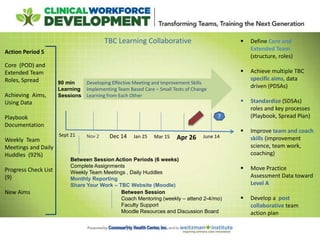
Here are some questions teams have about core and extended teams, pre-visit planning/huddles, self-management goal setting workflows, and the coaching role:
Core and Extended Teams:
- How are you identifying your patient care teams (PODS) so staff and patients know their team?
- What specific roles have you seen change on teams and how?
- How are you training staff on team-based care?
- How do you maintain team integrity with turnover/MAs covering multiple teams?
- Are managers/leaders part of your core and extended team model?
Pre-Visit Planning and Huddles:
- How do you manage prep time for huddles? Are