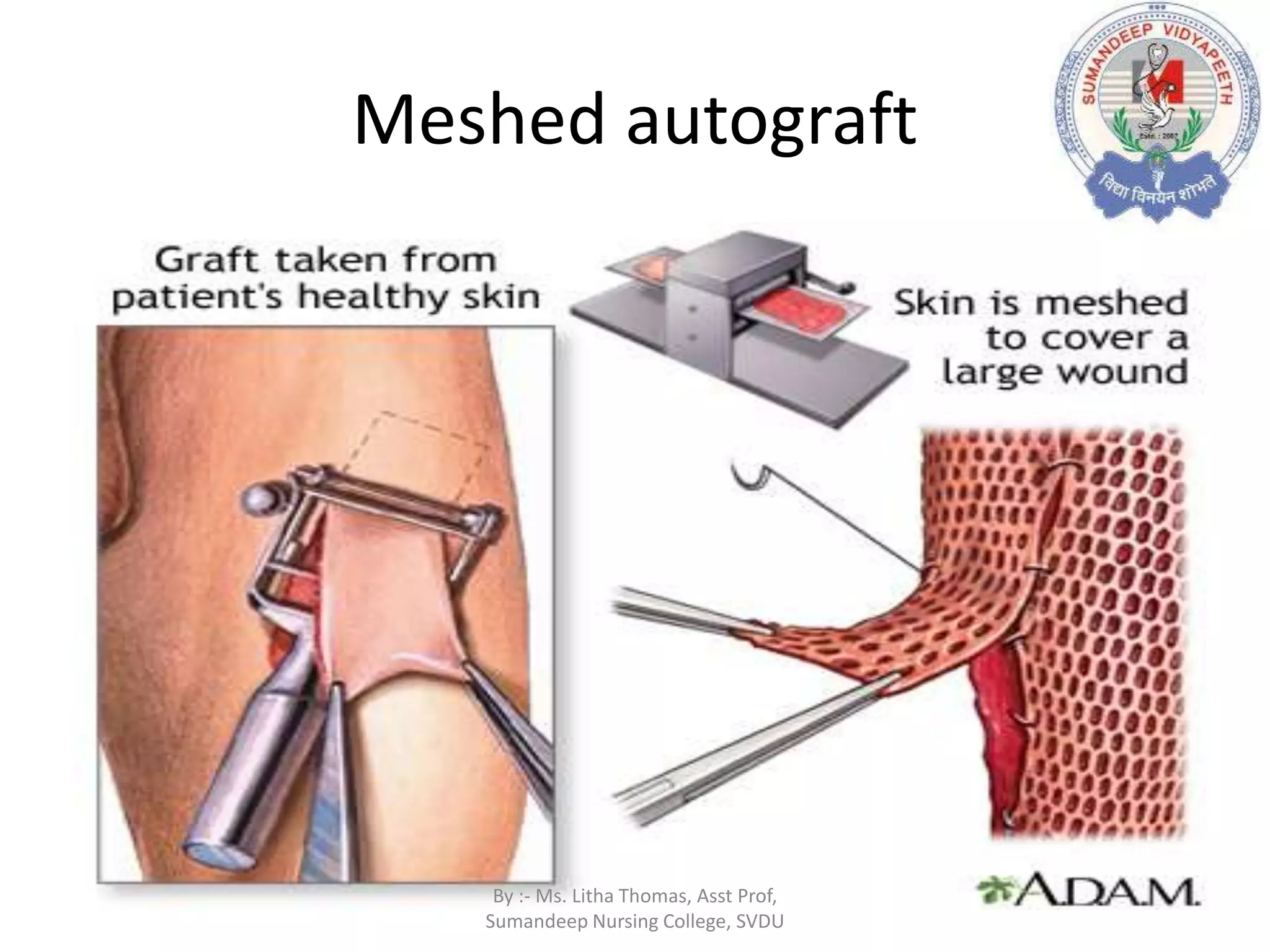
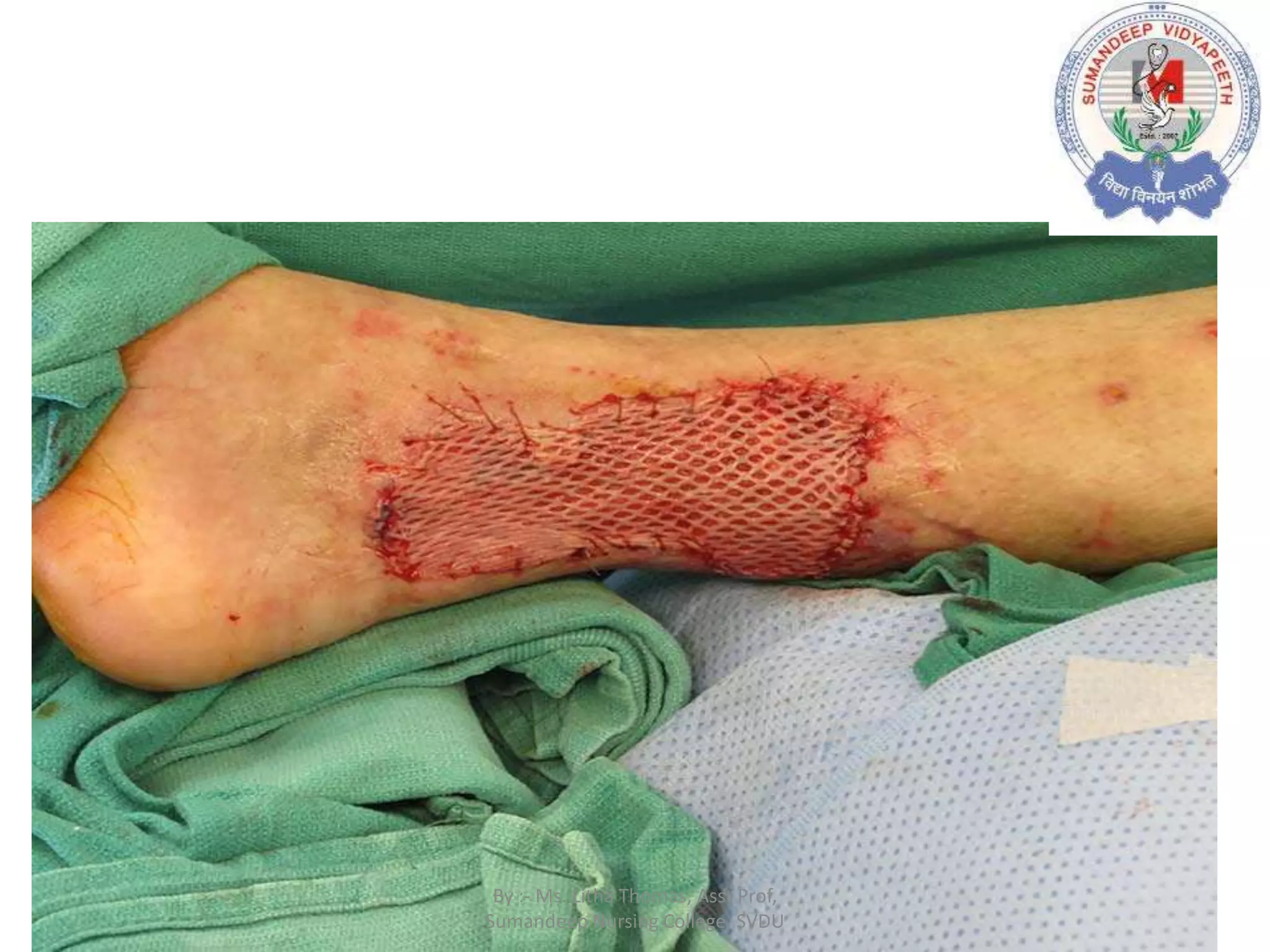
Plastic surgery aims to restore form and function through procedures like skin grafting. Skin grafting involves transferring skin from a donor site to cover wounds or defects. There are two main types - split thickness grafts which include the epidermis and part of the dermis, and full thickness grafts which include the full thickness of skin. The procedure involves harvesting skin using a dermatome for split grafts or scalpel for full grafts, then securing the graft to the recipient site. Post-operative care focuses on monitoring the graft for adherence and infection while it integrates over 3-5 days through plasmatic imbibition and vascular inosculation.



![Can be divided into 2 major areas
1] Reconstructive Surgery
2] Cosmetic (Aesthetic) Surgery
By :- Ms. Litha Thomas, Asst Prof,
Sumandeep Nursing College, SVDU](https://image.slidesharecdn.com/plasticsurgery-200506064809/75/Plastic-surgery-4-2048.jpg)
![1] Reconstructive Surgery
• Reconstructive Surgery is use of surgery to
restore the form and function of the body
and to approximate a normal appearance
• Eg :-
–in burns,
–congenital deformities like cleft palate,
cleft lip
–Infection, disease
–Removal of cancer or tumours.
By :- Ms. Litha Thomas, Asst Prof,
Sumandeep Nursing College, SVDU](https://image.slidesharecdn.com/plasticsurgery-200506064809/75/Plastic-surgery-5-2048.jpg)