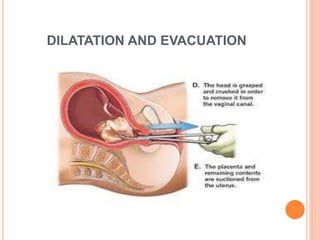
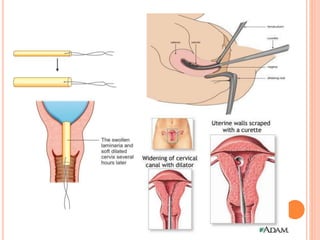
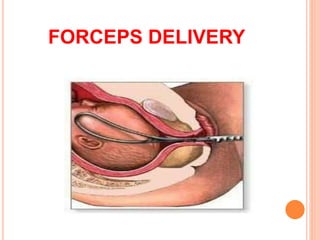
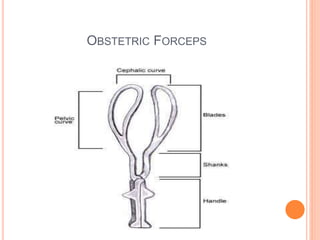
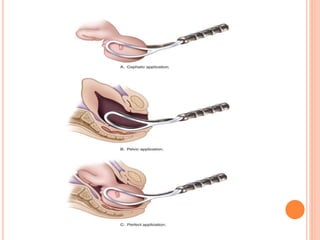
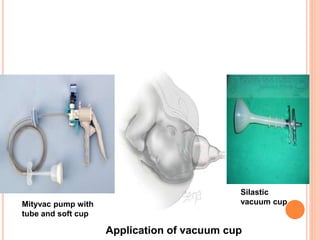
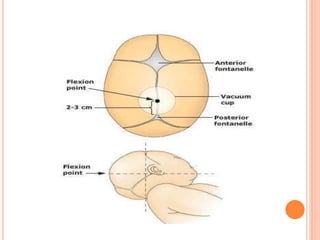
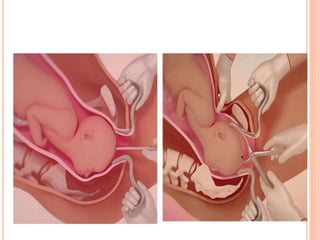
The document outlines various obstetrical procedures such as dilatation and evacuation, forceps delivery, vacuum extraction, and cesarean sections, explaining their indications, steps, complications, and management. It describes the specific techniques involved in forceps and vacuum deliveries, including prerequisites and maternal and fetal indications. Additionally, it touches on destructive surgeries like craniotomy, decapitation, and evisceration, specifying conditions for their application and postoperative care.