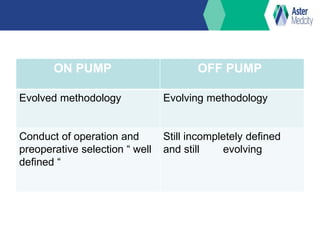
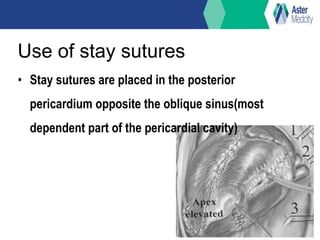
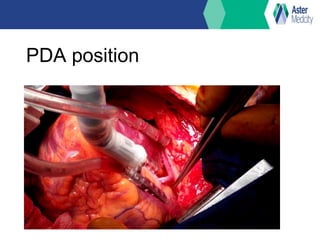
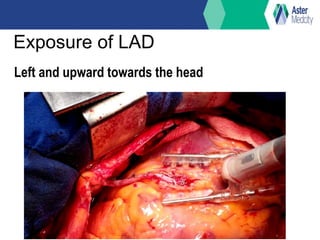
OP CAB (off-pump coronary artery bypass) involves bypass grafting without the use of cardiopulmonary bypass. It was first performed in the 1960s but later eclipsed by on-pump CABG using cardiopulmonary bypass. Interest in OP CAB resumed in the 1980s due to certain advantages over on-pump CABG like reduced blood loss, renal dysfunction, and short-term neurological complications. While both techniques are effective, studies have found OP CAB may reduce certain risks but be more technically challenging with a longer learning curve compared to on-pump CABG. Current indications for OP CAB include patients aged 70 or older, low ejection fraction, previous cardiac surgery, or comorbidities affecting the risk of