateral Median Paramedian Site of osteotomy Body or angle of mandible Midline Between lateral incisor and canine Exposure Limited Good Good Dental extraction May be required One central incisor Not required Inferior alveolar nerve and vessel Have to be transected Spared Spared Division of geneal muscle Not required Inevitable Not required only the mylohyoid needs division Mechanical stability Poor because of the unequal muscle pull on the 2 mandibular segment Good Good Fixation of osteotomy May required intermaxillary fixation Compression miniplates or stainless steel wire Compression miniplates or stainless steel wire Postoperative RT Osteotomy lies within the lateral portal increased risk Lies outside the lateral portal. Safe Lies outside the lateral portal. Safe
- 45. Lip split incision Paramedian mandibulotomy and a mandibular swing
- 46. The mandibulotomy site is exposed.
- 47. Four drill holes are made prior to bone division.
- 48. The mandible is divided and its two segments are retracted laterally.
- 51. Reconstruction Tissue reconstruction in oropharyngeal defects follows the standard ‘ladder’ approach, as with other tissue sites.
- 52. Aim of reconstruction The aim of reconstruction of the oral tongue following resection is to ensure maximum function of the residual tongue tissue
- 53. Reconstruction Small defects (<1/4) may be closed primarily with maximum preservation of tongue mobility and function. Larger defects, such as a hemiglossectomy defect, are best reconstructed with a thin fasciocutaneous flap, such as a radial forearm or thin anterolateral thigh flap. Defects larger than a hemiglossectomy will require more tissue bulk, and less muscle is left to move the reconstructed tongue.
- 54. Reconstruction Why is tissue bulk important?? 1. It is needed to help the tongue touch the palate to produce better speech and push food toward the hypopharynx. 2. The tissue bulk diverts saliva and food to the lateral gutters during swallowing to minimize aspiration
- 55. The skin paddle of the chosen free flap should be fashioned so as not to restrict residual tongue function and should hopefully augment swallowing. The free flap should be the same size, or slightly smaller than the defect created by the resection
- 56. Post op Radiotherapy 1. T3/T4 primary cancer 2. Positive surgical margins 3. Poor differentiation 4. Perineural invasion 5. Positive lymphnodes 6. Extracapsular spread of nodal disease 7. Perivascular invasion
- 58. recurrence Recurrence rates for oral tongue carcinoma are 10–50 per cent, usually being locoregional. Similar to other sites, recurrence usually occurs within the first two years. Factors that influence local recurrence include: Tumour thickness : due to difficulty in assessing deep clearance intraoperatively The presence of perineural spread. Patients younger than 40 years have been demonstrated to be significantly more likely to develop locoregional failure 10% of patients who have developed a tongue tumour will develop metachronous second tumours of the oral cavity.
- 59. reference Jatin shah 4th edition Stell and Maran 5th edition Scott Brown 7th edition Lodder WL, Teertstra HJ, Tan B, Pameijer FA, Smeele LE, van Velthuysen ML, van den Brekel MW. Tumour thickness in oral cancer using an intra-oral ultrasound probe. European radiology. 2011 Jan 1;21(1):98-106. Ong CK, Chong VF. Imaging of tongue carcinoma. Cancer imaging. 2006;6(1):186. Spiro RH, Huvos AG, Wong GY, Spiro JD, Gnecco CA, Strong EW. Predictive value of tumor thickness in squamous carcinomas confined to the tongue and floor of the mouth. Am J Surg. 1986;152:345–350.
- 60. Pentenero M, Gandolfo S, Carrozzo M. Importance of tumor thickness and depth of invasion in nodal involvement and prognosis of oral squamous cell carcinoma: a review of the literature. Head Neck. 2005;27:1080–1091. Yu P, Robb GL. Reconstruction for total and near-total glossectomy defects. Clinics in plastic surgery. 2005 Jul 31;32(3):411-9. Bertolin A, Ghirardo G, Lionello M, Giacomelli L, Lucioni M, Rizzotto G. Lateral pharyngotomy approach in the treatment of oropharyngeal carcinoma. European Archives of Oto-Rhino-Laryngology. 2017 Jun 1;274(6):2573-80. Sakamoto K, Matsuzaka K, Yama M, Kakizawa T, Inoue T. A case of leiomyosarcoma arising from the tongue. Oral Oncology Extra. 2005 Mar 31;41(3):49-52. Dubin MR, Chang EW. Liposarcoma of the tongue: case report and review of the literature. Head & face medicine. 2006 Jul 26;2(1):21. Huang SH. Oral cancer: Current role of radiotherapy and chemotherapy. Medicina oral, patologia oral y cirugia bucal. 2013 Mar;18(2):e233.
Editor's Notes
- Cancer of the anterior 2/3 of tongue are usually detected earlier than post 1/3 Corners of the anterior 2/3 also tend to be better differentiated
- Radiation is usually to the ipsilateral ear due to the lingual nerve and auricotemporal nerve Sign of distant mets- lung sob hemoptysis pleuritic pain, jaundice bone pain
- Place to inspect for oral cancer
- This is a circumscript lymphagioma of the tongue 4 types lymphagioma simplex, cavernous lymphagioma cystic lymphagioma lymphagioma complex
- Malignant transformation of erythroplakia is 17x higher than leukoplakia
- Squamous cell carcinoma is 90% Non squamous – melanoma, leiomyosarcoma, liposarcoma
- The biopsy site should be at the periphery of the lesion to include a sample of normal mucosa
- orthopantogram
- This is an axial view MRI which shows a right hypodense tongue mass which cross the midline there is still a clear plane between the tongue and the mandible. It involve the extrinsic muscle which is the styloglossus and the palatoglossus Subsequent scan shows 4.6x2.6x4.7 cm with multiple ipsilateral lymphnode Measuring 2xs1cm
- Stage
- Scott brown
- For some posterior floor of mouth tumor withouth mandibular involvement
- Better exposure than transoral – Intact lip sensation – Good facial cosmesis – Intact mandible
- The mylohyoid and digastric muscles are released from the mandible, followed by the genioglossus muscles. Intraoral mucosal cuts are then performed transorally with cautery along the lingual surface of the mandible, taking care to preserve a mucosal cuff of tissue along the inner surface of the mandible to allow for closure
- Pull-through technique. Continuing the cuts up to the retromolar trigone and into the tonsillar fossa and pharynx allows for enough mobility of the tongue so that it can be dropped beneath the mandible and visualized in the neck
- A- roux trotter incision – midline B- Robson incision lateral lip-splitting C-Mc Gregor the straight midline incision with extensions following the contour of the chin D – Modification of Mc Gregor chevron chin contour incision
- . 3
- Steps 1)tracheostomy 2) incision is made using lip split together with a modified schobinger and access via mandibular swing. Important to preserve mental nerve for sensation of the lower lip
- ) the periosteum iscleared either side of the mandibulotomy. With the mandibulotomy between tooth roots or through one Mandibulotomy is planned as stepped incision and is preplated with titanium plates and screw. Bone is cut then mandible is swung laterally as the mylohyoid and anterior belly of digastric are cut. Tumor is excised Lingual and hypoglossal nerves are identified and preserve Reconstruction is
- mucosa and submucosal soft tissues are divided and the mandible is retracted to expose the mylohyoid muscle. the proposed site of resection is marked.
- The tumor is resected en bloc with the surgical defect in the middle third of the tongue.
- Secondary healing intention Primary healing Delayed primary closure Skin graft Tissue expansion Local tissue transfer Free tissue transfer
- since the complex function of the tongue cannot be replicated with current reconstructive techniques. Eg of function of tongue is articulation For taste Formation of bolus
- ‘close’ resection margins tumor within 5 mm of the inked resection margin in formalin fixed surgical specimens
- Fig. 1. Summary of Risk Grouping and Role of Postoperative Radiotherapy +/- Chemotherapy. Abbreviations: LVI: lympho-vascular invasion; ECE: extra-capsular invasion; PORT: postoperative radiotherapy; POCRT: postoperative chemoradiotherapy; LRC: locoregional control; DFS: disease-free survival; OS: overall survival; NS: not statistical significant Note: 1. Crude estimates of expected outcomes were obtained from the following sources: • Low-risk: Huang, et al. (8) • Intermediate-risk: Langendjk, et al. (25), • High-risk: Bernier, et al. (2) from the experimental arms of the combined report of RTOG #9501 and EORTC #22931 2. Treatment effect size: • PORT vs. Surgery: Mishra, et al (55) • POCRT vs. PORT: Bernier, et al (2)