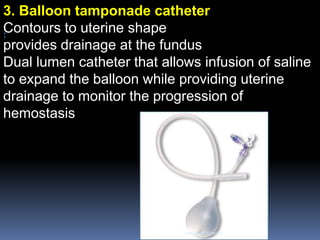
Uterine balloon tamponade is an effective treatment for postpartum haemorrhage when standard medical treatments have failed. Various balloon devices can be inserted into the uterine cavity and inflated to exert pressure and stop bleeding. Balloons are made of materials like condoms, Foley catheters, or purpose-built devices. When inflated, they work by applying pressure against the uterine walls to compress blood vessels and control bleeding. Balloon tamponade is a minimally invasive option that can prevent the need for hysterectomy in many cases by controlling bleeding without surgery.













![• Bleeding is observed, and when it is reduced
considerably, further inflation is stopped and the outer
end of the catheter is folded and tied with thread.
• Oxytocin drip for at least 6 h after the procedure.
• The uterine condom is kept tight in position by ribbon
gauze pack or another inflated condom placed in the
vagina.
• The condom catheter is kept for 24-48 h and then is
deflated gradually over (10-15 m) and removed.
• Triple antibiotic coverage (amoxicillin [500 mg/6 h] +
metronidazole [500 mg/8 h] + gentamicin [80 mg/8
hrs]) for 7 d.
Aboubakr Elnashar](https://image.slidesharecdn.com/pphgebaloon-140804152032-phpapp02/85/Baloon-tamponade-in-management-of-postpartum-haemorrhage-15-320.jpg)